 Back
BackPrinciples of Infectious Disease, Epidemiology, and Immunity
Study Guide - Smart Notes

Principles of Infectious Disease and Epidemiology
Basic Disease Terminology
Understanding infectious diseases and their spread is foundational in microbiology. Epidemiology is the study and control of disease occurrence to promote public health.
Infectious disease: Illness caused by a pathogen (e.g., bacteria, viruses, fungi, protozoa, helminths, prions).
Epidemiology: The science of monitoring and controlling disease occurrence in populations.
Pathogen: Any microorganism capable of causing disease.
Opportunistic pathogen: Causes disease only in weakened hosts.
True pathogen: Can cause disease in healthy hosts.
Patterns of Disease Occurrence
Sporadic: Isolated cases in a population (e.g., Ebola).
Endemic: Routinely detected in a population or region (e.g., cold viruses).
Epidemic: Widespread outbreak in a region during a specific time.
Pandemic: Epidemic that spreads across countries or continents.
Emerging, Reemerging, and Zoonotic Diseases
Emerging pathogens: Newly identified or expanding in distribution (e.g., SARS-CoV-2, Zika virus).
Reemerging pathogens: Previously controlled but now resurging (e.g., antibiotic-resistant bacteria).
Zoonotic diseases: Spread from animals to humans; many are noncommunicable.
Communicable vs. Noncommunicable Diseases
Communicable: Transmitted from human to human.
Contagious: Easily transmitted between hosts.
Latent infection: Pathogen is present but patient is asymptomatic.
Acute vs. Chronic Diseases
Acute: Rapid onset and progression.
Chronic: Slower onset and progression.
Koch’s Postulates and Their Limitations
Koch’s postulates are criteria for linking a specific microbe to a specific disease:
The same organism must be present in every case of the disease.
The organism must be isolated and grown as a pure culture.
The isolated organism should cause disease in a susceptible host.
The organism must be re-isolated from the inoculated host.
Limitations include inability to apply to noninfectious diseases, pathogens that cannot be cultured, or those that do not infect nonhuman hosts.
Reservoirs and Sources of Infection
Reservoir: Natural habitat of a pathogen (animate or inanimate).
Source: Immediate origin from which a host acquires the pathogen.
Endogenous source: Pathogen originates from the host’s own body.
Exogenous source: Pathogen is external to the host.
Modes of Disease Transmission
Pathogens can be transmitted via direct or indirect contact, vehicles, vectors, or environmental sources.
Direct contact: Person-to-person, animal bites, vertical (mother to child).
Indirect contact: Airborne, vehicle (fomites, food, water), vector (biological/mechanical).
Stages of Infectious Disease
Infections progress through five general stages:
1. Incubation period
2. Prodromal phase
3. Acute phase
4. Period of decline
5. Convalescent phase
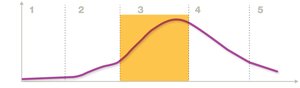
Infectivity: Ability to establish infection. Pathogenicity: Ability to cause disease. Virulence: Severity of disease caused.
Epidemiology and the Epidemiological Triangle
Core Concepts in Epidemiology
Epidemiology studies disease patterns in populations to prevent illness. The epidemiological triangle links the host, etiological agent, and environment.
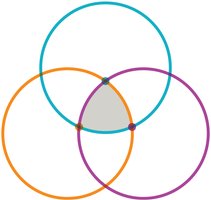
Host factors: General health, age, sex, lifestyle, genetics.
Etiological agent: Type of microbe (bacteria, virus, fungus, parasite, prion).
Environmental factors: Climate, geography, vectors, water/food sources.
Prevention strategies include public education, quarantine, and vector control.
Host–Microbe Interactions and Pathogenesis
Normal Microbiota and Pathogenicity
Host–microbe interactions are dynamic. Normal microbiota colonize various body sites and usually do not cause disease unless disrupted (dysbiosis).
Opportunistic pathogens: Cause disease under certain conditions (e.g., weakened immunity).
Tropism: Pathogen’s preference for specific host tissues.
Virulence and Virulence Factors
Virulence factors are traits that enable pathogens to cause disease, such as adhesion, invasion, immune evasion, and toxin production.

Adhesion: Pili, fimbriae, binding factors.
Invasion: Enzymes, flagella.
Immune evasion: Capsules, antigenic variation, latency.
Toxins: Endotoxins (LPS), exotoxins.
Pathogens may become attenuated (weakened) in culture, losing virulence factors but remaining infectious. Attenuated strains are used in some vaccines.
Toxins as Virulence Factors
Endotoxins: Lipopolysaccharide (LPS) from Gram-negative bacteria; can cause septic shock.
Exotoxins: Secreted proteins affecting specific cell types (neurotoxins, enterotoxins, etc.).
Exotoxins are classified by their mechanism of action:
Type I: Bind to host membrane and trigger signaling.
Type II: Disrupt host cell membranes.
Type III: Enter host cells and exert effects.
Steps to Infection
To establish infection, pathogens must:
Enter the host
Adhere to host tissues
Invade tissues and obtain nutrients
Replicate while evading immune defenses
Transmit to a new host
Cytopathic Effects
Cytocidal: Kill host cells.
Noncytocidal: Damage but do not kill host cells.
Pathogens may disrupt cell function, release toxins, or transform cells (e.g., cancer).
Immune Evasion Mechanisms
Intracellular lifestyle: Hiding inside host cells (e.g., Mycobacterium tuberculosis).
Latency: Remaining dormant in host (e.g., herpesviruses).
Antigenic masking/mimicry/variation: Concealing or altering surface antigens to avoid detection.
