 Back
BackFluid, Electrolyte, and Acid-Base Homeostasis: Study Notes
Study Guide - Smart Notes

Fluid, Electrolyte, and Acid-Base Homeostasis
Body Fluids and Fluid Balance
Body fluids encompass all water-based liquids in the body, including blood plasma, interstitial fluid, cytosol, cerebrospinal fluid, lymph, and exocrine secretions. Water is the main component of these fluids. Fluid balance refers to maintaining the appropriate volume and concentration of intracellular and extracellular fluids, following the principle of mass balance: what is gained must equal what is lost. Disruptions in this balance can lead to homeostatic disturbances.
Electrolytes and Nonelectrolytes
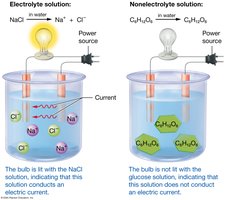
Electrolytes are compounds that dissociate into ions in water and conduct electricity, while nonelectrolytes do not dissociate and do not conduct electricity. The concentration and balance of electrolytes are crucial for physiological processes.
Electrolyte Balance: Maintained by matching intake with loss; concentration depends on water volume.
Examples: Sodium (Na+), potassium (K+), chloride (Cl-).
Acids, Bases, and pH
An acid releases hydrogen ions (H+) in water (e.g., HCl in the stomach), while a base accepts hydrogen ions (e.g., bicarbonate ion). Buffer systems resist dramatic swings in pH. The pH scale ranges from 0 (acidic) to 14 (basic), with 7 being neutral.
Total Body Water and Fluid Compartments
Total Body Water
Total body water varies by age, sex, and body composition. Adult males average about 42 liters, with women and older adults having less due to higher adipose tissue content.
Fluid Compartments: Intracellular and Extracellular Fluids
The body’s fluids are divided into intracellular fluid (ICF, about 60%) and extracellular fluid (ECF, about 40%). ECF includes plasma (8%) and interstitial fluid (32%).
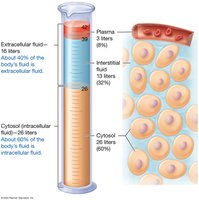
Solute composition differs between compartments: ECF is higher in sodium, chloride, calcium, and bicarbonate, while ICF is higher in potassium, magnesium, sulfate, and phosphate ions.
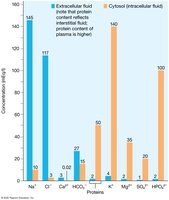
Movement of Water Between Compartments
Water moves freely between compartments, driven by hydrostatic and osmotic pressure gradients:
Hydrostatic Pressure: The force exerted by fluid; moves water from high to low pressure.
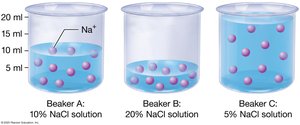
Osmotic Pressure: Determined by solute concentration (osmolarity); water moves toward higher osmolarity.
Tonicity describes the ability of a solution to cause water movement:
Isotonic: No net water movement.
Hypotonic: Cell gains water and swells.
Hypertonic: Cell loses water and shrinks (crenates).
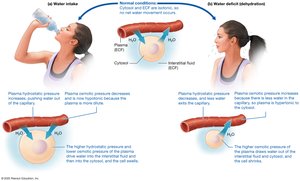
Water Losses and Gains
Water Losses
Obligatory Water Loss: Minimum urine output required to excrete solutes (~500 mL/day).
Sensible Loss: Noticeable losses via urine and feces.
Insensible Loss: Unnoticed losses via skin and respiration.
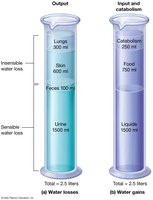
Water Gains
Metabolic Water: Produced by cellular respiration (~250 mL/day).
Food: Water content in food (~750 mL/day).
Liquids: Direct intake (~1500 mL/day).
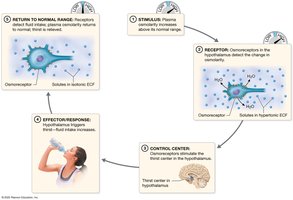
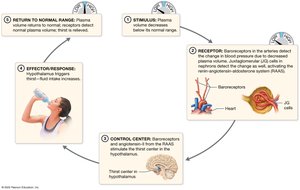
Thirst Mechanism
Controlled by osmoreceptors in the hypothalamus, which detect increased plasma osmolarity and stimulate thirst. Decreased plasma volume also triggers thirst via the renin-angiotensin-aldosterone system (RAAS).
Intravenous Fluids
IV fluids are administered directly into veins for rapid effect, used to restore fluid balance in clinical settings.
Hormonal Regulation of Fluid Balance
Antidiuretic Hormone (ADH): Increases water reabsorption in the kidneys.
Aldosterone: Increases sodium (and water) reabsorption.
Atrial Natriuretic Peptide (ANP): Decreases sodium and water reabsorption.
Angiotensin II: Stimulates thirst and aldosterone secretion.
Imbalances of Fluid Homeostasis
Dehydration
Characterized by decreased ECF volume and increased osmolarity, leading to electrolyte imbalances, dry mouth, oliguria, and potentially fatal complications if not corrected. Treated with fluids, preferably containing electrolytes and glucose.
Overhydration (Hypotonic Hydration)
Results from excessive water intake or impaired renal function, causing cells to swell and leading to hyponatremia and cerebral edema. Treated with hypertonic fluids.
Isosmotic Fluid Imbalances
Blood Loss (Hypovolemia): Proportional loss of water and solutes; treated with isotonic fluids.
