 Back
BackN1016 Nutrition, Dental Health, and Elimination - Class 5
Study Guide - Smart Notes

NUTRITION IN OLDER ADULTS
Importance of Nutrition
Nutrition is a leading indicator of health status and is critical for maintaining health in older adults. Good nutrition is closely related to happiness, quality of life, independence, and the maintenance of both physical and social/mental functioning.
Slows the aging process and improves immunity and recovery from illness.
Protects against some chronic conditions and reduces the risk of malnutrition and nutritional deficiencies, which are major problems in older adults.

Age-Related Changes Affecting Nutrition
Several physiological changes impact the nutritional status of older adults:
Changes in taste and smell can reduce appetite and enjoyment of food.
Digestive changes may cause older adults to feel full quicker and develop food intolerances.
Oral health issues such as periodontitis, worn or brittle teeth, and xerostomia (dry mouth) can make eating, chewing, and swallowing difficult.
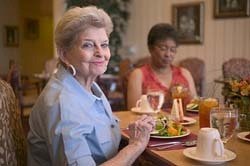
Interventions for Age-Related Changes
Strategies to address xerostomia and other oral health issues include:
Use of artificial saliva products
Ensuring adequate fluid intake (at least 2000 mL/day)
Chewing sugar-free gum and food slowly
Maintaining good dental hygiene
Nutritional Recommendations for Older Adults
While basic nutritional needs do not change significantly with age, total caloric intake should be adjusted for decreased metabolic rate and physical activity. Foods with high nutritional density are recommended.
Follow the Canada Food Guide (2019), which is less prescriptive and emphasizes variety and nutritional quality.
Recommended servings for adults 71 years and older:
Food Group | Men (71+) | Women (71+) |
|---|---|---|
Vegetables/Fruit | 7 | 7 |
Grain Products | 7 | 6 |
Milk/Alternatives | 3 | 3 |
Meat/Alternatives | 3 | 2 |



Key Nutritional Requirements
Protein: Essential for maintaining muscle mass and immune function.
Calcium and Vitamin D: Important for bone health.
Water: Body water proportion decreases with age; intake should be monitored.
Sodium: Intake should not exceed 1500 mg/day.
Alcohol: No more than one drink per day; latest research suggests no safe limit.

Practical Tips for Older Adults
Eat smaller, more frequent meals.
Prepare meals that can be divided and frozen.
Increase eggs, milk, and cheese in recipes for protein and calcium.
Avoid empty calories and monitor salt intake, especially for those with high blood pressure.
Add spices and herbs to enhance flavor.

Social and Environmental Factors Affecting Nutrition
Lifetime dietary habits
Socialization and eating with others
Income and financial resources
Transportation and access to food
Cultural beliefs



DENTAL AND ORAL HEALTH IN OLDER ADULTS
Importance of Dental Health
Oral health is a basic need and is crucial for overall health. Poor oral health can have physical and psychosocial effects, including increased risk of infections, poor nutrition, and reduced quality of life.

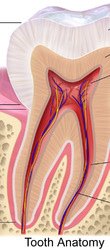
Normal Aging Changes in the Mouth
Loss of connective tissue
Decreased quality of blood vessels and nerves
Reduced size and volume of tooth pulp
Faster plaque buildup
Reduced saliva production, leading to more cavities
Exposed roots, increasing sensitivity and risk of bacterial infection
Loss of dentin and enamel

Gingivitis and Periodontal Disease
Gingivitis: Inflammation of the gums.
Periodontitis: Inflammation of the periodontium (tissues supporting the teeth); major cause of tooth loss in older adults.
Predisposing factors: Smoking, medications, teeth grinding, genetic susceptibility, estrogen deficiency (menopause).
Effects of Poor Oral Health
Bacterial infections (e.g., pneumonia, endocarditis, heart attacks, strokes)
Non-detection of oral cancer
Negative impact on nutrition
Psychosocial effects
Dental Care Recommendations
Brush with fluoride toothpaste twice daily and floss once daily.
Clean dentures and rinse mouth after eating.
Assess for swollen gums and massage gums with a warm, damp cloth.
Remove dentures at night.
See a dental health professional at least once a year.
Barriers to Dental Care
Financial costs and insurance coverage
Transportation issues
HYDRATION MANAGEMENT
Importance of Adequate Hydration
Maintaining adequate fluid intake is essential for health, promoting renal and bowel function and supporting metabolic processes. Dehydration can lead to poor health outcomes, including delirium, blood clots, infections, kidney stones, constipation, falls, medication toxicity, renal failure, seizures, electrolyte imbalance, hyperthermia, and delayed wound healing.


Risk Factors for Dehydration
Age-related decrease in water distribution and thirst sensation
Medications
Functional impairments
Illness
Screening for Dehydration
Drugs, end of life, high fever
Dark yellow urine
Dizziness (orthostatic hypotension)
Reduced oral intake, dry axillae, tachycardia
Incontinence (fear of), oral problems, neurological impairment (confusion), sunken eyes
Recommended Fluid Intake
Men: 3.7 L/day
Women: 2.7 L/day
Most older adults should aim for over 2 L/day
ELIMINATION IN OLDER ADULTS
Bowel Function
Constipation is common but not an expected age-related change; it is often a symptom of other problems such as poor habits, low fluid intake, poor diet, medication side effects, colonic dysmotility, masses, or other illnesses.
If not addressed, constipation can lead to fecal impaction, a serious condition requiring treatment.
Fecal incontinence (uncontrolled loss of fecal waste) is more prevalent in long-term care residents and is associated with diabetes, irritable bowel syndrome, spinal cord injuries, MS, and pelvic floor damage.


Bladder Function and Urinary Incontinence
Urinary incontinence is the unintentional loss of urine and is not an expected consequence of aging.
Types of urinary incontinence:
Urge: Overactive bladder, sudden need to urinate (most common type).
Stress: Loss of urine due to increased intra-abdominal pressure (e.g., coughing, sneezing, exercising).
Overflow: Loss of urine due to an overextended bladder.
Functional: Urinary tract is intact, but person cannot reach the toilet due to environmental barriers.
Iatrogenic: Caused by medical interventions or medications.
Negative health consequences include depression, social isolation, anxiety, avoidance of sexual activity, increased risk for falls, skin irritation, pressure ulcers, and urinary tract infections (UTIs).
Older adults may reduce fluid intake to control urine leakage, increasing the risk of dehydration.

Nurse’s Role in Promoting Bladder Health
Supportive measures and behavioral techniques to improve quality of life.
Provide information on bladder health:
Empty bladder before and after meals and at bedtime.
Urinate when the urge is felt.
Drink adequate fluids; cranberry juice or vitamin C may help prevent UTIs.
Reduce or eliminate coffee, tea, cola, and alcohol.
Perform pelvic floor exercises (Kegel exercises).
Take diuretics in the morning.
Maintain a healthy weight and ensure toilet accessibility.
Use protective products if necessary and practice good skin care.
