 Back
BackChapter 23: The Digestive System – Structure, Function, and Regulation
Study Guide - Smart Notes

The Digestive System: Overview and Major Processes
Introduction to the Digestive System
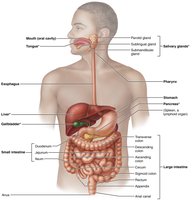
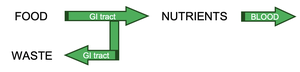
The digestive system is responsible for breaking down food into nutrients, which are then absorbed into the blood to provide energy for cellular processes. It consists of the alimentary canal (gastrointestinal tract) and accessory digestive organs.
Alimentary canal (GI tract): A continuous muscular tube that runs from the mouth to the anus, including the mouth, pharynx, esophagus, stomach, small intestine, and large intestine.
Accessory digestive organs: Teeth, tongue, salivary glands, liver, pancreas, and gallbladder, which assist in the digestive process.
Major Digestive Processes
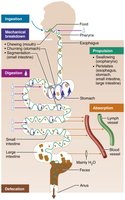
The digestive system carries out six essential activities to process food:
Ingestion: Taking food into the mouth.
Propulsion: Moving food through the GI tract, including swallowing (voluntary) and peristalsis (involuntary waves of contraction and relaxation).
Mechanical breakdown: Physically breaking food into smaller pieces to increase surface area for enzymes (chewing, mixing, churning, segmentation).
Digestion: Chemically breaking down food molecules into absorbable units by enzymes.
Absorption: Transporting digested nutrients from the GI tract lumen into the blood or lymph.
Defecation: Eliminating indigestible substances as feces.
Peristalsis and Segmentation
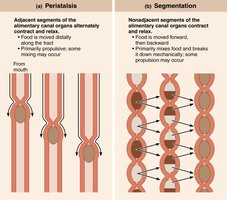
Two primary types of GI tract movements facilitate digestion and absorption:
Peristalsis: Alternating waves of contraction and relaxation that propel food distally along the tract.
Segmentation: Nonadjacent segments contract and relax, mixing food and breaking it down mechanically without significant propulsion.
Structural Organization of the GI Tract
Relationship to the Peritoneum
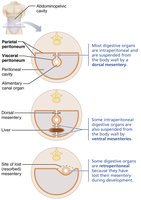
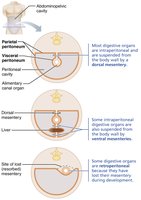
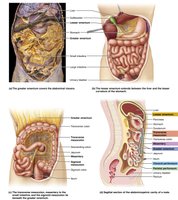
The peritoneum is a serous membrane lining the abdominopelvic cavity and covering digestive organs:
Visceral peritoneum: Covers external surfaces of most digestive organs.
Parietal peritoneum: Lines the body wall.
Peritoneal cavity: Space between the two layers, filled with lubricating serous fluid.
Mesentery: Double layer of peritoneum that supports and stabilizes digestive organs, stores fat, and provides a route for vessels and nerves.
Intraperitoneal organs: Surrounded by peritoneum and suspended by mesentery.
Retroperitoneal organs: Located posterior to the peritoneum (e.g., most of the pancreas, duodenum, parts of the large intestine).
Histology of the Alimentary Canal
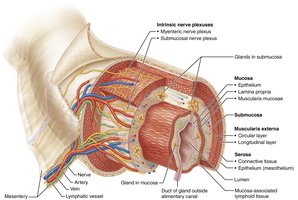
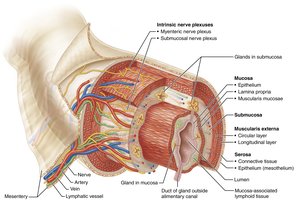
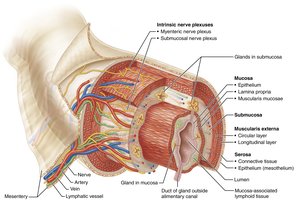
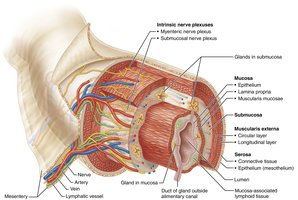
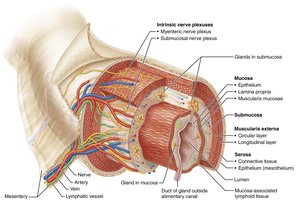
The walls of the alimentary canal share four basic layers (tunics):
Mucosa: Innermost layer; secretes mucus, digestive enzymes, and hormones; absorbs nutrients; protects against pathogens.
Submucosa: Areolar connective tissue with blood and lymphatic vessels, lymphoid follicles, and nerve fibers; allows stretch and recoil.
Muscularis externa: Responsible for segmentation and peristalsis; consists of inner circular and outer longitudinal layers of smooth muscle.
Serosa: Outermost layer (visceral peritoneum); replaced by adventitia in retroperitoneal organs.
