 Back
BackBreast Anatomy, Assessment, and Health Promotion: Study Guide for Personal Health Students
Study Guide - Smart Notes

The Breast and Regional Lymphatics
Breast Anatomy
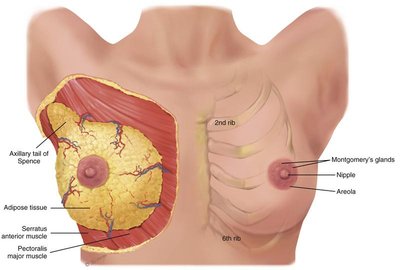
The breast is a complex structure composed of glandular, adipose, and connective tissues, and is supported by muscles and lymphatic drainage. Understanding its anatomy is essential for clinical assessment and health promotion.
Key Structures:
Axillary tail of Spence: Extension of breast tissue into the axilla, important for assessment.
Adipose tissue: Provides shape and protection.
Areola and nipple: Central features, contain Montgomery's glands.
Muscles: Pectoralis major and serratus anterior support the breast.
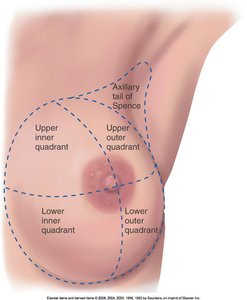
Quadrants: The breast is divided into four quadrants (upper/lower, inner/outer) for clinical localization of findings.
Health History and Risk Factors
Collecting a thorough health history is crucial for identifying potential breast issues and risk factors for disease.
Symptoms:
Pain (mastalgia)
Lump
Discharge
Rash
Swelling
Trauma
History:
Previous breast disease or surgery
Self-care behaviors (e.g., breast self-exam)
Axilla (armpit) symptoms
Developmental Considerations:
Preadolescent: Breast changes
Pregnant: Changes, breastfeeding
Menopausal: Changes
Risk Factors: Family history, age, hormonal factors, lifestyle
Physical Assessment of the Breast
Physical assessment includes inspection and palpation to detect abnormalities and ensure breast health.
Inspection:
Skin changes (orange-peel, prominent venous pattern)
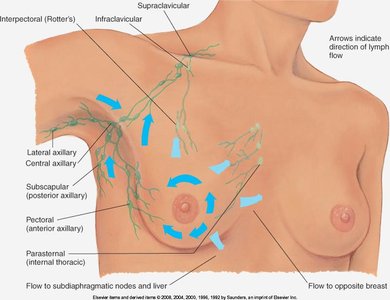
Lymphatic drainage areas
Nipple and areola (discharge, color, retraction)
Axillae
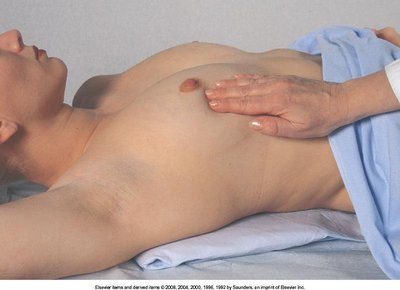
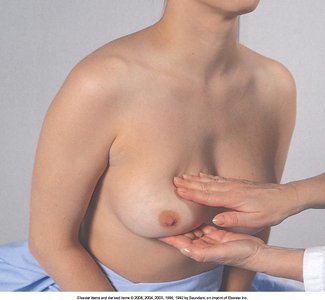
Palpation:
Support arm and move through range of motion
Use 3 finger pads with rotary motion
Palpate every inch of breast and tail of Spence
Apply light, medium, and firm pressure
Bimanual technique for large breasts
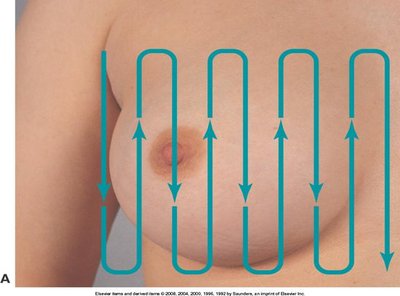
Palpation Patterns:
Grid pattern
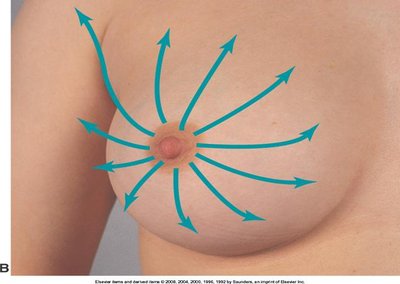
Spokes of wheel
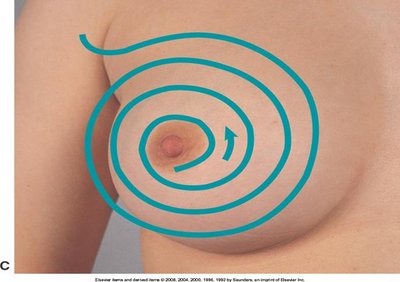
Circular pattern
Masses:
Note location, size, shape, distinctness, consistency, mobility, tenderness, lymphadenopathy
Nipples:
Induration, mass under areola, discharge, color
Retraction or deviation
Common Breast Findings
Several findings may be observed during breast assessment, some of which require further investigation.
