 Back
BackAssessment and Health of the Eye: Clinical Concepts and Examination
Study Guide - Smart Notes

The Eye: Clinical Concepts and Health Assessment
Introduction to Eye Health and Assessment
The eye is a vital sensory organ responsible for vision, and its assessment is a key component of personal health evaluation. Understanding the structure, function, and common examination techniques is essential for identifying visual problems and maintaining ocular health.
Health History in Eye Assessment
Key Components of Ocular Health History
Visual Difficulty: Includes blurred vision, double vision (diplopia), or sudden vision loss.
Pain: Ocular pain may indicate infection, inflammation, or injury.
Strabismus/Diplopia: Misalignment of the eyes or double vision.
Redness/Swelling: Signs of infection, allergy, or trauma.
Watering/Discharge: May indicate infection or blocked tear ducts.
History of Ocular Problems: Includes glaucoma, cataracts, or previous surgeries.
Use of Glasses/Contact Lenses: Important for understanding baseline vision.
Self-care Behaviors: Eye hygiene, use of protective eyewear.
Medications: Some drugs affect vision or ocular health.
Vision Loss: Sudden or gradual loss requires urgent evaluation.
Infants: Maternal history (e.g., vaginal infections), developmental milestones, and visual tracking are assessed.
Aging: Common issues include loss of depth perception, peripheral vision, night vision, glaucoma, and cataracts.
Physical Assessment of the Eye
Central Visual Acuity
Central visual acuity measures the eye's ability to see details at a distance and near. It is a fundamental part of the eye examination.
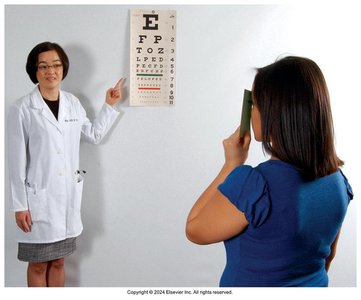
Distant Vision: Assessed using the Snellen Eye Chart. The numerator is the testing distance (usually 20 feet), and the denominator is the smallest line read correctly.
Interpretation: 20/30 means the patient sees at 20 feet what a normal eye sees at 30 feet. A higher denominator indicates myopia (nearsightedness).
Near Vision: Tested with a Jaeger card held 14 inches from the eyes. Normal is 14/14.
Common Refractive Errors: Presbyopia (age-related near vision loss), Myopia (nearsightedness), Hyperopia (farsightedness).


Visual Fields and Peripheral Vision
Confrontation Test
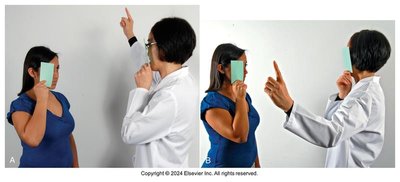
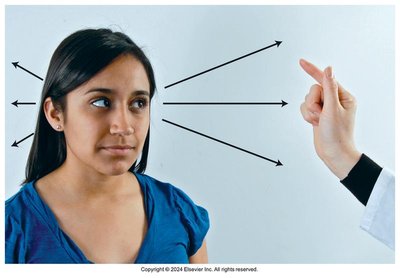
The confrontation test assesses the range of peripheral vision by comparing the patient's field of vision with that of the examiner.
Procedure: The examiner and patient cover opposite eyes and move a finger or object into the visual field from various angles.
Normal Ranges: 50° superiorly, 60° nasally, 90° temporally, 70° inferiorly.

