 Back
BackThe Autonomic Nervous System (ANS): Structure, Function, and Neurotransmitters
Study Guide - Smart Notes

Chapter 14: The Autonomic Nervous System (ANS)
Overview of the Nervous System
The nervous system is divided into the central nervous system (CNS) and the peripheral nervous system (PNS). The PNS includes both sensory (input) and motor (output) divisions. The motor division is further subdivided into the somatic nervous system (SNS) and the autonomic nervous system (ANS). The ANS is responsible for involuntary control of smooth muscle, cardiac muscle, and glands, maintaining homeostasis through subconscious regulation.
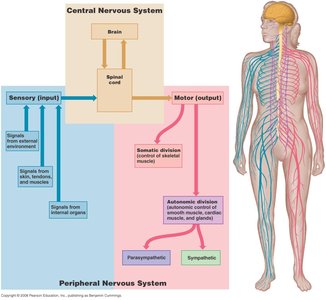
Somatic vs. Autonomic Nervous Systems
The somatic and autonomic nervous systems differ in their effectors, efferent pathways, and neurotransmitter effects:
Effectors: The SNS controls skeletal muscles, while the ANS innervates cardiac muscle, smooth muscle, and glands.
Efferent Pathways: The SNS uses a single, heavily myelinated neuron from the CNS to the effector. The ANS uses a two-neuron chain: a lightly myelinated preganglionic neuron and an unmyelinated postganglionic neuron.
Neurotransmitter Effects: SNS neurons release acetylcholine (ACh), always producing a stimulatory effect. ANS preganglionic fibers release ACh, while postganglionic fibers release either norepinephrine (NE) or ACh, producing either stimulatory or inhibitory effects depending on the receptor type.
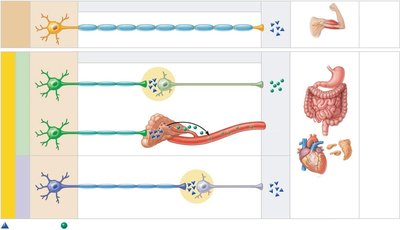
Divisions of the Autonomic Nervous System
Parasympathetic Division
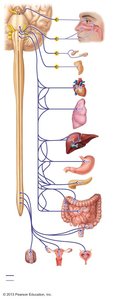
The parasympathetic division is responsible for 'rest and digest' activities. It promotes maintenance functions and conserves body energy. Its fibers originate from the craniosacral region (brainstem and sacral spinal cord), have long preganglionic and short postganglionic fibers, and use ACh as the neurotransmitter at both synapses. Effects are generally localized and short-lived.
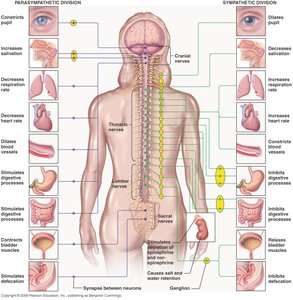
Physiological Effects: Increases salivation, lacrimation, urination, digestion, and defecation ("SLUDD"). Decreases heart rate, constricts airways, and constricts pupils.
Cranial Outflow: Involves cranial nerves III, VII, IX, and X, with cell bodies in the brainstem.
Sacral Outflow: Originates from S2-S4, serving pelvic organs and the distal half of the large intestine.
Sympathetic Division
The sympathetic division is responsible for 'fight or flight' responses, mobilizing the body during activity. Its fibers originate from the thoracolumbar region (thoracic and lumbar spinal cord), have short preganglionic and long postganglionic fibers, and use ACh at the preganglionic and NE (except sweat glands, which use ACh) at the postganglionic synapse. Effects are widespread and long-lasting.
Physiological Effects: Increases heart rate, dilates airways and pupils, inhibits digestion and elimination, and mobilizes energy stores. Activated during exercise, emergencies, excitement, or embarrassment ("E situations").
Adrenal Medulla Pathway: Some preganglionic fibers stimulate the adrenal medulla, causing the release of NE and epinephrine into the bloodstream for systemic effects.
Dual Innervation and Tone
Most visceral organs receive dual innervation from both divisions, which usually have opposing effects. Sympathetic tone maintains blood vessel constriction and blood pressure, while parasympathetic tone dominates heart rate and digestive/urinary tract activity under resting conditions. The sympathetic division can override parasympathetic effects during stress.
Neurotransmitters and Receptors in the ANS
Cholinergic and Adrenergic Neurons
Cholinergic Neurons: Release acetylcholine (ACh). Includes all ANS preganglionic neurons and all parasympathetic postganglionic neurons.
Adrenergic Neurons: Release norepinephrine (NE) or epinephrine. Includes most sympathetic postganglionic neurons.
Receptor Types
Nicotinic Receptors: Found on all postganglionic neurons and adrenal medulla cells. Always excitatory when bound by ACh.
Muscarinic Receptors: Found on all parasympathetic target organs. Can be excitatory or inhibitory depending on the organ and receptor subtype.
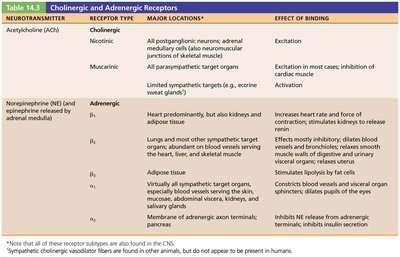
Adrenergic Receptors: Two main types: alpha (α) and beta (β), each with subtypes (α1, α2, β1, β2, β3). Effects depend on receptor subtype and location:
α1: Generally excitatory (e.g., constricts blood vessels, dilates pupils)
α2: Generally inhibitory (e.g., inhibits insulin release)
β1: Excitatory (e.g., increases heart rate, stimulates renin release)
β2: Inhibitory (e.g., dilates bronchioles, relaxes smooth muscle)
β3: Excitatory (e.g., stimulates lipolysis in adipose tissue)
Control of ANS Functioning
The hypothalamus is the main integrative center for ANS activity, receiving input from the limbic system, cerebral cortex, reticular formation, and spinal cord. This allows for subconscious regulation of visceral functions and integration with emotional and behavioral responses.
Summary Table: Parasympathetic vs. Sympathetic Divisions
Feature | Parasympathetic | Sympathetic |
|---|---|---|
Origin | Craniosacral (brainstem & sacral spinal cord) | Thoracolumbar (thoracic & lumbar spinal cord) |
Preganglionic Fibers | Long | Short |
Postganglionic Fibers | Short | Long |
Neurotransmitters | ACh (both synapses) | ACh (preganglionic), NE (postganglionic; ACh for sweat glands) |
Effects | Localized, short-lived | Widespread, long-lasting |
Physiological Role | "Rest and Digest" (SLUDD) | "Fight or Flight" (E situations) |
Key Equations
Neurotransmitter Inactivation:
ACh is inactivated by acetylcholinesterase (AChE):
NE and E are inactivated by monoamine oxidase (MAO) and catechol-O-methyltransferase (COMT):
Additional info: The ANS is essential for maintaining homeostasis and responding to internal and external stressors. Understanding its structure and function is foundational for advanced studies in physiology, pharmacology, and medicine.
