 Back
BackEnergy Balance, Body Weight, and Eating Disorders: Study Notes
Study Guide - Smart Notes

Energy Balance and Body Weight
Body Mass Index, Body Fat Content, and Fat Distribution
Understanding body weight and its distribution is essential for assessing health risks and guiding nutrition interventions. Body Mass Index (BMI) is a widely used tool, but it has limitations, and other measures provide a more complete picture of health.
Body Mass Index (BMI): A numerical value calculated from height and weight, used to classify underweight, normal weight, overweight, and obesity.
BMI Calculation Formulas:
Limitations of BMI: Does not distinguish between fat and muscle mass; may underestimate fat in overweight individuals and overestimate in muscular individuals.
Body Fat Content: Optimal fat content is 20–30% for females and 12–20% for males.
Measuring Body Fat: Methods include skin-fold tests, underwater weighing, bioelectric impedance analysis (BIA), and dual-energy X-ray absorptiometry (DEXA).
Fat Distribution: Visceral fat (abdominal fat) is a stronger predictor of disease risk than total fat mass. Waist circumference and waist-to-hip ratio are used to assess abdominal obesity.
Theories for Energy Balance
Energy balance is the relationship between energy intake (calories consumed) and energy expenditure (calories burned). Maintaining energy balance is crucial for weight management and overall health.
Positive Energy Balance: Occurs when energy intake exceeds energy expenditure, leading to weight gain.
Negative Energy Balance: Occurs when energy intake is less than energy expenditure, resulting in weight loss.
Estimated Energy Requirement (EER): The average dietary energy intake predicted to maintain energy balance in a healthy adult.
EER Formulas:
Adult Male: Adult Female:
METs (Metabolic Equivalents): A unit to estimate the amount of oxygen used by the body during physical activity. 1 MET = 3.5 ml O2/kg/min.
Total Energy Expenditure (TEE): The sum of energy used for basal metabolism, digestion (thermic effect of food), and physical activity.
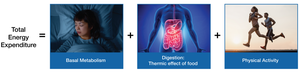
Basal Metabolic Rate (BMR): The energy required to maintain basic physiological functions at rest. Accounts for 50–70% of daily energy expenditure. Influenced by body size, composition, sex, age, nutritional status, and genetics.
Factors Affecting Energy Intake and Expenditure
Energy intake and expenditure are regulated by complex physiological, genetic, psychological, and societal factors.
Physiological/Genetic Influences: Hunger and satiety signals, hormone levels (e.g., leptin), genetic predisposition to body size and appetite.
Psychological/Behavioral Influences: Food preferences, mood, emotions, exposure to calorie-dense foods, portion sizes, and societal norms.
Societal Factors: Access to healthy foods, opportunities for physical activity, socioeconomic status, and cultural attitudes toward body size.
Sedentary Behavior: Activities with low energy expenditure, such as sitting or lying down while awake, contribute to reduced total energy expenditure.
Health Risks Associated with Body Size
Health at Every Size
The Health at Every Size® (HAES) movement promotes a weight-inclusive, non-diet approach to health care, focusing on intuitive eating, reducing weight stigma, and prioritizing overall well-being rather than weight loss.
Healthism: The belief that health is solely an individual responsibility and that societal productivity depends on meeting specific health standards.
HAES Principles: Encourage eating and moving for health, not for changing body size; address physical, emotional, spiritual, and economic health.
Risks of Being Underweight and Eating Disorders
Being underweight can lead to serious health risks, including nutritional deficiencies, delayed wound healing, hormonal abnormalities, increased infection risk, and chronic diseases such as osteoporosis. In children, underweight status can stunt growth.
Anorexia Nervosa: A psychiatric disorder characterized by extreme restriction of food intake, fear of weight gain, and distorted body image. It has the highest mortality rate among mental illnesses.
Bulimia Nervosa: Characterized by cycles of binge eating followed by purging. Individuals may have normal weight, making diagnosis challenging. Associated with depression and anxiety.
Binge Eating Disorder: Involves recurrent episodes of uncontrolled eating, often leading to obesity and increased risk of chronic diseases.
Other Eating Disorders: ARFID (avoidant/restrictive food intake disorder), OSFED (other specified feeding or eating disorder), and orthorexia nervosa (obsession with healthy eating).
Dietary, Behavioral, and Physical Activity Recommendations for Health
Evidence-Based Dietary Recommendations
Meeting nutritional needs through nutrient-dense foods and beverages is essential for health. Variety, portion control, and cultural preferences should be considered in dietary planning.
Choose a variety of foods from each food group.
Pay attention to portion sizes, especially for calorie-dense foods.
Smaller portions help reduce calorie intake.
Evidence-Based Physical Activity Recommendations
Physical activity is a key component of energy balance and overall health. The 2008 Physical Activity Guidelines for Americans recommend:
Move more and sit less throughout the day.
At least 2.2–5 hours per week of moderate-intensity aerobic activity, or 1 hour and 15 minutes per week of vigorous-intensity activity.
Muscle-strengthening activities involving all major muscle groups at least two days per week.
Health at Every Size® Recommendations
Eat intuitively—respond to hunger and fullness cues without distractions.
Prioritize good-quality sleep and stress management (e.g., meditation, yoga).
Focus on movement for health, not just exercise for weight loss.
Key Takeaways
BMI is a useful screening tool but has limitations; body fat content and distribution are better predictors of disease risk.
Energy balance is influenced by physiological, genetic, behavioral, and societal factors.
Both underweight and overweight statuses carry health risks; eating disorders require multidisciplinary treatment.
Evidence-based dietary and physical activity guidelines support health at any size, emphasizing nutrient-dense foods, regular movement, and holistic well-being.
