 Back
BackRickettsias, Chlamydias, Spirochetes, and Vibrios: Structure, Physiology, and Diseases
Study Guide - Smart Notes

Rickettsias, Chlamydias, Spirochetes, and Vibrios
Overview
This chapter focuses on the structure, physiology, and clinical significance of Rickettsias, Chlamydias, and related genera, which are important obligate intracellular bacterial pathogens. These organisms are notable for their small size, unique cell structures, and their roles in causing significant human diseases transmitted by arthropod vectors.
Rickettsias
Structure and Physiology
Genera Causing Disease: Rickettsia, Orientia, Ehrlichia, and Anaplasma
Size: Extremely small bacteria, appearing almost wall-less due to minimal peptidoglycan.
Obligate Intracellular Parasites: Require living host cells for survival and replication.
Unique Features: Despite being intracellular, they possess genes for protein synthesis, ATP production, and reproduction.
Transmission: Spread by arthropod vectors (e.g., ticks, lice, fleas, mites).
Medically Important Species and Diseases
Rickettsia rickettsii: Causes Rocky Mountain Spotted Fever (RMSF); transmitted by hard ticks.
Rickettsia prowazekii: Causes epidemic typhus; transmitted by human body lice.
Rickettsia typhi: Causes murine (endemic) typhus; transmitted by fleas.
Orientia tsutsugamushi: Causes scrub typhus; transmitted by chiggers (mites).
Rocky Mountain Spotted Fever (RMSF)
Etiology: Caused by R. rickettsii.
Transmission: Hard ticks (e.g., Dermacentor species) transmit the bacteria among humans and rodents.
Symptoms: Rash on trunk and appendages, fever, and potentially severe complications.
Treatment: Antimicrobials (e.g., doxycycline).
Prevention: Avoiding tick exposure.
Epidemic Typhus
Etiology: Caused by R. prowazekii.
Transmission: Human body lice (Pediculus humanus).
Symptoms: High fever, depression, rash; prevalent in crowded, unsanitary conditions.
Treatment: Antimicrobials.
Prevention: Avoiding lice exposure.

Murine (Endemic) Typhus
Etiology: Caused by R. typhi.
Transmission: Fleas (e.g., Xenopsylla cheopis, Ctenocephalides felis); rodents are reservoirs.
Symptoms: Fever, headache, chills, muscle pain, nausea; rash in fewer than 50% of cases.
Treatment: Doxycycline.
Prevention: Avoiding flea exposure.

