 Back
BackDigestive System: Structure, Function, and Regulation
Study Guide - Smart Notes

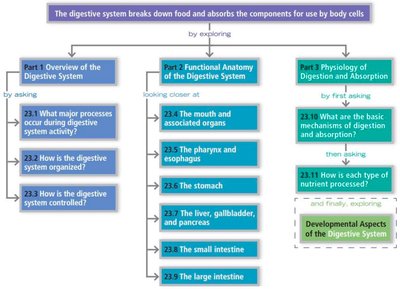
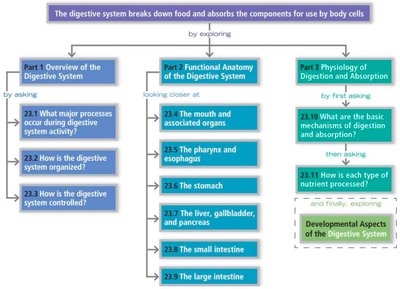
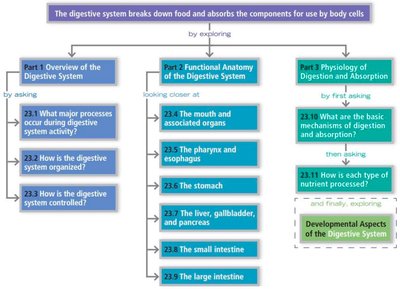
Digestive System Overview
Introduction to the Digestive System
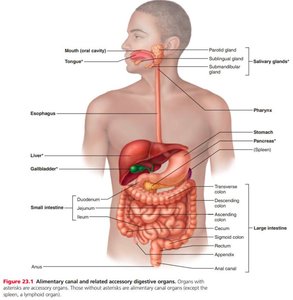
The digestive system is responsible for the intake, breakdown, absorption, and elimination of food and nutrients. It is anatomically located within the abdominopelvic cavity and consists of the alimentary canal and accessory digestive organs. The system ensures that nutrients are absorbed into the bloodstream and indigestible remains are expelled from the body.
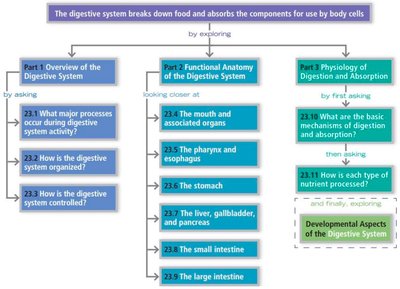
Major Processes of the Digestive System
Ingestion: Taking food into the digestive tract (eating).
Propulsion: Moving food through the alimentary canal via peristalsis (rhythmic contractions).
Mechanical Breakdown: Chewing, mixing, and segmentation to increase surface area for enzymes.
Digestion: Chemical breakdown of food into absorbable molecules by digestive enzymes.
Absorption: Passage of digested nutrients from the GI tract into blood or lymph.
Defecation: Elimination of indigestible substances as feces.
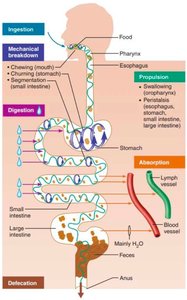
Anatomical Organization of the Digestive System
Divisions of the Digestive System
Digestive Tract Organs (Alimentary Canal): Continuous tube from mouth to anus (oral cavity, pharynx, esophagus, stomach, small intestine, large intestine, anus).
Accessory Digestive Organs: Aid digestion by producing or storing substances (liver, gallbladder, pancreas).
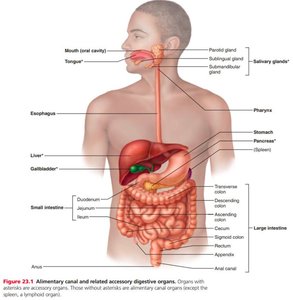
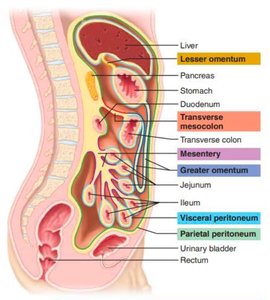
The Peritoneum and Mesenteries
The peritoneum is a thin, shiny membrane lining the abdominal cavity and covering digestive organs. It consists of:
Parietal peritoneum: Lines the abdominal wall.
Visceral peritoneum: Covers the organs.
Mesenteries are double folds of peritoneum that anchor organs to the abdominal wall and provide pathways for blood vessels, nerves, and lymphatics.
