 Back
BackEnergy Balance, Body Weight, Obesity, and Eating Disorders: Structured Study Notes
Study Guide - Smart Notes

Weight and Health
Categories of Body Weight and Associated Health Risks
Body weight is classified into categories based on health risk, not a single 'healthy weight.' These categories reflect the likelihood of developing chronic diseases.
Obese: Significant excess of Calories. - High risk of chronic diseases: Type 2 diabetes, heart disease, hypertension, some cancers, increased mortality.
Healthy weight: Sufficient Calories for age, height, and sex. - Able to maintain weight without constant dieting. - Low risk of weight-related disease.
Overweight: Excess Calories. - Moderate risk of chronic disease: Type 2 diabetes, heart disease, some cancers.
Underweight: Insufficient Calories. - Can impair body function, increasing risk of nutritional deficiencies, compromised immune function, and death.
Energy Balance
Concepts of Energy Balance
Energy balance is the relationship between energy intake and energy expenditure, determining weight changes.
Energy balance: Intake equals expenditure; weight is maintained.
Positive energy balance: Intake exceeds expenditure; weight is gained.
Negative energy balance: Intake is less than expenditure; weight is lost.
Calculating Energy Intake and Expenditure
Energy intake is derived from macronutrients in food, each with specific caloric values:
Fat: 9 Calories/gram
Carbohydrates: 4 Calories/gram
Protein: 4 Calories/gram
Alcohol: 7 Calories/gram
Example calculation:


Energy Expenditure Components
Energy expenditure is divided into several components:
Basal Metabolic Rate (BMR): Energy used for basic body functions (50-70% of total expenditure).
Thermic Effect of Food (TEF): Energy used to digest, absorb, and metabolize food (5-15%).
Exercise Activity Thermogenesis (EAT): Calories used during exercise.
Non-Exercise Activity Thermogenesis (NEAT): Calories used for non-exercise movements (walking, chores, fidgeting).
Assessing Weight-Related Health Risk
Body Mass Index (BMI)
BMI is a common tool for assessing health risk based on weight and height:
Formula:
Categories:
Obese: BMI > 30
Overweight: 25 ≤ BMI ≤ 30
Healthy Weight: 18.5 ≤ BMI < 25
Underweight: BMI < 18.5
BMI is a screening tool and does not account for muscle mass, bone density, or other health factors.
Body Composition and Fat Distribution
Body composition measures the relative amounts of lean body mass and fat mass. Fat distribution affects health risk:
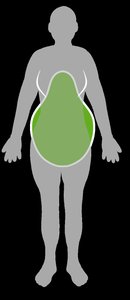
Visceral fat: Fat around organs; high central obesity increases chronic disease risk.
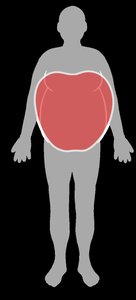
Subcutaneous fat: Fat under the skin; lower risk compared to visceral fat.
Methods for Measuring Body Composition
Method | How it Works | Pros | Cons |
|---|---|---|---|
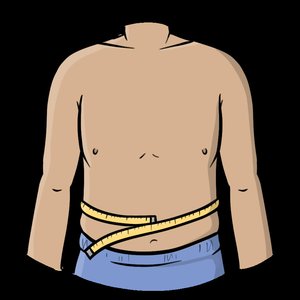
Waist Circumference | Measures central obesity | Easy, inexpensive | Does not directly measure body composition |
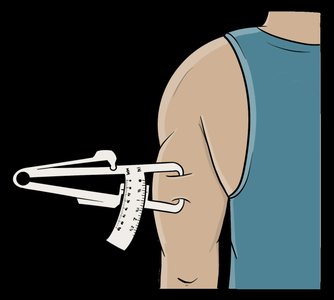
Skinfold Test | Calipers measure subcutaneous fat | Easy, portable | Can be less accurate |
Bioelectrical Impedance | Electrical current measures lean mass | Quick, household scales | Less accurate, hydration-dependent |
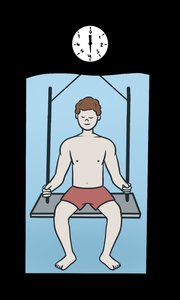
Underwater Weighing | Weighing in/out of water calculates fat | Accurate | Requires equipment, fasting |
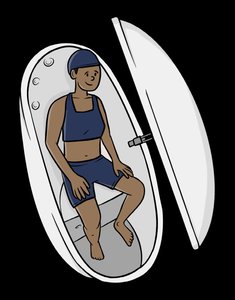
Air Displacement Pod | Measures air displacement | Accurate, easier | Specialized equipment |
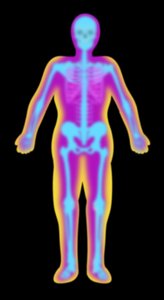
Dual Energy X-ray Absorptiometry | X-ray differentiates tissue types | Accurate, bone density | Expensive, specialized equipment |

