Back
BackThe Human Body & Digestion: Hunger, Satiety, Hormones, and the Digestive System
Study Guide - Smart Notes

Hunger, Satiety, and Hormones
Introduction to Hunger and Satiety
The regulation of hunger and satiety is a complex process involving physiological, hormonal, and neural mechanisms. Understanding these processes is essential for nutrition students, as they underpin eating behaviors and energy balance.
Hunger: The physiological drive to eat, triggered by internal cues such as an empty stomach.
Appetite: The psychological desire to eat, often stimulated by external cues like the sight or smell of food.
Satiety: The feeling of fullness that signals us to stop eating.
The body uses hormonal and neural signals to regulate hunger and satiety.
Hormonal Regulation
Hormones act as chemical messengers in the body, playing a crucial role in signaling hunger and satiety to the brain, particularly the hypothalamus.
Ghrelin: Produced in the stomach, stimulates hunger when the stomach is empty.
Cholecystokinin (CCK): Released from the small intestine, promotes satiety by stimulating the release of digestive fluids and slowing gastric emptying.
Insulin: Secreted by the pancreas in response to elevated blood glucose, promotes satiety.
Leptin: Produced by fat cells, signals long-term energy stores and suppresses appetite.
Neural Regulation
Nerve cells in the stomach and small intestine detect stretching and chemical composition, sending signals to the brain to indicate hunger or fullness.
Stretch receptors in the stomach wall detect fullness.
Chemoreceptors sense nutrient content, contributing to satiety signals.
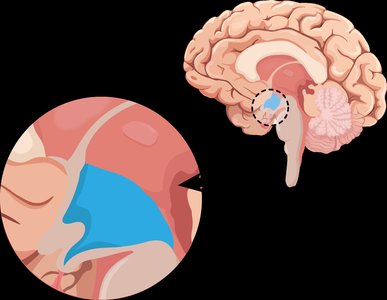
The Role of the Hypothalamus
The hypothalamus is a region of the brain that integrates hormonal and neural signals to regulate hunger and satiety.
Contains both a hunger center and a satiety center.
Receives information from hormones and nerve cells, then sends signals to initiate or stop eating.

Hormones and the Digestive System
Blood Glucose Regulation
Blood glucose levels are tightly regulated by hormones produced by the pancreas.
Insulin: Promotes uptake of glucose by the liver and other tissues, lowering blood sugar.
Glucagon: Stimulates the liver to release glucose, raising blood sugar.
Hormonal Control of Hunger and Satiety
Cholecystokinin (CCK): Released from the small intestine, stimulates the gallbladder and pancreas, and signals satiety to the hypothalamus.
Leptin: Released from fat cells, regulates long-term food intake and energy balance.
Ghrelin: Released from the stomach when empty, stimulates hunger.
Overview of the Digestive System
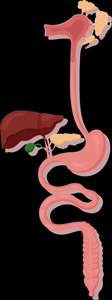
Gastrointestinal Tract (GI Tract)
The GI tract is a 30-foot-long muscular tube responsible for the digestion and absorption of nutrients.
Mouth: Ingestion of food and water.
Esophagus: Transports food to the stomach.
Stomach: Breaks down food into smaller molecules.
Small Intestine: Digests food molecules and absorbs nutrients.
Large Intestine: Absorbs water and eliminates waste as feces.
Sphincters: Ensure one-way movement of food.
Accessory Organs
Accessory organs aid digestion but are not part of the GI tract itself.
Teeth & Tongue: Mechanically break apart food.
Salivary Glands: Release saliva containing digestive enzymes.
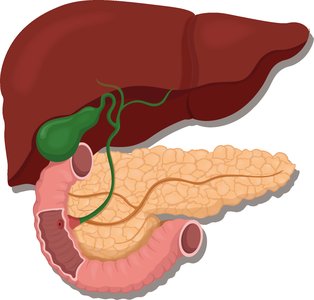
Liver: Produces bile and stores nutrients.
Gallbladder: Stores and releases bile.
Pancreas: Produces digestive enzymes.
Functions of the Digestive System
Major Processes
Ingestion: Intake of food and water.
Propulsion: Movement of food through the GI tract via swallowing and peristalsis.
Digestion: Breakdown of food into absorbable molecules.
Absorption: Uptake of nutrients and water into blood or lymph.
Defecation: Elimination of waste as feces.
Types of Digestion
Mechanical Digestion: Physical breakdown of food (e.g., chewing, churning).
Chemical Digestion: Enzymatic breakdown of macromolecules.
Key Enzymes:
Amylase: Carbohydrates → simple sugars
Lipase: Fats → fatty acids
Protease/Pepsin: Proteins → amino acids
Organs of the Gastrointestinal Tract
Mouth and Esophagus
The mouth is the first site of digestion, involving both mechanical and chemical processes.
Mechanical Digestion: Chewing with teeth and mixing with saliva.
Chemical Digestion: Saliva contains amylase (for carbohydrates) and lipase (for lipids).
Esophagus: Connects mouth to stomach; food is propelled by peristalsis.
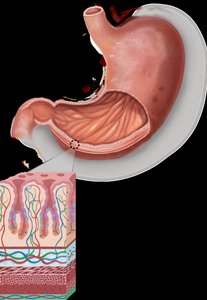
Stomach
The stomach is a muscular organ that continues mechanical and chemical digestion.
Mechanical Digestion: Peristalsis mixes food with gastric juices.
Chemical Digestion: Gastric acid denatures proteins; pepsin digests proteins; gastric lipase digests fats.
Protection: Mucous lining protects stomach tissue from acid.
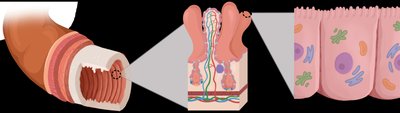
Small Intestine
The small intestine is the primary site for digestion and absorption of nutrients.
Divided into duodenum (initial area), jejunum (digestion and absorption), and ileum (absorption).
Mechanical Digestion: Peristalsis and segmentation.
Chemical Digestion: Bile from the gallbladder emulsifies fats; pancreatic juice contains amylase, lipase, and protease.
Features: Villi and microvilli increase surface area for absorption; brush border enzymes complete digestion.
Large Intestine
The large intestine absorbs water, minerals, and some vitamins, and forms feces.
Includes the cecum, colon, and rectum.
Absorbs water, sodium, potassium, and vitamins K, B1, B7, B12.
Hosts the gut microbiome: a diverse ecosystem of bacteria.
Accessory Organs
Liver, Gallbladder, and Pancreas
Liver: Produces bile, processes and stores nutrients.
Gallbladder: Stores and releases bile as needed.
Pancreas: Releases digestive enzymes (amylase, lipase, protease) into the small intestine.

