 Back
BackMusculoskeletal Assessment and Health Promotion: Study Notes for Personal Health Students
Study Guide - Smart Notes

Musculoskeletal System: Overview and Health Promotion
Introduction to the Musculoskeletal System
The musculoskeletal system provides the body with structure, support, movement, and protection. It consists of bones, muscles, joints, tendons, and ligaments, all working together to facilitate mobility and maintain posture.
Bones: Provide structural support and protect internal organs.
Muscles: Enable movement by contracting and relaxing.
Joints: Allow for flexibility and a range of movements.
Tendons and Ligaments: Connect muscles to bones and bones to each other, respectively.

Additional info: The musculoskeletal system is essential for daily activities and overall health, and its assessment is a key component of personal health evaluation.
Health History and Functional Assessment
Key Components of Musculoskeletal Health History
Obtaining a thorough health history is crucial for identifying risk factors, current issues, and functional limitations related to the musculoskeletal system.
Joints: Pain, swelling, stiffness, or decreased range of motion (ROM).
Muscles: Weakness, cramps, or atrophy.
Bones: History of fractures, deformities, or bone pain.
Functional Assessment: Ability to perform activities of daily living (ADLs) and self-care behaviors.
Age-Specific Considerations:
Infants/Children: Birth trauma, motor development, injuries, bone deformities.
Adolescents: Sports injuries, rapid growth phases.
Older Adults: Changes in ADLs, increased falls, use of mobility aids.
Chronic Diseases and Health Promotion
Common Chronic Musculoskeletal Diseases
Osteoporosis: Characterized by decreased bone density, increasing fracture risk. Affects approximately 2 million Canadians.
Arthritis: Inflammation of joints, with over 6.1 million Canadians affected. Includes osteoarthritis and rheumatoid arthritis.
Health Promotion and Illness Prevention
Workplace Injuries: Back strain is common; most Canadians experience back pain at least once.
Prevention Strategies:
Proper sitting, standing, and lifting techniques
Active lifestyle and regular exercise
Physical Examination of the Musculoskeletal System
Principles and Sequence of Examination
Musculoskeletal examination follows a systematic approach to ensure thorough assessment and comparison.
Principles:
Head-to-toe and proximal-to-distal assessment
Support joints and maintain relaxed muscles
Compare bilaterally for symmetry
Sequence:
Inspection (I): Observe for deformities, swelling, or abnormal posture.
Palpation (P): Assess skin, muscles, bony articulations, and joint capsules for tenderness or abnormalities.
Range of Motion (ROM): Evaluate active and passive movement; use a goniometer if needed.
Muscle Testing (MT): Assess muscle strength using a standardized scale.
Muscle Strength Testing
Muscle strength is graded on a scale from 0 to 5, with 5 being normal strength and 0 indicating paralysis.
Scale | % of Normal | Assessment |
|---|---|---|
5 | 100 | Full ROM against gravity and full resistance (Normal) |
4 | 75 | Full ROM against gravity and some resistance (Good) |
3 | 50 | Full ROM with gravity (Fair) |
2 | 25 | Full ROM with gravity eliminated (Poor) |
1 | 10 | Slight contraction (Trace) |
0 | 0 | No contraction (Zero) |
Assessment of Major Joints
Temporomandibular Joint (TMJ)
Assessment includes inspection, palpation, ROM, and muscle testing of the temporalis and masseter muscles.
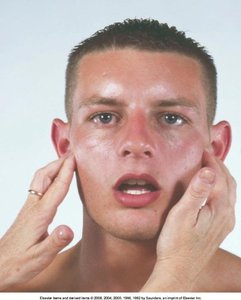

