 Back
BackLiver, Gallbladder, and Pancreas: Structure and Function in Digestion
Study Guide - Smart Notes

Liver, Gallbladder, and Pancreas: Accessory Organs of Digestion
Overview of Accessory Organs
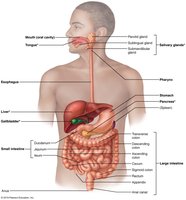
The liver, gallbladder, and pancreas are essential accessory organs associated with the small intestine (SI) and play critical roles in digestion. Each organ contributes unique functions that facilitate the breakdown and absorption of nutrients.
Liver: Produces bile, which emulsifies fats for digestion.
Gallbladder: Stores and concentrates bile, releasing it as needed.
Pancreas: Supplies digestive enzymes and bicarbonate to neutralize stomach acid.
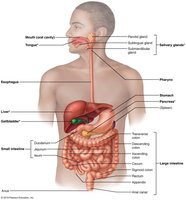
Liver: Gross Anatomy
Structure and Location
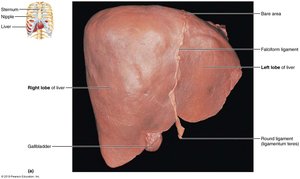
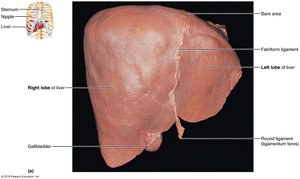
The liver is the largest gland in the human body, weighing approximately 3 pounds. It is divided into four primary lobes: right, left, caudate, and quadrate. The liver is suspended from the diaphragm and anterior abdominal wall by the falciform ligament, which separates the right and left lobes. The round ligament (ligamentum teres) is a remnant of the fetal umbilical vein.
Falciform ligament: Separates right and left lobes; suspends liver.
Round ligament: Remnant of fetal circulation.
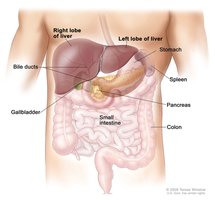
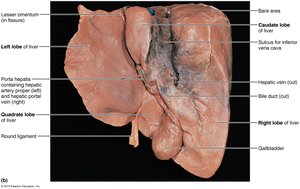
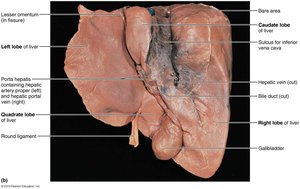
Blood Supply and Bile Ducts
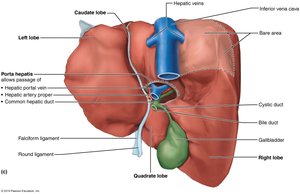
The hepatic artery and vein enter the liver at the porta hepatis. Bile ducts are organized as follows:
Common hepatic duct: Leaves the liver.
Cystic duct: Connects to the gallbladder.
Bile duct: Formed by the union of hepatic and cystic ducts.
Liver: Microscopic Anatomy
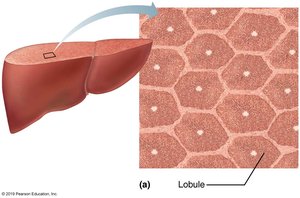
Liver Lobules and Portal Triad
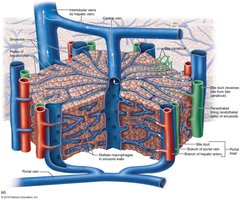
Liver lobules are hexagonal structural and functional units composed of plates of hepatocytes (liver cells). These cells filter and process nutrient-rich blood. Each lobule contains a central vein and a portal triad at each corner, which includes:
Branch of hepatic artery: Supplies oxygen.
Branch of hepatic portal vein: Brings nutrient-rich blood from the small intestine.
Bile duct: Receives bile from bile canaliculi.
Functions of Hepatocytes
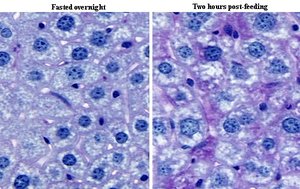
Hepatocytes are the main functional cells of the liver, performing a variety of tasks:
Bile production: ~900 ml per day.
Processing bloodborne nutrients: Includes storage of glucose as glycogen.
Plasma protein synthesis: Essential for blood clotting and transport.
Storage of fat-soluble vitamins: Vitamins A, D, E, and K.
Detoxification: Converts ammonia to urea for excretion.