Interference with phagocytosis: Capsules, neutralizing enzymes, escaping phagosomes.
Immune suppression: Targeting immune cells, degrading antibodies, interfering with signaling.
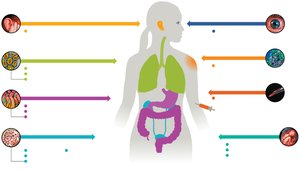
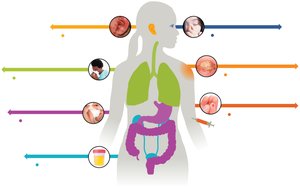
Transmission and Portals of Exit
Pathogens exit the host via specific portals, often the same as their entry route (e.g., respiratory, GI, urogenital tracts).
Innate Immunity
Overview of Immune Responses
The immune system eliminates antigens through innate (nonspecific) and adaptive (specific) responses. Both branches recognize, eliminate, and discriminate between self and foreign antigens.
First-Line Defenses
First-line defenses prevent pathogen entry and include mechanical, chemical, and physical barriers.
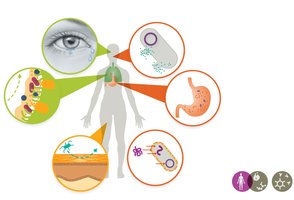
Mechanical: Flushing (tears, urine), trapping (mucus, cilia).
Chemical: Lysozyme, stomach acid, fatty acids, antimicrobial peptides (AMPs).
Physical: Skin, mucous membranes.
Primary and Secondary Lymphoid Tissues
Primary: Bone marrow, thymus (site of leukocyte production/maturation).
Secondary: Lymph nodes, spleen, MALT (filter lymph, sample antigens).
Leukocytes and Their Roles
Leukocytes (white blood cells) are essential for immune responses. They are classified as granulocytes or agranulocytes.
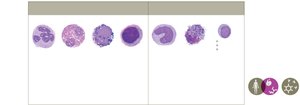
Neutrophils: Highly phagocytic, fight bacteria and viruses.
Eosinophils/Basophils/Mast cells: Attack parasites, involved in allergy.
Monocytes/Macrophages/Dendritic cells: Phagocytic, activate adaptive immunity.
Lymphocytes (NK, B, T cells): Innate and adaptive immunity.
Cytokines and Complement System
Cytokines: Signaling proteins coordinating immune actions; can be diagnostic markers.
Complement system: Cascade of proteins leading to opsonization, inflammation, and cytolysis.
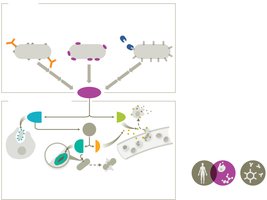
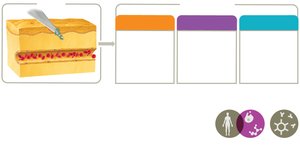
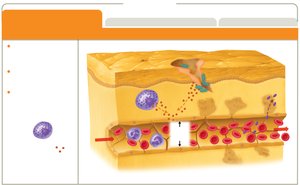
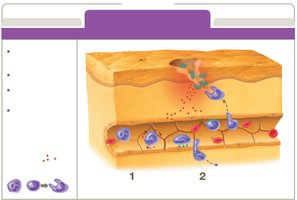
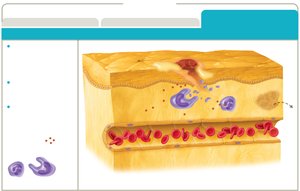
Inflammation
Inflammation is a key innate response to tissue injury or infection, with three main goals: recruit defenses, limit spread, and promote healing.
Phases: Vascular changes, leukocyte recruitment, resolution.
Fever
Enhances interferon effects, phagocyte efficiency, leukocyte production, limits pathogen growth, and promotes tissue repair.
Immune System Disorders
Primary and Secondary Immunodeficiencies
Primary: Congenital, genetic defects affecting immune function (e.g., SCID, DiGeorge syndrome).
Secondary: Acquired due to aging, infections, medical interventions, or systemic disorders.
Autoimmunity and Hypersensitivities
Autoimmunity: Immune attack against self-tissues (e.g., lupus, rheumatoid arthritis, type I diabetes).
Hypersensitivities: Inappropriate immune responses classified as:
Type | Mechanism | Examples |
|---|---|---|
I (Allergy) | IgE-mediated, immediate | Allergic rhinitis, anaphylaxis |
II (Cytotoxic) | IgG/IgM to cell-bound antigens | Hemolytic anemia, transfusion reactions |
III (Immune Complex) | IgG/IgM to soluble antigens | Lupus, serum sickness |
IV (Delayed) | T cell-mediated | Contact dermatitis, TB skin test |
Mnemonic: ACID (Allergy, Cytotoxic, Immune complex, Delayed).
Transfusion and Transplant Reactions
Blood typing: Prevents transfusion reactions (ABO, Rh factor).
Transplant rejection: Mediated by T cells; matching MHC reduces risk.
Graft-versus-host disease: Donor immune cells attack recipient tissues.
Summary Table: Key Concepts
Concept | Definition | Example/Application |
|---|---|---|
Pathogen | Microbe causing disease | Staphylococcus aureus |
Virulence factor | Trait aiding disease causation | Toxins, capsules |
Innate immunity | Non-specific, immediate defense | Skin, phagocytes |
Adaptive immunity | Specific, memory-based defense | Antibodies, T cells |
Autoimmunity | Immune attack on self | Type I diabetes |
Hypersensitivity | Inappropriate immune response | Allergy, contact dermatitis |
