 Back
BackDisorders of the Immune System: Hypersensitivities, Autoimmune Diseases, and Immunodeficiencies
Study Guide - Smart Notes

Disorders of the Immune System
Overview
The immune system is essential for defending the body against pathogens, but it can sometimes malfunction, leading to disorders such as hypersensitivities, autoimmune diseases, and immunodeficiencies. These disorders can result in tissue damage, chronic disease, or increased susceptibility to infections.
Hypersensitivities
Definition and General Concepts
Hypersensitivity refers to an antigenic response that leads to undesirable effects in the host.
It occurs when an individual is sensitized by previous exposure to an antigen (often called an allergen).
There are four major types of hypersensitivity reactions: anaphylactic, cytotoxic, immune complex, and delayed cell-mediated.
The hygiene hypothesis suggests that reduced exposure to pathogens in childhood may lower immune tolerance, increasing the risk of allergies.
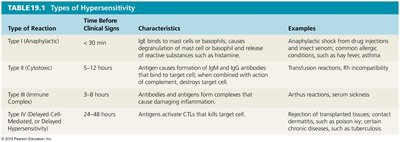
Type of Reaction | Time Before Clinical Signs | Characteristics | Examples |
|---|---|---|---|
Type I (Anaphylactic) | < 30 min | IgE binds to mast cells or basophils, causing degranulation and release of histamine and other mediators | Anaphylactic shock, asthma, hay fever, some food allergies |
Type II (Cytotoxic) | 5–12 hours | Antibodies (IgG or IgM) and complement cause cell lysis or damage | Transfusion reactions, hemolytic disease of the newborn |
Type III (Immune Complex) | 3–8 hours | Immune complexes deposit in tissues, activating complement and causing inflammation | Serum sickness, glomerulonephritis |
Type IV (Delayed Cell-Mediated) | 24–48 hours | T cells and macrophages mediate tissue damage | Contact dermatitis, transplant rejection |
Type I (Anaphylactic) Reactions
Type I hypersensitivity occurs within minutes of re-exposure to an allergen. It involves IgE antibodies, mast cells, and basophils.
Antigens combine with IgE antibodies, which are bound to mast cells and basophils.
Degranulation releases mediators such as histamine (causing vasodilation and increased capillary permeability) and leukotrienes (causing bronchospasm).
Systemic anaphylaxis can lead to shock and requires immediate treatment with epinephrine.
Localized anaphylaxis is associated with inhaled or ingested allergens, causing symptoms like hives, hay fever, and asthma.
Food Allergies
Not all food reactions are true hypersensitivities; some are intolerances (e.g., lactose intolerance).
Eight foods account for most food allergies: eggs, peanuts, tree nuts, milk, soy, fish, wheat, and peas.
Hives are a common symptom of food allergies.

Prevention and Diagnosis
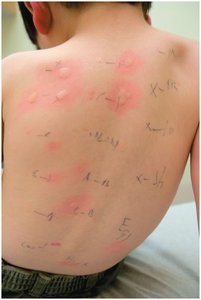
Skin testing involves inoculating antigens beneath the epidermis to observe for a rapid inflammatory reaction (wheal).
Desensitization therapy involves repeated, increasing doses of antigen to induce IgG production, which competes with IgE for antigen binding.
Type II (Cytotoxic) Reactions
Type II hypersensitivity involves antibody-mediated destruction of cells, often through complement activation.
IgG or IgM antibodies bind to antigens on cell surfaces, activating complement and causing cell lysis or phagocytosis.
Common examples include transfusion reactions and hemolytic disease of the newborn (HDNB).
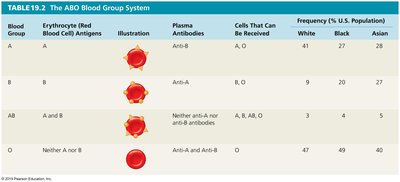
ABO Blood Group System
Antibodies form against carbohydrate antigens (A, B, or both) on red blood cells (RBCs).
Transfusion of incompatible blood leads to cell lysis.
Blood Group | RBC Antigens | Plasma Antibodies | Cells That Can Be Received | Frequency (%) |
|---|---|---|---|---|
A | A | Anti-B | A, O | White: 41, Black: 27, Asian: 28 |
B | B | Anti-A | B, O | White: 9, Black: 20, Asian: 27 |
AB | A and B | Neither anti-A nor anti-B | A, B, AB, O | White: 3, Black: 4, Asian: 5 |
O | Neither A nor B | Anti-A and Anti-B | O | White: 47, Black: 49, Asian: 40 |
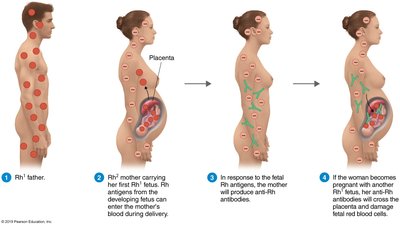
Rh Blood Group System and Hemolytic Disease of the Newborn (HDNB)
Rh antigen (Rh+) is present in 85% of the population.
