 Back
BackThe Respiratory System: Structure, Function, and Regulation
Study Guide - Smart Notes

The Respiratory System: Overview and Organization
Introduction to the Respiratory System
The respiratory system is essential for gas exchange, supplying oxygen to body tissues and removing carbon dioxide produced by cellular metabolism. It consists of anatomical structures that facilitate the movement, filtration, and exchange of gases between the atmosphere and the bloodstream.
Oxygen is obtained from the air via diffusion across lung surfaces.
Carbon dioxide is transported from tissues to the lungs for exhalation.
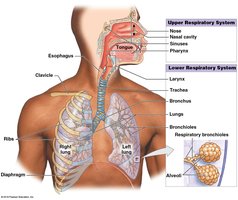
Structural Organization of the Respiratory System
Upper and Lower Respiratory Tracts
The respiratory system is divided into upper and lower tracts, each with specialized structures and functions.
Upper respiratory tract: Nose, nasal cavity, sinuses, pharynx
Lower respiratory tract: Larynx, trachea, bronchi, bronchioles, alveoli
Respiratory Mucosa and Defense System
The respiratory mucosa lines the conducting portions of the system, consisting of an epithelium and underlying areolar tissue (lamina propria). It plays a critical role in filtering, humidifying, and protecting the respiratory surfaces.
Mucous glands and mucous cells produce mucus to trap particles and pathogens.
Cilia sweep mucus toward the pharynx for swallowing.
Alveolar macrophages engulf small particles that reach the alveoli.
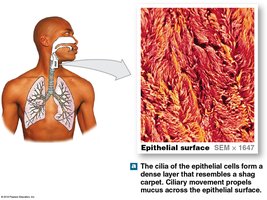
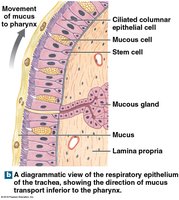
Histology of the Respiratory Tract
Respiratory Epithelium
The respiratory epithelium varies along the tract but is primarily pseudostratified ciliated columnar epithelium in the upper regions, transitioning to simple squamous epithelium in the alveoli for efficient gas exchange.
Lamina propria: Areolar tissue supporting the epithelium.
Mucous glands: Present in upper regions, absent in bronchioles.
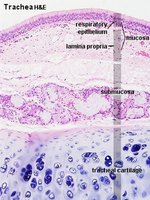
Functional Anatomy of the Airways
Trachea and Bronchial Tree
The trachea is a flexible tube supported by C-shaped cartilages, branching into the right and left main bronchi, which further divide into smaller bronchi and bronchioles.
Bronchioles lack cartilage and are dominated by smooth muscle, allowing regulation of airflow.
Terminal bronchioles mark the end of the conducting zone and lead to respiratory bronchioles and alveoli.
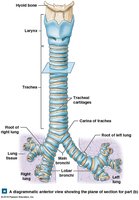
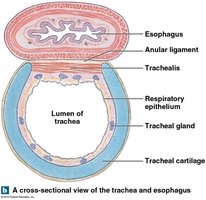
Bronchopulmonary Segments and Alveoli
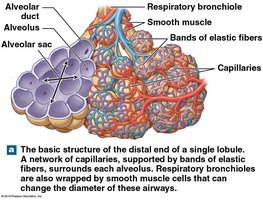
The lungs are divided into lobes and bronchopulmonary segments, each supplied by its own bronchus and blood vessels. The alveoli are the primary sites of gas exchange, surrounded by capillaries and elastic fibers.
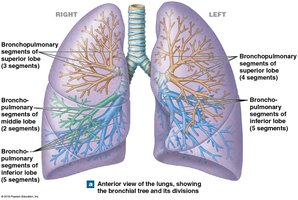
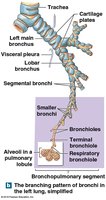
Alveolar Structure and Gas Exchange
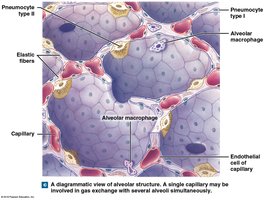
Alveolar Organization
Alveoli are lined by simple squamous epithelium (type I pneumocytes) and contain type II pneumocytes that secrete surfactant, reducing surface tension and preventing alveolar collapse.
Alveolar macrophages patrol and remove debris.
Surfactant is essential for maintaining open alveoli, especially in premature infants.
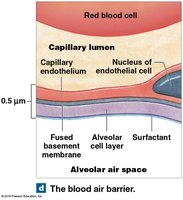
The Blood-Air Barrier
Gas exchange occurs across the blood-air barrier, which consists of the alveolar epithelium, fused basement membrane, and capillary endothelium. The thinness of this barrier allows rapid diffusion of O2 and CO2.
Pleura and Pulmonary Circulation
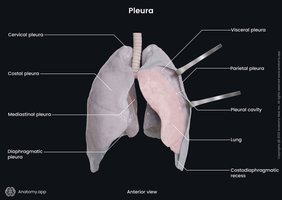
Pleural Cavities and Membranes
Each lung is enclosed in a pleural cavity lined by a double-layered serous membrane: the parietal pleura (lining the thoracic wall) and the visceral pleura (covering the lung surface). Pleural fluid lubricates the space between these layers, reducing friction during breathing.