Blood Supply and Innervation
Splanchnic Circulation
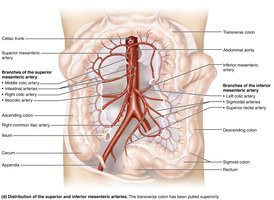
The digestive organs receive blood from branches of the abdominal aorta, collectively called splanchnic circulation:
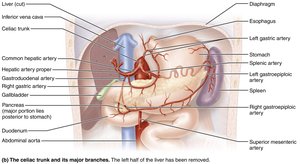
Celiac trunk: Supplies the spleen, liver, and stomach.
Superior and inferior mesenteric arteries: Supply the intestines.
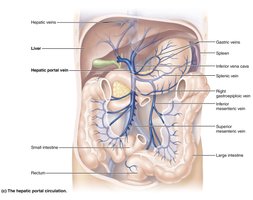
Hepatic portal circulation: Collects nutrient-rich blood from digestive organs and delivers it to the liver for processing.
Regulation of Digestive Activity
The Enteric Nervous System (ENS)
The GI tract has its own nervous system, the enteric nervous system (ENS), which regulates digestive activity independently of the central nervous system (CNS):
ENS: Contains more neurons than the spinal cord; organized into two major plexuses:
Submucosal plexus: Regulates glands and smooth muscle in the mucosa.
Myenteric plexus: Controls GI tract motility (between circular and longitudinal muscle layers).
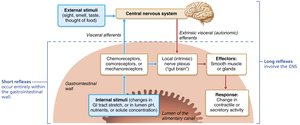
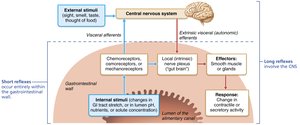
Short reflexes: Local ENS reflexes in response to stimuli within the GI tract.
Long reflexes: Involve CNS and autonomic nerves, responding to stimuli inside or outside the tract.
Parasympathetic input: Stimulates digestive activity; sympathetic input: inhibits it.
Regulation by Receptors and Effectors
Digestive activity is regulated by mechanical and chemical stimuli detected by receptors in the GI tract wall:
Mechanoreceptors: Detect stretch due to food in the lumen.
Chemoreceptors: Detect changes in osmolarity, pH, and the presence of substrates or end products.
Stimulation of these receptors initiates reflexes that activate or inhibit smooth muscle and glands, mixing and moving contents or altering secretions.
The Mouth, Pharynx, and Esophagus
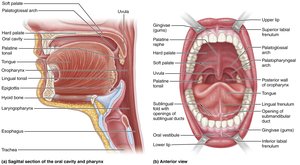
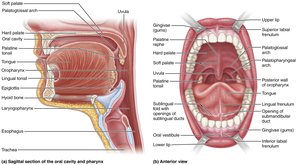
The Mouth (Oral Cavity)
The mouth is the entry point for food, where mechanical and chemical digestion begins:
Boundaries: Lips (anterior), cheeks (lateral), palate (superior), tongue (inferior).
Oral orifice: Anterior opening of the mouth.
Associated organs: Tongue, salivary glands, teeth.
The Salivary Glands
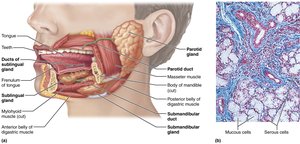
Salivary glands secrete saliva, which cleanses the mouth, dissolves food chemicals, moistens food, and begins starch digestion via amylase.
Major glands: Parotid (anterior to ear), submandibular (medial to mandible), sublingual (under tongue).
Saliva composition: 97–99.5% water, slightly acidic, contains electrolytes, amylase, lipase, mucin, lysozyme, IgA, and metabolic wastes.
Control: Primarily parasympathetic; chemoreceptors and mechanoreceptors in the mouth stimulate salivatory nuclei in the brainstem.
The Teeth and Mastication
Teeth are housed in sockets (alveoli) and are essential for mastication (chewing), which mechanically breaks food into smaller pieces.
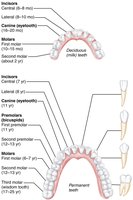
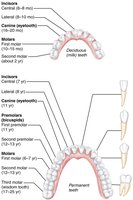
Deciduous teeth: 20 primary teeth, erupt between 6–24 months.
Permanent teeth: 32 teeth, replace primary teeth between ages 6–12 years.
Types: Incisors (cutting), canines (tearing), premolars and molars (grinding).
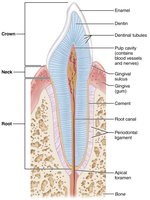
Structure: Crown (covered by enamel), neck, root (embedded in jawbone).
Digestive Processes in the Mouth
The mouth and its accessory organs are involved in four digestive processes:
Ingestion
Mechanical breakdown (mastication)
Propulsion (swallowing)
Digestion of polysaccharides (via salivary amylase)
The Pharynx and Esophagus
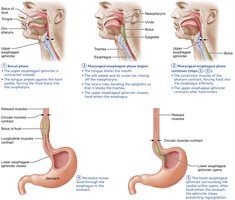
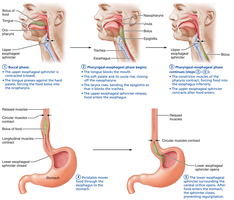
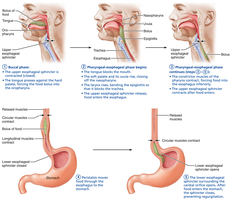
The pharynx and esophagus transport food from the mouth to the stomach by coordinated muscle contractions (deglutition or swallowing):
Pharynx: Passageway for food, fluids, and air; lined with stratified squamous epithelium.