Cervical Spine
Assessment involves inspection, palpation, ROM, and muscle testing of the spinous processes, trapezius, sternomastoid, and paravertebral muscles.
Movements include flexion, extension, lateral bending, and rotation.
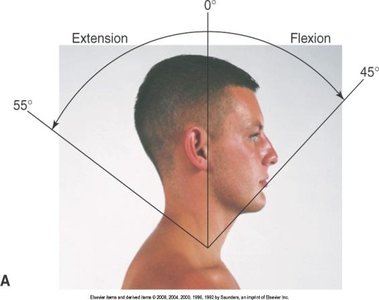
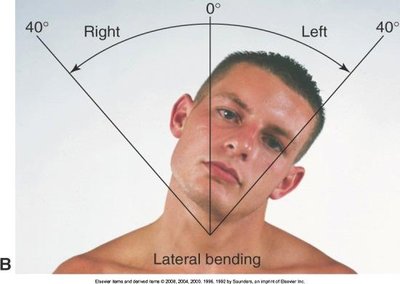
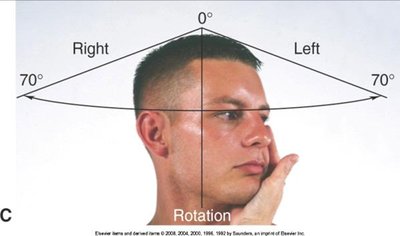
Shoulder Joint
The shoulder is a complex joint involving the clavicle, scapula, acromioclavicular joint, and glenohumeral joint. Assessment includes inspection, palpation, ROM, and muscle testing.
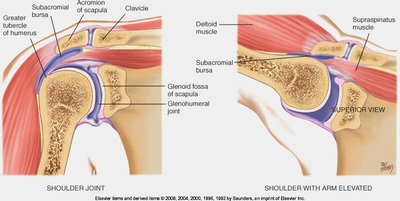
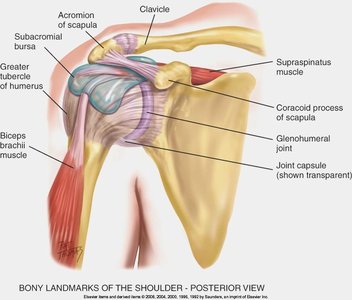
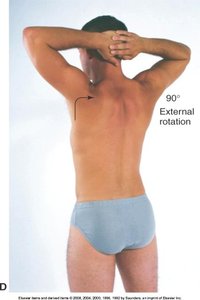
Movements: Forward flexion, hyperextension, internal/external rotation, abduction, adduction.
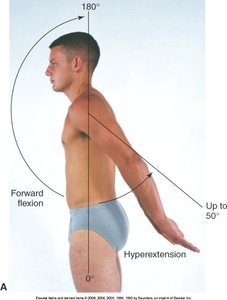
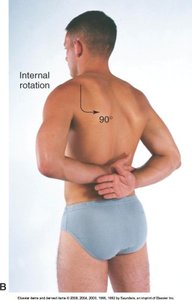

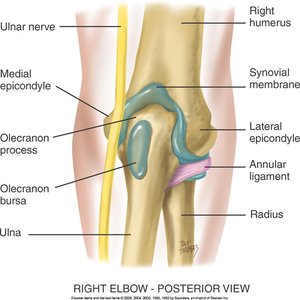
Elbow Joint
Assessment includes inspection, palpation, ROM, and muscle testing of the olecranon process and epicondyles.
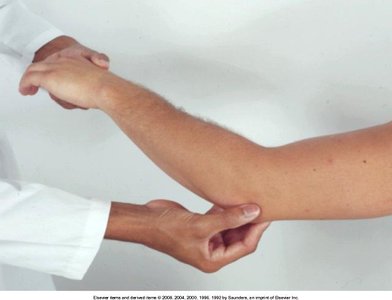
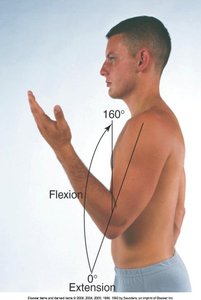
Movements: Flexion, extension, pronation, supination.
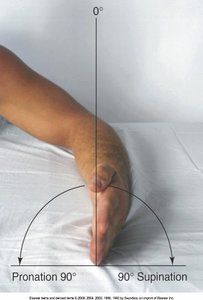

Hand and Wrist
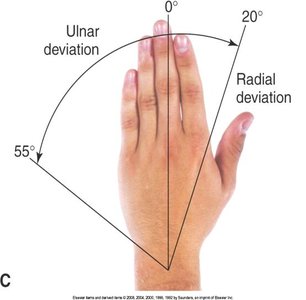
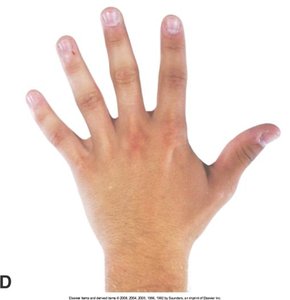
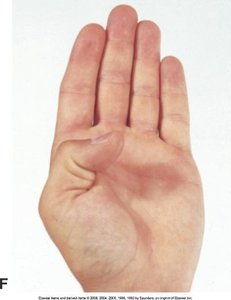
Assessment includes inspection, palpation, ROM, and muscle testing of the dorsal and palmar aspects, metacarpophalangeal joints, and interphalangeal joints.

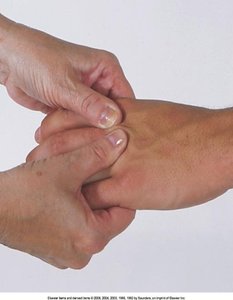

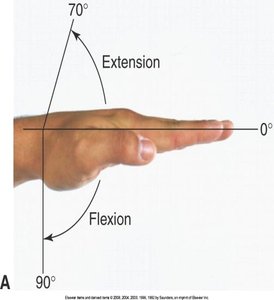
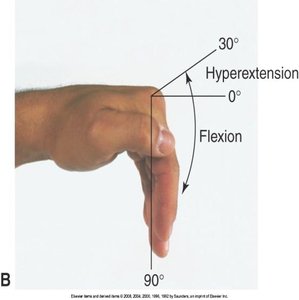
Movements: Extension, flexion, hyperextension, ulnar/radial deviation, abduction, adduction, opposition.

