 Back
BackMuscle Tissue and Contraction: Structure, Function, and Mechanisms
Study Guide - Smart Notes

Muscle Tissue: Types and Characteristics
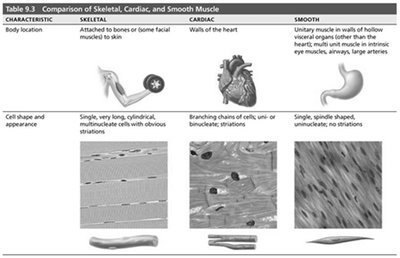
Comparison of Skeletal, Cardiac, and Smooth Muscle
Muscle tissue is classified into three main types, each with distinct structural and functional properties. Understanding these differences is essential for comprehending how muscles contribute to body movement and organ function.
Skeletal Muscle: Attached to bones or skin, responsible for voluntary movements. Cells are long, cylindrical, multinucleated, and striated.
Cardiac Muscle: Found only in the heart, responsible for pumping blood. Cells are branching, striated, usually uninucleate or binucleate, and connected by intercalated discs.
Smooth Muscle: Located in walls of hollow organs (except the heart), responsible for involuntary movements. Cells are spindle-shaped, uninucleate, and non-striated.
Key Characteristics Shared by All Muscle Types:
Excitability (Responsiveness): Ability to receive and respond to stimuli.
Contractility: Ability to shorten forcibly when stimulated.
Extensibility: Ability to be stretched.
Elasticity: Ability to recoil to resting length after stretching.
Structure of Skeletal Muscle
Connective Tissue Sheaths
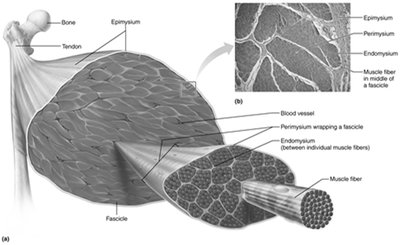
Skeletal muscles are organized into bundles and surrounded by connective tissue sheaths that provide support and protection.
Epimysium: Dense irregular connective tissue surrounding the entire muscle.
Perimysium: Fibrous connective tissue surrounding fascicles (bundles of muscle fibers).
Endomysium: Fine areolar connective tissue surrounding each individual muscle fiber.
Muscle Attachments
Origin: Attachment to immovable or less movable bone.
Insertion: Attachment to movable bone.
Direct Attachment: Epimysium fused to periosteum of bone or perichondrium of cartilage.
Indirect Attachment: Connective tissue wrappings extend beyond muscle as a tendon or aponeurosis.
Organizational Levels of Skeletal Muscle
Skeletal muscle is organized hierarchically from the whole muscle down to the molecular level.
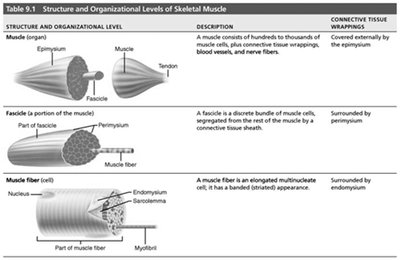
Structure and Organizational Level | Description | Connective Tissue Wrapping |
|---|---|---|
Muscle (organ) | Hundreds to thousands of muscle cells, connective tissue, blood vessels, and nerve fibers | Epimysium |
Fascicle (portion of muscle) | Discrete bundle of muscle cells segregated from rest by connective tissue sheath | Perimysium |
Muscle fiber (cell) | Elongated multinucleate cell with striated appearance | Endomysium |
Microscopic Anatomy of Skeletal Muscle
Muscle Fiber Structure
Skeletal muscle fibers are long, cylindrical cells containing multiple nuclei. The plasma membrane is called the sarcolemma, and the cytoplasm is the sarcoplasm, which contains glycosomes (for glycogen storage) and myoglobin (for oxygen storage).
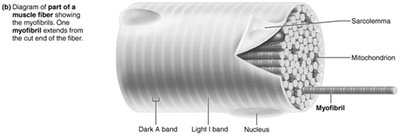
Myofibrils and Sarcomeres
Myofibrils are densely packed, rodlike elements that make up about 80% of muscle cell volume. They are composed of repeating units called sarcomeres, the smallest contractile units of muscle fibers.
Sarcomere: Region between two Z discs; contains thick (myosin) and thin (actin) filaments.
