 Back
BackBlood Vessels and Circulation: Structure, Function, and Regulation
Study Guide - Smart Notes

Blood Vessel Structure and Function
Overview of Blood Vessels
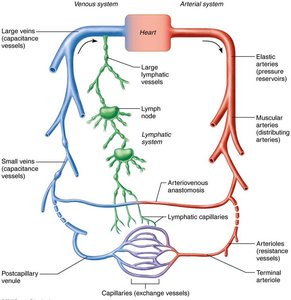
Blood vessels are dynamic structures that form a delivery system beginning and ending at the heart. They pulsate, constrict, relax, and multiply, working in concert with the lymphatic system to circulate fluids throughout the body.
Arteries: Carry blood away from the heart; typically oxygenated except for pulmonary circulation and fetal umbilical vessels.
Veins: Carry blood toward the heart; typically deoxygenated except for pulmonary circulation and fetal umbilical vessels.
Capillaries: Serve as exchange vessels, making direct contact with tissue cells to meet cellular needs.
Blood Vessel Wall Structure
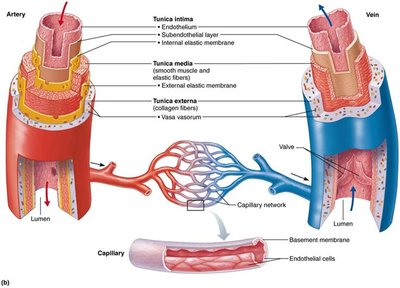
All vessels (except capillaries) have three layers, or tunics, surrounding a central lumen:
Tunica Intima: Innermost layer, in direct contact with blood.
Tunica Media: Middle layer, mainly smooth muscle and elastin; controls vasoconstriction and vasodilation.
Tunica Externa (Adventitia): Outermost layer, mostly loose collagen fibers; protects, reinforces, and anchors the vessel.
Capillaries consist only of endothelium with a sparse basal lamina. 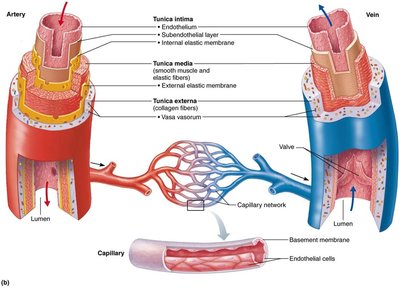
Types of Arteries
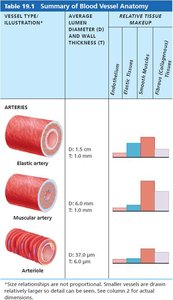
Arteries are classified by size and function:
Elastic Arteries: Thick-walled, large lumen; act as pressure reservoirs (e.g., aorta).
Muscular Arteries: Distribute blood to organs; active in vasoconstriction.
Arterioles: Smallest arteries; control flow into capillary beds via diameter changes.
Capillaries
Capillaries are microscopic vessels with walls of thin tunica intima. Their small diameter allows only a single red blood cell to pass at a time.
Pericytes: Spider-shaped stem cells that stabilize capillary walls and aid in repair.
Functions: Exchange of gases, nutrients, wastes, and hormones between blood and interstitial fluid.
Types of Capillaries
Continuous Capillaries: Least permeable; abundant in skin, muscles, lungs, and CNS. Brain capillaries form the blood-brain barrier.
Fenestrated Capillaries: Have pores for increased permeability; found in kidneys, intestines, and endocrine glands.
Sinusoidal Capillaries: Most permeable; found in liver, bone marrow, spleen, and adrenal medulla.
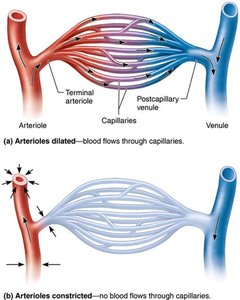
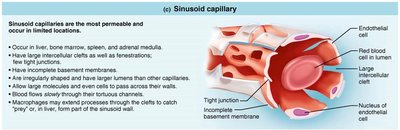
Capillary Beds and Microcirculation
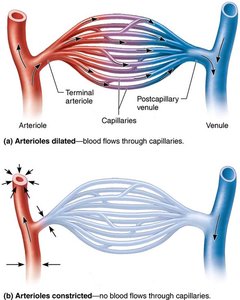
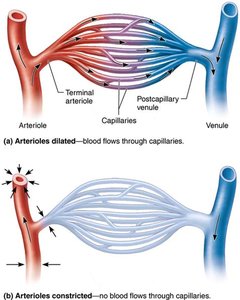
Capillary beds are networks between arterioles and venules. Microcirculation refers to blood flow from arteriole to venule through the capillary bed.
Terminal Arteriole: Branches into capillaries for exchange.
Postcapillary Venule: Drains capillaries.
Flow is controlled by diameter of arterioles and terminal arterioles.
Veins and Venous Return
Veins form as venules converge and have thinner walls and larger lumens than arteries.
Venous Valves: Prevent backflow; most abundant in limbs.
Venous Sinuses: Flattened veins with thin walls (e.g., coronary sinus).
Varicose Veins: Dilated veins due to incompetent valves; common in lower limbs.
Vascular Anastomoses
Importance of Vascular Anastomoses
Vascular anastomoses are interconnections between blood vessels.
Arterial Anastomoses: Provide alternate pathways (collateral channels) for blood flow.