Factors That Influence Weight
Social-Ecological Model of Health
This model describes layers of influence on health and weight:
Individual: Biology, genetics, personal choices
Relationship: Family and friends
Community: Food environment, local influences
Societal: Policies, economics
Genetic Influences
Genetics play a significant role in body weight regulation:
Set-point theory: Body resists weight changes, favoring a genetically determined weight.
Thrifty gene hypothesis: Genes favor energy storage, protecting against undernutrition.
BMI is roughly 40-70% genetically determined; hundreds of genes contribute small effects.
Hormonal Influences
Hormones regulate hunger, satiety, and metabolism:
Ghrelin: From stomach, cues hunger
Cholecystokinin (CCK): From small intestine, cues satiety
Leptin: From fat cells, regulates hunger and promotes satiety; leptin resistance in obesity
GLP-1: From intestine, promotes satiety
Thyroxine (T4): From thyroid, regulates BMR
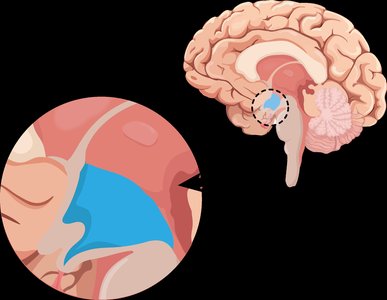
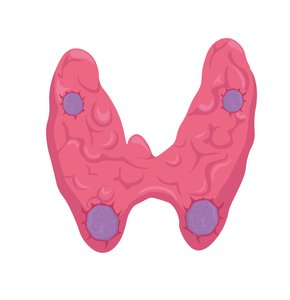
Environmental Influences
Environmental factors contributing to obesity include:
Increased access to high-calorie, low-nutrient foods
Larger portion sizes
More frequent meals, especially fast food
More sedentary lifestyles
Government policies affecting food prices




Weight Loss
Healthy Eating and Calorie Deficit
Weight loss requires a calorie deficit, where intake is less than expenditure. Approximately 3,500 Calories equals 1 pound of body fat.
Healthy weight loss: 0.5–2 lb/week
Behavioral modifications: mindful eating, food journals, stress management, avoiding food as reward
Physical Activity
Physical activity increases calorie expenditure and helps maintain lean muscle mass. However, exercise may increase hunger, and it is easier to reduce intake than to burn excess calories.

Healthy Eating for Weight Loss
Foods that promote satiety and maintain a calorie deficit are recommended:
Nutrient-dense, high-volume, low-energy-density foods (fruits, vegetables, whole grains)
Lean proteins
Avoid added sugars and artificial sweeteners



Fad Diets
Fad diets promise rapid results with little scientific evidence and often restrict food groups or require special products. Healthful diets meet nutritional targets and promote whole foods.

Medications and Supplements
Weight loss medications are prescribed for individuals with BMI > 30, or > 27 with risk factors. GLP-1 receptor agonists mimic GLP-1, stimulating satiety and slowing gastric emptying. Supplements are regulated for safety, not effectiveness, and may contain stimulants.
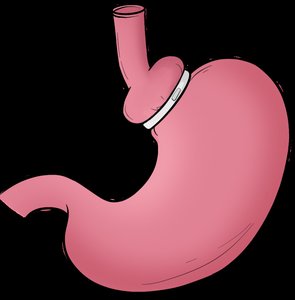
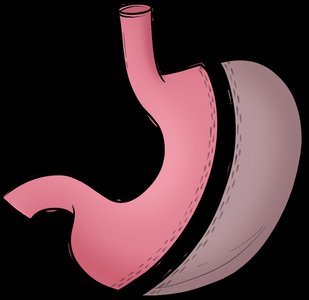
Surgical Interventions
Bariatric surgery modifies GI tract anatomy to reduce food intake and promote satiety. Types include gastric bypass, gastric banding, and gastric sleeve. Liposuction is a cosmetic procedure for localized fat reduction.

Maintaining Weight
Strategies for Weight Maintenance
After weight loss, BMR decreases, requiring fewer calories. Maintaining weight involves continuing healthy eating, regular physical activity, and behavioral modifications. Weight cycling (yo-yoing) is common if new habits are not sustained.


Gaining Weight
Healthy Weight Gain
Healthy weight gain for underweight individuals involves a calorie excess, resistance training to build muscle, and frequent small meals with calorie-dense foods (nuts, dried fruits).


Eating Disorders
Body Image and Disordered Eating
Body image includes thoughts and feelings about one's body. Negative body image can lead to disordered eating (atypical, unhealthful behaviors) and clinical eating disorders (anorexia nervosa, bulimia nervosa, binge eating disorder).
Anorexia Nervosa
Characterized by extreme calorie deficit and restrictive eating, leading to severe health consequences:
Electrolyte imbalances, low pulse and body temperature, reduced muscle mass, low bone density, brittle hair, amenorrhea, lanugo
High risk in weight-class or aesthetic sports
One of the highest mortality rates among psychological disorders

Bulimia Nervosa & Binge Eating Disorder
Feature | Bulimia | Binge Eating Disorder |
|---|---|---|
Definition | Binging and purging | Binging without purging |
Body Response | GI tract damage, electrolyte imbalances | Obesity, hypertension, heart disease, type 2 diabetes |
Prevalence | Females: 0.32%, Males: 0.05% | Females: 0.96%, Males: 0.26% |
Treatment of Eating Disorders
Treatment requires multidisciplinary teams and early intervention for best outcomes:
Medical: Stabilize physical health
Psychological: Address underlying issues (anxiety, depression)
Nutritional: Develop adequate, varied dietary plan