Rh– mothers exposed to Rh+ fetal blood can develop anti-Rh antibodies, which may attack fetal RBCs in subsequent pregnancies.
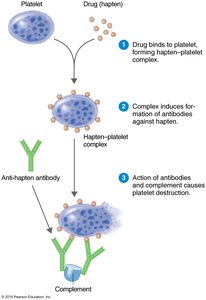
Drug-Induced Cytotoxic Reactions
Some drugs can bind to platelets or white blood cells, forming antigenic complexes that trigger immune destruction (e.g., thrombocytopenic purpura, agranulocytosis, hemolytic anemia).
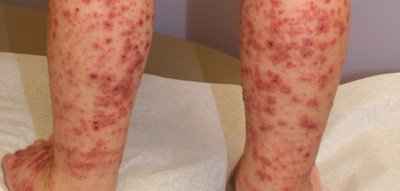
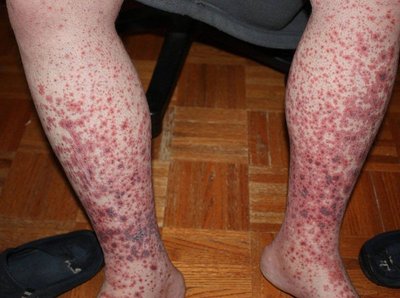
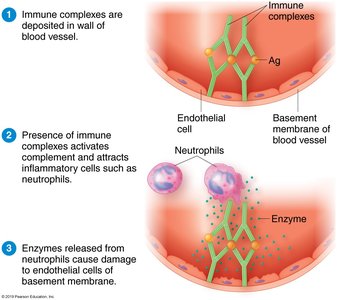
Type III (Immune Complex) Reactions
Type III hypersensitivity is caused by immune complexes (antigen-antibody complexes) that deposit in tissues, activating complement and causing inflammation.
Common sites include blood vessel walls and glomeruli of the kidneys.
Examples include glomerulonephritis and serum sickness.
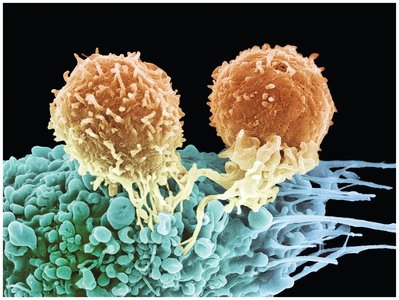
Type IV (Delayed Cell-Mediated) Reactions
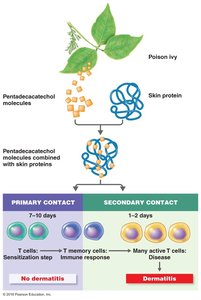
Type IV hypersensitivity is mediated by T cells rather than antibodies and is characterized by a delayed response (24–48 hours).
Antigens are processed by macrophages and presented to T cells, leading to cytokine release and tissue damage upon re-exposure.
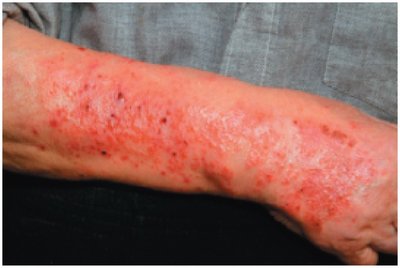
Examples include allergic contact dermatitis (e.g., poison ivy), transplant rejection, and some chronic diseases.
Autoimmune Diseases
Overview and Mechanisms
Autoimmune diseases occur when the immune system attacks self-antigens, leading to tissue and organ damage.
They are more common in females and may be linked to genetic, hormonal, or environmental factors.
Autoimmunity results from loss of self-tolerance, possibly due to failure of thymic selection or autoantibody production.
Three general types: cytotoxic, immune complex, and cell-mediated autoimmune diseases.
Cytotoxic Autoimmune Reactions
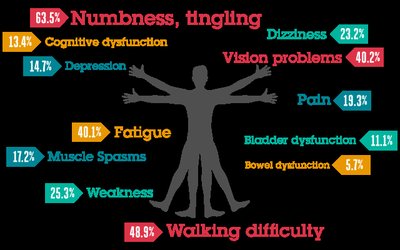
Multiple Sclerosis (MS): T cells, autoantibodies, and macrophages attack the myelin sheath in the central nervous system, causing neurological symptoms and scarring.
