 Back
BackLymphatic System and Immunity: Structured Study Notes
Study Guide - Smart Notes

Lymphatic System and Immunity
Introduction to the Lymphatic System
The lymphatic system is a secondary circulatory system that plays a crucial role in maintaining fluid balance and defending the body against disease. Lymphatic vessels collect excess tissue fluid from interstitial spaces and return it to the blood, while specialized vessels called lacteals transport absorbed fats. Lymph nodes, located along these vessels, contain lymphocytes that help protect the body from pathogens.
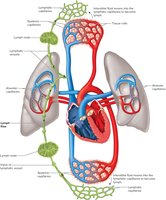
Lymphatic Pathways
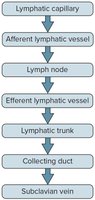
Lymphatic pathways begin as lymphatic capillaries, which merge to form larger vessels and trunks, eventually emptying into veins in the thoracic cavity. Lymphatic capillaries are tiny, closed-ended vessels found throughout the body except in the central nervous system. They receive tissue fluid through thin walls and slits between cells; once inside, the fluid is called lymph.
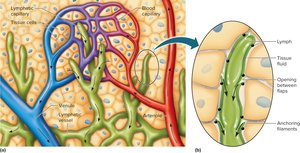
Lymphatic Vessels
Thinner walls than veins, but constructed with the same three layers.
Contain flap-like valves to prevent backflow.
Pass through lymph nodes and merge to form lymphatic trunks.
Lymphatic Trunks and Collecting Ducts
Lymphatic trunks drain lymph from vessels and are named for the regions they drain.
Collecting ducts: The right lymphatic duct drains the right side of the head, neck, arm, and thorax; the thoracic duct drains the rest of the body.
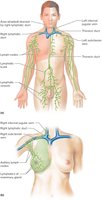
Tissue Fluid and Lymph
Lymph is tissue fluid that has entered a lymphatic capillary. Its formation depends on tissue fluid formation, which occurs when water and dissolved substances leave blood capillaries by filtration and diffusion. Most fluid returns to capillaries due to plasma colloid osmotic pressure, but some becomes tissue fluid and enters lymphatic capillaries.
Lymph transports foreign particles, including bacteria and viruses, to lymph nodes for recognition and destruction.
Lymph Movement
Driven by hydrostatic pressure of tissue fluid.
Muscular activity (skeletal muscle contraction, breathing, smooth muscle contraction) moves lymph.
Valves prevent backflow.
Edema: Accumulation of lymph in interstitial spaces due to interference with lymph flow.
Lymphatic Tissues and Organs
Lymphatic tissue contains lymphocytes, macrophages, and other cells. Unencapsulated lymphatic tissue associated with mucous membranes is called MALT (mucosa-associated lymphoid tissue). Tonsils, appendix, and Peyer's patches are compact masses of lymphatic nodules. Encapsulated lymphatic organs include lymph nodes, thymus, and spleen.
Lymph Nodes
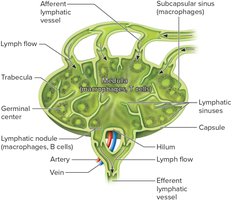
Lymph nodes are bean-shaped structures located in groups or chains along lymphatic vessels. They filter lymph, removing pathogens, and contain both lymphocytes and macrophages.
Blood vessels, nerves, and efferent lymphatic vessels enter/exit at the hilum.
Afferent lymphatic vessels enter on the convex surface.
Connective tissue capsule divides the node into nodules and sinuses.
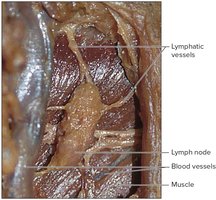
Locations of Lymph Nodes
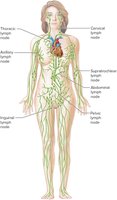
Occur in chains along larger lymphatic vessels.
Major concentrations: cervical, thoracic, axillary, supratrochlear, abdominal, pelvic, and inguinal regions.
Functions of Lymph Nodes
Filter lymph and remove bacteria and debris.
Immune surveillance by lymphocytes and macrophages.
Centers of lymphocyte production.
Lymphocytes attack pathogens; macrophages engulf and destroy foreign particles.
Thymus
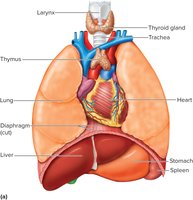
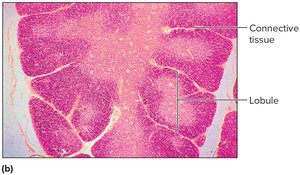
The thymus is a soft, bi-lobed organ located behind the sternum, anterior to the aorta. It is large in children and shrinks with age. The thymus is divided into lobules containing lymphocytes, some of which mature into T cells. It secretes hormones called thymosins that influence T cell maturation.
Spleen
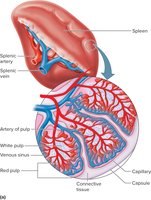
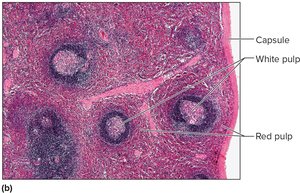
The spleen is the largest lymphatic organ, located in the upper left abdominal cavity. It filters blood, removes damaged cells, and contains white pulp (lymphocytes) and red pulp (red blood cells, macrophages, lymphocytes).
Body Defenses Against Infection
Pathogens are disease-causing agents such as bacteria, viruses, fungi, or protozoans. The body has two basic defense mechanisms: innate (nonspecific) defenses and adaptive (specific) defenses.
Innate defenses: Guard against many types of pathogens; respond quickly.
