 Back
BackBlood Glucose Regulation and Diabetes: Mechanisms, Types, and Nutrition Management
Study Guide - Smart Notes

Carbohydrates: Blood Glucose Regulation & Diabetes
Overview of Blood Glucose Regulation
The body maintains blood glucose within a narrow range (70–99 mg/dL fasting) through the coordinated actions of hormones, primarily insulin and glucagon, secreted by the pancreas. Proper regulation is essential for cellular energy and overall metabolic health.
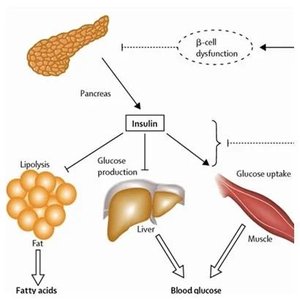
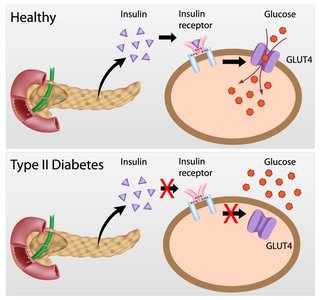
Insulin: An anabolic hormone produced by pancreatic beta cells. It promotes glucose uptake into cells, especially muscle and fat, and inhibits glucose production by the liver.
Glucagon: A catabolic hormone produced by pancreatic alpha cells. It stimulates glycogen breakdown (glycogenolysis) and glucose synthesis from amino acids (gluconeogenesis) in the liver during fasting.
Other Hormones: Epinephrine, norepinephrine, cortisol, and growth hormone also influence blood glucose, especially during stress or fasting.
Mechanisms of Insulin and Glucagon Action
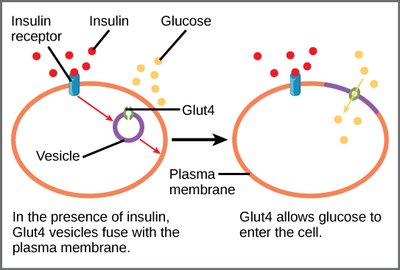
Insulin:
Facilitates glucose uptake into muscle and adipose tissue via GLUT4 transporters.
Promotes glycogen synthesis in the liver and muscle.
Inhibits lipolysis (fat breakdown) and gluconeogenesis.
Glucagon:
Stimulates glycogenolysis and gluconeogenesis in the liver, raising blood glucose during fasting.
Promotes the release of glucose into the bloodstream via GLUT2 transporters.
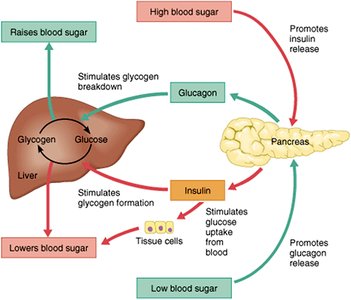
Healthy Blood Glucose Regulation
In healthy individuals, insulin and glucagon maintain blood glucose within the normal range. Disruption of this balance leads to metabolic disorders such as diabetes and hypoglycemia.
Diabetes Mellitus: Types and Pathophysiology
Prevalence and Types of Diabetes
Diabetes is a chronic disease characterized by elevated blood glucose due to impaired insulin secretion, action, or both. It affects millions globally and is a major public health concern.


Type 1 Diabetes: Autoimmune destruction of pancreatic beta cells leads to absolute insulin deficiency. Accounts for 5–10% of cases.
Type 2 Diabetes: Characterized by insulin resistance and relative insulin deficiency. Accounts for 90–95% of cases.
Diagnostic Criteria for Diabetes
Diagnosis is based on fasting plasma glucose, oral glucose tolerance test (OGTT), and HbA1c levels.