Striations: Alternating dark (A bands) and light (I bands) regions due to the arrangement of myofilaments.
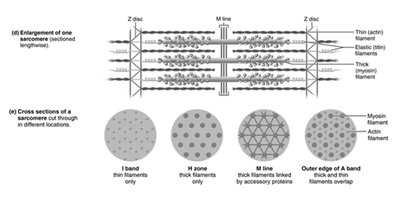
Molecular Composition of Myofilaments
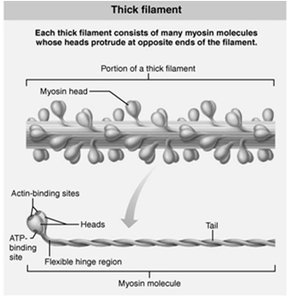
Thick Filaments: Composed of myosin molecules, each with a tail and two heads. Myosin heads bind to actin during contraction and have ATPase activity.
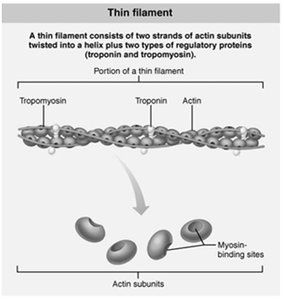
Thin Filaments: Composed of actin subunits (G actin) that form long chains (F actin). Regulatory proteins tropomyosin and troponin control myosin binding.
Elastic Filaments: Composed of titin, which helps maintain the structure and elasticity of the sarcomere.
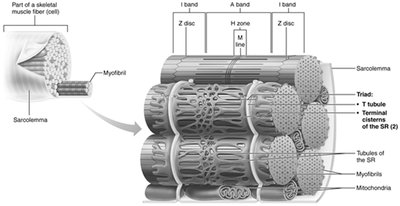
Sarcoplasmic Reticulum and T Tubules
The sarcoplasmic reticulum (SR) is a network of smooth endoplasmic reticulum that stores and releases calcium ions. T tubules are invaginations of the sarcolemma that conduct electrical impulses deep into the muscle fiber, ensuring simultaneous contraction.
Mechanism of Muscle Contraction
Sliding Filament Model of Contraction
Muscle contraction occurs when thin filaments slide past thick filaments, increasing their overlap. This process is powered by the formation and breaking of cross bridges between actin and myosin heads.
Neither thick nor thin filaments change length; only their degree of overlap changes.
Contraction is initiated when myosin heads bind to actin, forming cross bridges.


Neuromuscular Junction and Muscle Fiber Excitation
Ion Channels and Action Potentials
Ion channels play a critical role in generating and propagating action potentials in muscle fibers.
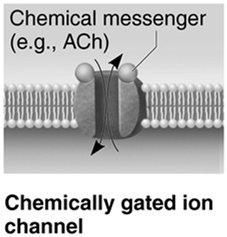
Chemically Gated Ion Channels: Open in response to neurotransmitters (e.g., acetylcholine).
Voltage-Gated Ion Channels: Open or close in response to changes in membrane potential.

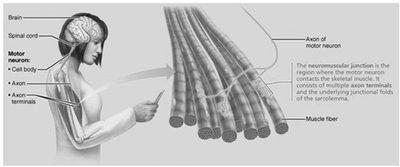
Neuromuscular Junction (NMJ)
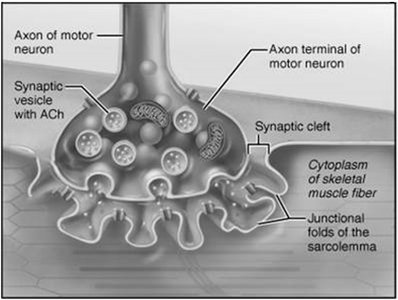
The NMJ is the site where a motor neuron communicates with a skeletal muscle fiber. It consists of the axon terminal, synaptic cleft, and junctional folds of the sarcolemma.
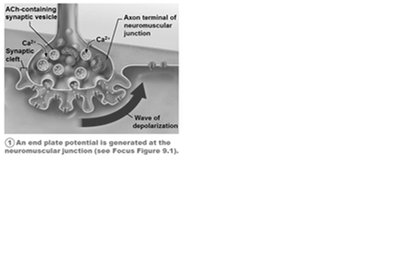
Acetylcholine (ACh) is released from synaptic vesicles in the axon terminal and binds to receptors on the sarcolemma, initiating an action potential.