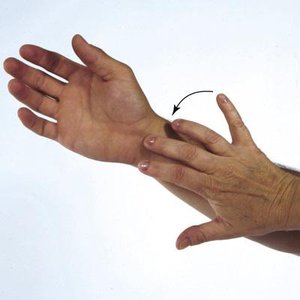
Special Tests: Carpal Tunnel Syndrome
Phalen’s test and Tinel’s sign are used to assess for carpal tunnel syndrome.

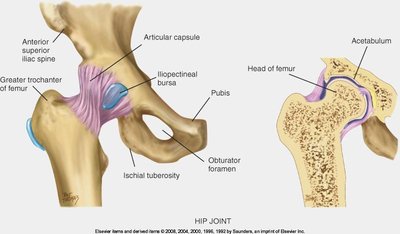
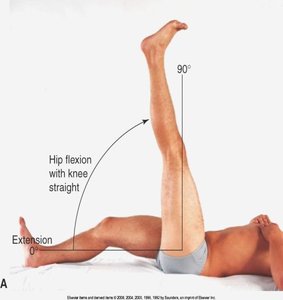
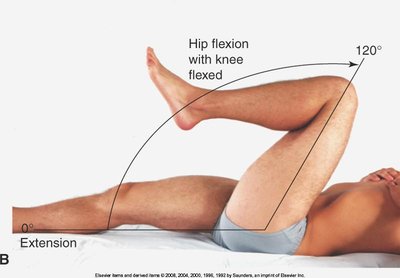
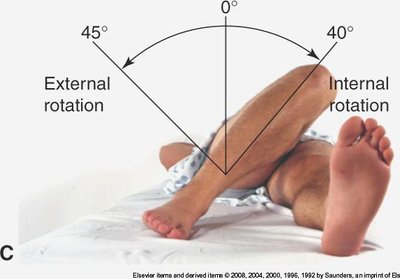
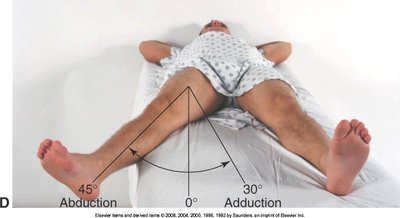
Hip Joint
Assessment includes inspection, palpation, ROM, and muscle testing of the iliofemoral joint, with attention to standing and gait.
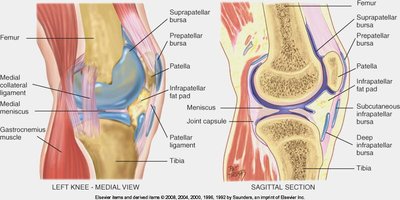
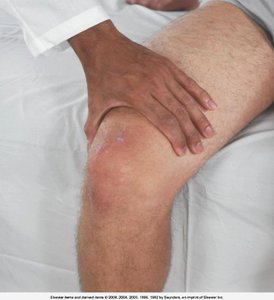
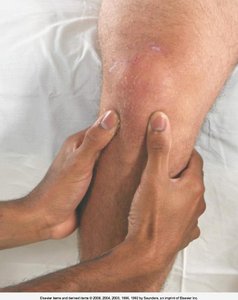
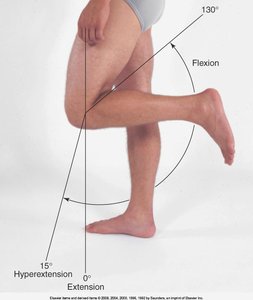
Knee Joint
Assessment includes inspection, palpation, ROM, and muscle testing of the quadriceps, suprapatellar pouch, and tibiofemoral joint.
Developmental and Cultural Considerations
Developmental Considerations
Infants: Assess for metatarsus adductus, tibial torsion, and perform Ortolani and Allis tests for hip stability.
Children: Observe for genu varum (bowlegs), genu valgum (knock-knees), and subluxation of hip and elbow.
Adolescents: Screen for kyphosis and scoliosis.
Pregnant Individuals: Assess for lordosis and kyphosis due to postural changes.
Older Adults: Note postural changes, decreased height, and functional limitations.
Transcultural Considerations
Bone density and curvature vary among populations (e.g., Black individuals have denser long bones).
Incidence of arthritis and injury patterns may differ due to social determinants of health.
Case Study: Pediatric Musculoskeletal Assessment
Clinical Scenario
A 3-year-old female presents with leg pain during a well-baby visit. Key findings include normal vital signs, clear lungs, regular heart rate, full range of motion, and normal muscle strength.
Assessment Considerations:
Ask about recent trauma, activity changes, or infections.
Use age-appropriate communication and distraction techniques during examination.
Assess for limping, swelling, redness, or tenderness.
Compare findings to developmental norms for children.
Plan of Care: Monitor symptoms, provide comfort, and educate caregivers on injury prevention and when to seek further care.
Additional info: In children, musculoskeletal pain is often due to minor trauma or overuse, but serious causes (e.g., infection, malignancy) must be ruled out if symptoms persist or worsen.
