 Back
BackRenal System: Filtration, Reabsorption, and Regulation
Study Guide - Smart Notes

Renal System Overview
Main Functions of the Renal System
The renal system, primarily composed of the kidneys, is essential for maintaining homeostasis by filtering blood, reabsorbing vital substances, and secreting wastes. The three main functions are:
Filtration: Removal of water and small solutes from the blood into the nephron.
Reabsorption: Recovery of water, glucose, amino acids, and electrolytes from the filtrate back into the blood.
Secretion: Active transport of substances from the blood into the filtrate for excretion.
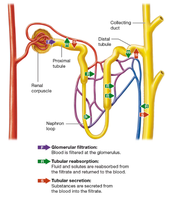
Glomerular Filtration
Filtration Membrane Structure and Function
Glomerular filtration is the first step in urine formation, occurring in the renal corpuscle. The filtration membrane consists of three layers:
Fenestrated glomerular capillary endothelial cells: Large pores (70-100 nm) allow passage of water and small solutes but prevent blood cells and platelets from exiting.
Basal lamina: A thin extracellular matrix that acts as a meshwork, repelling most plasma proteins due to its negative charge.
Podocytes: Specialized cells with filtration slits that restrict passage of large proteins (e.g., albumin) and macromolecules.
The result is a filtrate containing water, electrolytes, acids, bases, organic compounds, and metabolic wastes, but not large proteins or cells.
Glomerular Filtration Rate (GFR)
The glomerular filtration rate (GFR) is the volume of filtrate formed by both kidneys per minute, typically about 125 mL/min. This means the entire plasma volume is filtered approximately 60 times per day.
Filtration Pressures and Net Filtration Pressure
Filtration is driven by the balance of hydrostatic and osmotic pressures across the filtration membrane. The net filtration pressure determines the rate and efficiency of filtration.
Regulation of GFR
Factors Affecting GFR
GFR is tightly regulated to ensure proper waste removal and fluid/electrolyte balance. Regulatory mechanisms include:
Autoregulation: Myogenic mechanisms and tubuloglomerular feedback adjust afferent arteriole diameter in response to blood pressure changes.
Hormonal Regulation: The renin-angiotensin-aldosterone system (RAAS) and atrial natriuretic peptide (ANP) modulate arteriole tone and sodium reabsorption.
Neural Regulation: Sympathetic nervous system activity can constrict arterioles and stimulate RAAS, especially during stress or blood loss.
Renin-Angiotensin-Aldosterone System (RAAS)
RAAS is activated by decreased blood pressure or GFR, leading to renin release, conversion of angiotensinogen to angiotensin I, and then to angiotensin II (by ACE). Angiotensin II increases blood pressure and GFR by vasoconstriction and stimulating aldosterone release.
Tubular Reabsorption and Secretion
Mechanisms of Tubular Reabsorption
Most filtrate is reabsorbed, especially in the proximal tubule and nephron loop. Reabsorption mechanisms include:
Facilitated diffusion: Passive movement of solutes via carrier proteins down their concentration gradient.
Primary active transport: Direct use of ATP to move solutes against their gradient.
Secondary active transport: Uses gradients established by primary active transport to move other solutes.

Carrier-Mediated Transport and Transport Maximum
Carrier proteins (antiporters and symporters) have a limited number of binding sites, leading to a transport maximum (TM). When all carriers are saturated, excess solute remains in the filtrate and is excreted in urine (e.g., glucose in diabetes mellitus).

Main Roles of the Proximal Tubule
Reabsorption of most electrolytes (Na+, Cl-, K+, SO42-, PO43-).
Reabsorption of nearly all nutrients (glucose, amino acids, vitamins).
Reabsorption of bicarbonate ions, critical for acid-base homeostasis.
Sodium Ion Reabsorption
Facilitated by carrier proteins and symporters (e.g., Na+-glucose symporter).
Antiporters exchange Na+ for H+, aiding in acid-base balance.
Regulation of Urine Concentration and Volume
Osmolarity Changes Along the Nephron
Filtrate osmolarity changes as it moves through the nephron:
Isosmotic upon entering the renal tubule.
Becomes more concentrated in the descending limb of the nephron loop (up to ~900 mOsm).
Becomes dilute in the ascending limb and early distal tubule (down to ~100 mOsm).
Hormonal Regulation
The final 15% of water reabsorption is regulated by hormones (e.g., ADH), allowing the kidneys to adjust urine concentration and volume according to the body's needs.
Countercurrent Mechanism
The countercurrent mechanism in the nephron loop and vasa recta establishes and maintains the medullary osmotic gradient, enabling the production of concentrated urine. Key components include:
Countercurrent multiplier (nephron loop of juxtamedullary nephrons)
Urea recycling in the medullary collecting ducts
Countercurrent exchanger (vasa recta)
Production of Dilute vs. Concentrated Urine
Dilute urine: Produced when ADH is low and water reabsorption is minimized.
Concentrated urine: Produced when ADH is high, increasing water reabsorption in the distal tubule and collecting duct.
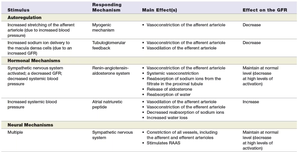
Summary Table: GFR Control Mechanisms
Stimulus | Responding Mechanism | Main Effect(s) | Effect on the GFR |
|---|---|---|---|
Increased stretching of the afferent arteriole due to increased blood pressure | Myogenic mechanism | Vasoconstriction of the afferent arteriole | Decrease |
Increased sodium ion delivery to the macula densa cells (due to increased GFR) | Tubuloglomerular feedback | Vasoconstriction of the afferent arteriole | Decrease |
Decreased systemic blood pressure | Renin-angiotensin-aldosterone system | Vasoconstriction of the efferent arteriole, reabsorption of sodium ions, release of aldosterone, stimulation of thirst | Maintain at normal or slightly decreased levels at high levels of stimulation |
Increased systemic blood pressure | Atrial natriuretic peptide | Vasodilation of the afferent arteriole, decreased reabsorption of sodium ions | Increase |
Multiple | Sympathetic nervous system | Constriction of all vessels, including afferent and efferent arterioles; stimulates RAAS | Maintain at normal or slightly decreased levels |
Practice Questions (Selected)
During glomerular filtration, water and small solutes exit glomerular capillaries.
Reclaiming substances from the tubular filtrate and returning them to the blood is called tubular reabsorption.
The pressure that promotes filtration is the glomerular hydrostatic pressure.
If GFR is low and needs to increase, the afferent arteriole will dilate and the efferent arteriole will constrict (False if reversed).
The immediate effect of the hormone ANP on GFR is to increase it (True).
The thin descending limb of the nephron loop is freely permeable to water.
When ADH is present, there is more water absorption in the distal tubule and the collecting ducts (True).
Respiratory acidosis (chronic hypoventilation) leads to increased reabsorption of bicarbonate ions by the kidneys.
Kidneys produce dilute urine when the ECF contains excess water.
All of the following contribute to the medullary osmotic gradient: countercurrent multiplier, urea recycling, and countercurrent exchanger (all of the above).
Alcohol inhibits ADH, leading to increased urine volume and decreased urine concentration.
