 Back
BackBones and Skeletal Tissues: Structure, Function, and Development
Study Guide - Smart Notes

Bones and Skeletal Tissues
Introduction
The human skeleton is a dynamic organ system composed of bones and cartilages. It provides structural support, protection, and facilitates movement, while also serving as a reservoir for minerals and a site for blood cell formation.
Cartilage Structure, Types, and Locations
Skeletal Cartilage
Skeletal cartilage is made of resilient, molded cartilage tissue, primarily water, and contains no blood vessels or nerves.
Perichondrium is a dense connective tissue layer surrounding cartilage, providing nutrients and resisting outward expansion.
Cartilage cells, called chondrocytes, are found in lacunae within a jelly-like extracellular matrix.
Types of Cartilage
Hyaline cartilage: Most abundant; provides support, flexibility, and resilience. Found in articular surfaces, costal cartilages, respiratory structures, and the nose.
Elastic cartilage: Contains elastic fibers; found in the external ear and epiglottis.
Fibrocartilage: Contains thick collagen fibers; provides tensile strength. Found in menisci, pubic symphysis, and intervertebral discs.
Growth of Cartilage
Appositional growth: New matrix is laid down on the surface by cells in the perichondrium.
Interstitial growth: Chondrocytes divide and secrete new matrix from within the cartilage.
Cartilage growth ends during adolescence.
Functions of Bones
Major Functions
Support: Framework for the body and soft organs.
Protection: Shields brain, spinal cord, and vital organs.
Anchorage: Acts as levers for muscle action.
Mineral storage: Reservoir for calcium and phosphorus.
Blood cell formation (hematopoiesis): Occurs in red bone marrow.
Triglyceride storage: Energy reserve in bone cavities.
Hormone production: Osteocalcin regulates insulin, glucose, and energy expenditure.
Classification of Bones
By Location
Axial skeleton: Skull, vertebral column, rib cage.
Appendicular skeleton: Limbs and girdles attaching limbs to axial skeleton.
By Shape
Long bones: Longer than wide, with a shaft and two ends (e.g., femur, humerus).
Short bones: Cube-shaped (e.g., carpals, tarsals); includes sesamoid bones (e.g., patella).
Flat bones: Thin, flat, slightly curved (e.g., sternum, ribs, cranial bones).
Irregular bones: Complicated shapes (e.g., vertebrae, hip bones).
Bone Structure
Gross Anatomy
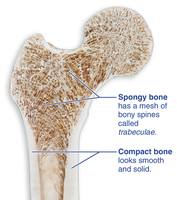
Compact bone: Dense outer layer; appears smooth and solid.
Spongy bone: Honeycomb of trabeculae filled with marrow.
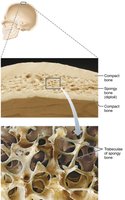
Structure of Short, Irregular, and Flat Bones
Thin plates of spongy bone (diploë) covered by compact bone.
Periosteum covers outside; endosteum covers inside.
Bone marrow is scattered throughout spongy bone; no defined marrow cavity.
Hyaline cartilage covers joint surfaces.
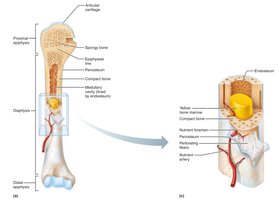
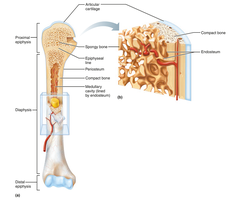
Structure of a Typical Long Bone
Diaphysis: Shaft; compact bone surrounds medullary cavity (yellow marrow in adults).
Epiphyses: Bone ends; compact bone externally, spongy bone internally; articular cartilage covers joint surfaces.
Epiphyseal line: Remnant of growth plate between diaphysis and epiphysis.
Membranes: Periosteum (outer, double-layered), endosteum (internal, lines canals and trabeculae).
Hematopoietic Tissue in Bones
Red bone marrow: Found in trabecular cavities of spongy bone and diploë of flat bones; site of hematopoiesis.
In adults, active in flat bones and some irregular bones (e.g., hip bone).
Yellow bone marrow: Can convert to red marrow if necessary (e.g., anemia).
