 Back
BackThe Urinary System: Structure and Function
Study Guide - Smart Notes

The Urinary System
Overview and Gross Anatomy
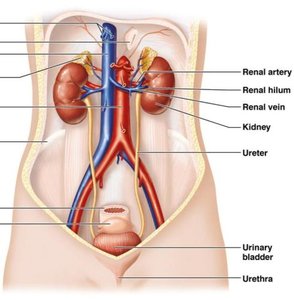
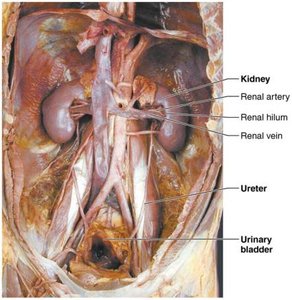
The urinary system is essential for maintaining the body's internal environment by regulating water, solute concentrations, and removing metabolic wastes. It consists of the kidneys, ureters, urinary bladder, and urethra.
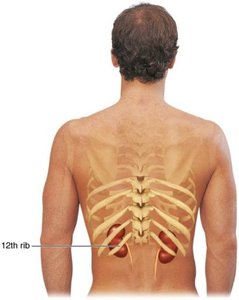
Kidneys: Major excretory organs, located retroperitoneally between T12 and L5 vertebrae. The right kidney is slightly lower due to the liver.
Ureters: Tubes that transport urine from the kidneys to the urinary bladder.
Urinary bladder: Temporary storage reservoir for urine.
Urethra: Tube that conveys urine out of the body.
Functions of the Kidneys
Regulate total water volume and solute concentration.
Regulate ion concentrations in extracellular fluid.
Maintain long-term acid-base balance.
Excrete metabolic wastes, toxins, and drugs.
Produce erythropoietin (stimulates RBC production) and renin (regulates blood pressure).
Activate vitamin D and perform gluconeogenesis if needed.
Kidney Structure
Location and External Anatomy
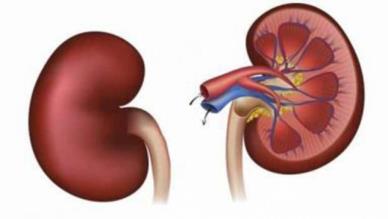
The kidneys are retroperitoneal, lying between the dorsal body wall and the parietal peritoneum. The adrenal glands sit atop each kidney. The medial surface is concave, with the renal hilum serving as the entry/exit for vessels, nerves, and the ureter.
Supportive Tissue Layers
Renal fascia: Anchors the kidney to surrounding structures.
Perirenal fat capsule: Cushions the kidney.
Fibrous capsule: Transparent layer that prevents infection spread.
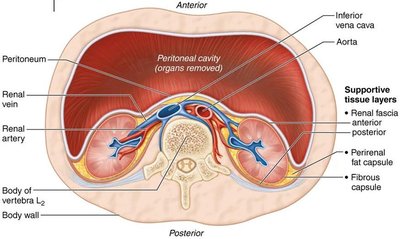
Internal Gross Anatomy
Renal cortex: Superficial, granular-appearing region.
Renal medulla: Deep region with cone-shaped renal pyramids separated by renal columns.
Renal pelvis: Funnel-shaped tube continuous with the ureter, collecting urine from major and minor calyces.
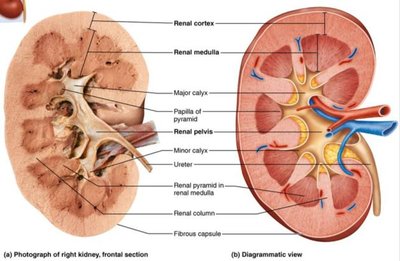
Blood Supply of the Kidneys
Renal Circulation
The kidneys receive about 25% of cardiac output. Blood flows through a series of arteries and veins, with the renal artery entering and the renal vein exiting at the hilum.
Arterial flow: Renal → Segmental → Interlobar → Arcuate → Cortical radiate arteries.
Venous flow: Cortical radiate → Arcuate → Interlobar → Renal veins (no segmental veins).
