 Back
BackMaternal Health and Complications of Pregnancy: Study Guide for Personal Health Students
Study Guide - Smart Notes

Maternal Health
Definition and Importance
Maternal health refers to the health of women during pregnancy, labor, and the postpartum period. It is a critical aspect of public health, as complications during these stages can have significant consequences for both mother and child.
Maternal mortality remains a global concern, with over 700 women dying daily from preventable causes related to pregnancy and childbirth in 2023.
Care by skilled health professionals before, during, and after childbirth is essential for saving lives.

Global Trends in Maternal Mortality
Statistics and Patterns
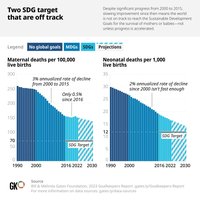
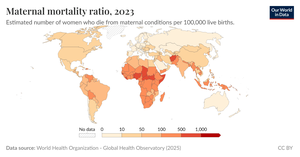
Maternal mortality ratio (MMR) is defined as the number of maternal deaths per 100,000 live births. Global trends show a decline, but disparities persist.
Between 2000 and 2023, MMR dropped by about 40% worldwide.
Over 90% of maternal deaths occur in low- and lower-middle-income countries.
MMR stagnated or increased in some high-income countries, including the US.
Major Complications of Pregnancy
Leading Causes of Maternal Death
Nearly 75% of all maternal deaths are due to a few major complications:
Severe bleeding (mostly after childbirth)
Infections (usually after childbirth)
High blood pressure during pregnancy (pre-eclampsia and eclampsia)
Complications from delivery
Unsafe abortion
Infection in Pregnancy
Maternal Physiological Changes and Risks
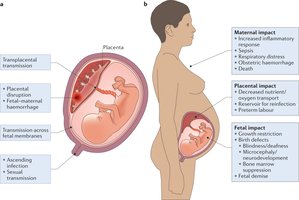
Pregnancy alters maternal physiology, increasing susceptibility to infections. Subtle shifts in immunity and hormonal changes place mothers at greater risk.
High progesterone and decreased smooth muscle tone increase risk of urinary tract infections (pyelonephritis).
The impact of infection depends on the type and timing during gestation.
Sepsis
Sepsis is a life-threatening condition defined as organ dysfunction resulting from infection during pregnancy, childbirth, post-abortion, or postpartum period.
Sepsis is the third most common cause of death in pregnant women.
Accurate assessment is complicated by underreporting of infections.
Bacterial and Viral Infections
Bacterial: Group A strep (maternal sepsis), Group B strep (neonatal infection), Listeria (miscarriage, congenital infection), Hemophilus (meningitis, neonatal infection).
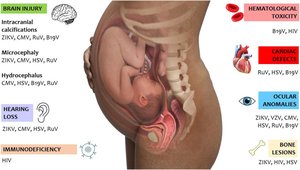
Viral: Rubella (congenital defects), Measles (high maternal mortality), CMV (growth restriction), Parvovirus B19 (hydrops), Varicella (maternal pneumonia), Hepatitis B (miscarriage, death), Zika (microcephaly), Influenza (maternal morbidity), COVID-19 (increased maternal mortality).
Pre-eclampsia
Definition and Diagnosis
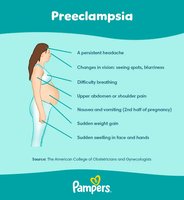
Pre-eclampsia is a pregnancy-specific condition occurring after 20 weeks, characterized by new-onset hypertension and proteinuria.
Blood pressure >140/90 mmHg on two occasions at least 4 hours apart, or one reading >170/110 mmHg.
New onset proteinuria is required for diagnosis.

Global Impact and Risk Factors
Accounts for 14% of all maternal deaths globally.
Associated with limited access to care, obesity, insulin resistance, and hypertension.
Commonest cause of pre-term birth.
Pathophysiology
Pre-eclampsia is a two-stage disease:
Abnormal placentation in early pregnancy
Exaggerated maternal response after 20 weeks
Failure of spiral arteries to adapt leads to decreased placental blood flow and uteroplacental ischemia.
Maternal and Fetal Complications
Maternal: Hypertension, stroke, liver failure (HELLP syndrome), renal dysfunction, clotting disorders, cerebral edema.
Fetal: Growth restriction, stillbirth, pre-term delivery, respiratory distress.

