 Back
BackThe Endocrine System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Endocrine System Overview
Introduction to the Endocrine System
The endocrine system is a major regulatory system of the body, working alongside the nervous system to coordinate and integrate the activities of body cells. It primarily influences metabolic activities through the release of hormones into the bloodstream. Endocrine responses are generally slower but longer-lasting than those of the nervous system.
Endocrinology: The scientific study of hormones and endocrine organs.
Major functions include regulation of reproduction, growth and development, maintenance of electrolyte, water, and nutrient balance, regulation of cellular metabolism and energy balance, and mobilization of body defenses.
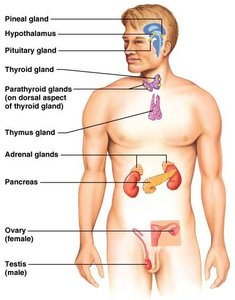
Comparison of Nervous and Endocrine Systems
The nervous and endocrine systems both regulate body functions, but they do so in distinct ways:
Nervous System | Endocrine System | |
|---|---|---|
Response Initiation | Rapid | Slow |
Duration | Short | Long |
Signaling Mechanism | Action potentials and neurotransmitters | Hormones in blood |
Target Location | Specific (axon pathways) | Diffuse (anywhere blood reaches) |
Distance of Action | Short | Long |
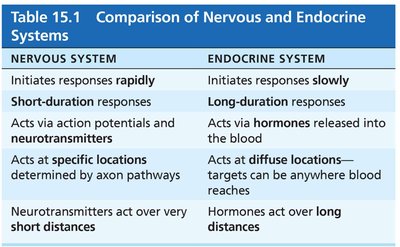
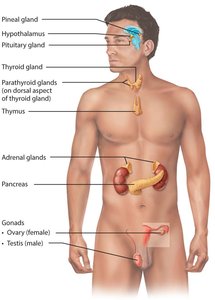
Endocrine Glands and Organs
Endocrine glands are ductless glands that secrete hormones directly into the bloodstream. Major endocrine glands include the pituitary, thyroid, parathyroid, adrenal, and pineal glands. The hypothalamus is considered a neuroendocrine organ. Some organs, such as the pancreas, gonads, and placenta, have both endocrine and exocrine functions. Other tissues, including adipose cells, thymus, and cells in the gastrointestinal tract, kidneys, and heart, also produce hormones.
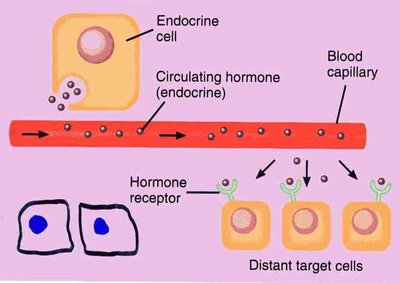
Hormones: Chemical Messengers of the Endocrine System
Types of Chemical Messengers
Hormones: Long-distance chemical signals that travel in blood or lymph to target cells.
Autocrines: Chemicals that exert effects on the same cells that secrete them (local action).
Paracrines: Locally acting chemicals that affect cells other than those that secrete them (local action).
Autocrines and paracrines are not considered part of the endocrine system.
Classes of Hormones
Amino acid–based hormones: Includes amino acid derivatives, peptides, and proteins.
Steroid hormones: Synthesized from cholesterol; includes gonadal and adrenocortical hormones.
Eicosanoids: Sometimes considered hormones, but most classify them as paracrines.
Hormone Action on Target Cells
Hormones affect only target cells that have specific receptors for them. They can:
Alter plasma membrane permeability or membrane potential by opening or closing ion channels
Stimulate synthesis of enzymes or other proteins
Activate or deactivate enzymes
Induce secretory activity
Stimulate mitosis
Mechanisms of Hormone Action
Water-Soluble vs. Lipid-Soluble Hormones
The mechanism of hormone action depends on the chemical nature of the hormone and the location of its receptor:
Lipid-Soluble Hormones | Water-Soluble Hormones | |
|---|---|---|
Consist of | All steroid hormones and thyroid hormone | All amino acid–based hormones except thyroid hormone |
Sources | Adrenal cortex, gonads, thyroid gland | All other endocrine glands |
Transport in Blood | Bound to plasma proteins | Usually free in plasma |
Location of Receptors | Usually inside cell | On plasma membrane |
Mechanism of Action | Activate genes, causing synthesis of new proteins | Usually act through second-messenger systems |

Second Messenger Systems
Most amino acid–based hormones (except thyroid hormone) use second-messenger systems to exert their effects. The two main systems are:
Cyclic AMP (cAMP) system
PIP2-calcium system
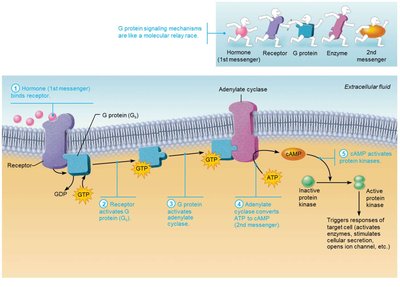
Cyclic AMP (cAMP) Second-Messenger System
Hormone (first messenger) binds to receptor.