Nutrient Absorption and Transport
Mechanisms of Absorption
Passive Diffusion: Movement from high to low concentration across the membrane without energy.
Facilitated Diffusion: Movement from high to low concentration through a protein carrier, no energy required.
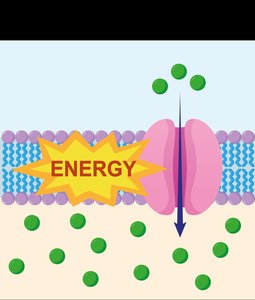
Active Transport: Movement against the concentration gradient using a protein carrier and energy.
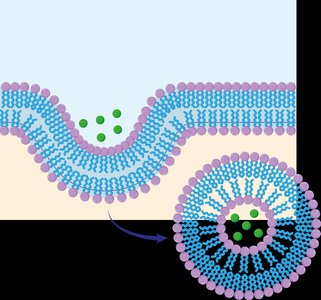
Endocytosis: Cell membrane engulfs nutrients to bring them into the cell.
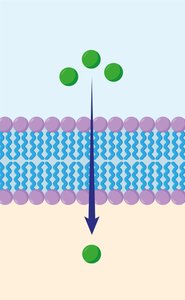
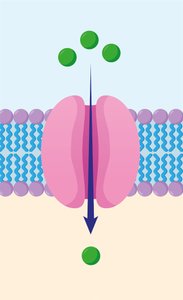
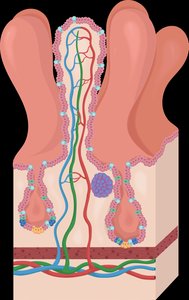
Nutrient Transport
Water-soluble nutrients: Absorbed into capillaries, travel to the liver via the hepatic portal vein.
Fat-soluble nutrients: Absorbed into lacteals (lymphatic system), then enter the bloodstream.
Gut Microbiome
Functions and Importance
The gut microbiome consists of trillions of bacteria in the large intestine, playing vital roles in health and digestion.
Ferments undigested carbohydrates, producing gases and short-chain fatty acids.
Produces certain vitamins (K and B vitamins).
Inhibits harmful bacteria and stimulates the immune system.
Prebiotics and Probiotics
Prebiotics: Non-digestible food components (e.g., fiber, inulin) that nourish beneficial gut bacteria.
Probiotics: Live beneficial bacteria found in fermented foods (e.g., yogurt, kimchi, sauerkraut).
Disorders of the Digestive System
Stomach and Esophagus Pathologies
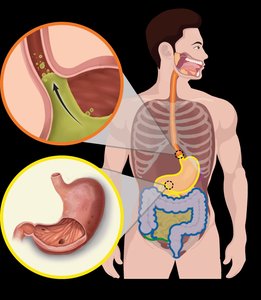
Heartburn: Stomach acid moves into the esophagus, causing a burning sensation.
Gastroesophageal Reflux Disease (GERD): Chronic heartburn due to malfunction of the esophageal sphincter.
Peptic Ulcers: Open sores in the stomach lining, often caused by Helicobacter pylori infection or NSAIDs.
Small and Large Intestine Pathologies
Celiac Disease: Autoimmune disorder where gluten triggers immune damage to the small intestine villi.
Diarrhea: Excess water in stool, risk of dehydration.
Constipation: Too little water in stool, resulting in hard, difficult-to-pass feces.
Irritable Bowel Syndrome (IBS): Chronic abdominal pain, bloating, and altered bowel habits with no known cause.
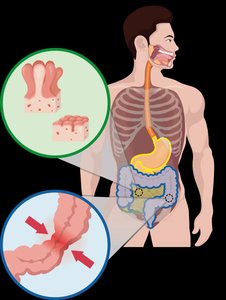
Cancer of the GI Tract
Colorectal cancer: Third most common and second most deadly cancer in the GI tract.
Symptoms: Persistent changes in bowel habits, blood in stool, abdominal pain.
Prevention: Diets high in fiber, regular colonoscopies to remove polyps.
Risk Factors: Obesity, sedentary lifestyle, smoking, alcohol, red meat consumption.