Extraocular Muscle Function
Assessment of Muscle Strength and Cranial Nerve Function
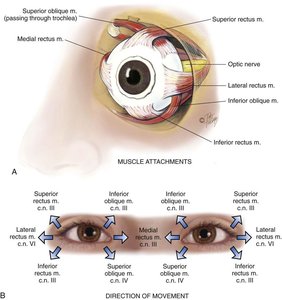
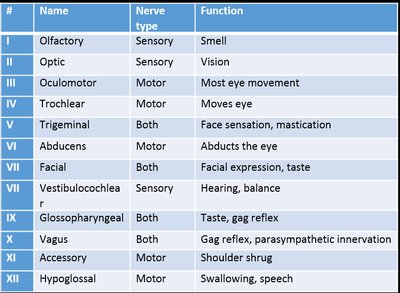
Extraocular muscle function is tested to evaluate the integrity of the muscles and cranial nerves controlling eye movement.
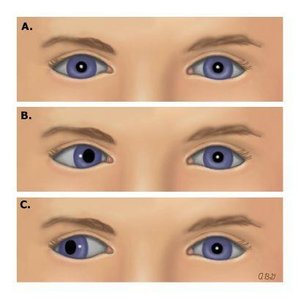
Corneal Light Reflex (Hirschberg's Test): Assesses parallel alignment of the eyes by observing the reflection of light on the corneas.
Cover-Uncover Test: Detects deviated alignment (strabismus) by covering one eye and observing movement in the uncovered eye.
Diagnostic Positions Test: Evaluates parallel tracking, nystagmus (involuntary movement), and lid lag by moving a finger in six cardinal directions.

External Ocular Structures
Inspection and Palpation
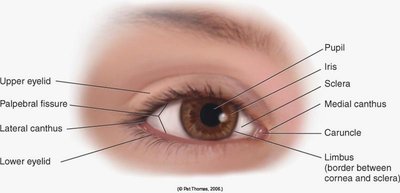
Assessment of external ocular structures includes inspection of the eyebrows, eyelids, eyelashes, eyeballs, conjunctiva, sclera, and lacrimal apparatus.
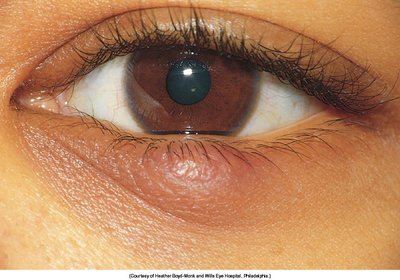
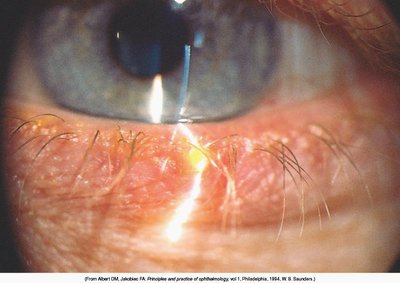
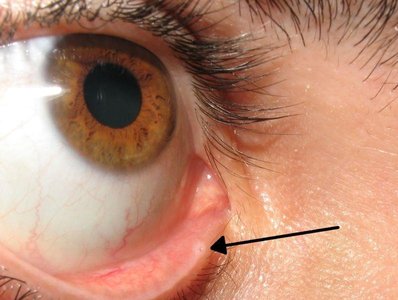
Chalazion: Chronic inflammation of a meibomian gland, presenting as a painless nodule.
Hordeolum (Stye): Acute infection of an eyelash follicle or gland, presenting as a painful, red swelling.
Palpation of Lacrimal Sac: Checks for tenderness or swelling, which may indicate infection or blockage.
Eversion of Upper Lid: Used to inspect for foreign bodies or lesions.

Anterior Eyeball Structures
Cornea, Lens, Iris, and Pupil
The anterior segment of the eye includes the cornea, lens, iris, and pupil. These structures are inspected for clarity, shape, and response to light.
Pupil Size: Normal at rest is 3–5 mm. Unequal pupils (anisocoria) may be normal or indicate pathology.
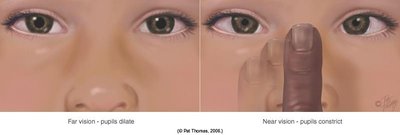
Pupillary Light Reflex: Direct and consensual constriction of the pupils in response to light. Normal response is described as PERRLA (Pupils Equal, Round, Reactive to Light and Accommodation).
Accommodation: Constriction and convergence of the pupils when focusing on a near object.


