 Back
BackThe Urinary System and Excretory Function: Structure, Histology, and Physiology
Study Guide - Smart Notes

Excretory System Overview
Introduction to Excretion
The excretory system is responsible for removing metabolic wastes from the internal environment, maintaining homeostasis by regulating water, salts, and other substances. Major excretory organs include the lungs, skin, liver, gastrointestinal tract, and especially the kidneys, which account for the bulk of excretion.
Wastes removed: Water, heat, salts, urea, and other metabolic byproducts
Homeostatic role: Maintains fluid, electrolyte, and acid-base balance
Fluid Input and Output
Body fluid balance is maintained by regulating intake and output. The kidneys play a central role in this regulation.
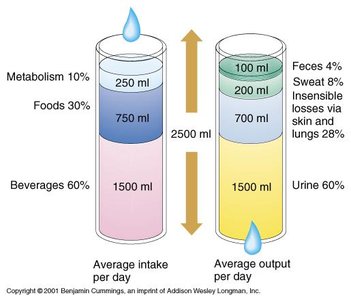
Average intake: 2500 ml/day (from beverages, food, and metabolism)
Average output: 2500 ml/day (mainly urine, but also sweat, feces, and insensible losses)
Urinary System Anatomy
Gross Anatomy of the Urinary System
The urinary system consists of the kidneys, ureters, urinary bladder, and urethra. These organs work together to filter blood, form urine, and eliminate it from the body.
Kidneys: Filter blood and form urine
Ureters: Transport urine from kidneys to bladder
Urinary bladder: Stores urine until excretion
Urethra: Conducts urine out of the body
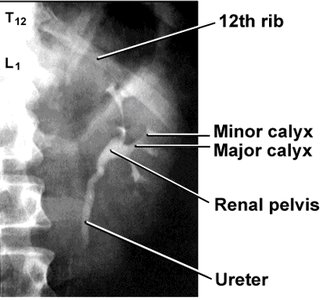
Kidney Location and Structure
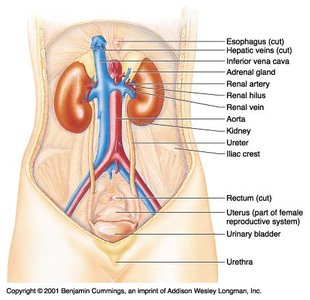
The kidneys are retroperitoneal organs located on either side of the vertebral column. They are protected by the lower ribs and surrounded by fat and connective tissue.
Renal hilus: Entry/exit site for vessels, nerves, and ureter
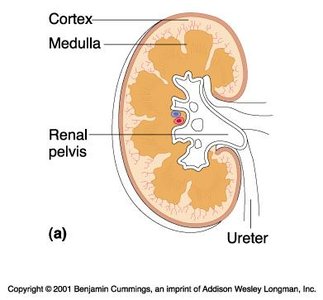
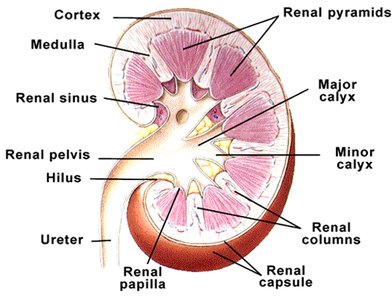
Renal cortex: Outer region containing glomeruli
Renal medulla: Inner region with renal pyramids
Renal pelvis: Funnel-shaped reservoir that collects urine
Histology of the Urinary Tract
Ureter Histology
The ureter wall is composed of three layers: mucosa (with transitional epithelium), muscularis (smooth muscle), and adventitia. The transitional epithelium allows for stretching as urine passes through.
