 Back
BackNutrients in Bone Metabolism and Osteoporosis: A Comprehensive Study Guide
Study Guide - Smart Notes

Nutrients in Bone Metabolism
Functions of Bone
Bones are dynamic organs that provide structure, protection, and metabolic functions essential for human health. They are composed of both mineral and organic components, which contribute to their hardness, strength, and flexibility.
Mineral Content: About 65% of bone is mineral, primarily calcium and phosphorus, providing rigidity.
Organic Matrix: The remaining 35% is organic, mainly collagen, which imparts flexibility and durability.
Key Functions:
Support and protection of organs
Movement (as levers for muscles)
Storage of minerals (especially calcium and phosphorus)
Production of blood cells (in bone marrow)
Bone Turnover and Remodeling
Bone is constantly being renewed through a process called remodeling, which involves both the breakdown and formation of bone tissue. This process is essential for bone health, repair, and adaptation to stress.
Bone Growth: Increase in bone size, mainly during childhood and adolescence.
Bone Modeling: Shaping of bone, which largely ceases after puberty.
Bone Remodeling: Ongoing replacement of old bone with new bone throughout life.
Resorption: Osteoclasts break down bone tissue, releasing minerals into the blood.
Formation: Osteoblasts build new bone by producing collagen and facilitating mineralization.
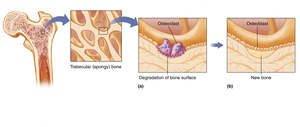
Assessing Bone Health
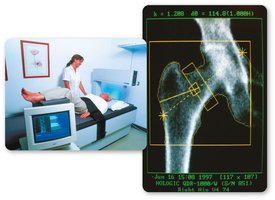
Bone density is a key indicator of bone strength and risk for osteoporosis. Dual-energy x-ray absorptiometry (DXA or DEXA) is the standard method for measuring bone density.
DXA Scan: Noninvasive, uses low-level x-rays to assess bone density in the whole body or specific regions (e.g., wrist, hip).
T-score: Compares patient bone density to that of a healthy 30-year-old; used to diagnose osteoporosis.
Recommended for: Postmenopausal women and others at risk for bone loss.
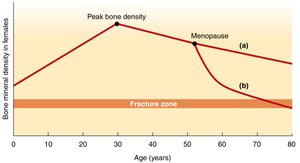
Bone Turnover Across the Lifespan
Bone formation and breakdown rates change with age:
Childhood: Formation exceeds breakdown, leading to increased bone mass and density.
Young Adults (30–40 years): Formation and breakdown are balanced; peak bone mass is achieved in the late twenties.
Older Adults (>40 years): Breakdown exceeds formation, resulting in gradual bone loss.
Postmenopausal Women: Accelerated bone loss due to hormonal changes; hormone replacement therapy may help slow this process.
Nutrients Essential for Bone Metabolism
Calcium
Calcium is the most abundant mineral in the body and is critical for bone structure and various physiological functions.
Distribution: 99% in bones and teeth, 1% in blood and soft tissues.
Functions:
Bone and teeth formation and maintenance
Acid–base balance
Nerve impulse transmission
Muscle contraction
Vascular control (blood pressure regulation)
Regulation: Blood calcium is tightly regulated by parathyroid hormone (PTH), vitamin D, and calcitonin.
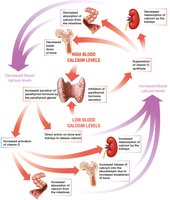
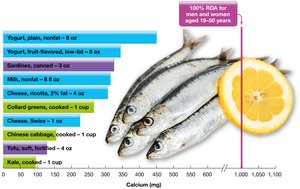
Recommended Intake: 1,000 mg/day for adults aged 19–50 years.
Food Sources: Dairy products, beans, green leafy vegetables, tofu (with calcium), and fortified foods.
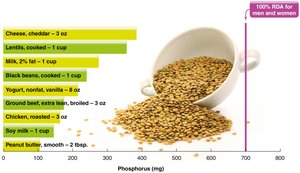
Phosphorus
Phosphorus is a major mineral found primarily in bones and is essential for many cellular processes.
Distribution: 85% in bones as phosphate.
Functions:
Mineralization of bone
Fluid balance
Component of DNA, RNA, cell membranes, and ATP
Recommended Intake: 700 mg/day for adults.
Food Sources: Protein-rich foods (milk, meats, eggs), processed foods, soft drinks (phosphoric acid).
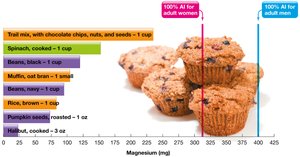
Magnesium
Magnesium is a major mineral, with 50–60% stored in bones. It is a cofactor for hundreds of enzymes and is vital for energy production and nucleic acid synthesis.
Functions:
Bone structure
Cofactor for over 300 enzymes
ATP production
DNA and protein synthesis and repair
Recommended Intake: 310 mg/day for women, 400 mg/day for men (ages 19–30).
Food Sources: Green leafy vegetables, whole grains, seeds, nuts, seafood, beans, some dairy products.
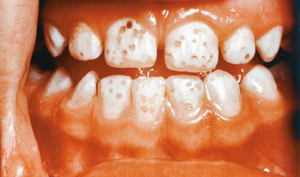
Fluoride
Fluoride is a trace mineral stored mainly in bones and teeth. It strengthens tooth enamel and helps prevent dental caries.
Functions:
Development and maintenance of teeth and bones
Combines with calcium and phosphorus to strengthen enamel
Sources: Fluoridated water and dental products
Toxicity: Fluorosis (porous, stained, and pitted teeth)
Deficiency: Increased risk of dental caries
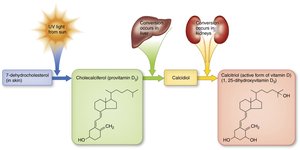
Vitamin D
Vitamin D is a fat-soluble vitamin that acts as a hormone. It is essential for calcium and phosphorus absorption and bone mineralization.
Synthesis: Produced in the skin upon exposure to UV light; activated in the liver and kidneys.
Functions:
Enhances calcium and phosphorus absorption
Regulates blood calcium levels
Stimulates osteoclast activity
Necessary for bone calcification
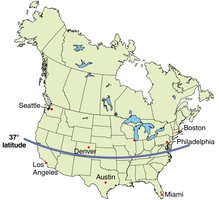
Geographic Considerations: Sunlight exposure varies by latitude, affecting vitamin D synthesis.
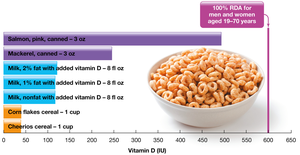
Food Sources: Fortified foods (milk, cereals), fatty fish, supplements.
Toxicity: Hypercalcemia from excessive supplements (not sunlight).
Deficiency: Rickets in children, osteomalacia in adults.

