Back
BackAutonomic Nervous System: Structure, Function, and Control
Study Guide - Smart Notes

Autonomic Nervous System (ANS): Overview
The Autonomic Nervous System (ANS) is a division of the peripheral nervous system responsible for involuntary regulation of internal organs, smooth muscle, cardiac muscle, and glands. It maintains homeostasis by balancing the activities of the sympathetic and parasympathetic divisions, which often have opposing effects on target organs.
Structural Organization of the Nervous System
Central Nervous System (CNS): Brain and spinal cord.
Peripheral Nervous System (PNS): Sensory (afferent) and motor (efferent) divisions.
Motor Division: Subdivided into the somatic nervous system (voluntary control of skeletal muscles) and the autonomic nervous system (involuntary control of viscera).
Sympathetic and Parasympathetic Divisions
The ANS is divided into two main branches:
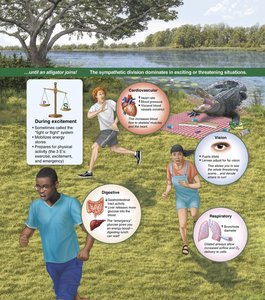
Sympathetic Division: Prepares the body for 'fight or flight' responses during stress or emergency situations.
Parasympathetic Division: Promotes 'rest and digest' activities, conserving energy and maintaining daily bodily functions.


Key Anatomical Differences
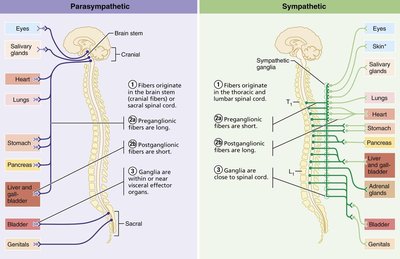
Origin: Sympathetic fibers originate from thoracolumbar regions (T1–L2); parasympathetic fibers from craniosacral regions (brainstem and S2–S4).
Ganglia Location: Sympathetic ganglia are close to the spinal cord; parasympathetic ganglia are near or within target organs.
Fiber Length: Sympathetic: short preganglionic, long postganglionic; Parasympathetic: long preganglionic, short postganglionic.
Functional Roles
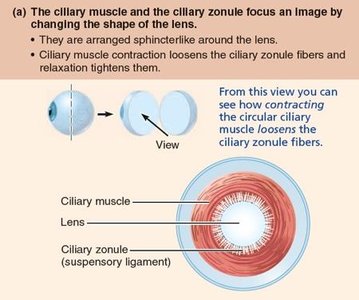
Sympathetic: Increases heart rate, dilates pupils, inhibits digestion, mobilizes energy stores.
Parasympathetic: Decreases heart rate, constricts pupils, stimulates digestion, promotes energy storage.
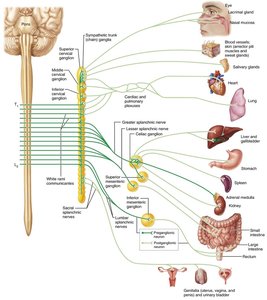
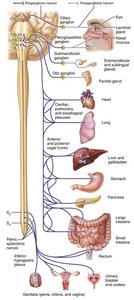
Anatomy of the ANS Pathways
Parasympathetic Pathways
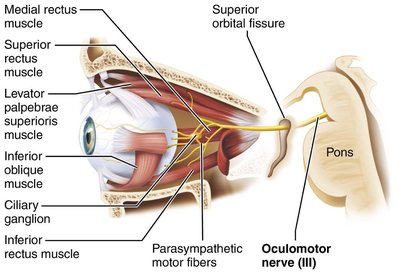
Cranial Outflow: Cranial nerves III (oculomotor), VII (facial), IX (glossopharyngeal), and X (vagus) carry parasympathetic fibers to head, thoracic, and abdominal organs.
Sacral Outflow: S2–S4 spinal nerves innervate the distal large intestine, bladder, and reproductive organs.
Sympathetic Pathways
Thoracolumbar Origin: Preganglionic neurons arise from T1–L2 segments of the spinal cord.
Sympathetic Trunk: Paired chains of ganglia running alongside the vertebral column.
Collateral Ganglia: Located anterior to the vertebral column, serving abdominal and pelvic organs.
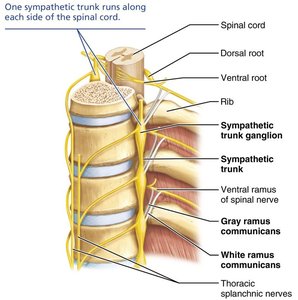
Three Pathways of Sympathetic Innervation
Synapse in the same level trunk ganglion.
Ascend or descend to synapse in a different trunk ganglion.
Pass through trunk to synapse in a collateral ganglion anterior to the vertebral column.
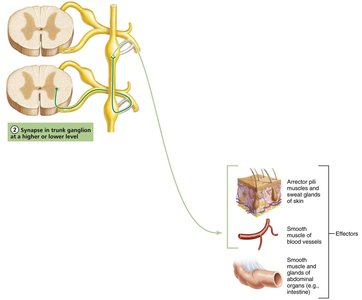
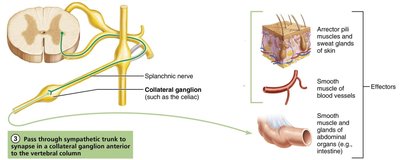
Autonomic Ganglia: Classification and Location
Name | Division | Location |
|---|---|---|
Terminal ganglia | Parasympathetic | Within or near organ (intramural) |
Sympathetic trunk ganglia | Sympathetic | Beside vertebral column |
Collateral (prevertebral) ganglia | Sympathetic | Anterior to vertebral column |
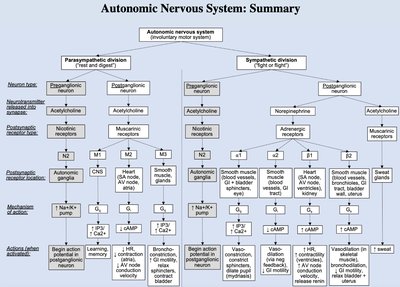
Neurotransmitters and Receptors in the ANS
Cholinergic Receptors
Nicotinic Receptors (N): Found on all postganglionic neurons (sympathetic and parasympathetic) and adrenal medulla; always excitatory.
Muscarinic Receptors (M): Found on all parasympathetic target organs; effect can be excitatory or inhibitory depending on the organ and receptor subtype (M1, M2, M3).
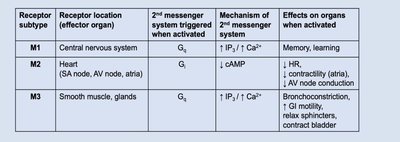

