 Back
BackN1016 Exercise, Sleep, and Pain Management - Class 6
Study Guide - Smart Notes

Exercise, Sleep, and Pain Management
Pain: Definition and Impact
Pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage. It is a complex phenomenon with multiple components that affect both psychological and physical functioning.
Pain as the 5th Vital Sign: Pain is considered a vital sign, reflecting not only body function but also how a person feels.
Prevalence: Pain is not a normal part of aging, but its occurrence increases with age. It is one of the most common and feared symptoms, especially at the end of life.
Types of Pain: Physical, psychological, and spiritual pain.
Consequences of Unrelieved Pain: Disruption of physiological and psychological needs, reduced activity, immobility, social isolation, depression, and existential distress.
Pain Myths and Facts
Myths: Pain is a normal part of aging; sensitivity decreases with age; older adults frequently complain of pain; narcotics are unsafe for older adults.
Facts: Pain is often underreported; older adults are sensitive to pain but may have higher tolerance; narcotics can be safely used for moderate to severe pain in older adults.
Pain Assessment in Older Adults
Assessing pain in older adults can be challenging due to communication difficulties, dementia, aphasia, hearing loss, or depression. Pain expression is influenced by history, culture, and individual meaning.
Assessment Methods: Behavioral, activity, vocalization, and physical changes.
Assessment Tools: Brief Pain Inventory, Visual Analogue Scale (VAS), Numerical Rating Scale (1-10).
Example: The Visual Analogue Scale uses faces to represent pain intensity, while the Numerical Rating Scale assigns numbers to grades of pain.
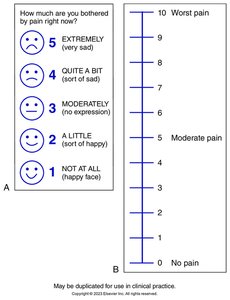
Pain Management Strategies
Pain management involves both pharmacological and non-pharmacological approaches. The goal is to promote comfort and maintain the highest level of function.
Pharmacological Approaches: Analgesics, including non-narcotic and narcotic medications.
Non-Pharmacological Approaches: Physical therapy, biofeedback, distraction, imagery, hypnosis, massage, acupuncture, heat/cold therapy.
Pharmacological Approaches
Non-narcotic Medications: Used for mild to moderate pain. First-line: acetaminophen (max 4 grams/day). NSAIDs (e.g., aspirin, ibuprofen) may cause GI irritation and bleeding; assess risk.


Narcotic Analgesics: Used for acute and persistent pain (moderate to severe), e.g., morphine. Opioids should be used cautiously due to adverse effects; avoid Demerol in older adults.

Non-Pharmacological Approaches
Physical therapy
Biofeedback
Distraction
Imagery
Hypnosis
Massage
Acupuncture
Heat vs Cold
Evaluation of Pain Management
Effectiveness of pain treatment is assessed through ongoing evaluation of pain levels, functional status, and quality of life. The client is the best judge of pain, and medication administration should be based on continuous assessment. Placebos should not be used for pain control.
Fatigue: Definition and Impact
Fatigue in Older Adults
Fatigue is a distressing, persistent, subjective sense of physical, emotional, and/or cognitive tiredness or exhaustion that is not proportional to recent activity and interferes with usual functioning.
Impact: Fatigue can affect daily activities, reduce quality of life, and signal underlying health issues.
Activity and Exercise
Benefits of Exercise for Older Adults
Physical activity is a key indicator of health and wellness. Being active can arrest or delay changes associated with cardiac, respiratory, and musculoskeletal function.
Canadian Guidelines: 150 minutes of moderate to vigorous intensity aerobic activity per week, in bouts of 10 minutes or more. Muscle and bone strengthening activities for major muscle groups at least 2 days per week.
Types of Exercise: Endurance, strength, flexibility, balance, and coordination. Activities should be realistic, meet client goals, be inexpensive, and enjoyable.
Examples: Games, dancing, swimming, yoga, tai chi, and weight-bearing activities.



Rest and Sleep
Importance of Rest and Sleep
All individuals need adequate sleep to conserve energy, prevent fatigue, provide organ respite, and relieve tension. Sleep is a basic physiological need.

Normal Age-Related Changes in Sleep
Longer onset to sleep
Frequent awakenings
Changes in total sleep time
Increased time in bed after age 65
More naps
Lighter sleep: more stage 1, less stages 3 & 4
Increased leg movements
Increased abnormal breathing patterns
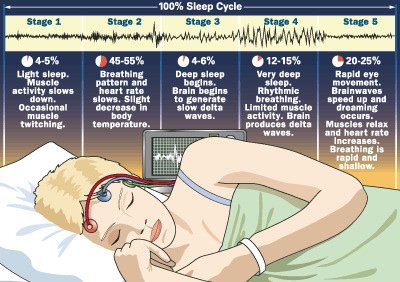
Sleep Disorders in Older Adults
Insomnia
Narcolepsy
Sleep apnea
Restless leg syndrome (nocturnal myoclonus)


Clinical Manifestations of Sleep Disturbance
Difficulty concentrating
Altered thought processes, disorientation, confusion
Irritability
Slurred speech
Delusions and behavioral changes
Nursing Care for Sleep Disturbance
Nursing care involves obtaining a thorough sleep history, assessing sleep/wake patterns, bedtime routines, medications, dietary considerations, environmental factors, and physiological/illness factors.
Sleep Hygiene Strategies: Limit daytime naps to 30 minutes, avoid caffeine near bedtime, maintain a balance of natural light and darkness, reduce noise, ensure comfortable temperature, avoid exercise close to bedtime, establish routines, and manage technology use.

Summary Table: Pain Assessment Tools
Tool | Description | Application |
|---|---|---|
Visual Analogue Scale (VAS) | Faces representing pain intensity | Useful for clients with communication difficulties |
Numerical Rating Scale | Numbers 1-10 for pain intensity | Standard for grading pain |
Brief Pain Inventory | Combination of questions and functional observations | Comprehensive pain assessment |
Summary Table: Pharmacological Approaches
Medication Type | Examples | Indication | Adverse Effects |
|---|---|---|---|
Non-narcotic | Acetaminophen, NSAIDs | Mild to moderate pain | GI irritation, GI bleed (NSAIDs) |
Narcotic | Morphine, opioids | Moderate to severe pain | Adverse effects, avoid Demerol in older adults |
Summary Table: Sleep Hygiene Strategies
Strategy | Description |
|---|---|
Limit naps | 30 minutes, one per day |
Avoid caffeine | Especially near bedtime |
Balance light/dark | Maintain sleep-wake cycle |
Reduce noise | Quiet environment |
Comfortable temperature | Optimal for sleep |
Exercise | Not too close to bedtime |
Establish routines | Consistent bedtime |
Manage technology | Limit screen time before bed |
Conclusion
Effective management of exercise, sleep, and pain is essential for promoting health and wellness in older adults. Comprehensive assessment, evidence-based interventions, and individualized care are key to optimizing function and quality of life.