Reducing Risk and Management
Aspirin 75mg daily and calcium supplements may reduce risk.
Weight loss before pregnancy is recommended.
Management includes treating hypertension, magnesium sulfate for seizure prevention, regular monitoring, thromboprophylaxis, and steroids for fetal lung maturation.

Postpartum Considerations
40% of eclamptic fits occur after delivery.
Blood pressure should be monitored closely postpartum.
Women with pre-eclampsia are at increased risk of hypertension later in life.
Labor and Delivery
Definition and Stages
Labor is defined as the onset of regular, painful uterine contractions with progressive cervical dilation and effacement.
Three stages: First (onset to full dilation), Second (full dilation to delivery), Third (delivery of placenta).
Active labor: Cervix 4-6 cm dilated, regular contractions.

Monitoring and Pain Relief
Fetal heart rate monitoring (normal: 120-160 bpm).
Maternal monitoring: heart rate, blood pressure, urine analysis, temperature, contractions, cervical dilation.
Pain relief options: breathing techniques, water, hypnotherapy, TENs, nitrous oxide, narcotics, epidural.
Support and Outcomes
Understanding labor, birth choices, pain relief, and support increases likelihood of successful vaginal delivery.
Complications in Labor
Failure to progress, insufficient contractions, fetal distress, maternal hemorrhage.
Skilled care is essential for recognition and management of complications.
Cesarean Section and Obstetric Fistula
Indications and Prevention
Cesarean section indicated for obstructed labor, malposition, fetal distress, multiple pregnancy, previous cesarean, and other complications.
Obstetric fistula is a preventable injury caused by prolonged obstructed labor without skilled care.
Prevention requires access to emergency obstetric care.

Postpartum Hemorrhage
Causes and Management
Postpartum hemorrhage is the most common cause of maternal death worldwide.
Blood loss >600ml, often due to uterine atony or retained placental tissue.
Management: uterotonics, removal of retained tissue, manual compression, brace sutures, hysterectomy.
Care After Pregnancy
Postnatal Care
Postnatal care is crucial for screening complications, infections, postnatal depression, establishing breastfeeding, managing medical problems, and contraception.
63% of maternal deaths in the USA occur after delivery.
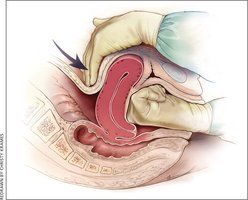
Reducing Maternal Deaths
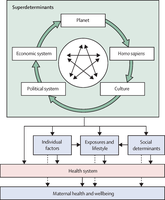
Interventions and Social Determinants
Interventions include access to care, contraception, structured antenatal care, birth spacing, skilled labor care, emergency drills, and postnatal care.
Social determinants such as gender norms, violence, child marriage, and health system failures significantly impact maternal health outcomes.
Access to Contraception
Contraception prevents pregnancy-related health risks and allows birth spacing.
77% of women aged 15-49 have their contraceptive needs met in 2024.

Summary Table: Major Maternal Complications
Complication | Maternal Impact | Fetal Impact | Prevention/Management |
|---|---|---|---|
Severe Bleeding | Shock, death | Premature birth | Uterotonics, skilled care |
Infection/Sepsis | Organ dysfunction, death | Growth restriction, death | Antibiotics, hygiene |
Pre-eclampsia | Stroke, organ failure | Growth restriction, preterm | Aspirin, monitoring, magnesium sulfate |
Obstructed Labor | Fistula, death | Birth injury, death | Cesarean section, skilled care |
Unsafe Abortion | Hemorrhage, infection, death | Fetal death | Safe abortion services, contraception |
Conclusion
Maternal health is a multifaceted issue involving medical, social, and systemic factors. Addressing complications and reducing maternal mortality requires comprehensive interventions, skilled care, and attention to social determinants of health.