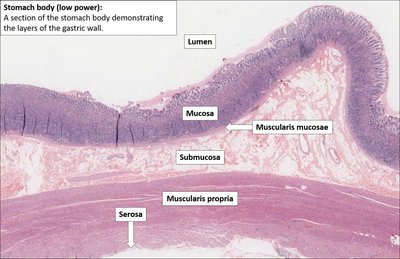
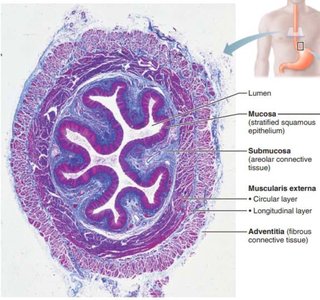
Histological Structure of the Alimentary Canal
Four Main Layers
Mucosa: Innermost layer; epithelium specialized for protection, absorption, and secretion.
Submucosa: Connective tissue containing blood vessels, nerves (Meissner’s plexus), and glands.
Muscularis externa: Smooth muscle (inner circular and outer longitudinal layers) for motility; contains myenteric plexus.
Serosa (or Adventitia): Outermost layer; serosa reduces friction (intraperitoneal organs), adventitia anchors organs (retroperitoneal organs like the esophagus).
Summary Table: Digestive Tract Epithelia
Location | Epithelium Type | Function |
|---|---|---|
Oral cavity, pharynx, esophagus, lower anal canal | Non-keratinized stratified squamous | Protection against abrasion |
Stomach, small intestine, large intestine, rectum, upper anal canal | Non-ciliated simple columnar | Secretion and absorption |
Regulation of Digestive Activity
Control Mechanisms
Stimuli: Stretch, pH, and chemical composition activate receptors in the GI tract wall.
Effectors: Smooth muscle (motility) and glands (secretion) respond to stimuli.
Control Systems: The enteric nervous system (ENS) regulates local reflexes; the central nervous system (CNS) and hormones modulate activity via long reflexes.
Enteric Nervous System (ENS)
ENS is the "brain of the gut," capable of independent reflexes.
Two major plexuses:
Meissner’s (submucosal) plexus: Controls secretion and blood flow.
Myenteric plexus: Controls motility (peristalsis).
Autonomic Nervous System Influence
Parasympathetic: Stimulates digestion (increases motility and secretion).
Sympathetic: Inhibits digestion (decreases motility and secretion).
Functional Anatomy of the Digestive System
Mouth (Oral Cavity) and Associated Structures
The oral cavity is the entry point for food and the site of mechanical and chemical digestion. Structures include lips, cheeks, palate, tongue, and teeth.
Mechanical digestion: Chewing (mastication) by teeth.
Chemical digestion: Salivary amylase begins starch breakdown.
Formation of bolus: Food mixed with saliva and shaped by the tongue.
Teeth
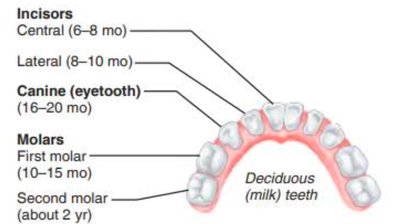
Deciduous teeth: Erupt between 6–24 months.
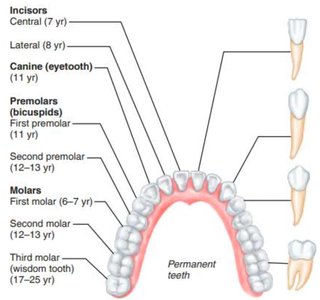
Permanent teeth: Replace deciduous teeth between 6–12 years.
Types: Incisors (cutting), canines (tearing), premolars and molars (grinding).
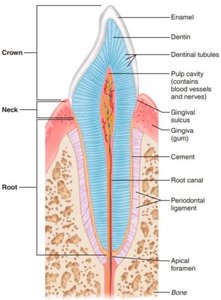
Structure: Crown (enamel), neck (gingiva), root (cementum, periodontal ligament).
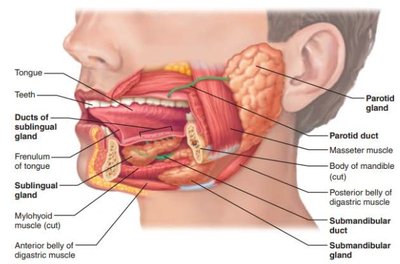
Salivary Glands
Parotid, submandibular, sublingual glands produce saliva containing amylase, lysozyme, mucus, and IgA.
Saliva moistens food, begins starch digestion, and protects oral cavity.
Regulated by parasympathetic nervous system (CN VII, IX).
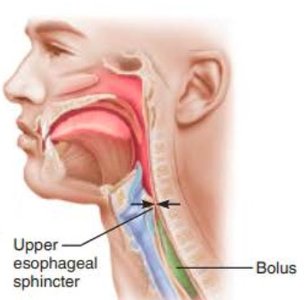
Pharynx and Esophagus
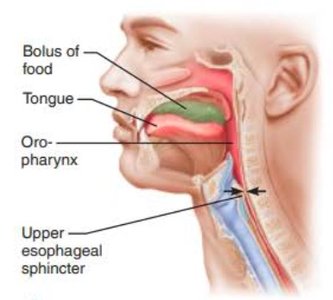
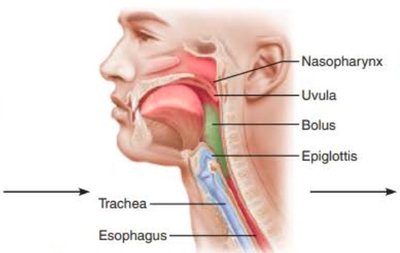
Food passes from mouth to pharynx, then esophagus.