Receptor activates a G protein.
G protein activates or inhibits adenylate cyclase.
Adenylate cyclase converts ATP to cAMP (second messenger).
cAMP activates protein kinases, which phosphorylate other proteins, leading to cellular responses.
cAMP is rapidly degraded by phosphodiesterase, stopping the cascade. This mechanism allows for amplification of the hormone signal.
PIP2-Calcium Signaling Mechanism
Hormone-activated G protein activates phospholipase C.
Phospholipase C splits PIP2 into two second messengers: diacylglycerol (DAG) and inositol trisphosphate (IP3).
DAG activates protein kinases; IP3 causes Ca2+ release from intracellular stores.
Calcium ions act as another second messenger, often binding to calmodulin to activate enzymes.
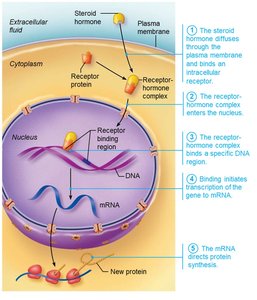
Direct Gene Activation by Lipid-Soluble Hormones
Lipid-soluble hormones (steroids and thyroid hormone) diffuse into target cells and bind to intracellular receptors. The hormone-receptor complex enters the nucleus, binds to DNA, and initiates transcription of specific genes, resulting in protein synthesis.
Regulation of Hormone Release
Control of Hormone Levels
Blood levels of hormones are controlled by negative feedback mechanisms, maintaining hormone concentrations within a narrow range. Hormone release is triggered by:
Endocrine gland stimuli (humoral, neural, hormonal)
Nervous system modulation
Types of Endocrine Gland Stimuli
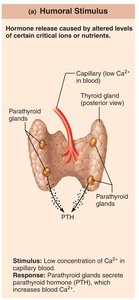
Humoral stimuli: Changing blood levels of ions or nutrients directly stimulate hormone secretion (e.g., low Ca2+ stimulates parathyroid hormone release).
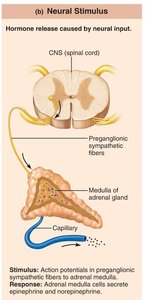
Neural stimuli: Nerve fibers stimulate hormone release (e.g., sympathetic nervous system stimulates adrenal medulla to secrete catecholamines).
Hormonal stimuli: Hormones stimulate other endocrine organs to release their hormones (e.g., hypothalamic hormones stimulate anterior pituitary hormones).
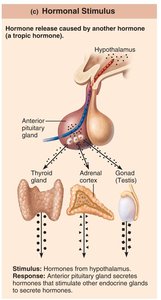
Nervous System Modulation
The nervous system can override or modulate endocrine controls, especially during stress, to ensure the body responds appropriately (e.g., overriding insulin release to increase blood glucose during fight-or-flight response).
Target Cell Specificity and Hormone Activity
Target Cell Activation
Only cells with specific receptors for a hormone (target cells) respond to that hormone. The degree of activation depends on:
Blood levels of the hormone
Number of receptors on/in the target cell
Affinity (strength) of binding between hormone and receptor
Cells can adjust their sensitivity by up-regulating (increasing receptors) or down-regulating (decreasing receptors) in response to hormone levels.
Hormone Transport, Half-Life, and Duration
Steroid and thyroid hormones are transported bound to plasma proteins; others circulate freely.
Hormones are removed by degrading enzymes, kidneys, or liver.
Half-life: Time required for hormone blood level to decrease by half; varies from minutes to a week.
Response times and duration depend on hormone type and solubility.
Hormone Interactions at Target Cells
Permissiveness: One hormone requires another to exert its full effect (e.g., reproductive hormones need thyroid hormone).
Synergism: More than one hormone produces the same effect, amplifying the response (e.g., glucagon and epinephrine both increase blood glucose).
Antagonism: One hormone opposes the action of another (e.g., insulin vs. glucagon).
The Hypothalamus and Pituitary Gland
Structure and Function
The hypothalamus is connected to the pituitary gland (hypophysis) via the infundibulum. The pituitary gland is known as the "master gland" and secretes at least eight major hormones. It has two lobes:
Posterior pituitary (neurohypophysis): Neural tissue; stores and releases neurohormones produced by the hypothalamus (oxytocin and ADH).
Anterior pituitary (adenohypophysis): Glandular tissue; produces and releases its own hormones under hypothalamic regulation.
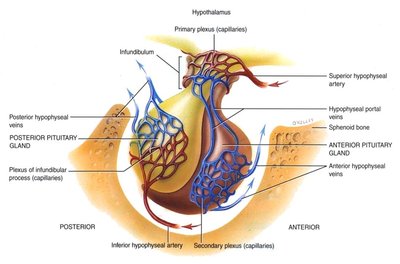
Pituitary-Hypothalamic Relationships
The posterior pituitary maintains a neural connection to the hypothalamus via the hypothalamic-hypophyseal tract. The anterior pituitary is connected via the hypophyseal portal system, a network of blood vessels that allows hypothalamic hormones to regulate anterior pituitary hormone secretion.
