 Back
BackEnergy Balance, Body Weight, and Obesity: Assessment and Health Implications
Study Guide - Smart Notes

Energy Balance and Body Weight
Introduction to Body Weight Regulation
Body weight is determined by a complex interplay of physiological, genetic, behavioral, societal, and environmental factors. Understanding how the body uses, stores, and balances energy is essential for maintaining a healthy weight and preventing obesity-related diseases.
Energy Balance: The relationship between energy intake (calories consumed) and energy expenditure (calories burned). Positive energy balance leads to weight gain, while negative energy balance results in weight loss.
Energy Storage: Excess energy is stored primarily as fat in adipose tissue.
Societal and Environmental Influences: Modernization, industrialization, and urbanization have created 'obesogenic' environments that promote increased intake of non-healthful foods and physical inactivity.
Obesity and Society
Prevalence and Contributing Factors
Obesity rates have risen dramatically in the United States and globally, with significant health and economic consequences. Multiple factors contribute to this trend:
Obesogenic Environment: Environments that encourage excessive calorie intake and discourage physical activity.
Socioeconomic Factors: Higher obesity rates are observed among lower income and educational groups, and risk varies by race/ethnicity.
Modern Lifestyles: Increased availability of fast food, larger portion sizes, mechanized workplaces, and sedentary leisure activities (e.g., television viewing) all contribute to reduced physical activity and increased calorie consumption.
Health Risks: Obesity increases the risk of cardiovascular disease, type 2 diabetes, certain cancers, and imposes significant financial costs on individuals and society.
Strategies for Addressing Obesity
Individual Level: Choose whole foods, reduce portion sizes, increase physical activity, and limit sedentary behaviors.
Community Level: Advocate for healthier food options in schools and workplaces, support local agriculture, and improve access to recreational spaces.
National Level: Support policies that promote walkable cities, fund obesity prevention programs, and increase access to affordable healthy foods.
Indicators of Health: Body Mass Index, Body Composition, and Fat Distribution
Definitions and Classifications
Assessing body weight and health risk involves several key indicators:
Body Weight: The sum of lean mass (bone, muscle, organs), water, and fat mass.
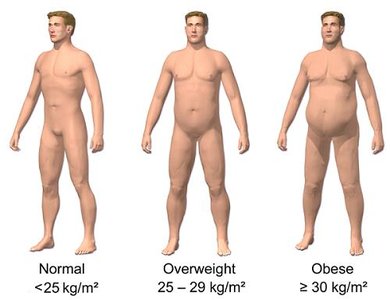
Overweight: Having more weight than is typical for a given height.
Obese: Having excess body fat, which is associated with increased health risks.
The 'ideal' body weight varies by frame size, sex, muscle mass, bone density, age, height, and cultural perceptions.
Body Mass Index (BMI)
BMI is a widely used tool for assessing weight status and health risk. It is calculated as:
BMI categories are as follows:
Category | BMI (kg/m2) |
|---|---|
Underweight | < 18.5 |
Normal weight | 18.5–24.9 |
Overweight | 25–29.9 |
Obese | ≥ 30.0 |
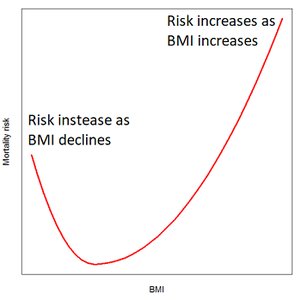
Mortality Risk: Both low and high BMI values are associated with increased mortality risk, forming a J-shaped curve. The lowest risk is observed with BMI values between 18 and 25.
Limitations of BMI
BMI does not distinguish between muscle and fat mass, so it may misclassify muscular individuals as overweight or obese.
It may not accurately reflect health risks in children, pregnant women, or the elderly.
BMI is a screening tool, not a diagnostic measure; further assessment by healthcare professionals is necessary.
Measuring Body Fat Content
Body fat percentage is a more direct measure of health risk than BMI. Methods include:
Underwater Weighing: Compares body weight in and out of water to estimate fat percentage.
Skin-fold Measurement: Uses calipers to measure subcutaneous fat at various body sites.
Bioelectric Impedance Analysis (BIA): Estimates body composition based on electrical conductivity differences between fat and lean tissue.
Dual-energy X-ray Absorptiometry (DEXA): Measures bone density and body fat distribution using low-dose X-rays.
Optimal fat content: 20–30% for females, 12–20% for males.
Measuring Fat Distribution
Fat distribution is a critical predictor of health risk. Visceral fat (abdominal fat) is more strongly associated with disease risk than subcutaneous fat (hip/thigh fat).
Waist Circumference: Measured just above the navel; >40 inches for men and >35 inches for women indicates increased risk.
Waist-to-Hip Ratio: Calculated as waist circumference divided by hip circumference. Ratios above 0.90 for males and 0.85 for females indicate abdominal obesity and higher health risk.
Body Shapes: 'Apple-shaped' (central obesity) individuals have higher chronic disease risk than 'pear-shaped' (lower body fat) individuals.
Metabolic Syndrome
Definition and Prevention
Metabolic syndrome is a cluster of risk factors that increase the likelihood of heart disease, type 2 diabetes, and stroke. Diagnosis requires any three of the following five criteria:
Abdominal obesity
Elevated plasma triglycerides
Low HDL ('good') cholesterol
High blood pressure
High fasting blood glucose
Prevention: Eat a diet rich in whole grains, vegetables, and lean proteins; limit saturated and trans fats, added sugars, sodium, and processed foods; engage in at least 150 minutes per week of moderate exercise; and maintain a healthy weight.
References and Further Reading
Centers for Disease Control and Prevention. “Adult Obesity Facts.”
National Heart, Lung, and Blood Institute BMI Calculator: http://www.nhlbisupport.com/bmi/
CDC BMI Calculator: http://www.cdc.gov/healthyweight/assessing/bmi/adult_bmi/english_bmi_calculator/bmi_calculator.html
American Heart Association: https://www.heart.org/en/health-topics/metabolic-syndrome