Osteoporosis
Definition and Pathophysiology
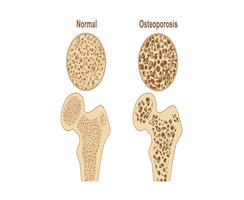
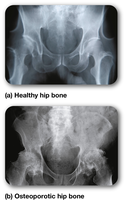
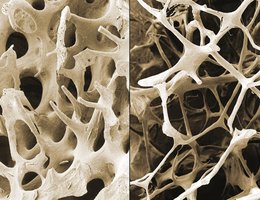
Osteoporosis is a disease characterized by low bone mass and deterioration of bone tissue, leading to fragile bones and increased fracture risk.
Features: Thinner, more porous bones; reduced ability to bear weight; increased risk of fractures.
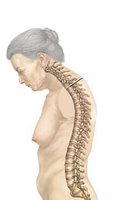
Physical Signs: Compaction of bone, decreased height, and kyphosis (dowager’s hump).
Signs and Symptoms
Persistent and sharp back pain
Decline in height
Dowager’s hump (spinal curvature)

Risk Factors for Osteoporosis
Multiple factors influence the risk of developing osteoporosis, including genetics, nutrition, lifestyle, and hormonal status.
Nutritional Factors: Adequate intake of calcium, vitamin D, and protein is protective; deficiencies increase risk.
Diet: Diets high in fruits and vegetables are associated with improved bone health.
Malnutrition and Eating Disorders: Increase risk, especially during adolescence.
Physical Activity: Regular weight-bearing exercise increases bone mass and reduces fall risk; excessive exercise with inadequate nutrition (as in RED-S) is harmful.
Other Factors: Age, gender (higher risk in women), family history, smoking, alcohol abuse, hormonal changes (e.g., menopause).

Prevention and Treatment of Osteoporosis
There is no cure for osteoporosis, but progression can be slowed and risk reduced through lifestyle and dietary strategies.
Adequate calcium and vitamin D intake
Regular weight-bearing exercise
Maintaining a healthy body weight
Avoiding smoking and excessive alcohol consumption
Medications may be prescribed in some cases
Summary Table: Key Nutrients in Bone Metabolism
Nutrient | Main Functions | Recommended Intake | Major Food Sources | Deficiency Effects | Toxicity Effects |
|---|---|---|---|---|---|
Calcium | Bone/teeth structure, muscle contraction, nerve transmission | 1,000 mg/day (adults 19–50) | Dairy, leafy greens, fortified foods | Osteoporosis, muscle spasms | Kidney stones, impaired absorption of other minerals |
Phosphorus | Bone mineralization, energy metabolism | 700 mg/day | Milk, meats, eggs, processed foods | Rare | Muscle spasms, convulsions |
Magnesium | Bone structure, enzyme cofactor, ATP production | 310 mg (women), 400 mg (men) | Leafy greens, nuts, whole grains | Muscle cramps, weakness | Diarrhea (from supplements) |
Fluoride | Tooth and bone strength | 3–4 mg/day | Fluoridated water, dental products | Dental caries | Fluorosis |
Vitamin D | Calcium/phosphorus absorption, bone mineralization | 600 IU/day (adults <70) | Fortified milk, fatty fish, sunlight | Rickets, osteomalacia | Hypercalcemia |
