 Back
BackRegulation of Food Intake and Dietary Approaches to Weight Management
Study Guide - Smart Notes

Biological, Psychological, and Social-Cultural Factors in Food Intake
Role of the Hypothalamus
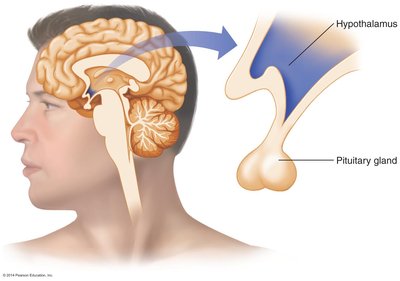
The hypothalamus is the primary control center for hunger and satiety, integrating signals from the gastrointestinal tract and the bloodstream to regulate food intake. It senses nutrient levels and responds to hormonal and neural signals to determine when to initiate or stop eating.
Low nutrient levels stimulate the hunger center.
High nutrient levels stimulate the satiety center.
Physiological and Psychological Drivers of Eating
Hunger: The Physiological Need to Eat
Hunger is a non-specific physiological drive that can be satisfied by a variety of foods. It is triggered by signals such as stomach contractions and the release of the hormone ghrelin, which increases before meals and decreases after nutrient absorption.
Stomach contractions send neural signals to the hypothalamus.
Ghrelin is the only gut hormone known to increase hunger.

Appetite: The Psychological Desire to Eat
Appetite refers to the psychological desire to eat specific foods, often driven by cravings rather than physiological need. It can be influenced by sensory experiences, emotions, and environmental cues.

Satiety: The Sensation of Fullness
Satiety is the feeling of fullness that signals the cessation of eating. It is regulated by the stretching of the stomach and the release of various hormones from the GI tract, pancreas, and adipose tissue.
Cholecystokinin (CCK): Released in response to fat and protein in the gut, decreases hunger and stimulates digestive processes.
Leptin: Secreted by adipose tissue, signals long-term energy stores and suppresses hunger.
Hormonal Regulators of Hunger and Satiety
Several hormones play key roles in regulating hunger and satiety by acting on the hypothalamus and other brain regions.
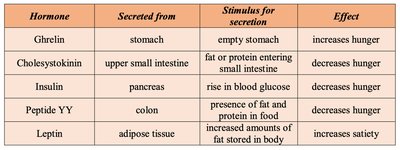
Hormone | Secreted from | Stimulus for secretion | Effect |
|---|---|---|---|
Ghrelin | Stomach | Empty stomach | Increases hunger |
Cholecystokinin (CCK) | Upper small intestine | Fat or protein entering small intestine | Decreases hunger |
Insulin | Pancreas | Rise in blood glucose | Decreases hunger |
Peptide YY | Colon | Presence of fat and protein in food | Decreases hunger |
Leptin | Adipose tissue | Increased amounts of fat stored in body | Increases satiety |
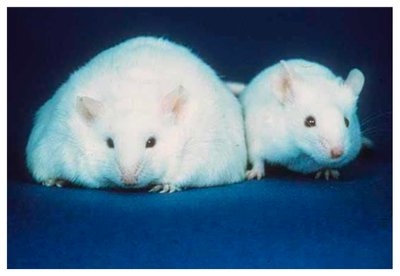
Leptin and Obesity
Leptin is a hormone that signals satiety and energy sufficiency. In animal studies, a lack of leptin leads to constant hunger and obesity. However, most obese humans are resistant to leptin's effects, so leptin supplementation is not effective for weight loss in humans.
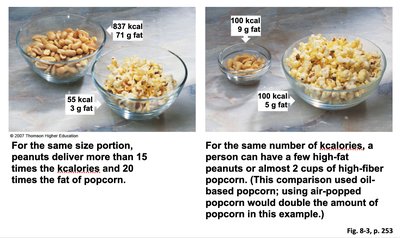
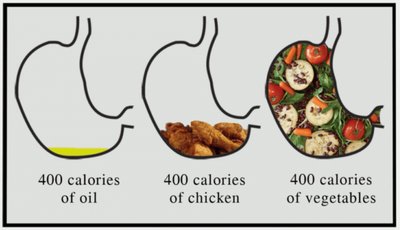
How Types of Foods Affect Hunger and Satiety
Different foods have varying effects on hunger and satiety. Protein-rich foods have the highest satiety value, followed by fats and then carbohydrates. Bulky, high-fiber, and water-rich foods promote fullness by distending the stomach.
Solid foods are more filling than semi-solid or liquid foods.
Nutrient-dense, low-calorie, plant-based diets help promote satiety.