Diagnosis | Fasting Plasma Glucose (mg/dL) | Oral Glucose Tolerance Test (mg/dL) | A1C (%) |
|---|---|---|---|
Diabetes | 126 or above | 200 or above | 6.5 or above |
Prediabetes | 100 to 125 | 140 to 199 | 5.7 to 6.4 |
Normal | 99 or below | 139 or below | About 5 |
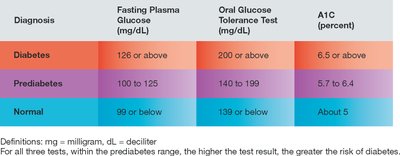
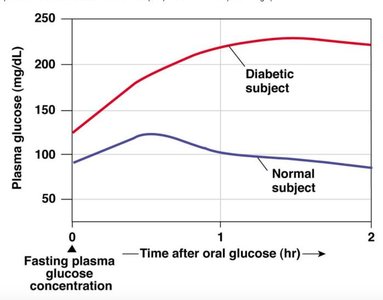
Oral Glucose Tolerance Test (OGTT)
The OGTT measures the body's ability to clear glucose from the blood after ingestion. Diabetic subjects show higher and prolonged glucose levels compared to normal subjects.
Type 1 Diabetes Mellitus
Etiology and Pathogenesis
Type 1 diabetes is an autoimmune disorder where the immune system destroys insulin-producing beta cells in the pancreas. The exact cause is unknown, but genetic predisposition and environmental triggers are implicated.
Onset: Often in childhood or adolescence, but can occur at any age.
Treatment: Requires lifelong insulin therapy, healthy diet, physical activity, and stress management.
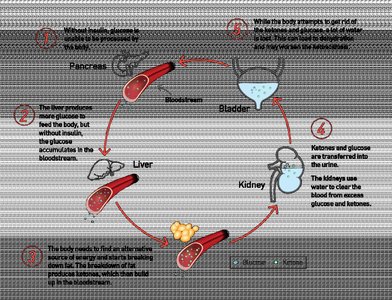
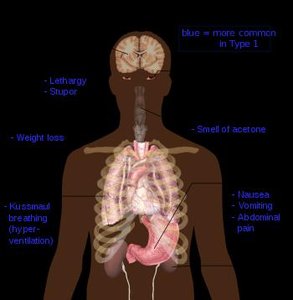
Diabetic Ketoacidosis (DKA)
DKA is a life-threatening complication of uncontrolled type 1 diabetes, resulting from severe insulin deficiency. It leads to hyperglycemia, ketone body production, and metabolic acidosis.
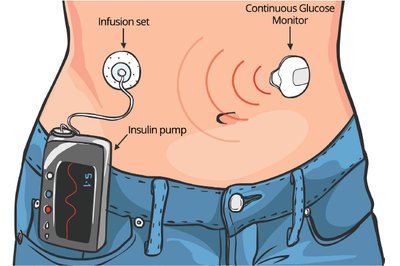
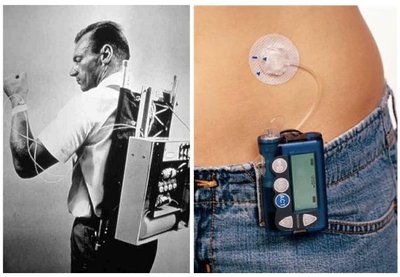
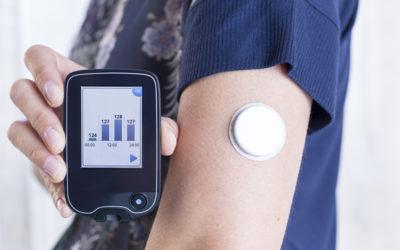
Insulin Delivery and Blood Glucose Monitoring
Insulin can be administered via syringes, pens, or pumps.
Continuous glucose monitoring is essential for optimal management.

Type 2 Diabetes Mellitus
Pathophysiology
Type 2 diabetes is characterized by insulin resistance (decreased cellular response to insulin) and eventual decline in insulin production. It is strongly associated with obesity, sedentary lifestyle, and genetic factors.
Risk Factors: Advanced age, family history, ethnicity, visceral fat, sedentary lifestyle, gestational diabetes, and inadequate sleep.