Ophthalmoscopic Examination
Use and Features of the Ophthalmoscope
The ophthalmoscope is used to examine the internal structures of the eye, including the retina, optic disc, and blood vessels.
Lens Selector Dial: Adjusts for refractive errors (black/green for farsighted, red for nearsighted).
Viewing Apertures: Different apertures for dilated/undilated pupils, red-free filter, grid, and slit for specialized examination.
Technique: Performed in a dark room, both examiner and patient remove glasses, and the examiner uses the right hand and eye for the patient's right eye.
Red Reflex: The first sign seen when light reflects off the retina.




Ocular Fundus (Retina) Examination
Structures and Findings
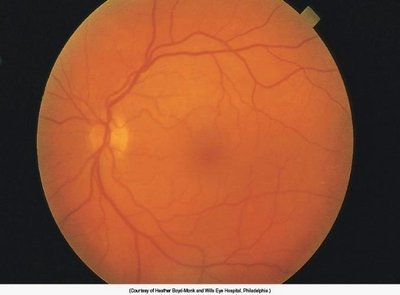
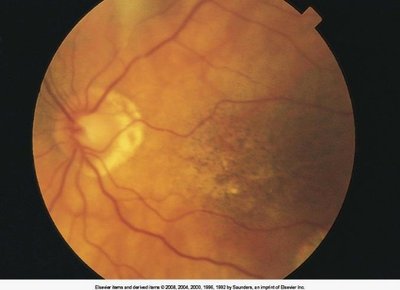
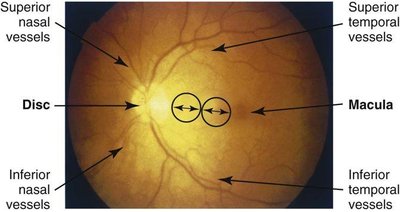
The ocular fundus includes the optic disc, retinal vessels, background, and macula. Examination can reveal signs of systemic disease and ocular pathology.
Optic Disc: The point where the optic nerve enters the retina; contains a physiological cup.
Retinal Vessels: Assessed for signs of vascular disease.
Macula and Fovea: Area of sharpest vision, inspected last due to sensitivity.
Scleral Crescent and Disc Diameter (DD): Anatomical variations seen during examination.

Developmental Considerations
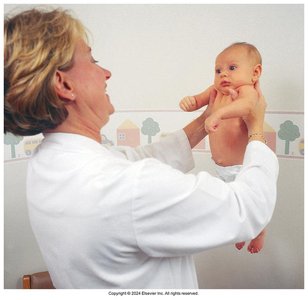
Infants and Children
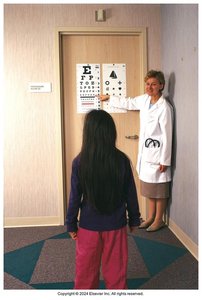
Visual Acuity: Assessed by response to objects, Allen test (2–2.5 years), and Snellen E chart (3–6 years).
Extraocular Movements (EOM): Slight nystagmus is normal under 2 months.
Chemical Conjunctivitis: May occur in newborns due to prophylactic eye drops.
Fundus Examination: May require distraction or play.
Aging Adult
Decreased Central Acuity: Common after age 70.
Decreased Lacrimation: Leads to dry eyes.
Decreased Pupil Size: Pupils become smaller and less responsive.
Pingueculae: Yellowish nodules on the sclera due to sun exposure.
Arcus Senilis: Gray-white arc around the cornea, common with aging.
Xanthelasma: Yellowish plaques on the eyelids, associated with lipid disorders.
Summary Table: Common Eye Examination Techniques
Test | Purpose | Normal Finding |
|---|---|---|
Snellen Chart | Distant visual acuity | 20/20 |
Jaeger Card | Near visual acuity | 14/14 |
Confrontation Test | Peripheral vision | Full visual fields |
Corneal Light Reflex | Eye alignment | Symmetrical reflection |
Cover-Uncover Test | Strabismus detection | No movement of uncovered eye |
Diagnostic Positions | Extraocular muscle function | Smooth, coordinated movement |
Ophthalmoscopy | Internal eye structures | Clear disc, vessels, macula |
Additional info: This guide integrates clinical concepts from nursing and personal health, emphasizing the importance of eye assessment in overall health and disease prevention.
