 Back
BackControl of Microbial Growth and Antimicrobial Strategies
Study Guide - Smart Notes

Control of Microbial Growth
Introduction to Microbial Control
Microorganisms are ubiquitous and can be found on nearly all surfaces, including those in homes, hospitals, and food environments. While some microbes are essential and beneficial, others can cause disease or spoilage. The control of microbial growth is crucial in various settings to ensure safety and health.
Microbial diversity: Includes bacteria, fungi, viruses, and more.
Not all microbes need removal: Some are beneficial and necessary for health (e.g., normal microbiota).
Removal depends on: Microbe type, resistance, and context (e.g., food, medical, home).
Microbiota and Environmental Interaction
Humans are constantly interacting with their environment, exchanging microbes with surfaces and other individuals. The human microbiota plays a significant role in health and disease, and environmental surfaces can act as reservoirs for microbial transfer.
Microbiota follows individuals: Studies show that families transfer their microbiota to new homes, rapidly colonizing new environments.
Environmental surfaces: Non-sterile surfaces can harbor diverse microbial communities.


Methods of Microbial Control
Physical Methods: Heat and Cold
Physical methods such as heat and cold are commonly used to control microbial growth. The effectiveness depends on the type of microbe and the method applied.
Heat: High temperatures can kill or inactivate microbes. Key concepts include:
Thermal Death Point (TDP): Lowest temperature at which all microbes in a liquid suspension are killed in 10 minutes.
Thermal Death Time (TDT): Minimum time required to kill all microbes at a set temperature.
Cold: Freezing kills most cells but not all viruses or spores. Refrigeration slows microbial growth but does not kill microbes.

Chemical Methods: Disinfectants and Antiseptics
Chemical agents are widely used to control microbial populations on surfaces and living tissues. The choice of chemical depends on the application and the type of microbe targeted.
Disinfectants: Used on inanimate objects to kill or inhibit microbes (e.g., bleach, alcohol).
Antiseptics: Used on living tissues to reduce microbial load (e.g., hydrogen peroxide, iodine).
Degerming: Physical removal of microbes from a surface, often by washing or scrubbing.
Germicides/Microbicides: General terms for agents that kill microbes.
Microbiostatic agents: Inhibit microbial reproduction but do not kill (e.g., some antibiotics, diluted ethanol).

Special Microbial Forms: Endospores and Prions
Certain microbial forms, such as endospores and prions, are highly resistant to standard control methods and require specialized approaches.
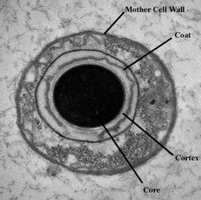
Endospores: Dormant, tough structures formed by some bacteria (e.g., Bacillus, Clostridium) that are resistant to heat, chemicals, and radiation.
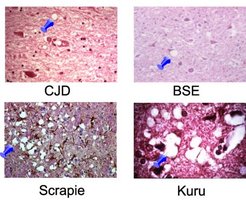
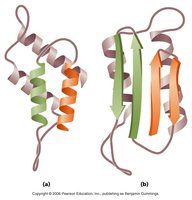
Prions: Infectious proteins that cause neurodegenerative diseases and are extremely resistant to denaturation and standard sterilization.
Indicators of Microbial Contamination
Visible signs such as bloated cans can indicate microbial contamination, often by gas-producing bacteria like Clostridium botulinum.
Bloated cans: Suggest the presence of gas-producing, potentially pathogenic microbes.

Applications and Importance of Microbial Control
Home and Food Safety
Proper sanitation and disinfection in the home, especially in kitchens and bathrooms, are essential for preventing foodborne illness and maintaining a healthy environment.
Disinfection: Commercial chemicals are generally sufficient for home use.
Safe cooking practices: Wash produce, keep meats frozen until use, and cook meats to appropriate temperatures (e.g., 155ºC or higher for safety).
Medical and Hospital Settings
In healthcare environments, strict microbial control is critical to prevent infections, especially in surgical and immunocompromised patients.
Sterilization: Required for surgical instruments, catheters, and implantable devices.
Aseptic technique: Includes hand hygiene, use of personal protective equipment (PPE), and environmental controls to prevent healthcare-associated infections (HAIs).
Antisepsis: Reducing microbial load on living tissues, such as skin, using chemical agents.
Mechanisms of Antimicrobial Action
Modes of Action
Antimicrobials can kill or inhibit microbes through various mechanisms, targeting essential cellular structures or functions.
Cell wall damage
Cytoplasmic membrane disruption
Disruption of cellular synthesis (e.g., DNA, RNA, proteins)
Inhibition or destruction of vital proteins
Examples of Chemical Agents
Alcohol: Denatures proteins and dissolves lipid membranes; must be diluted for optimal effectiveness.
Bleach (sodium hypochlorite): Denatures proteins; effective disinfectant.
Dyes: Crystal violet, methylene blue, and malachite green have antimicrobial properties but are often toxic and have narrow spectra.
Organic acids: Used in food preservation (e.g., acetic acid in pickling, propionic acid in bread).
Antimicrobial Drugs and Resistance
Antibiotics and Chemotherapeutics
Antibiotics are substances produced by microorganisms to inhibit or kill other microbes. Chemotherapeutics include both natural antibiotics and synthetic antimicrobial agents.
Penicillin: First purified antibiotic, targets bacterial cell wall synthesis.
Sulfonamides: Early synthetic antibacterial agents, inhibit folic acid synthesis.
Broad vs. narrow spectrum: Broad-spectrum drugs target a wide range of microbes; narrow-spectrum drugs are specific to certain pathogens.
Mechanisms of Antibiotic Action
Cell wall synthesis inhibition (e.g., penicillins, vancomycin)
Protein synthesis inhibition (e.g., tetracyclines, macrolides)
DNA/RNA synthesis inhibition (e.g., quinolones, rifamycins)
Disruption of cell membrane (e.g., polymyxins)
Folic acid synthesis inhibition (e.g., sulfonamides)
Antibiotic Resistance
Antibiotic resistance arises through genetic changes in bacteria, often accelerated by misuse or overuse of antibiotics. Resistance genes can be transferred horizontally between bacteria.
Mechanisms: Enzymatic inactivation, target modification, efflux pumps, reduced permeability.
Horizontal gene transfer: Transformation, transduction, conjugation.
Multi-drug resistance (MDR): Bacteria resistant to multiple antibiotics, posing significant treatment challenges.
Testing Antimicrobial Effectiveness
Minimum Inhibitory Concentration (MIC): Lowest concentration of a drug that inhibits visible growth of a microbe.
Kirby-Bauer Disk Diffusion Test: Measures the effectiveness of antibiotics by the size of the zone of inhibition around a drug-impregnated disk on a bacterial lawn.
Summary Table: Key Terms and Definitions
Term | Definition |
|---|---|
Sterilization | Complete destruction or removal of all forms of microbial life, including spores. |
Disinfection | Destruction of vegetative pathogens on inanimate objects. |
Antisepsis | Destruction of vegetative pathogens on living tissue. |
Degerming | Physical removal of microbes from a limited area. |
Sanitization | Lowering microbial counts to safe public health levels. |
Microbiostatic | Agent that inhibits microbial growth but does not kill. |
Bactericidal | Agent that kills bacteria. |
Broad-spectrum | Antimicrobial effective against a wide range of organisms. |
Narrow-spectrum | Antimicrobial effective against specific organisms. |