Transitional epithelium: Specialized for distension
Muscularis: Smooth muscle for peristalsis
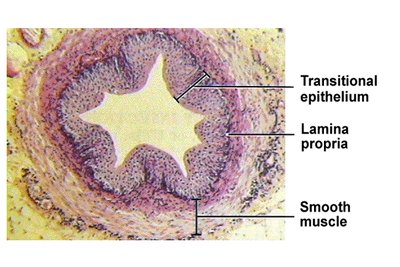
Urinary Bladder Structure and Histology
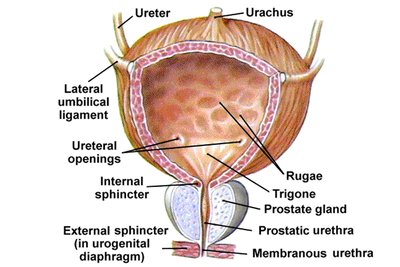
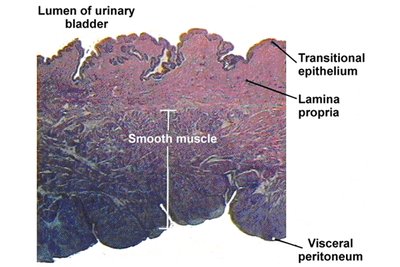
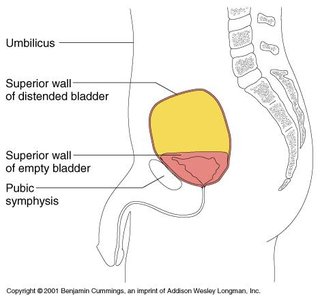
The urinary bladder is a highly distensible organ with a mucosa of transitional epithelium, a thick muscular wall (detrusor muscle), and an outer serosa. It can store 10–600 ml of urine, with the capacity to expand further if needed.
Rugae: Folds that allow expansion
Internal and external sphincters: Control urine release
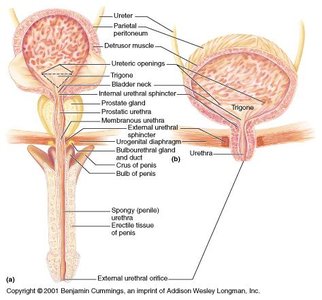
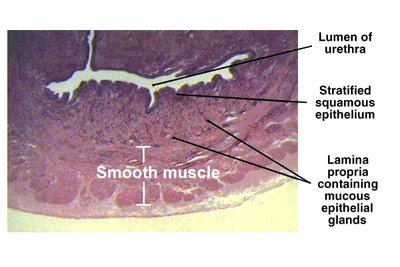
Urethra Structure and Histology
The urethra's epithelium transitions from transitional to stratified squamous along its length, with numerous mucous glands present. The wall contains smooth muscle and a lamina propria with mucous glands.
Male vs. female urethra: Male urethra is longer and passes through the prostate and penis; female urethra is shorter and opens anterior to the vaginal opening.
Physiology of Urine Storage and Voiding
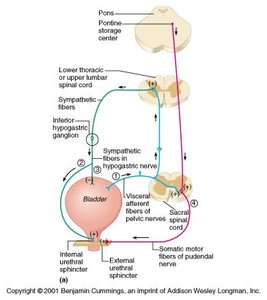
Bladder (Storage) Reflex
As urine accumulates, the bladder wall thins and rugae disappear. Sympathetic innervation keeps the internal sphincter closed and inhibits bladder contraction, allowing storage of urine.
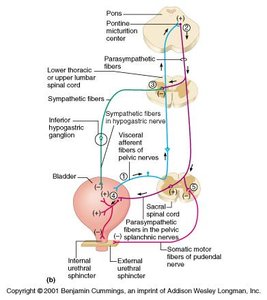
Micturition Reflex (Voiding)
When the bladder fills, stretch receptors in the detrusor muscle trigger increased parasympathetic activity, causing bladder contraction and internal sphincter relaxation. Voluntary relaxation of the external sphincter allows urination.
Parasympathetic stimulation: Contracts detrusor muscle
Somatic control: Pudendal nerve controls external sphincter
Renal Circulation and Nephron Structure
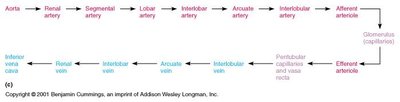
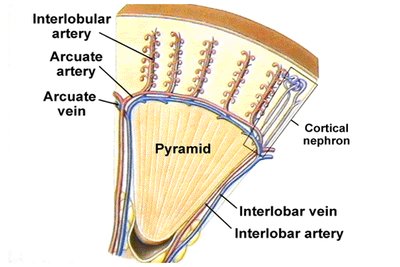
Renal Circulation
Blood enters the kidney via the renal artery, branches into smaller arteries and arterioles, and is filtered in the glomerulus. The arrangement of blood vessels supports filtration and reabsorption processes.
Glomerulus: Capillary tuft where filtration occurs
Peritubular capillaries and vasa recta: Surround nephron tubules for reabsorption and secretion
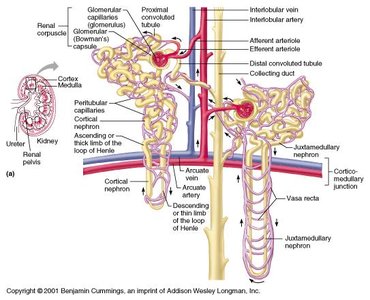
Nephron Structure and Function
The nephron is the functional unit of the kidney, responsible for filtering blood and forming urine. Each nephron consists of a renal corpuscle (glomerulus and Bowman’s capsule) and a renal tubule (PCT, loop of Henle, DCT, and collecting duct).