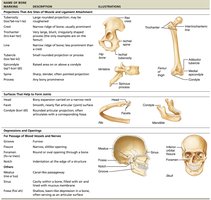
Bone Markings
Bone markings are anatomical features that serve as sites for muscle, ligament, and tendon attachment, joint formation, or passageways for blood vessels and nerves.
Marking | Description | Example |
|---|---|---|
Projection | Site of muscle/ligament attachment | Tuberosity, crest, trochanter |
Surface | Form joints | Head, facet, condyle |
Depression/Opening | Passage for vessels/nerves | Foramen, fossa, groove |
Microscopic Anatomy of Bone
Bone Cells
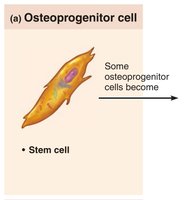
Osteoprogenitor (osteogenic) cells: Stem cells in periosteum and endosteum; differentiate into osteoblasts or bone-lining cells.
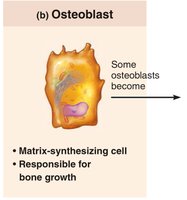
Osteoblasts: Bone-forming cells; secrete osteoid (collagen and calcium-binding proteins).
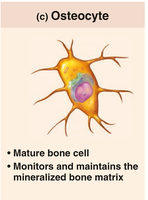
Osteocytes: Mature bone cells in lacunae; maintain bone matrix and act as mechanosensors.
Bone-lining cells: Flat cells on bone surfaces; help maintain matrix.
Osteoclasts: Multinucleate cells; resorb bone matrix.
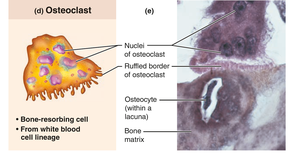
Compact Bone (Lamellar Bone)
Osteon (Haversian system): Structural unit; concentric lamellae around a central canal.
Canals and canaliculi: Central canal contains blood vessels and nerves; canaliculi connect lacunae for nutrient/waste exchange.
Interstitial and circumferential lamellae: Fill gaps and encircle the diaphysis, respectively.
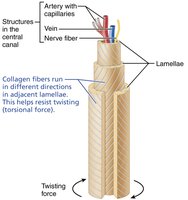
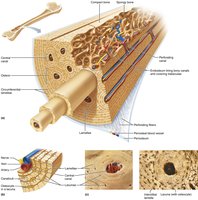
Spongy Bone
Composed of trabeculae aligned along lines of stress.
No osteons; contains irregularly arranged lamellae and osteocytes connected by canaliculi.
Capillaries in endosteum supply nutrients.
Chemical Composition of Bone
Organic Components
Cells (osteogenic, osteoblasts, osteocytes, bone-lining cells, osteoclasts) and osteoid (collagen and ground substance).
Provide tensile strength and flexibility.
Inorganic Components
Hydroxyapatites (mineral salts): 65% of bone by mass; mainly calcium phosphate crystals.
Responsible for hardness and resistance to compression.
Bone Development (Ossification)
Overview
Ossification (osteogenesis): Process of bone tissue formation.
Begins in the embryo (month 2); continues through childhood and adolescence.
Endochondral Ossification
Bone forms by replacing hyaline cartilage (endochondral bones).
Forms most of the skeleton (except clavicles and some skull bones).
Five main steps: bone collar formation, cartilage calcification, periosteal bud invasion, diaphysis elongation, epiphyses ossification.
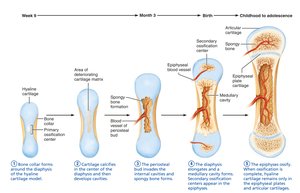
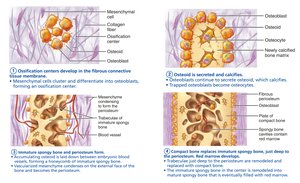
Intramembranous Ossification
Bone develops from fibrous membrane (membrane bones).
Forms cranial bones and clavicles.
Four steps: ossification center formation, osteoid secretion and calcification, woven bone formation, lamellar bone and red marrow appearance.
Postnatal Bone Growth
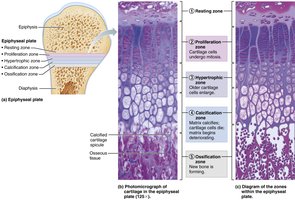
Growth in Length (Interstitial Growth)
Occurs at the epiphyseal plate; involves five zones: resting, proliferation, hypertrophic, calcification, ossification.
