 Back
BackMuscle Tissue: Structure, Function, and Physiology
Study Guide - Smart Notes

Muscle Tissue: Structure, Function, and Physiology
Introduction to Muscle Tissue
Muscle tissue is essential for movement, posture, and various physiological processes. There are three main types of muscle tissue: skeletal, cardiac, and smooth muscle, each with distinct structures and functions.
Properties of Muscular Tissue
Electrical excitability: Ability to respond to stimuli by producing electrical signals.
Contractility: Ability to shorten forcefully when stimulated.
Extensibility: Ability to stretch without being damaged.
Elasticity: Ability to return to original shape after stretching or contracting.
Muscles are organs that use chemical energy from nutrients to contract and move attached structures. They also provide muscle tone, propel body fluids and food, generate the heartbeat, and produce body heat.
Types of Muscle Tissue
Skeletal Muscle
Skeletal muscle is attached to bones and is responsible for voluntary movements of the body. It is striated and multinucleated.
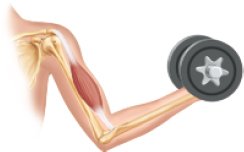
Cardiac Muscle
Cardiac muscle is found only in the heart. It is striated, branched, and usually has a single nucleus per cell. Cardiac muscle contracts involuntarily to pump blood throughout the body.
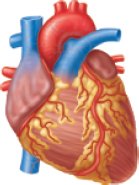
Smooth Muscle
Smooth muscle is found in the walls of hollow organs such as the stomach, intestines, and blood vessels. It is non-striated and involuntary, controlling movements like peristalsis and vasoconstriction.
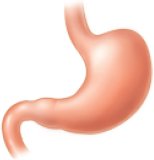
Muscle Structure and Organization
Connective Tissue Coverings
Each skeletal muscle is an organ composed of muscle tissue, connective tissue, blood vessels, and nerves. Connective tissue layers include:
Epimysium: Surrounds the entire muscle.
Perimysium: Surrounds bundles of muscle fibers called fascicles.
Endomysium: Surrounds individual muscle fibers.
Fascia: Dense connective tissue that separates muscles and forms tendons and aponeuroses.
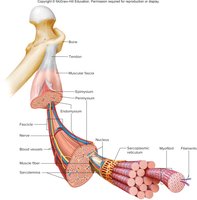
Skeletal Muscle Fiber Anatomy
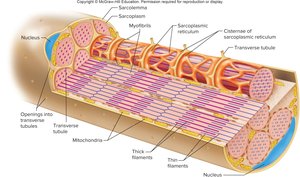
Each muscle fiber is a long, cylindrical cell with multiple nuclei. The cell membrane is called the sarcolemma, and the cytoplasm is the sarcoplasm, which contains mitochondria and myofibrils. Myofibrils are composed of repeating units called sarcomeres, the functional units of contraction.
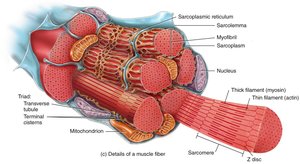
Striations and Sarcomere Structure
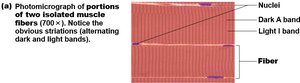
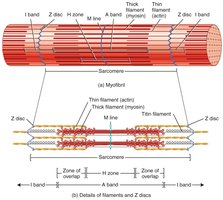
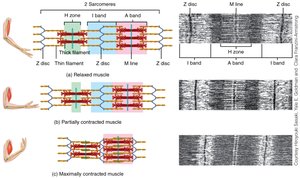
Striations in skeletal muscle are due to the arrangement of thick (myosin) and thin (actin) filaments within the sarcomeres. Key regions include:
A bands: Dark regions containing thick filaments.
I bands: Light regions containing thin filaments.
Z discs: Boundaries of each sarcomere.
H zone: Lighter region in the middle of the A band with only thick filaments.
M line: Center of the H zone, holding thick filaments in place.
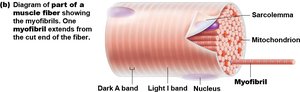
Sarcoplasmic Reticulum and T Tubules
The sarcoplasmic reticulum (SR) is a network of membranous channels that stores calcium ions, essential for muscle contraction. Transverse (T) tubules are invaginations of the sarcolemma that help transmit action potentials deep into the muscle fiber, ensuring coordinated contraction.
Muscle Proteins
Types of Muscle Proteins
Contractile proteins: Myosin (thick filament) and actin (thin filament).
Regulatory proteins: Troponin and tropomyosin, which control the interaction between actin and myosin.
Structural proteins: Titin, nebulin, alpha-actinin, myomesin, and dystrophin, which maintain the alignment and stability of sarcomeres.
Neuromuscular Junction and Muscle Contraction
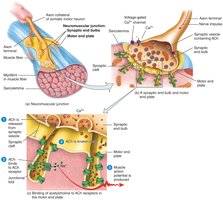
Neuromuscular Junction (NMJ)
The NMJ is the synapse between a motor neuron and a skeletal muscle fiber. When an action potential reaches the axon terminal, the neurotransmitter acetylcholine (ACh) is released, triggering muscle contraction.