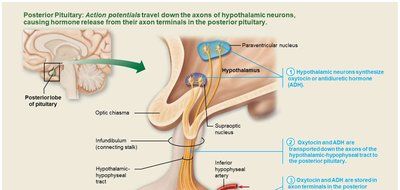
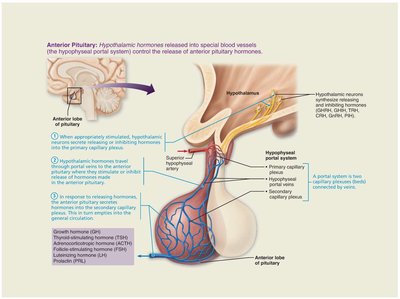
Posterior Pituitary and Hypothalamic Hormones
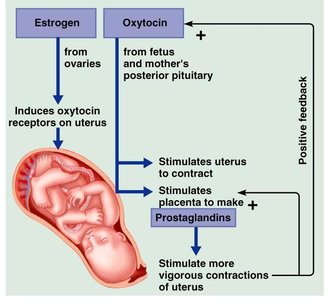
Oxytocin
Strong stimulant of uterine contractions during childbirth (positive feedback mechanism).
Triggers milk ejection during lactation.
Acts as a neurotransmitter in the brain.
Uses the PIP2-calcium second messenger system.
Antidiuretic Hormone (ADH)
Produced in the hypothalamus and released by the posterior pituitary.
Regulates water balance by targeting kidney tubules to reabsorb more water, reducing urine output.
Release is triggered by high solute concentration, pain, low blood pressure, and certain drugs; inhibited by alcohol and diuretics.
High concentrations cause vasoconstriction (vasopressin).
Clinical Significance
Diabetes insipidus: ADH deficiency, leading to excessive urination and thirst.
SIADH: Excessive ADH secretion, causing fluid retention and hyponatremia.
Anterior Pituitary Hormones
Overview
All six anterior pituitary hormones are peptides.
All but growth hormone (GH) activate target cells via cAMP second-messenger system.
All but two are tropic hormones (regulate secretion of other hormones).
Growth Hormone (GH)
Also called somatotropin; produced by somatotropic cells.
Direct actions: Increases blood glucose (anti-insulin effect), stimulates breakdown of glycogen, increases fatty acid levels, and encourages protein synthesis.
Indirect actions: Stimulates liver, skeletal muscle, and bone to produce insulin-like growth factors (IGFs), promoting cell division, collagen formation, and bone matrix deposition.
Regulation: Stimulated by growth hormone–releasing hormone (GHRH); inhibited by growth hormone–inhibiting hormone (GHIH, or somatostatin) and negative feedback from IGFs and GH.
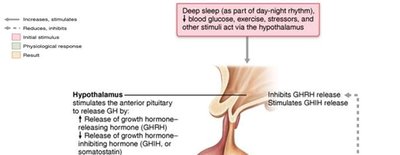
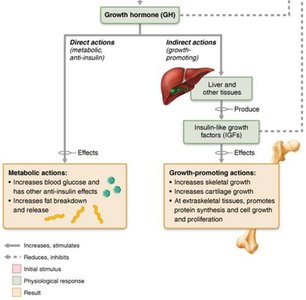
Clinical Significance: GH Imbalances
Hypersecretion (usually due to pituitary tumor):
In children: Gigantism (excessive growth, height up to 8 feet).
In adults: Acromegaly (overgrowth of hands, feet, face).
Hyposecretion:
In children: Pituitary dwarfism (short stature, up to 4 feet).
In adults: Usually no significant effects.

Thyroid-Stimulating Hormone (TSH)
Also called thyrotropin; produced by thyrotropic cells.
Stimulates normal development and secretory activity of the thyroid gland.
Release is triggered by thyrotropin-releasing hormone (TRH) from the hypothalamus and inhibited by rising thyroid hormone levels and GHIH.
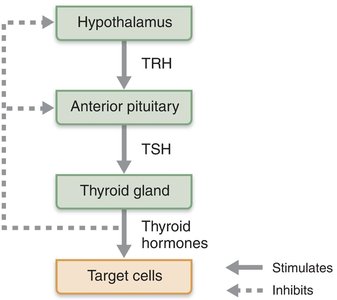
Adrenocorticotropic Hormone (ACTH)
Also called corticotropin; secreted by corticotropic cells.
Stimulates the adrenal cortex to release corticosteroids.
Release is triggered by corticotropin-releasing hormone (CRH) from the hypothalamus, with highest levels in the morning; stress, fever, and hypoglycemia can increase CRH release.
Gonadotropins (FSH and LH)
Follicle-stimulating hormone (FSH) and luteinizing hormone (LH) are secreted by gonadotropic cells.
FSH stimulates gamete production (egg or sperm).
LH promotes production of gonadal hormones (estrogen, progesterone, testosterone); triggers ovulation in females.