Genetic susceptibility and Epstein-Barr virus (EBV) infection are associated with MS.
Immune Complex Autoimmune Reactions
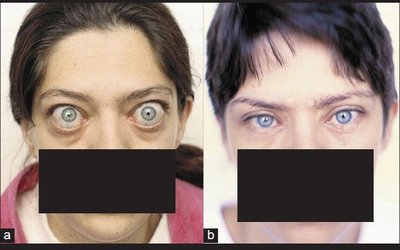
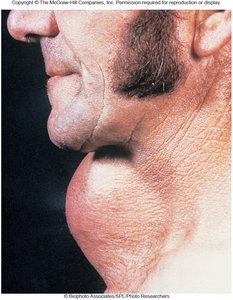
Graves' Disease: Abnormal antibodies mimic thyroid-stimulating hormone (TSH), causing overproduction of thyroid hormones. Symptoms include increased heart rate, anxiety, weight loss, and goiter.
Myasthenia Gravis: Antibodies block acetylcholine receptors at neuromuscular junctions, leading to muscle weakness and fatigue.
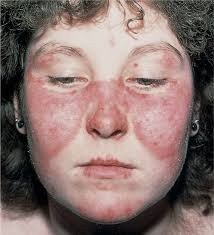
Systemic Lupus Erythematosus (SLE): Autoantibodies target cell components, forming immune complexes that deposit in tissues, especially the kidneys.
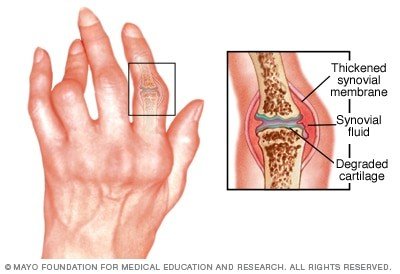
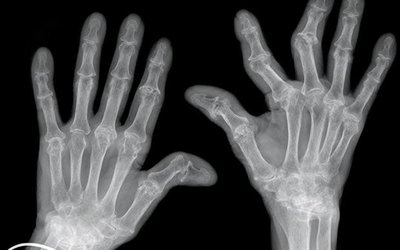
Rheumatoid Arthritis: Immune complexes (IgM and IgG) deposit in joints, causing chronic inflammation and joint damage.
Cell-Mediated Autoimmune Reactions
Type 1 Diabetes Mellitus: T cells destroy insulin-producing β-cells in the pancreas.
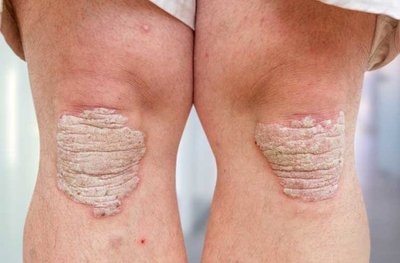
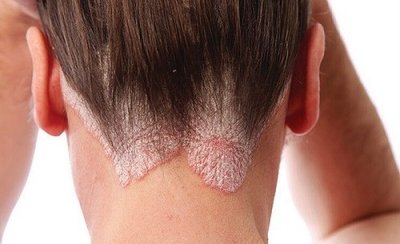
Psoriasis: T helper cells and cytokines (e.g., TNF-α) cause chronic skin inflammation, resulting in red, scaly plaques.
Reactions Related to the Human Leukocyte Antigen (HLA) Complex
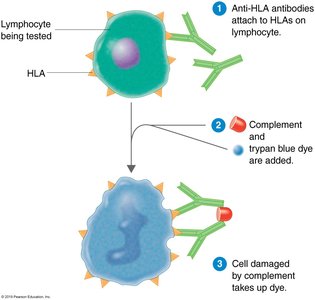
Transplantation and HLA Typing
Transplanted tissues are recognized as foreign and may be attacked by the recipient's immune system.
Matching HLA (MHC class I) and ABO blood groups is critical to reduce rejection risk.
Some HLA types are associated with increased susceptibility to certain diseases.
Transplant Rejection and Privileged Sites
Transplants to immune-privileged sites (e.g., cornea) or using privileged tissues (e.g., decellularized heart valves) are less likely to be rejected.
Stem Cells
Types and Applications
Stem cells are undifferentiated cells capable of giving rise to various cell types.
Embryonic stem cells (pluripotent) can generate all cell types and are harvested from blastocysts.
Adult stem cells (multipotent) are more limited and can only differentiate into a specific family of cells.
Stem cells are used in regenerative medicine to repair or replace damaged tissues and organs.