Signs and Symptoms of Hyperglycemia
Excessive thirst (polydipsia)
Excessive urination (polyuria)
Hunger (polyphagia)
Weight loss
Blurred vision
Fatigue
Poor wound healing
Long-Term Complications of Uncontrolled Diabetes
Retinopathy: Damage to the blood vessels in the retina, leading to vision loss.
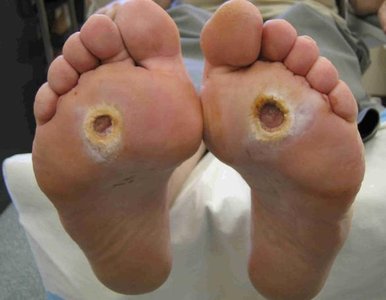
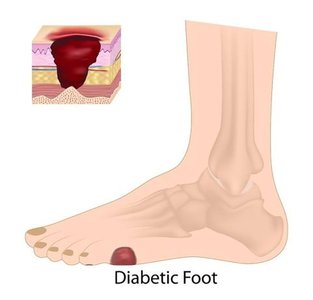
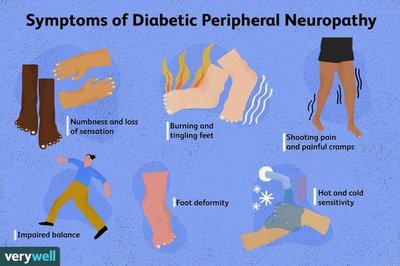
Neuropathy: Nerve damage, especially in the extremities, causing pain, numbness, and foot ulcers.
Nephropathy: Kidney damage.
Cardiovascular Disease: Increased risk of heart attack and stroke.

Management of Type 2 Diabetes
Healthy eating (focus on complex carbohydrates and fiber)
Regular physical activity
Weight management (reduce visceral fat)
Blood glucose monitoring
Medications as needed
Prevention of complications
Stress management
Nutrition Recommendations for Type 2 Diabetes
Eat meals and snacks regularly (every 3–4 hours).
Distribute carbohydrate intake evenly throughout the day.
Choose complex carbohydrates over simple sugars.
Consume foods high in soluble fiber.
Include protein and fat with each meal to slow glucose absorption.
Avoid alcohol.
Hypoglycemia
Definition and Types
Hypoglycemia is defined as blood glucose below 70 mg/dL. It can be reactive (after a high-carbohydrate meal) or fasting (without food intake).
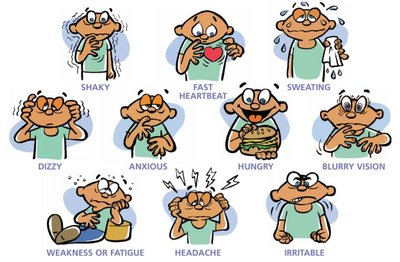
Symptoms: Shakiness, sweating, dizziness, hunger, irritability, headache, weakness, blurred vision, fast heartbeat.
Nutrition Recommendations for Hypoglycemia
Follow similar dietary guidelines as for type 2 diabetes.
In case of a hypoglycemic episode, use the 15-15 Rule: consume 15 grams of carbohydrate, check blood glucose after 15 minutes, and repeat if necessary until levels are above 70 mg/dL.
Examples of 15 grams of carbohydrate: glucose tablets, 4 oz juice or regular soda, 1 tbsp sugar/honey/corn syrup, hard candies.
Key Terms and Concepts
Monosaccharide: Single sugar molecule (e.g., glucose, fructose).
Disaccharide: Two monosaccharides linked together (e.g., sucrose).
Oligosaccharide: Short chains of monosaccharides.
Polysaccharide: Long chains of monosaccharides (e.g., starch, glycogen).
Glycogen: Storage form of glucose in animals.
Soluble Fiber: Dissolves in water, helps lower blood cholesterol and glucose.
Insoluble Fiber: Does not dissolve in water, promotes bowel regularity.
Nutritive Sweeteners: Provide calories (e.g., sucrose, glucose).
Non-Nutritive Sweeteners: Provide little or no calories (e.g., aspartame, sucralose).