Mechanics of Breathing
Pulmonary Ventilation and Boyle's Law
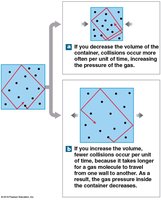
Pulmonary ventilation is the physical movement of air into and out of the lungs, driven by pressure differences created by changes in thoracic volume. According to Boyle's Law:
Where P is pressure and V is volume. As thoracic volume increases, pressure decreases, drawing air in; as volume decreases, pressure increases, pushing air out.
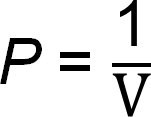
Muscles of Respiration
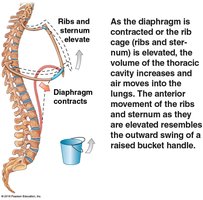
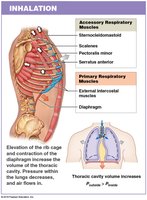
Inhalation is primarily driven by the diaphragm and external intercostal muscles. Exhalation is usually passive but can involve internal intercostals and abdominal muscles during forced breathing.
Accessory muscles assist during deep or forced breathing.
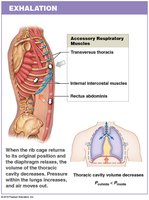
Pressure Changes and Lung Volumes
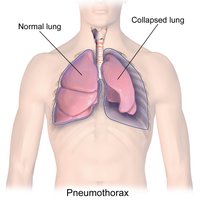
During the respiratory cycle, intrapulmonary pressure fluctuates slightly around atmospheric pressure, while intrapleural pressure remains negative, helping keep the lungs inflated. Pneumothorax (air in the pleural cavity) can cause lung collapse (atelectasis).
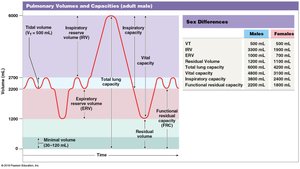
Respiratory Volumes and Capacities
Pulmonary Volumes
Key volumes measured in respiratory physiology include:
Tidal volume (VT): Air moved in a single breath
Expiratory reserve volume (ERV): Air exhaled after normal exhalation
Residual volume: Air remaining after maximal exhalation
Inspiratory reserve volume (IRV): Air inhaled after normal inhalation
Respiratory Capacities
Inspiratory capacity: VT + IRV
Functional residual capacity (FRC): ERV + residual volume
Vital capacity: ERV + VT + IRV
Total lung capacity: Vital capacity + residual volume
Gas Exchange: Physical Principles
Partial Pressures and Gas Laws
Gas exchange depends on differences in partial pressures of O2 and CO2 (Dalton's Law) and the solubility of gases (Henry's Law). Gases diffuse from areas of higher to lower partial pressure.
Dalton's Law: Total pressure is the sum of partial pressures of individual gases.
Henry's Law: The amount of gas dissolved in a liquid is proportional to its partial pressure.
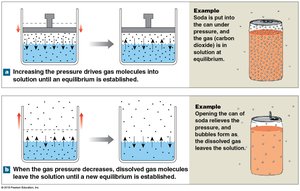
Efficiency of Gas Exchange
Gas exchange is efficient due to substantial partial pressure gradients, short diffusion distances, lipid solubility of gases, large surface area, and coordinated blood and airflow.
Oxygen and Carbon Dioxide Transport
Hemoglobin and Oxygen Transport
Oxygen is transported primarily by binding to hemoglobin (Hb) in red blood cells, forming oxyhemoglobin (HbO2) in a reversible reaction:
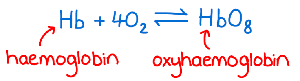
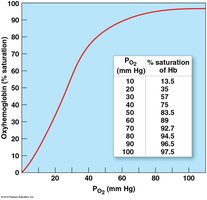
Oxygen-Hemoglobin Saturation Curve
The percentage of heme units bound to oxygen is affected by PO2, pH, temperature, and metabolic activity. Lower pH or higher temperature shifts the curve right, promoting O2 release.
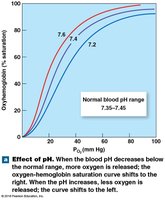
Carbon Dioxide Transport
CO2 is transported in three forms:
As bicarbonate ions (HCO3-) after conversion to carbonic acid
Bound to hemoglobin
Dissolved in plasma
Control of Respiration
Neural Regulation
Respiratory rate and depth are regulated by centers in the medulla oblongata and pons, responding to chemoreceptor, baroreceptor, and stretch receptor input. The dorsal respiratory group (DRG) controls inspiration, while the ventral respiratory group (VRG) is active during forced breathing.
Chemoreceptor and Baroreceptor Reflexes
Central and peripheral chemoreceptors monitor CO2, O2, and pH, adjusting ventilation accordingly. Baroreceptors in the aorta and carotid sinuses respond to blood pressure changes, influencing respiratory rate.
Age-Related Changes and System Integration
Effects of Aging
Aging leads to decreased lung elasticity, reduced vital capacity, and increased susceptibility to respiratory diseases such as emphysema. Coordination with the cardiovascular system is essential for maintaining homeostasis of O2 and CO2 levels.
Summary Table: Key Respiratory Volumes and Capacities
Volume/Capacity | Definition |
|---|---|
Tidal Volume (VT) | Air moved in a single breath |
Expiratory Reserve Volume (ERV) | Air exhaled after normal exhalation |
Inspiratory Reserve Volume (IRV) | Air inhaled after normal inhalation |
Residual Volume | Air remaining after maximal exhalation |
Vital Capacity | ERV + VT + IRV |
Total Lung Capacity | Vital Capacity + Residual Volume |