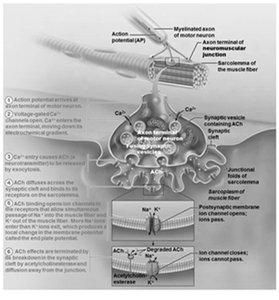
Events at the Neuromuscular Junction
Action potential arrives at axon terminal.
Voltage-gated calcium channels open; calcium enters the neuron.
Calcium triggers release of ACh into the synaptic cleft.
ACh binds to receptors on the sarcolemma, opening Na+ channels and generating an end plate potential.
Acetylcholinesterase degrades ACh, terminating the signal.
Generation and Propagation of Action Potentials
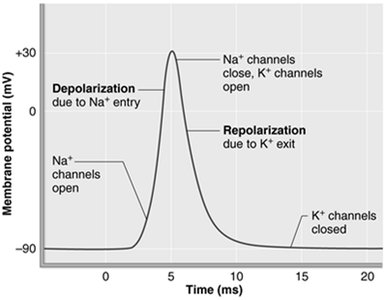
Phases of Action Potential
Generation of End Plate Potential: Local depolarization due to Na+ influx.
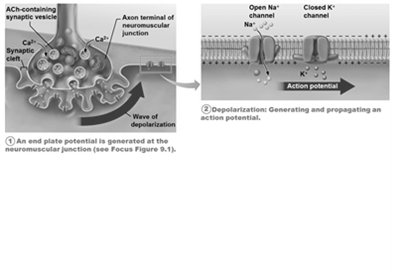
Depolarization: If threshold is reached, voltage-gated Na+ channels open, and an action potential is propagated along the sarcolemma.
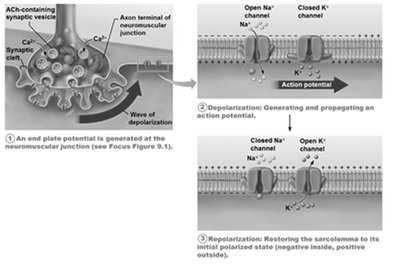
Repolarization: Na+ channels close, K+ channels open, restoring the resting membrane potential.
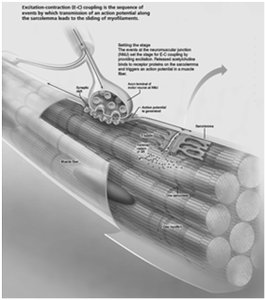
Excitation-Contraction (E-C) Coupling
Sequence of Events
Excitation-contraction coupling links the action potential in the sarcolemma to the sliding of myofilaments, resulting in muscle contraction.
Action potential travels along sarcolemma and down T tubules.
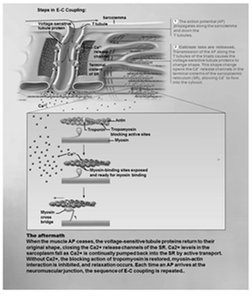
Voltage-sensitive proteins trigger Ca2+ release from the SR.
Ca2+ binds to troponin, moving tropomyosin and exposing myosin-binding sites on actin.
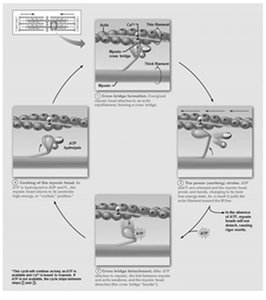
Cross Bridge Cycling
Steps of the Cross Bridge Cycle
Cross Bridge Formation: Myosin head attaches to actin.
Power Stroke: Myosin head pivots, pulling actin toward the M line.
Cross Bridge Detachment: ATP binds to myosin, causing it to detach from actin.
Cocking of Myosin Head: ATP hydrolysis re-energizes the myosin head for the next cycle.
Note: When nervous stimulation ceases, Ca2+ is pumped back into the SR, and muscle contraction ends.
Clinical Application: Rigor Mortis
Rigor mortis is the stiffening of muscles after death due to the lack of ATP, which prevents detachment of myosin from actin and reuptake of Ca2+ into the SR. Muscles remain contracted until proteins degrade.
Additional info: This guide covers the structure and function of muscle tissue, the mechanism of contraction, and the physiological basis of muscle excitation and contraction, as outlined in a typical college-level Anatomy and Physiology curriculum.