Scrub Typhus
Etiology: Caused by Orientia tsutsugamushi.
Transmission: Mites (chiggers); transovarian transmission among mites.
Symptoms: Fever, headache, muscle pain, sometimes rash.
Geography: Endemic to eastern Asia, Australia, India; seen in U.S. among immigrants from endemic areas.
Treatment: Appropriate antimicrobials.
Prevention: Avoiding mite exposure.
Ehrlichiosis and Anaplasmosis
Ehrlichia chaffeensis: Causes human monocytic ehrlichiosis (HME).
Anaplasma phagocytophilum: Causes anaplasmosis (formerly human granulocytic ehrlichiosis, HGE).
Transmission: Ticks (e.g., Lone Star tick, Amblyomma americanum for Ehrlichia; Ixodes spp. for Anaplasma).
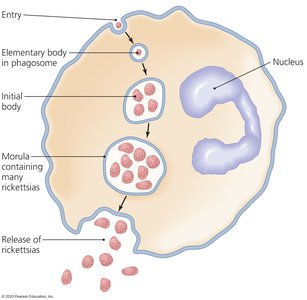
Developmental Stages in Leukocytes: Elementary body, initial body, and morula.
Symptoms: Resemble spotted fever rickettsiosis but usually without rash.
Treatment: Immediate antimicrobials to prevent complications.
Prevention: Avoiding tick exposure.
Summary Table: Rickettsial Diseases
Organism | Primary Vectors | Reservoirs | Diseases |
|---|---|---|---|
R. rickettsii | Hard ticks | Ticks, rodents | Rocky Mountain spotted fever |
R. prowazekii | Human body louse | Humans, squirrels, squirrel fleas | Epidemic typhus |
R. typhi | Rat and cat fleas | Rodents | Murine typhus |
Orientia tsutsugamushi | Mite (chigger) | Mites | Scrub typhus |
Ehrlichia chaffeensis | Lone Star tick | Ticks | Ehrlichiosis (HME) |
Anaplasma phagocytophilum | Ixodes spp. ticks | Ticks | Anaplasmosis (HGE) |
Chlamydias
Structure and Physiology
Cell Wall: Lack peptidoglycan; have two membranes.
Obligate Intracellular Parasites: Grow and multiply only within vesicles of host cells.
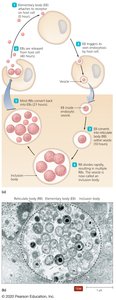
Developmental Cycle: Involves two forms—elementary bodies (EBs, infectious) and reticulate bodies (RBs, replicative).
Pathogenesis and Epidemiology of Chlamydia trachomatis
Host Range: Primarily infects humans; one strain infects mice.
Entry: Through abrasions and lacerations; infects conjunctiva and mucous membranes.
Prevalence: Most common reportable sexually transmitted disease (STD) in the U.S.
Clinical Manifestations: Due to cell destruction and inflammation; major cause of eye infections worldwide.
Risk Factors: Endemic in poor communities lacking hygiene and medical care.
Diseases Caused by Chlamydia trachomatis
Sexually Transmitted Infections (STIs): Nongonococcal urethritis, proctitis, cervicitis.
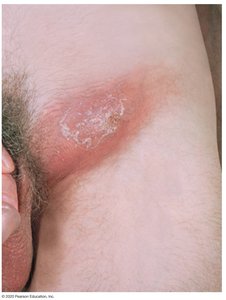
Lymphogranuloma Venereum (LGV): Initial genital lesion followed by swollen lymph nodes (buboes), which may rupture and drain.
Asymptomatic Infections: Most common in women; reinfection can cause pelvic inflammatory disease (PID).
Diagnosis, Treatment, and Prevention of Chlamydia trachomatis Infections
Diagnosis: Microscopy to view bacteria inside cells; nucleic acid amplification tests (NAATs).
Treatment: Antibiotics for STIs; surgical correction for trachoma-related deformities.
Prevention: Safe sexual practices; prompt antibacterial treatment to prevent blindness.
Other Chlamydial Diseases
Chlamydophila pneumoniae: Causes pneumonia, bronchitis, and sinusitis; most cases are mild but can resemble atypical pneumonia.
Treatment: Doxycycline or azithromycin; some infections persist despite therapy.
Prevention: Difficult due to ubiquity of organism.
Chlamydophila psittaci: Causes ornithosis (psittacosis); flulike symptoms, transmitted from birds to humans via aerosols or contact.
Treatment: Tetracycline or azithromycin.
Prevention: Proper handling of birds.
Summary Table: Characteristics of the Smallest Microbes
Feature | Rickettsias | Chlamydias | Mycoplasmas | Viruses |
|---|---|---|---|---|
Cellular Structure | Small cells, little peptidoglycan | Small, wall-less, two membranes | Small, wall-less, pleomorphic, sterols in membrane | Acellular |
Diameter | 0.3 μm | EBs: 0.2–0.4 μm; RBs: 0.6–1.5 μm | 0.1–0.8 μm | 0.01–0.3 μm |
Lifestyle | Obligate intracellular (cytosol) | Obligate intracellular (vesicles) | Free-living | Obligate intracellular (cytosol/nuclei) |
Replication | Binary fission | Binary fission of RBs | Binary fission | Chemical assembly |
Nucleic Acid(s) | DNA and RNA | DNA and RNA | DNA and RNA | DNA or RNA |
Functional Ribosomes | Present | Present | Present | Absent |
Metabolism | Present | Present | Limited | Absent |
ATP-Generating System | Present | Absent | Present | Absent |
Phylum | Proteobacteria | Chlamydiae | Firmicutes | None |
Key Concepts and Review Questions
Transmission of RMSF: Spread by ticks.
Organs Infected by Chlamydia trachomatis: Eyes, trachea, rectum, and urethra.
Cause of Lymphogranuloma Venereum: Chlamydia trachomatis.