Swallowing involves three phases: buccal (voluntary), pharyngeal (involuntary), esophageal (involuntary).
Peristalsis moves bolus to stomach; lower esophageal sphincter regulates entry.
Stomach
Receives food, mixes it with gastric juice to form chyme.
Regions: cardia, body, pyloric region (ends at pyloric sphincter).
Rugae (folds) allow expansion and aid mechanical digestion.
Stomach Wall Structure
Mucosa: Simple columnar epithelium, secretes mucus, acid, enzymes.
Muscularis externa: Three layers (longitudinal, circular, oblique) for churning.

Gastric Glands and Secretions
Mucous neck cells: Secrete acidic mucus.
Parietal cells: Secrete HCl and intrinsic factor.
Chief cells: Secrete pepsinogen and gastric lipase.
Enteroendocrine (G) cells: Secrete gastrin.
Regulation of Gastric Secretion
Cephalic phase: Triggered by sight, smell, thought of food (vagus nerve stimulation).
Gastric phase: Triggered by food in stomach (stretch and chemoreceptors, gastrin release).
Intestinal phase: Triggered by chyme in duodenum; initially stimulates, then inhibits gastric activity (via secretin and CCK).
Stomach Protection and Absorption
Protection: Rapid epithelial turnover, zymogen secretion, tight junctions, bicarbonate-rich mucus.
Absorption: Limited to water, electrolytes, alcohol, and some drugs (e.g., aspirin).
Accessory Digestive Organs
Liver
Synthesis: Produces bile, heparin, and contributes to vitamin D metabolism.
Detoxification: Metabolizes drugs/toxins, breaks down old RBCs (produces bilirubin).
Storage: Stores fat-soluble vitamins and glycogen.
Liver Microanatomy
Liver lobules: Functional units containing hepatocytes (detoxification, bile synthesis), Kupffer cells (macrophages), and a central vein.
Portal triad: Bile duct, branch of portal vein, branch of hepatic artery.
Bile Flow
Bile flows from hepatocytes → bile canaliculi → bile ductules → right/left hepatic ducts → common hepatic duct → (joins cystic duct) → common bile duct → duodenum (regulated by hepatopancreatic sphincter).
Gallbladder
Stores and concentrates bile; releases bile into duodenum in response to CCK.
Cystic duct allows two-way flow (storage and release).
Pancreas
Exocrine function: Acinar cells produce pancreatic juice (enzymes and bicarbonate) for digestion.
Endocrine function: Islets of Langerhans secrete insulin, glucagon, somatostatin (blood glucose regulation).
Pancreatic Juice Components
Proteases: Trypsinogen (activated to trypsin), chymotrypsinogen, etc.
Amylase: Digests starch.
Lipases: Digest fats (aided by bile).
Nucleases: Digest nucleic acids.
Bicarbonate: Neutralizes acidic chyme.
Small Intestine
Function and Structure
Major site of digestion and absorption.
Highly folded (circular folds, villi, microvilli) to maximize surface area.
Divided into duodenum (mixing, neutralization), jejunum (absorption), ileum (absorption, ends at ileocecal valve).
Microanatomy and Cell Types
Enterocytes: Absorptive cells with brush border enzymes.
Goblet cells: Secrete mucus.
Enteroendocrine cells: Secrete CCK and secretin.
Paneth cells: Secrete lysozyme (antimicrobial).
Stem cells: Regenerate epithelium.
Submucosal Specializations
Peyer’s patches: Lymphoid tissue for immune defense.
Duodenal glands: Secrete alkaline mucus to neutralize acid.
Large Intestine
Function and Anatomy
Reabsorbs water and electrolytes; forms and expels feces.
Divided into cecum, colon (ascending, transverse, descending, sigmoid), rectum, and anal canal.
Anal canal contains internal (involuntary) and external (voluntary) sphincters.
Histological Specializations
Lined with simple columnar epithelium (except lower anal canal).
Teniae coli: Three longitudinal muscle bands segment colon into haustra.
Haustra: Pouch-like segments for mixing and moving contents.
Defecation Reflex
Triggered by rectal wall distention (parasympathetic reflex).
Internal sphincter relaxes (involuntary), external sphincter allows voluntary control of defecation.
Gut Microbiota
Large intestine harbors beneficial bacteria that ferment indigestible carbohydrates and synthesize vitamins B and K.
Helps suppress harmful bacteria and maintain gut health.