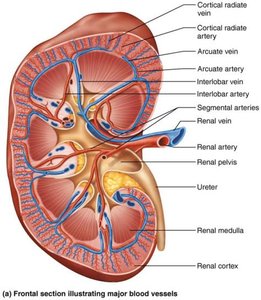
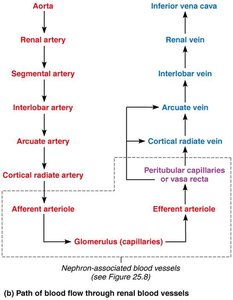
Nephrons: The Functional Units
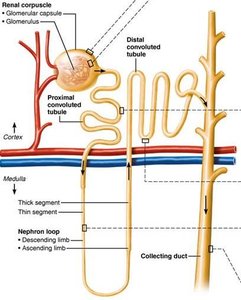
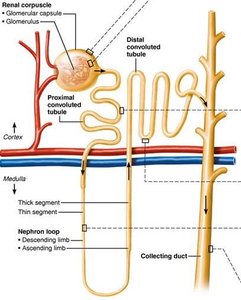
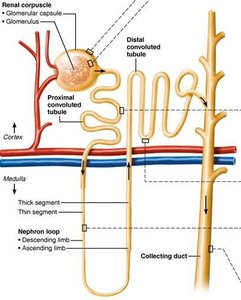
Structure of a Nephron
Each kidney contains over one million nephrons, which are responsible for urine formation. Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Includes the glomerulus (a tuft of capillaries) and the glomerular (Bowman's) capsule.
Renal tubule: Composed of the proximal convoluted tubule (PCT), nephron loop (loop of Henle), distal convoluted tubule (DCT), and collecting duct.
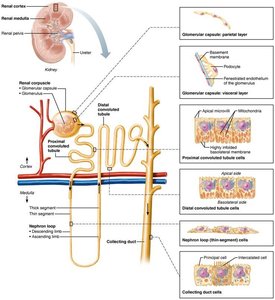
Renal Corpuscle: Glomerulus and Capsule
Glomerulus: Fenestrated capillaries that allow efficient filtrate formation.
Glomerular capsule: Surrounds the glomerulus and consists of two layers:
Parietal layer: Simple squamous epithelium.
Visceral layer: Podocytes with foot processes and filtration slits.
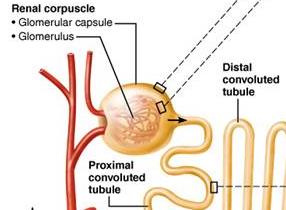
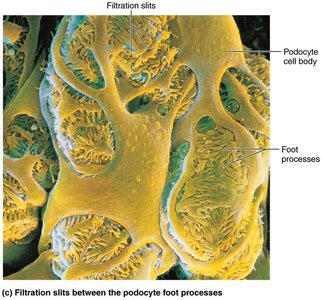
Renal Tubule Segments
Proximal convoluted tubule (PCT): Cuboidal cells with microvilli for reabsorption and secretion.
Nephron loop (Loop of Henle): Descending limb (permeable to water) and ascending limb (permeable to solutes).
Distal convoluted tubule (DCT): Cuboidal cells, mainly for secretion.
Collecting duct: Receives filtrate from multiple nephrons; principal cells regulate water/Na+ balance, intercalated cells regulate acid-base balance.
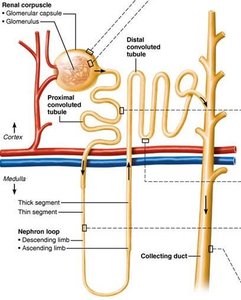
Types of Nephrons
Cortical nephrons: 85% of nephrons, almost entirely in the cortex.
Juxtamedullary nephrons: Long loops deeply invade the medulla, crucial for producing concentrated urine.
Nephron Capillary Beds
Glomerulus: High-pressure capillary bed for filtration.
Peritubular capillaries: Low-pressure, adapted for absorption.
Vasa recta: Long, thin-walled vessels associated with juxtamedullary nephrons, important for urine concentration.
