 Back
BackChapter 21: The Immune System – Innate and Adaptive Body Defenses
Study Guide - Smart Notes

Immune System Overview
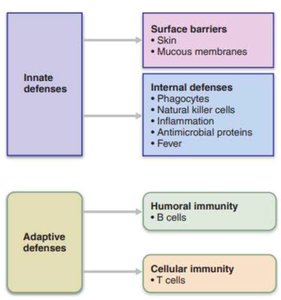
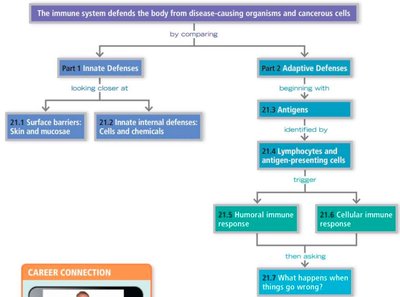
The immune system is responsible for defending the body against disease-causing organisms and cancerous cells. It achieves this through two main defense systems: innate (nonspecific) defenses and adaptive (specific) defenses. These systems work together to provide immunity, or resistance to disease.
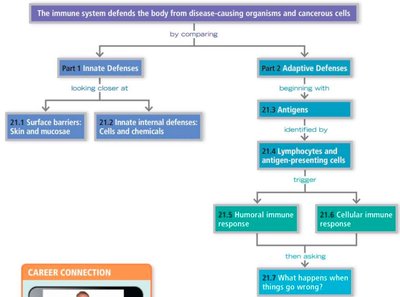
Innate (Nonspecific) Defenses
First Line of Defense: Surface Barriers
The first line of defense consists of physical and chemical barriers that prevent pathogens from entering the body.
Skin: Acts as a physical barrier with keratinized cells and produces protective chemicals (acids, enzymes like lysozyme).
Mucous membranes: Trap microbes and debris; secretions (e.g., stomach acid) destroy pathogens.
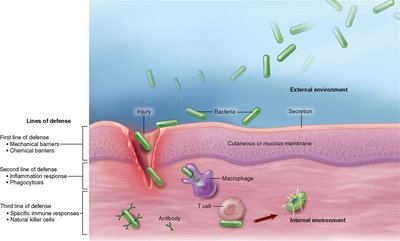
Second Line of Defense: Internal Defenses
If pathogens breach surface barriers, the body relies on internal defenses, including cellular and chemical mechanisms.
Phagocytes: Cells that engulf and digest pathogens (e.g., neutrophils, eosinophils, macrophages).
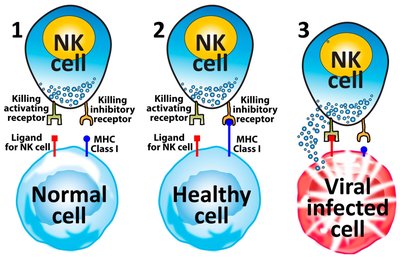
Natural Killer (NK) Cells: Detect and destroy virus-infected or cancerous cells by recognizing the absence of MHC class I molecules.
Inflammation: Local tissue response to injury, characterized by redness, heat, swelling, pain, and loss of function. Inflammatory chemicals (histamine, prostaglandins, cytokines) recruit immune cells and promote healing.
Fever: Systemic increase in body temperature triggered by pyrogens released from macrophages, which inhibits bacterial growth and enhances immune function.
Antimicrobial Proteins: Interferons (produced by virus-infected cells) alert neighboring cells and activate antiviral mechanisms; complement proteins tag microbes, trigger inflammation, and form membrane attack complexes to lyse bacteria.
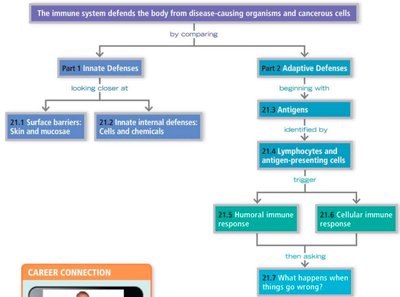