Sliding Filament Model
Muscle contraction occurs when myosin heads bind to actin, forming cross-bridges and pulling the thin filaments toward the center of the sarcomere. This process shortens the sarcomere and generates force.
Role of Myosin and Actin
Myosin molecules have heads that attach to actin binding sites. Troponin and tropomyosin regulate this interaction by covering or exposing the binding sites on actin in response to calcium ions.
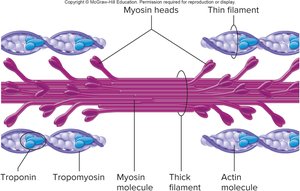
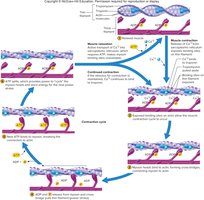
Contraction Cycle
The contraction cycle involves repeated formation and breaking of cross-bridges, powered by ATP hydrolysis. The cycle continues as long as calcium ions and ATP are available.
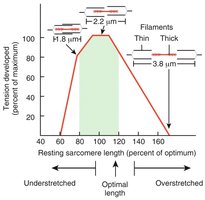
Length-Tension Relationship
The force a muscle can generate depends on the initial length of its sarcomeres. Optimal overlap between thick and thin filaments produces maximal tension.
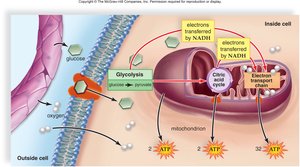
Muscle Metabolism and Energy Sources
ATP Production in Muscle
Muscle fibers require ATP for contraction, which is generated by three main pathways:
Creatine phosphate: Provides rapid ATP regeneration for short bursts of activity.
Anaerobic glycolysis: Produces ATP without oxygen, resulting in lactic acid formation.
Aerobic respiration: Uses oxygen to produce large amounts of ATP in mitochondria.
Creatine Phosphate System
Creatine phosphate donates a phosphate group to ADP to rapidly regenerate ATP during the initial seconds of intense activity.
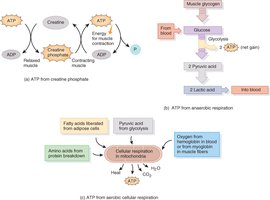
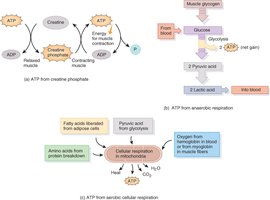
Anaerobic and Aerobic Respiration
During high-intensity exercise, anaerobic glycolysis provides ATP but also produces lactic acid. Aerobic respiration, which occurs in mitochondria, is more efficient and supports prolonged activity.
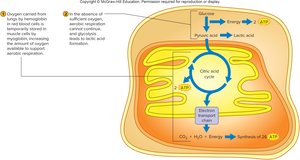
Muscle Fiber Types
Classification of Skeletal Muscle Fibers
Slow oxidative fibers (Type I): Red, high myoglobin, many mitochondria, fatigue-resistant, used for endurance.
Fast oxidative-glycolytic fibers (Type IIa): Pink, intermediate properties, used for moderate activity.
Fast glycolytic fibers (Type IIb): White, low myoglobin, few mitochondria, fatigue quickly, used for short bursts of power.

Muscle Contraction Types
Isotonic and Isometric Contractions
Isotonic contraction: Muscle changes length to move a load (concentric = shortens, eccentric = lengthens).
Isometric contraction: Muscle generates tension without changing length (e.g., holding a posture).
Clinical Aspects and Muscle Disorders
Muscular Dystrophy
Muscular dystrophy is a group of inherited diseases causing progressive muscle weakness and degeneration. Duchenne muscular dystrophy is the most common form, caused by a defect in the dystrophin gene.
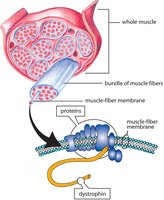
Myasthenia Gravis
Myasthenia gravis is an autoimmune disorder where antibodies attack acetylcholine receptors at the neuromuscular junction, leading to muscle weakness.
Development and Adaptation of Muscle Tissue
Muscle Growth and Repair
Muscle fibers grow in size (hypertrophy) in response to resistance training. Satellite cells aid in repair and regeneration, but the number of muscle fibers does not increase significantly after birth.
Effects of Exercise
Aerobic exercise: Increases endurance, capillary density, and mitochondrial content.
Resistance exercise: Increases muscle size and strength through hypertrophy.
Aging and Muscle Tissue
With aging, muscle mass decreases (sarcopenia), and connective tissue increases. Regular exercise can slow these changes and maintain muscle function.
Additional info: This guide covers the structure, function, and physiology of muscle tissue, including clinical correlations and adaptations to exercise, as relevant to an introductory college-level anatomy and physiology course.
