 Back
BackInfection, Diseases, and Epidemiology: Microbiology Study Notes
Study Guide - Smart Notes

Symbiotic Relationships and Normal Microbiota
Symbiosis and Human Microbiota
Symbiosis refers to the close association between two different biological species, often involving microorganisms and their hosts. In humans, symbiotic relationships with microbiota are essential for health and disease prevention.
Resident microbiota: Microorganisms that are consistently present on body surfaces throughout life, typically without causing disease.
Transient microbiota: Microorganisms that temporarily colonize the body but do not persist due to competition, immune responses, or environmental changes.
Types of Symbiotic Relationships:
Type | Effect on Organism 1 | Effect on Organism 2 | Example |
|---|---|---|---|
Mutualism | Benefits | Benefits | Bacteria in human colon |
Commensalism | Benefits | Neither benefits nor is harmed | Mites in human hair follicles |
Amensalism | Is harmed | Neither benefits nor is harmed | Fungus secreting antibiotic inhibiting bacteria |
Parasitism | Benefits | Is harmed | Mycobacterium tuberculosis in human lung |
Acquisition of Normal Microbiota: Humans are generally free of microorganisms in the womb. Colonization begins during birth and continues in the first months of life.
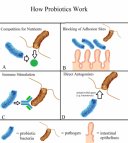
Opportunistic Pathogens
Normal flora can become pathogenic under certain conditions, such as immune suppression, changes in normal flora, or introduction into unusual body sites.
Immune suppression: Weakening of host defenses allows opportunists to cause disease.
Changes in normal flora: Antibiotic use or illness can disrupt the balance, allowing overgrowth of harmful microbes.
Unusual site introduction: Microbes entering sterile body sites may cause infection.
Chain of Infection and Disease Transmission
Contamination, Infection, and Disease
Contamination is the presence of microbes on or in the body. Infection occurs when pathogens evade defenses, multiply, and establish themselves. Disease results when infection leads to altered body function (morbidity).
Contamination ≠ Infection ≠ Disease
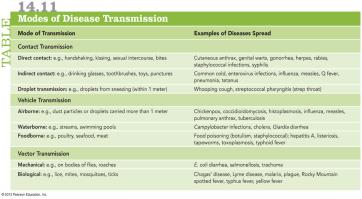
Modes of Disease Transmission
Pathogens are transmitted from reservoirs or portals of exit to new hosts via three main routes:
Contact transmission: Direct (person-to-person), indirect (fomites), or droplet (coughing, sneezing).
Vehicle transmission: Airborne (aerosols), waterborne (fecal-oral), or foodborne (contaminated food).
Vector transmission: Biological (biting arthropods) or mechanical (passive transfer by insects).
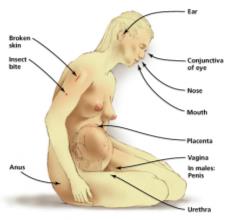
Portals of Entry and Exit
Major Portals of Entry
Pathogens enter the body through specific sites:
Skin: Through cuts, abrasions, or by burrowing/digesting outer layers.
Mucous membranes: Lining respiratory, gastrointestinal, and urogenital tracts; provide moist environments for pathogens.
Placenta: Usually a barrier, but some pathogens can cross and infect the fetus (e.g., syphilis, HIV).
Parenteral route: Direct deposition into tissues via punctures, bites, or surgery (not a true portal but circumvents others).
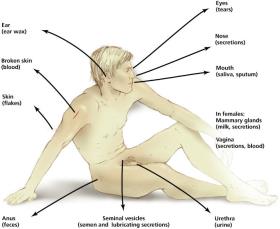
Portals of Exit
Pathogens leave the host through similar routes as entry, often in secretions or excretions (e.g., saliva, feces, blood).
Reservoirs of Infection
Types of Reservoirs
Animal reservoirs: Zoonoses are diseases naturally spread from animals to humans (e.g., rabies, influenza).
Human carriers: Infected individuals who may be asymptomatic but can transmit pathogens.
Nonliving reservoirs: Soil, water, and food contaminated with infectious agents.
Etiology and Manifestations of Disease
Etiology and Koch’s Postulates
Etiology is the study of disease causation. Koch’s postulates are criteria to prove a specific pathogen causes a disease.