Liver: Bile Composition and Circulation
Bile Composition
Bile is a yellow-green, alkaline solution containing:
Bile salts: Cholesterol derivatives that emulsify and aid in absorption of fats.
Bilirubin: Waste product from the breakdown of hemoglobin (Hb) in red blood cells.
Cholesterol, triglycerides, phospholipids, electrolytes: Additional components of bile.
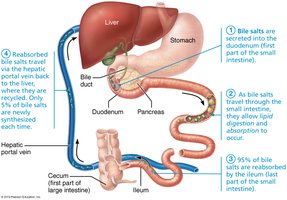
Enterohepatic Circulation
Bile salts are recycled through the enterohepatic circulation, which conserves these important molecules for continued fat digestion.
Liver: Pathology
Hepatitis and Cirrhosis
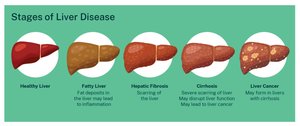
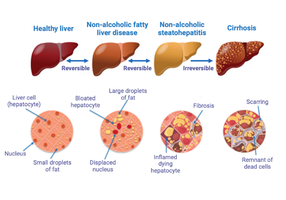
Hepatitis is inflammation of the liver, most commonly caused by viral infection, drug toxicity, or wild mushroom poisoning. Cirrhosis is a progressive, chronic inflammation resulting from chronic hepatitis or alcoholism, leading to impaired liver function.
Gallbladder: Structure and Function
Gallbladder Anatomy and Physiology
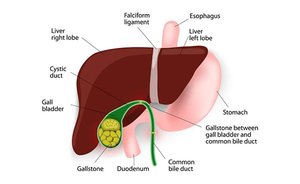
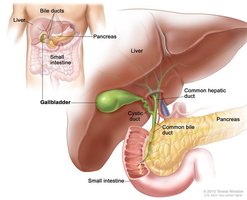
The gallbladder is a thin-walled muscular sac that stores and concentrates bile by absorbing water and ions. Muscular contractions release bile via the cystic duct, which then flows into the bile duct and ultimately into the small intestine.
Gallstones
Gallstones are caused by excessive cholesterol or insufficient bile salts, leading to obstruction of bile flow and pain during gallbladder contraction.

Pancreas: Structure and Function
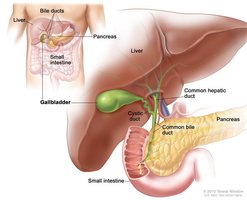
Pancreatic Anatomy and Functions
The pancreas is located deep to the greater curvature of the stomach. It has both exocrine and endocrine functions:
Exocrine: Produces pancreatic juice via acinar cells, which contain inactive digestive enzymes (proenzymes). Ducts transport these secretions to the duodenum. Small duct cells produce water and bicarbonate.
Endocrine: Secretes insulin and glucagon from pancreatic islet cells, regulating blood glucose.
Composition of Pancreatic Juice
Pancreatic juice is a watery, alkaline solution (pH 8) that neutralizes chyme from the stomach. It contains:
Electrolytes: Especially bicarbonate (HCO3-).
Digestive enzymes: Proteases (for proteins), amylase (for carbohydrates), lipases (for lipids), nucleases (for nucleic acids).
Proteases are secreted in inactive form and activated in the duodenum.
Bile and Pancreatic Secretion into the Small Intestine
Anatomy of Ducts and Regulation
The bile duct and pancreatic duct unite in the wall of the duodenum, forming the hepatopancreatic ampulla, which opens into the duodenum via the major duodenal papilla. The hepatopancreatic sphincter controls entry of bile and pancreatic juice. An accessory pancreatic duct empties directly into the duodenum.
Regulation of Secretion
Bile and pancreatic secretions are regulated by neural and hormonal controls. Key hormones include:
Cholecystokinin (CCK): Stimulates release of bile and pancreatic juice.
Secretin: Stimulates secretion of bicarbonate-rich pancreatic juice.
Summary Table: Functions of Liver, Gallbladder, and Pancreas
Organ | Main Function | Key Products |
|---|---|---|
Liver | Bile production, metabolism, detoxification | Bile, plasma proteins, glycogen |
Gallbladder | Bile storage and concentration | Concentrated bile |
Pancreas | Digestive enzyme and hormone secretion | Pancreatic juice, insulin, glucagon |
Key Equations
Bicarbonate neutralization:
Conversion of ammonia to urea (detoxification):
Additional info: The notes have been expanded to include definitions, examples, and academic context for each organ and process. All images included are directly relevant to the anatomical and physiological explanations provided.