Epiphyseal plate closure marks the end of longitudinal growth (females ~18, males ~21).
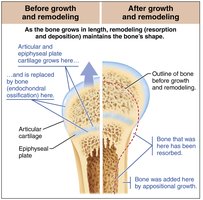
Growth in Width (Appositional Growth)
Bones thicken in response to stress; osteoblasts add bone matrix externally, osteoclasts remove it internally.
Usually more bone is built than removed, resulting in stronger bones.
Hormonal Regulation of Bone Growth
Growth hormone: Stimulates epiphyseal plate activity.
Thyroid hormone: Modulates growth hormone effects.
Sex hormones: Promote growth spurts and epiphyseal plate closure.
Bone Remodeling
Overview
Bone remodeling is a continuous process involving bone deposit (by osteoblasts) and resorption (by osteoclasts).
Remodeling units coordinate the process at periosteal and endosteal surfaces.
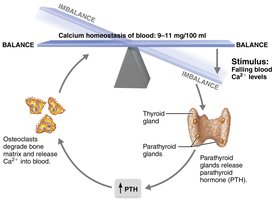
Control of Remodeling
Hormonal controls: Parathyroid hormone (PTH) increases blood calcium by stimulating osteoclasts; calcitonin lowers blood calcium at high doses.
Mechanical stress: Wolff’s law states that bone grows/remodels in response to mechanical demands.
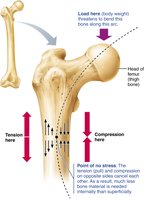
Bone Repair
Fracture Classification
Position: Nondisplaced (normal alignment) vs. displaced (misaligned).
Completeness: Complete (all the way through) vs. incomplete.
Skin penetration: Open (compound) vs. closed (simple).
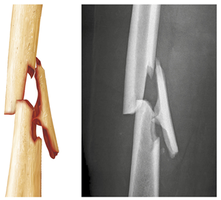
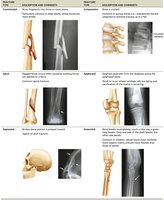
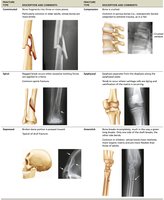
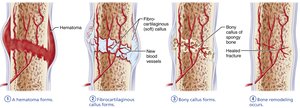
Fracture Repair
Four stages: hematoma formation, fibrocartilaginous callus formation, bony callus formation, bone remodeling.
Bone Disorders
Osteomalacia and Rickets
Osteomalacia: Poor mineralization in adults; soft, weak bones.
Rickets: Osteomalacia in children; bone deformities due to vitamin D or calcium deficiency.
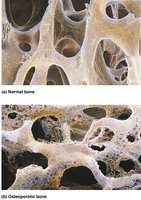
Osteoporosis
Bone resorption exceeds deposit; bone mass declines, especially in spongy bone of spine and femur neck.
Risk factors: age, postmenopausal females, low exercise, poor diet, smoking, genetics, hormone imbalances.
Treatments: calcium, vitamin D, exercise, hormone therapy, bisphosphonates, denosumab.
Prevention: adequate calcium, reduced alcohol/soda, weight-bearing exercise.
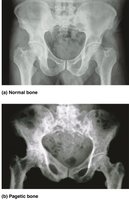
Paget’s Disease
Excessive, disorganized bone remodeling; high ratio of spongy to compact bone.
Common in spine, pelvis, femur, skull; cause unknown, possibly viral.
Treatment: bisphosphonates, calcitonin.
Developmental and Age-Related Aspects of Bone
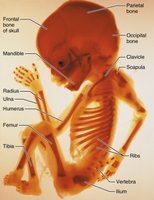
Embryonic and Fetal Development
Skeleton ossifies predictably; fetal age can be determined by ossification centers.
Most long bones begin ossifying by 8 weeks; primary centers by week 12.
Birth to Adulthood and Aging
At birth, most long bones are ossified except at epiphyses; epiphyseal plates persist through adolescence.
By age 25, all bones are completely ossified.
Bone formation exceeds resorption in youth, is balanced in young adults, and resorption exceeds formation in older adults.
Bone mass and healing ability decrease with age, especially in females and individuals with certain genetic backgrounds.