Infection: Invasion and multiplication of pathogens in the host.
Disease: Results when infection alters normal body functions.
Signs, Symptoms, and Syndromes
Symptoms: Subjective characteristics felt only by the patient (e.g., pain, fatigue).
Signs: Objective, measurable changes (e.g., fever, rash).
Syndrome: Group of signs and symptoms that characterize a disease.
Asymptomatic: Infections without symptoms but may have signs.
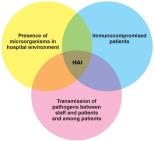
Nosocomial (Healthcare-Associated) Infections
Types and Control
Exogenous: Acquired from the healthcare environment.
Endogenous: Arise from normal microbiota due to factors in the healthcare setting.
Iatrogenic: Result from medical procedures.
Superinfections: Occur when antimicrobial drugs reduce normal flora, allowing other microbes to thrive.
Prevention: Handwashing is the most effective method to reduce HAIs.
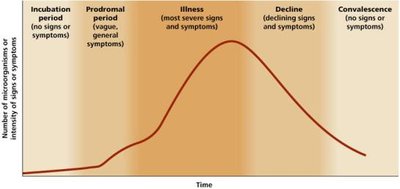
Stages of Infectious Diseases
The Disease Process
Many infections follow a five-stage sequence:
Incubation period: Time between infection and appearance of symptoms.
Prodromal period: Short period of mild, general symptoms.
Illness: Most severe signs and symptoms.
Decline: Signs and symptoms subside as immune response/treatment occurs.
Convalescence: Recovery; no signs or symptoms remain.
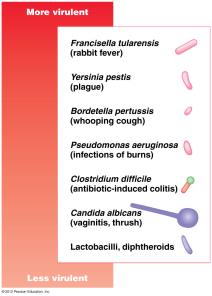
Virulence Factors
Determinants of Pathogenicity
Virulence is the degree of pathogenicity, determined by several factors:
Biofilms: Communities of microbes that are highly resistant to immune responses and antibiotics.
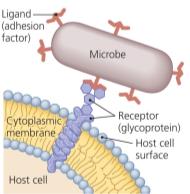
Adhesion factors: Enable attachment to host cells via ligands and receptors.
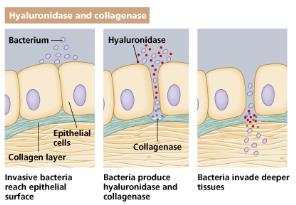
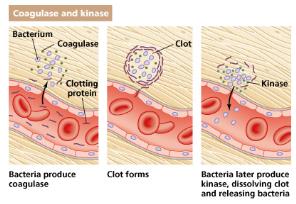
Extracellular enzymes: Degrade host tissues, aiding invasion and evasion of defenses.
Siderophores: Molecules that scavenge iron from the host for bacterial growth.
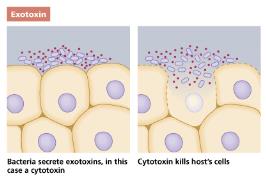
Toxins: Chemicals that damage host tissues (exotoxins and endotoxins).
Antiphagocytic factors: Prevent destruction by host phagocytes (e.g., capsules, leukocidins).
Epidemiology of Infectious Diseases
Measures of Disease Frequency
Incidence: Number of new cases in a given area during a specific period.
Prevalence: Total number of cases (new and existing) in a given area during a specific period.
Patterns of Disease Occurrence
Endemic: Constant presence of a disease within a geographic area.
Sporadic: Occurs infrequently and irregularly.
Epidemic: More cases than expected in a given area or group.
Pandemic: Epidemic spread over several countries or continents.
Public Health and Epidemiology
Public health agencies (e.g., CDC, WHO) monitor, report, and control infectious diseases.
Descriptive epidemiology tabulates data on who, what, where, and when of disease cases.
Analytical epidemiology investigates causes, transmission, and prevention (how and why).

Prevention and Control
Enforcing water and food safety standards
Reducing disease vectors and reservoirs
Immunization programs
Isolation and quarantine measures
Public health education campaigns
Additional info: These notes integrate foundational concepts from microbiology, including definitions, examples, and mechanisms, to provide a comprehensive overview of infection, disease, and epidemiology relevant to college-level study.