Arteriovenous Anastomoses: Shunt blood across capillary beds.
Venous Anastomoses: So abundant that occluded veins rarely block blood flow.
Vasoconstriction and Vasodilation
Definitions
Vasoconstriction: Decrease in vessel lumen diameter due to smooth muscle contraction.
Vasodilation: Increase in vessel lumen diameter due to smooth muscle relaxation.
Blood Flow, Blood Pressure, and Resistance
Definitions and Relationships
Blood Flow: Volume of blood flowing through a vessel, organ, or entire circulation per unit time (ml/min).
Blood Pressure (BP): Force per unit area exerted on vessel wall by blood; measured in mm Hg.
Resistance: Opposition to flow; mainly due to friction with vessel walls.
Blood Viscosity: Thickness of blood; increased viscosity increases resistance.
Total Vessel Length: Longer vessels increase resistance.
Vessel Diameter: Greatest influence; smaller diameter increases resistance.
Blood Pressure Differences in Vessels
Pressure Gradient and Vessel Types
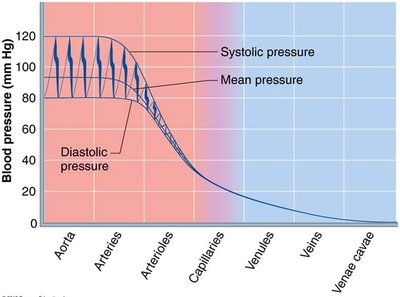
Systemic pressure is highest in the aorta and declines throughout the pathway.
Steepest drop occurs in arterioles.
Blood pressure is pulsatile near the heart, rising and falling with each heartbeat.
Arterial Blood Pressure
Systolic Pressure: Pressure during ventricular contraction (average 120 mm Hg).
Diastolic Pressure: Lowest aortic pressure during heart rest.
Pulse Pressure: Difference between systolic and diastolic pressure.
Regulation of Blood Flow and Pressure
General and Organ-Specific Regulation
Blood flow is regulated by extrinsic (neural and hormonal) and intrinsic (local autoregulation) mechanisms.
Extrinsic Control: Sympathetic nervous system and hormones adjust flow throughout the body.
Intrinsic Control: Local arterioles modify diameter to meet tissue needs.
Factors Aiding Venous Return
Muscular Pump: Skeletal muscle contractions "milk" blood toward the heart.
Respiratory Pump: Breathing changes pressure, moving blood toward the heart.
Sympathetic Venoconstriction: Smooth muscle constriction pushes blood back to the heart.
Blood Pressure Regulation Mechanisms
Cardiac Output (CO)
Peripheral Resistance (PR)
Blood Volume
Blood pressure varies directly with CO, PR, and blood volume.
Neural Regulation
Baroreceptors: Detect changes in pressure; initiate reflexes to maintain MAP.
Chemoreceptors: Detect changes in CO2, pH, and O2; increase BP when needed.
Higher Brain Centers: Medulla and hypothalamus regulate BP during stress and exercise.
Renal Regulation
Direct Mechanism: Kidneys alter blood volume directly.
Indirect Mechanism: Renin-angiotensin-aldosterone system adjusts BP hormonally.
Capillary Exchange and Bulk Flow
Factors and Significance
Velocity of blood flow is fastest in the aorta, slowest in capillaries, and increases in veins.
Slow capillary flow allows time for exchange between blood and tissues.
Bulk fluid flow across capillary walls maintains interstitial environment.
Direction and amount of fluid flow depend on hydrostatic and colloid osmotic pressures.
Clinical Implications: Edema
Edema is an abnormal increase in interstitial fluid, caused by increased outward pressure or decreased inward pressure.
Can result from incompetent venous valves, vessel blockage, heart failure, inflammation, or low plasma proteins.
Pathways of Circulation
Pulmonary and Systemic Circuits
Pulmonary Circulation: Short loop from heart to lungs and back.
Systemic Circulation: Long loop to all body parts and back.
Hepatic Portal Circulation
Blood flows from digestive organs to the liver via the hepatic portal vein, then returns to the heart.
Summary Table: Blood Vessel Anatomy
Vessel Type | Average Lumen Diameter | Wall Thickness | Relative Tissue Makeup |
|---|---|---|---|
Elastic Artery | 1.5 cm | 1.0 mm | High elastin, moderate smooth muscle |
Muscular Artery | 6.0 mm | 1.0 mm | High smooth muscle, moderate elastin |
Arteriole | 37.0 µm | 6.0 µm | Mostly smooth muscle |

Key Equations
Relationship between Flow, Pressure, and Resistance:
Mean Arterial Pressure (MAP):
Resistance (R) and Vessel Radius:
Blood Pressure Gradient:
Bulk Flow Forces:
Clinical Monitoring
Vital Signs
Pulse and blood pressure, respiratory rate, and body temperature are key indicators of circulatory efficiency.
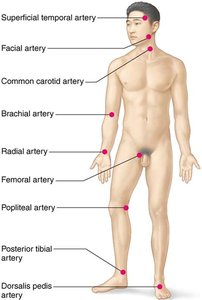
Radial pulse is most commonly used; pressure points can be compressed to stop blood flow during hemorrhage.
Additional info:
Blood vessel structure and function are foundational to understanding cardiovascular physiology and pathology.
Regulation of blood flow and pressure is critical for maintaining homeostasis and responding to physiological demands.