Receptor subtype | Location | 2nd Messenger | Effect |
|---|---|---|---|
M1 | CNS | Gq / ↑IP3, ↑Ca2+ | Memory, learning |
M2 | Heart | Gi / ↓cAMP | ↓HR, ↓contractility |
M3 | Smooth muscle, glands | Gq / ↑IP3, ↑Ca2+ | Bronchoconstriction, ↑GI motility, contract bladder |
Adrenergic Receptors
Alpha (α1, α2) and Beta (β1, β2) Receptors: Found on sympathetic target organs; effects depend on receptor subtype and location.
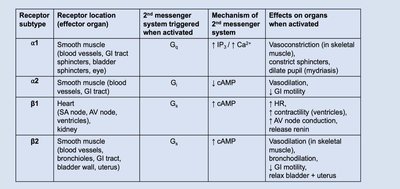
Receptor subtype | Location | 2nd Messenger | Effect |
|---|---|---|---|
α1 | Blood vessels, GI tract, bladder sphincters, eye | Gq / ↑IP3, ↑Ca2+ | Vasoconstriction, constrict sphincters, dilate pupil |
α2 | Blood vessels, GI tract | Gi / ↓cAMP | ↓GI motility |
β1 | Heart, kidney | Gs / ↑cAMP | ↑HR, ↑contractility, release renin |
β2 | Bronchioles, GI tract, bladder wall, uterus | Gs / ↑cAMP | Bronchodilation, relax bladder & uterus |
Functional Effects of the ANS on Organs
Target | Parasympathetic Effects | Sympathetic Effects |
|---|---|---|
Heart | Decreases heart rate | Increases heart rate and force |
Lungs | Constricts bronchioles | Dilates bronchioles |
Digestive tract | Increases motility, relaxes sphincters | Decreases motility, constricts sphincters |
Pupil (iris) | Constricts pupil | Dilates pupil |
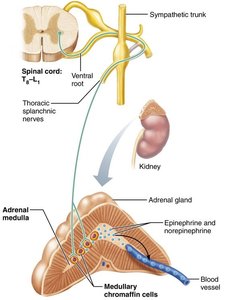
Adrenal medulla | No effect | Stimulates epinephrine/norepinephrine release |
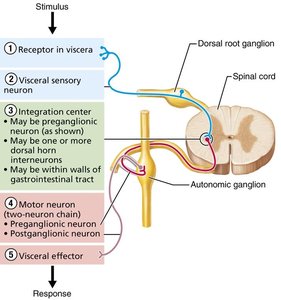
Visceral Reflexes
Visceral reflex arcs control involuntary responses of smooth muscle, cardiac muscle, and glands. They share the same basic components as somatic reflex arcs but differ in having two motor neurons and visceral effectors.
Components: Receptor, sensory neuron, integration center, motor neuron (preganglionic and postganglionic), effector.
Effectors: Smooth muscle, cardiac muscle, glands.
CNS Control of the ANS
The ANS is regulated at multiple levels of the CNS, including the spinal cord, brainstem, hypothalamus, and cerebral cortex. The hypothalamus is the main integration center for autonomic functions, coordinating responses to maintain homeostasis.
Summary Table: Anatomical and Physiological Differences
Characteristic | Parasympathetic | Sympathetic |
|---|---|---|
Origin | Craniosacral (brainstem, S2–S4) | Thoracolumbar (T1–L2) |
Ganglia location | Near/within target organ | Close to spinal cord |
Preganglionic fiber length | Long | Short |
Postganglionic fiber length | Short | Long |
Neurotransmitter (postganglionic) | Acetylcholine (ACh) | Norepinephrine (NE) (except sweat glands: ACh) |
Functional role | Rest and digest | Fight or flight |
Autonomic Nervous System: Summary Diagram