 Back
BackDeterminants of Health and Disease: Foundations for Personal Health
Study Guide - Smart Notes

Introduction to Health, Disease, and Wellness
Defining Health, Disease, Illness, and Sickness
Understanding the foundational concepts of health, disease, and wellness is essential for personal and population health studies. These terms, while related, have distinct meanings and implications for health outcomes and interventions.
Health: According to the World Health Organization (WHO), health is "a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity." A functional definition emphasizes the capacity to adapt to, respond to, or control life's challenges and changes.
Disease: A biological or physical malady affecting the body.
Illness: The perception of dysfunction by the afflicted individual.
Sickness: The social acknowledgement of impairment or affliction.
Example: A person with well-managed diabetes may be considered healthy if they can function well, despite having a disease.
The Relationship Between Disease, Illness, and Sickness
The relationships among disease, illness, and sickness are complex and not always linear. For example:
Disease without Illness: Hypertension may not cause symptoms, so the individual does not feel ill.
Illness without Disease: A person may feel unwell (e.g., hypochondria) without a diagnosable disease.
Sickness without Illness: Social expectations may label someone as sick even if they do not feel ill.
Health and Disease: Not Always Opposites
Health and disease are not necessarily opposites. One can have a disease and still be healthy if the condition is well managed, or be unhealthy without a specific disease due to lifestyle or environmental factors.
Factors That Cause Disease
Major Theories of Disease Causation
Multiple factors contribute to disease, including germs, genetics, lifestyle, and environmental triggers. Understanding these theories helps in designing effective interventions.
Germ Theory: Diseases are caused by microorganisms. Key contributors include:
Koch: Developed postulates to link specific germs to diseases.
Lister: Introduced antiseptic techniques to reduce surgical infections.
Pasteur: Discovered microbial fermentation, sterilization, and pasteurization.



Genetic Theories: Emphasize hereditary vulnerability and the interplay between genetics and environment.
Lifestyle Theories: Focus on individual behaviors such as smoking, alcohol consumption, and diet.
Multifactorial Disease Causation: Diseases often result from a combination of genetic predisposition and environmental triggers (e.g., BRCA gene and breast cancer).
Well-Being and Wellness
Distinguishing Health, Well-Being, and Wellness
While related, these concepts are not identical:
Well-Being: A broad concept encompassing financial security, work, family, environment, and more.
Wellness: The state of feeling well, often used synonymously with health but more focused on the absence of illness.
Determinants of Health
Key Determinants and Models
Determinants of health are broad, interconnected factors influencing individual and population health. The WHO defines them as personal, social, economic, and environmental factors.
Income and social status
Employment and working conditions
Education and literacy
Physical environments
Social supports and coping skills
Healthy behaviors
Access to health services
Biology and genetic endowment
Gender, culture, race/racism
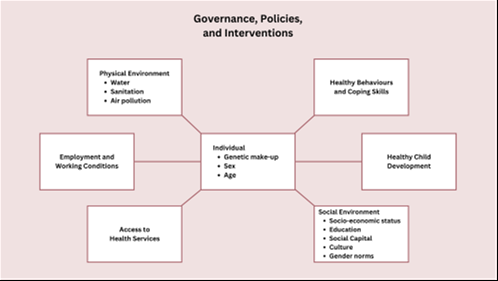
Dahlgren and Whitehead Model
This model groups determinants into layers, from individual factors (age, sex, genetics) to broader socio-economic, cultural, and environmental conditions.
Social and Physical Determinants
Social Determinants: Conditions in which people are born, grow, work, live, and age, shaped by the distribution of money, power, and resources.
Physical Determinants: Environmental factors such as air and water quality, housing, and occupational hazards.
Contextualizing Determinants
Multiple determinants can interact to exacerbate health hazards, such as poverty, poor housing, and lack of education.
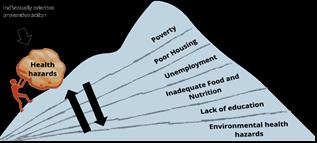
Levels of Determinants
Root Causes: Broad, distal factors (e.g., climate, governance, economic policies).
Underlying Causes: Medium-range factors (e.g., built environment, social context).
Proximal Causes: Immediate factors (e.g., personal behaviors, material circumstances).
Risk Factors
Categories and Examples
Intrinsic: Age, sex, genetic makeup (non-modifiable).
Disease-Related: Existing diseases (e.g., diabetes).
Behavioral: Smoking, alcohol use, diet.
Physical Environment: Air pollution, lack of healthcare access.
Social Environment: Lack of social support, community networks.
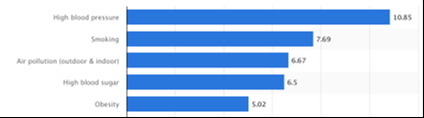
Most Common Risk Factors and Mortality
High blood pressure
Smoking
Air pollution
High blood sugar
Obesity
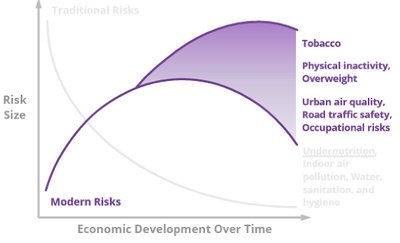
Risk Transition and Societal Development
As societies develop, major health risks shift from traditional (e.g., undernutrition, unsafe water) to modern (e.g., tobacco use, obesity, urban air quality) risks.
Health Inequities
Health Status Indicators
Health status indicators are used to measure and compare health within and across populations. Common indicators include:
Life expectancy at birth
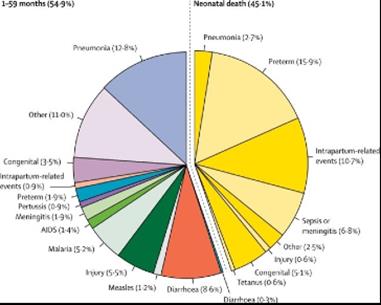
Neonatal mortality rate
Infant mortality rate
Under-5 mortality rate
Maternal mortality ratio
Health Disparities and Inequalities
Health disparities (or inequalities) are differences in health outcomes linked to social or economic disadvantage. These disparities are often patterned by income, geography, and other social determinants.
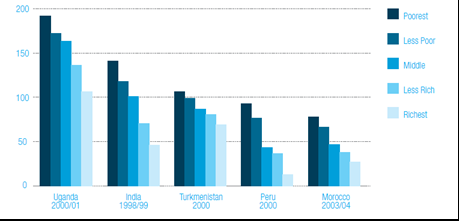
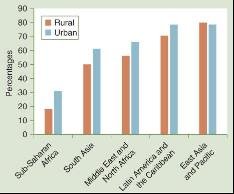
Health Inequity vs. Health Inequality
Health Inequality: Differences in health that are unavoidable (e.g., by age or gender).
Health Inequity: Differences that are avoidable, unnecessary, and unfair, often arising from social conditions.
Conclusion
This module provides a comprehensive foundation for understanding the determinants of health and disease, the complex interplay of social, physical, and behavioral factors, and the importance of addressing health inequities to improve population health outcomes.