Adaptive defenses: Respond against specific pathogens; respond more slowly.
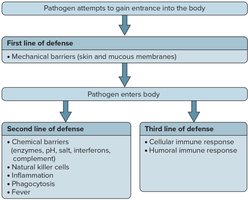
Innate (Nonspecific) Defenses
Species resistance: Resistance to diseases affecting other species.
Mechanical barriers: Physical separation (skin, mucous membranes, hair, mucus, sweat).
Inflammation: Tissue response to injury/infection; characterized by redness, swelling, heat, pain.
Chemical barriers: Chemicals that kill pathogens (e.g., HCl in gastric juice, enzymes, interferons, complement).
Natural killer (NK) cells: Lymphocytes that defend against viruses and cancer cells by secreting perforins.
Phagocytosis: Engulfment and digestion of pathogens by neutrophils and monocytes.
Fever: Elevated body temperature creates a hostile environment for pathogens and enhances phagocytic activity.
Adaptive (Specific) Defenses or Immunity
Immunity is the body's response against specific pathogens, toxins, or metabolic products. It is the third line of defense and involves lymphocytes and macrophages that recognize and remember specific foreign molecules.
Includes cellular immune response (cell-mediated) and humoral immune response (antibody-mediated).
Antigens
Molecules that evoke an immune response; can be proteins, polysaccharides, glycoproteins, or glycolipids.
Immune response is directed against "nonself" antigens.
Small molecules called haptens become antigenic when combined with larger molecules.
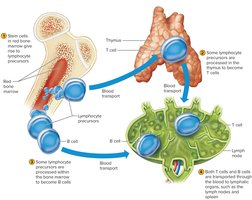
Lymphocyte Origins
Red bone marrow releases undifferentiated lymphocyte precursors.
Some precursors migrate to the thymus and become T cells; others mature in bone marrow as B cells.
T cells and B cells settle in lymphatic organs and tissues.
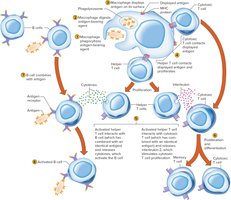
T Cells and the Cellular Immune Response
T cells require activation by antigen-presenting cells (APCs) such as macrophages or B cells. APCs display antigenic fragments on their membranes, complexed with MHC proteins, which help T cells recognize antigens. Activated T cells interact directly with antigen-bearing cells and secrete cytokines to enhance immune responses.
Helper T cells stimulate B cells to produce antibodies.
Cytotoxic T cells eliminate cancer and virus-infected cells by releasing perforin.
Memory T cells provide rapid response to future exposures.
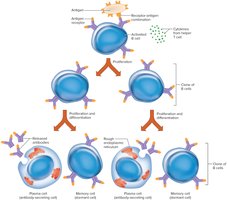
B Cells and the Humoral Immune Response
B cells become activated when they encounter matching antigens, often with help from helper T cells. Activated B cells proliferate and differentiate into plasma cells (which secrete antibodies) and memory B cells (which respond to future exposures).
Antibodies travel through body fluids to inactivate and destroy antigens.
This is called the humoral immune response.
Types of Antibodies (Immunoglobulins)
IgG: Most abundant; found in tissue fluid and plasma; defends against bacteria, viruses, toxins; activates complement.
IgA: Found in exocrine gland secretions (breast milk, saliva, tears, etc.).
IgM: Found in plasma; activates complement; contains Anti-A and Anti-B for blood transfusions.
IgD: Found on B lymphocytes; functions in B cell activation.
IgE: Found on basophils and mast cells; associated with allergic reactions.
Antibody Actions
Direct attack: agglutination, precipitation, neutralization.
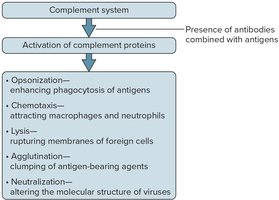
Activation of complement: opsonization, chemotaxis, inflammation, agglutination, neutralization, lysis.
Stimulation of local inflammation.
Immune Responses
Primary immune response: Activation of B or T cells during first encounter; antibodies appear in plasma in 5-10 days.
Secondary immune response: Rapid, long-lasting response to subsequent encounters; memory B and T cells proliferate, antibodies appear in 1-2 days and remain for months to years.
Practical Classification of Immunity
Naturally acquired active immunity: Exposure to antigen; long-term resistance due to memory B cells.
Artificially acquired active immunity: Vaccines; long-term immunity without illness.
Naturally acquired passive immunity: Antibodies passed from mother to fetus; short-term immunity.
Artificially acquired passive immunity: Injection of antibodies; short-term immunity.
Hypersensitivity
Type I (immediate-reaction): Allergy; IgE antibodies attach to mast cells and basophils, releasing mediators (histamine, prostaglandin, leukotrienes).
Type II (antibody-dependent cytotoxic): IgG/IgM antibodies; transfusion reactions.
Type III (immune complex): IgG antibodies; rheumatoid arthritis.
Type IV (delayed-reaction): T cell activation; skin eruptions, inflammation (e.g., poison ivy).
Transplantation and Tissue Rejection
Transplantation replaces damaged body parts.
Immune system may react with foreign antigens, causing tissue rejection.
Close matching of donor and recipient tissues and immunosuppressive drugs reduce rejection risk.
Autoimmunity
Immune system turns against self antigens, producing autoantibodies and cytotoxic T cells.
Autoimmune disorders may result from viral infection, faulty T cell development, or cross-reactivity.
Example: Type 1 Diabetes mellitus—autoantibodies destroy insulin-producing beta cells.