Hypervolemia: Increased ECF volume, often causing edema; managed by addressing underlying causes and removing excess fluid.
Major Electrolytes
Sodium Ions (Na+)
Most abundant extracellular cation, essential for action potentials and fluid balance. Maintained by the Na+/K+ ATPase pump and hormonal regulation (RAAS, ANP).
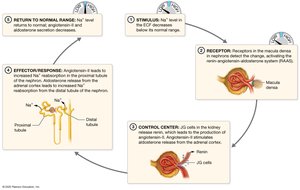
Hypernatremia: High sodium, usually due to dehydration; causes cell shrinkage.
Hyponatremia: Low sodium, often from overhydration or SIADH; causes cell swelling.
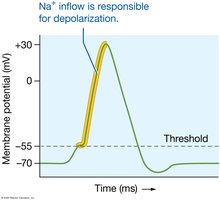
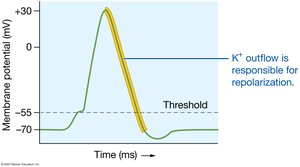
Potassium Ions (K+)
Most abundant intracellular cation, crucial for repolarization of action potentials and resting membrane potential. Regulated by aldosterone, insulin, and epinephrine.
Hyperkalemia: High potassium; can cause cardiac arrest.
Hypokalemia: Low potassium; leads to muscle weakness and arrhythmias.
Calcium and Phosphate Ions
Calcium is vital for muscle contraction, neurotransmission, and blood clotting; phosphate is important for ATP and bone structure. Both are regulated by parathyroid hormone (PTH) and vitamin D.
Hypercalcemia: Decreases neuronal activity, causes muscle weakness.
Hypocalcemia: Increases neuronal excitability, can cause tetany and spasms.
Other Ions
Chloride (Cl-): Major ECF anion, important for osmotic balance and HCl production.
Magnesium (Mg2+): Enzyme cofactor, bone structure, and can act as an osmotic laxative in excess.
Acid-Base Homeostasis
Sources of Acids and Bases
Volatile Acids: CO2 (can be exhaled).
Fixed Acids: Lactic acid, uric acid, ketones (excreted by kidneys).
Dietary Acids/Bases: Minor effect on overall pH.
Chemical Buffer Systems
Buffers resist changes in pH by binding or releasing hydrogen ions. Major buffer systems include:
Carbonic Acid–Bicarbonate Buffer: Main ECF buffer.
Phosphate Buffer: Important in cytosol and kidney tubules.
Protein Buffer: Intracellular and plasma proteins, including hemoglobin.
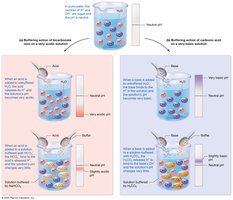
Physiological Buffer Systems
Respiratory System: Regulates CO2 (volatile acid) via ventilation.
Renal System: Excretes fixed acids and regulates bicarbonate reabsorption and hydrogen ion secretion.
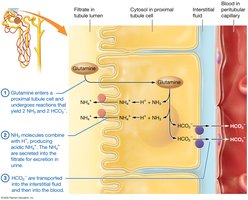
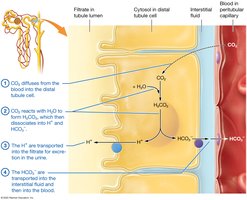
Acid-Base Imbalances
Acidosis
Defined as pH < 7.35. Causes nervous system depression. Types include:
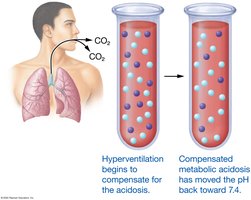
Respiratory Acidosis: Due to hypoventilation and CO2 retention.
Metabolic Acidosis: Due to excess metabolic acids or loss of bicarbonate (e.g., diarrhea, ketoacidosis).
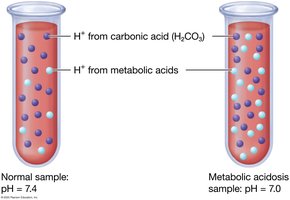
Alkalosis
Defined as pH > 7.45. Increases neuronal excitability, can cause tetany and seizures. Types include:
Respiratory Alkalosis: Due to hyperventilation and CO2 loss.
Metabolic Alkalosis: Due to loss of hydrogen ions (vomiting) or excess bicarbonate intake.
Arterial Blood Gases (ABGs)
ABGs measure blood pH, CO2, and bicarbonate to assess acid-base status. Compensation can be respiratory or renal, and may be partial or complete.
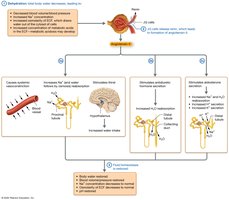
Case Study: Dehydration
Dehydration from inadequate fluid intake leads to decreased blood volume, increased ECF osmolarity, and metabolic acidosis. The body responds by activating RAAS, ADH, and aldosterone to restore fluid and electrolyte balance.
Disorder | Primary Disturbance | Compensation | Key Features |
|---|---|---|---|
Respiratory Acidosis | CO2 retention (hypoventilation) | Renal: ↑ HCO3- reabsorption | Low pH, high CO2 |
Metabolic Acidosis | ↑ Metabolic acids or ↓ HCO3- | Respiratory: hyperventilation | Low pH, low HCO3- |
Respiratory Alkalosis | CO2 loss (hyperventilation) | Renal: ↑ HCO3- excretion | High pH, low CO2 |
Metabolic Alkalosis | Loss of H+ or ↑ HCO3- | Respiratory: hypoventilation | High pH, high HCO3- |