Cortical nephrons: Located mainly in the cortex
Juxtamedullary nephrons: Long loops of Henle extend into the medulla, important for concentrating urine
Urine Formation
Processes of Urine Formation
Urine formation involves four main processes: pressure filtration, reabsorption, secretion, and water reabsorption.
Pressure filtration: Blood pressure forces water and solutes from glomerulus into Bowman’s capsule
Reabsorption: Useful substances are reabsorbed from filtrate back into blood
Secretion: Additional wastes are actively transported into the tubule
Water reabsorption: Water is reabsorbed to concentrate urine
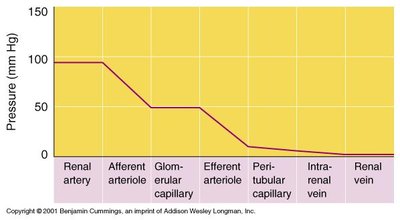
Glomerular Filtration
Filtration in the glomerulus is driven by blood pressure and facilitated by fenestrated capillaries and podocytes. The glomerular filtration rate (GFR) is the volume of filtrate produced per minute, typically 120–125 ml/min.
Filtration barrier: Endothelium, basement membrane, and podocyte slit pores
Forces opposing filtration: Osmotic pressure of blood proteins and hydrostatic pressure in Bowman’s capsule
Equation for Net Filtration Pressure (NFP):
Where: GHP = Glomerular hydrostatic pressure CHP = Capsular hydrostatic pressure COP = Colloid osmotic pressure
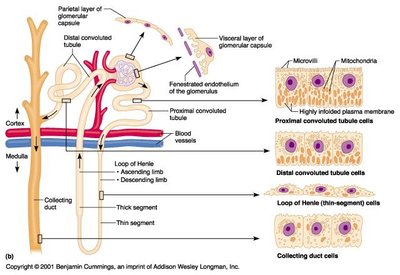
Tubular Reabsorption and Secretion
Most filtrate is reabsorbed in the proximal convoluted tubule (PCT), with further reabsorption and secretion occurring in the loop of Henle, distal convoluted tubule (DCT), and collecting duct (CD).
Passive and active transport: Na+ reabsorption drives co-transport of other substances
Transport maximum (Tm): Maximum rate of reabsorption for substances with carrier proteins
Secretion: Active transport of H+, K+, and drugs into the tubule
Loop of Henle and Counter-Current Mechanism
The loop of Henle acts as a counter-current multiplier, creating a high osmotic gradient in the medulla. This allows the kidney to produce concentrated urine when necessary.
Descending limb: Permeable to water, not salt
Ascending limb: Permeable to salt, not water
Vasa recta: Maintains osmotic gradient via counter-current exchange
Hormonal Regulation of Kidney Function
Antidiuretic Hormone (ADH)
ADH increases water reabsorption in the collecting duct, producing a low-volume, concentrated urine. It is released in response to dehydration or increased plasma osmolality.
Renin-Angiotensin-Aldosterone System (RAAS)
The juxtaglomerular apparatus releases renin in response to low blood pressure, activating the RAAS pathway. This leads to increased aldosterone, Na+ reabsorption, water retention, and blood pressure.
Renin: Converts angiotensinogen to angiotensin I
Angiotensin II: Vasoconstriction and stimulates aldosterone release
Aldosterone: Increases Na+ reabsorption in DCT
Acid-Base Balance
The kidneys regulate blood pH by controlling the secretion and reabsorption of H+ and HCO3- in the PCT and DCT.
Secretion of H+: Lowers blood pH
Reabsorption of HCO3-: Raises blood pH
Summary Table: Main Functions of the Urinary System
Function | Location | Mechanism |
|---|---|---|
Filtration | Glomerulus | Blood pressure forces plasma into Bowman’s capsule |
Reabsorption | PCT, Loop of Henle, DCT, CD | Active and passive transport of water and solutes back to blood |
Secretion | PCT, DCT | Active transport of wastes from blood to tubule |
Water Conservation | Loop of Henle, CD | Counter-current mechanism, ADH action |
Acid-Base Balance | PCT, DCT | Secretion/reabsorption of H+ and HCO3- |