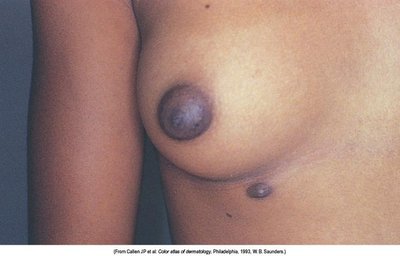
Supernumerary Nipple: Extra nipple along the embryonic milk line.
Edema (Peau d’Orange): Skin appears like an orange peel, often due to lymphatic obstruction.
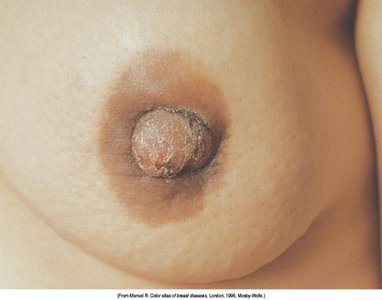
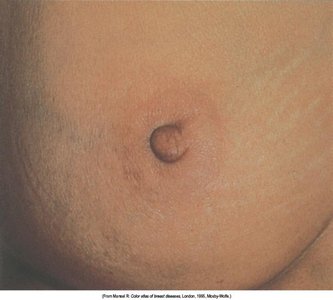
Retraction: Nipple or skin pulled inward, may indicate underlying mass.
Induration: Hardening of tissue under the areola.
Discharge: Color and consistency should be noted.
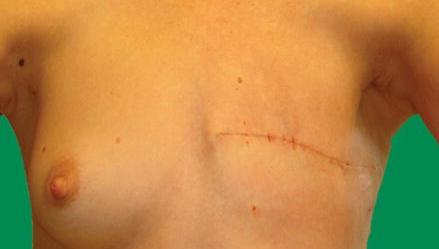
Mastectomy Site: Assess scar and remaining tissue for recurrence or complications.
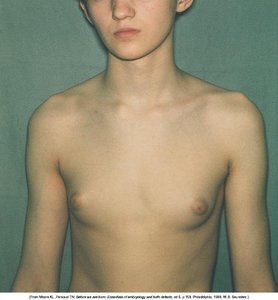
Male Breast Assessment
Male breast assessment is similar to female, with attention to gynecomastia (enlargement) and other abnormalities.
Gynecomastia: Benign enlargement of male breast tissue, often due to hormonal changes.
Inspection and Palpation: As with female breast, check for masses, tenderness, and skin changes.

Developmental Considerations
Breast development and changes occur throughout life, influenced by hormonal and physiological factors.
Infants & Children:
Enlargement due to maternal estrogen
Witch’s milk: Temporary milk secretion
Adolescents:
Asymmetry common during growth
Tanner’s Staging: Five stages of breast development
Pregnant:
Increased size, vascularity, striae, darker areola/nipples, colostrum production
Lactating:
Milk production begins 3rd day postpartum
Engorgement, redness, warmth, hard tissue
Nipples may be cracked or sore
Older Adult:
Pendulous, sagging, retracted nipples
Breast awareness important due to increased risk after age 50
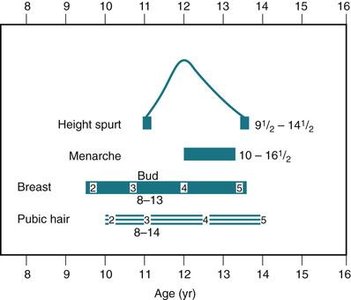
Tanner’s Staging of Breast Development
Tanner’s Staging is used to classify breast development in adolescents:
Stage 1 (Preadolescent): Only a small elevated nipple is present.
Stage 2 (Breast bud stage): Small mound of breast and nipple develops; areola widens.
Stage 3: Breast and areola enlarge; nipple flush with breast surface.
Stage 4: Areola and nipple form a secondary mound over the breast.
Stage 5 (Mature breast): Only the nipple protrudes; areola flush with breast contour.
Health Promotion and Screening Recommendations
Health promotion focuses on education, risk reduction, and appropriate screening for breast cancer.
Canadian Task Force on Preventive Health Care (CTFPHC) Recommendations:
Do not use MRI, tomosynthesis, or ultrasound for screening in women not at increased risk.
Do not perform clinical breast examinations to screen for breast cancer.
Do not advise women to practice breast self-examination for screening.
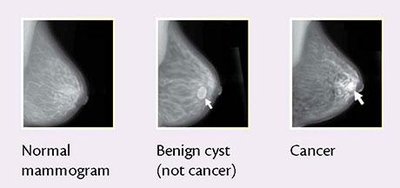
Mammography: Remains the primary screening tool for breast cancer.
Summary Table: Breast Assessment Patterns
The following table summarizes the main breast palpation patterns used in clinical assessment:
Pattern | Description | Image Reference |
|---|---|---|
Grid | Vertical strips across the breast | image_11 |
Spokes of Wheel | Radial lines from nipple outward | image_12 |
Circular | Concentric circles from nipple outward | image_13 |
Additional info:
Breast self-examination is no longer recommended for routine screening, but breast awareness is encouraged for recognizing changes.
Clinical judgment, client education, and communication are essential concepts in breast health promotion.