Psychological and Environmental Influences on Eating
Overriding Satiety
Appetite, social interactions, stress, boredom, and the availability of ultra-processed foods can override physiological satiety signals, leading to overeating. Foods high in fat, sugar, and salt are often engineered to promote 'mindless munching.'




Dietary Approaches to Weight Loss
There is no single superior dietary strategy for weight loss. Effective approaches include the Mediterranean Diet, DASH Diet, vegetarian diets, and lower-calorie macronutrient diets. Each has unique benefits and considerations.
Mediterranean Diet
The Mediterranean Diet emphasizes whole grains, fruits, vegetables, legumes, nuts, olive oil, and moderate consumption of fish and poultry. It is associated with reduced risk of cardiovascular disease and cancer, but may be high in calories if not portion-controlled.




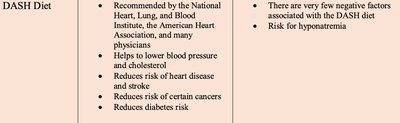
DASH Diet
The DASH (Dietary Approaches to Stop Hypertension) Diet is designed to lower blood pressure and LDL cholesterol. It emphasizes vegetables, fruits, whole grains, low-fat dairy, fish, poultry, beans, and nuts, while limiting sodium, sweets, and red meats.

Vegetarian and Vegan Diets
Vegetarian and vegan diets may reduce the risk of chronic diseases and aid in weight management. However, they require careful planning to avoid nutrient deficiencies, particularly in protein, iron, zinc, omega-3 fatty acids, and vitamin B12.


Low-Carbohydrate and Keto Diets
Low-carb and ketogenic diets restrict carbohydrate intake and increase fat and protein consumption. While they may improve blood sugar and cholesterol levels temporarily, they are not entirely evidence-based and may not meet the recommended dietary allowance (RDA) for carbohydrates.


Caloric Restriction and Intermittent Fasting
Moderate-fat, high-carbohydrate, moderate-protein diets (e.g., Weight Watchers, Jenny Craig) promote gradual weight loss through energy deficits of 500-1000 kcal/day. Intermittent fasting involves cycles of eating and fasting, which may provide some benefits similar to caloric restriction.

Other Approaches to Treat Obesity
Additional interventions include prescription drugs (e.g., fat-binding agents, appetite suppressants), over-the-counter supplements, and bariatric surgeries (e.g., gastric bypass, sleeve gastrectomy). These approaches carry risks such as nutrient deficiencies and surgical complications.
Glucagon-Like Peptide 1 (GLP-1) Agonists
GLP-1 agonists (e.g., semaglutide) are effective in decreasing appetite and slowing gastric emptying, but are expensive and may cause gastrointestinal side effects. Weight regain is common after discontinuation.
Summary Table: Hormonal Regulation of Hunger and Satiety
Hormone | Source | Stimulus | Effect |
|---|---|---|---|
Ghrelin | Stomach | Empty stomach | Increases hunger |
CCK | Small intestine | Fat/protein in gut | Decreases hunger |
Insulin | Pancreas | High blood glucose | Decreases hunger |
Peptide YY | Colon | Fat/protein in food | Decreases hunger |
Leptin | Adipose tissue | Increased fat stores | Increases satiety |
Additional info: The notes above integrate and expand upon the provided content, ensuring a comprehensive overview of the regulation of food intake and dietary strategies for weight management, as relevant to college-level nutrition studies.