Esophagus: Muscular tube connecting pharynx to stomach; propels food via peristalsis.
Swallowing phases: Buccal phase (voluntary, tongue pushes bolus into pharynx), pharyngeal-esophageal phase (involuntary, controlled by medulla and pons, food moves to stomach).
The Stomach: Structure and Function
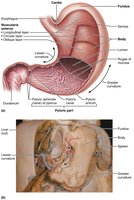
Gross Anatomy of the Stomach
The stomach is a temporary storage tank that continues the breakdown of food, producing chyme for delivery to the small intestine.
Regions: Cardia, fundus, body, pyloric part (antrum, canal, pylorus).
Pyloric sphincter: Controls stomach emptying into the duodenum.
Rugae: Folds in the mucosa and submucosa that allow expansion.
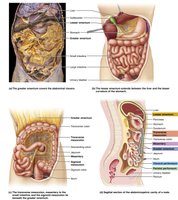
Curvatures: Greater (lateral) and lesser (medial).
Omenta: Mesenteries tethering the stomach to other organs (lesser and greater omentum).
Microscopic Anatomy of the Stomach
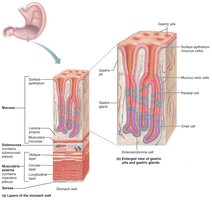
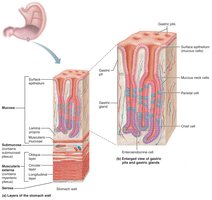
The stomach wall contains the four basic tunics, with modifications:
Muscularis externa: Has an additional oblique layer for enhanced churning and mixing.
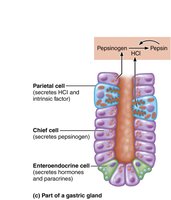
Mucosa: Simple columnar epithelium with mucous cells; contains gastric pits leading to gastric glands.
Gland cells:
Mucous neck cells: Secrete thin, acidic mucus.
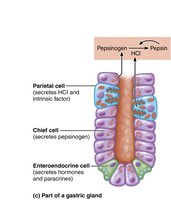
Parietal cells: Secrete hydrochloric acid (HCl) and intrinsic factor (for vitamin B12 absorption).
Chief cells: Secrete pepsinogen (activated to pepsin by HCl) and gastric lipase.
Enteroendocrine cells: Secrete hormones and paracrines (e.g., gastrin, histamine, serotonin, somatostatin).
Mucosal barrier: Protects stomach from self-digestion via a thick mucus layer, tight junctions, and rapid cell turnover.
Digestive Processes in the Stomach
The stomach performs several key digestive functions:
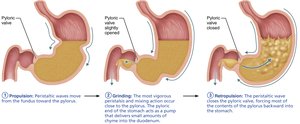
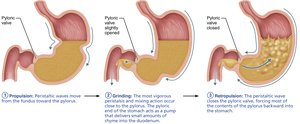
Propulsion: Peristaltic waves move food toward the pylorus.
Mechanical breakdown: Churning action mixes food with gastric juice.
Chemical digestion: HCl denatures proteins; pepsin digests proteins; gastric lipase digests fats (minor role).
Absorption: Limited to lipid-soluble substances (e.g., alcohol, aspirin).
Essential function: Secretion of intrinsic factor for vitamin B12 absorption (required for red blood cell maturation).
Regulation of Gastric Secretion and Motility
Gastric secretion is regulated by neural and hormonal mechanisms:
Neural: Long (vagus nerve) and short (ENS) reflexes stimulate secretion; sympathetic input inhibits it.
Hormonal: Gastrin stimulates HCl secretion; enterogastrones from the small intestine inhibit it.
Phases of secretion: Cephalic (before food enters), gastric (food in stomach), intestinal (chyme in duodenum).
Motility: Stomach stretches to accommodate food; peristaltic waves mix and propel chyme; only small particles pass through the pyloric sphincter.
Regulation of emptying: Duodenum controls rate of gastric emptying via enterogastric reflex and hormones.
Summary Table: Layers of the Alimentary Canal
Layer | Main Components | Functions |
|---|---|---|
Mucosa | Epithelium, lamina propria, muscularis mucosae | Secretion, absorption, protection |
Submucosa | Areolar connective tissue, blood/lymph vessels, nerves | Support, elasticity, vascular supply |
Muscularis externa | Inner circular and outer longitudinal smooth muscle | Segmentation, peristalsis |
Serosa | Areolar connective tissue, mesothelium | Protection, reduces friction |
Additional info: The notes above cover the first half of Chapter 23, focusing on the structure and function of the digestive system up to the stomach, as outlined in the provided lecture plan. For exam preparation, students should also review the regulation of digestive processes, the roles of accessory organs, and the continuation of digestion and absorption in the small and large intestines.