Juxtaglomerular Complex (JGC)
The JGC regulates filtrate formation and blood pressure. It consists of macula densa cells (sense NaCl), granular cells (release renin), and extraglomerular mesangial cells (signal transmission).
Urine Formation
Three Major Processes
Glomerular filtration: Passive process producing cell- and protein-free filtrate.
Tubular reabsorption: Selective return of 99% of substances from filtrate to blood.
Tubular secretion: Selective movement of substances from blood to filtrate.
Glomerular Filtration
Driven by hydrostatic pressure; no energy required.
Filtration membrane allows passage of water and small solutes, but not proteins or cells.
Pressures Affecting Filtration
Outward pressure: Hydrostatic pressure in glomerular capillaries (HPgc, ~55 mm Hg).
Inward pressures: Hydrostatic pressure in capsular space (HPcs, 15 mm Hg) and colloid osmotic pressure in capillaries (OPgc, 30 mm Hg).
Net filtration pressure (NFP): Outward minus inward pressures; determines glomerular filtration rate (GFR).
Glomerular Filtration Rate (GFR)
Normal GFR: 120–125 ml/min.
Directly proportional to NFP, surface area, and membrane permeability.
Regulation of GFR
Intrinsic controls (renal autoregulation): Myogenic mechanism and tubuloglomerular feedback maintain GFR within 80–180 mm Hg MAP.
Extrinsic controls: Sympathetic nervous system and renin-angiotensin-aldosterone mechanism regulate systemic blood pressure and GFR.
Tubular Reabsorption and Secretion
Tubular Reabsorption
Most nutrients, water, and ions are reabsorbed, mainly in the PCT.
Reabsorption occurs via transcellular (through cells) or paracellular (between cells) routes.
Transport maximum (Tm) limits reabsorption based on carrier availability.
Hormonal regulation: Aldosterone increases Na+ reabsorption; ADH increases water reabsorption in collecting ducts.
Tubular Secretion
Active process, mainly in the PCT.
Removes drugs, wastes, excess ions, and helps maintain blood pH.
Regulation of Urine Concentration and Volume
Countercurrent Mechanisms
Countercurrent multiplier: Interaction of filtrate flow in nephron loops creates a medullary osmotic gradient.
Countercurrent exchanger: Vasa recta preserves the gradient by exchanging water and solutes.
Allows kidneys to produce concentrated urine when dehydrated or dilute urine when overhydrated.
Clinical Aspects
Urinalysis and Renal Function
Urinalysis: Examines urine for disease or illegal substances.
Renal clearance: Volume of plasma cleared of a substance per minute; used to assess GFR and kidney health.
Chronic renal disease: GFR < 60 ml/min for 3 months.
Renal failure: GFR < 15 ml/min; requires dialysis or transplant.
Urine Composition and Properties
95% water, 5% solutes (urea, uric acid, creatinine, ions).
Normally clear, yellow, slightly acidic.
Abnormal substances (e.g., glucose, proteins, blood) indicate pathology.
Transport, Storage, and Elimination of Urine
Ureters
Slender tubes conveying urine from kidneys to bladder.
Three layers: mucosa (transitional epithelium), muscularis (smooth muscle for peristalsis), adventitia (fibrous connective tissue).
Urinary Bladder
Muscular sac for temporary urine storage.
Wall layers: mucosa, detrusor muscle (three smooth muscle layers), adventitia, and peritoneum.
Trigone: triangular area prone to infection.
Capacity: ~500 ml (can double if needed).
Urethra
Muscular tube draining the bladder.
Internal urethral sphincter (involuntary, smooth muscle) and external urethral sphincter (voluntary, skeletal muscle).
Female urethra: 3–4 cm; Male urethra: 20 cm, three regions (prostatic, intermediate, spongy).
Micturition (Urination)
Requires contraction of detrusor muscle, opening of internal and external sphincters.
Infants: reflexive; Adults: voluntary control via brain centers.
Disorders
Urinary incontinence: Involuntary leakage, often due to weak pelvic muscles.
Urinary retention: Inability to expel urine, often due to prostate enlargement or anesthesia; treated with catheterization.