Adaptive (Specific) Defenses
The adaptive immune system is slower to respond but highly specific, targeting unique antigens. It is divided into humoral immunity (B cells and antibodies) and cell-mediated immunity (T cells).
Antigens
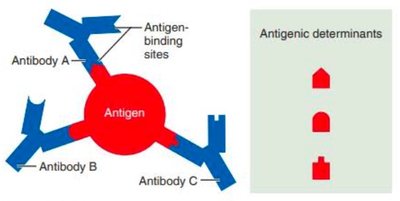
Antigens are foreign substances that trigger an adaptive immune response. They possess multiple antigenic determinants (epitopes) to which antibodies or lymphocyte receptors can bind. The immune system distinguishes self from non-self using MHC proteins on cell surfaces.
MHC Self-Antigens
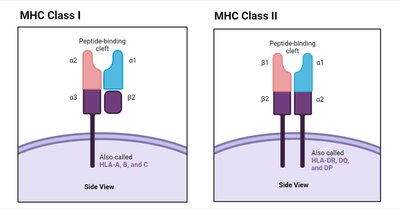
Major Histocompatibility Complex (MHC) proteins are unique to each individual and allow the immune system to recognize self-cells. There are two classes:
MHC Class I: Found on all nucleated cells; present antigens to CD8+ T cells.
MHC Class II: Found on antigen-presenting cells (APCs) such as dendritic cells, macrophages, and B cells; present antigens to CD4+ T cells.
Lymphocyte Development and Maturation
Lymphocytes are divided into B cells (mature in bone marrow) and T cells (mature in thymus). Maturation involves two key processes:
Immunocompetence: Ability to recognize and bind specific antigens.
Self-tolerance: Ability to avoid attacking self-antigens.
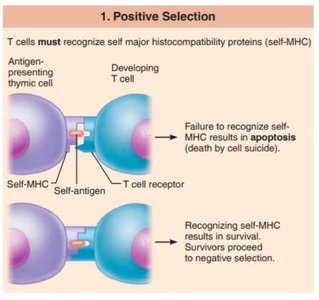
Selection of T-Lymphocytes
Positive Selection: T cells must recognize self-MHC proteins to survive; failure leads to apoptosis.
Negative Selection: T cells that bind too strongly to self-antigens are eliminated to prevent autoimmunity.
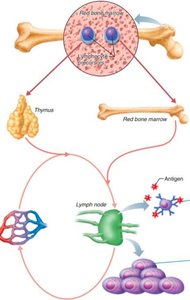
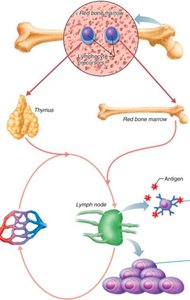
Lymphocyte Activation
Naïve B and T cells circulate to secondary lymphoid organs (e.g., lymph nodes), where they become activated upon encountering their specific antigen. Activation leads to proliferation into effector cells (combat infection) and memory cells (provide long-term immunity).

Antigen Presenting Cells (APCs)
APCs (dendritic cells, macrophages, B cells) engulf antigens and present fragments on MHC molecules to activate naïve T cells. This is essential for initiating adaptive immune responses.
B-Cell Mediated (Humoral) Immunity
B cells and antibodies mediate humoral immunity, targeting pathogens in body fluids. The process involves:
Activation: Antigen binds to B cell receptor, activating the B cell.
Clonal Selection: Activated B cell proliferates into plasma cells (secrete antibodies) and memory B cells.
Re-exposure: Memory B cells respond rapidly to subsequent exposures, forming the basis for vaccinations.
Antibodies (Immunoglobulins)
Antibodies are Y-shaped proteins with variable (V) regions for antigen binding and constant (C) regions that determine class. There are five main classes (IgG, IgM, IgA, IgD, IgE), each with distinct roles.
IgG: Most abundant, crosses placenta, triggers complement.
IgM: First produced, large, stays in circulation.
IgA: Found in secretions (sweat, breast milk).
IgD: Surface receptor on B cells.
IgE: Binds to basophils/mast cells, causes allergies.
Antibodies inactivate antigens by:
Complement fixation: Triggers lysis of pathogens.
Neutralization: Blocks harmful effects of toxins/viruses.
Agglutination: Clumps pathogens for easier removal.
Precipitation: Forms insoluble complexes for phagocytosis.
T-Cell Mediated (Cellular) Immunity
T cells mediate cellular immunity by directly attacking infected or abnormal cells. There are two main types:
CD4 (Helper) T cells: Activate B cells, CD8 T cells, and macrophages; coordinate immune response.
CD8 (Cytotoxic) T cells: Destroy infected, cancerous, or foreign cells by recognizing antigens on MHC class I proteins.
Activation of T Cells
CD8 T cells recognize antigens on MHC class I proteins (all nucleated cells).
CD4 T cells recognize antigens on MHC class II proteins (APCs only).
Full activation requires antigen recognition and co-stimulatory signals.
Immune System Disorders
Hypersensitivities
Hypersensitivities occur when the immune system damages tissue in response to harmless substances (e.g., pollen, dander). Allergies are immediate hypersensitivities mediated by IgE antibodies, mast cells, and histamine release.
Immunodeficiencies
Immunodeficiencies are conditions where immune cell function is impaired. Examples include:
SCID: Congenital, affects both B and T cells.
AIDS: Acquired, destroys CD4 T cells, crippling adaptive immunity.
Autoimmune Diseases
Autoimmune diseases result from failure of self-tolerance, causing the immune system to attack self-tissues. Examples include multiple sclerosis, type 1 diabetes (CD8+ T cells), and lupus (B cells, autoantibodies). Treatments may involve blocking cytokines or co-stimulatory molecules.
Additional info: This guide expands on the original notes with definitions, mechanisms, and clinical relevance for each immune component, and includes only images that directly reinforce the described concepts.
