 Back
BackN1015 Population Health - Class 2
Study Guide - Smart Notes

Population Health: Concepts and Approaches
Definition and Essence of Population Health
Population health is a framework for understanding and improving the health outcomes of groups of people by addressing the broad range of factors that influence health. This approach considers the physical, social, and economic environments that shape health outcomes, as well as individual health practices, genetics, early childhood development, and access to health services.
Population Health: Focuses on the health of groups rather than individuals, aiming to improve overall health and reduce health inequities.
Determinants of Health: Includes social, economic, and physical environments, personal health practices, and access to health services.
Health Status Indicators: Used to measure the health of populations (e.g., life expectancy, disease prevalence).

Population Health vs. Public Health
While both population health and public health aim to improve health outcomes, they differ in scope and methods:
Population Health: Gathers and analyzes information about conditions affecting population health, aiming to maintain and improve health and reduce inequities.
Public Health: Uses health information to improve community health, focusing on health promotion and disease prevention through implementing recommendations from population health studies.
Population Health vs. Biomedical Approach
The population health approach contrasts with the traditional biomedical model:
Population Health: Addresses a wide range of health determinants, targets entire populations or subgroups, and emphasizes health promotion, disease prevention, and healthy public policy.
Biomedical Approach: Focuses on individual risks and clinical factors, treating individuals one at a time, with an emphasis on diagnosis and cure.
Evolution of Population Health in Canada
Key Milestones
The population health approach in Canada has evolved through several landmark reports and conferences:
1974: The Lalonde Report – Introduced the concept of health determinants beyond healthcare.
1978: Alma Ata Conference – Emphasized primary health care.
1986: Ottawa Charter for Health Promotion – Defined health promotion strategies.
1986: The Epp Report – Focused on achieving health for all.
1996: Toward a Healthy Future – First comprehensive report on the health of Canadians.

Population Health Approach to Health Promotion
Key Features
The population health approach to health promotion differs from traditional medical thinking by:
Addressing the full range of health determinants
Designing interventions for entire populations
Reducing health inequities through social and material balance
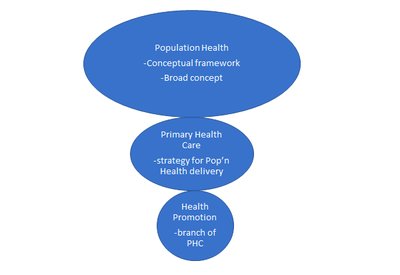
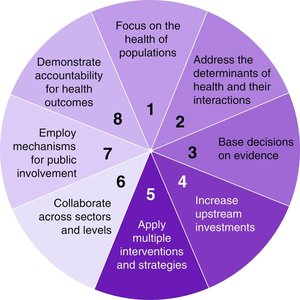
Framework and Key Elements
The population health framework focuses on improving social and economic environments, physical environments, personal health practices, individual coping skills, and health services.
Measure population health status
Analyze determinants of health
Use evidence-based decision making
Employ upstream investments
Use multiple strategies
Engage the public
Think intersectoral collaboration
Demonstrate accountability for health outcomes
Determinants of Health: Expanding the Concept
Social Determinants of Health (SDOH)
Social determinants of health are the conditions in which people are born, grow, live, work, and age. These factors are critical in shaping health outcomes and include:
Income and income distribution
Education
Unemployment and job security
Employment and working conditions
Early childhood development
Food insecurity
Housing
Social exclusion
Social safety net
Health services
Geography
Disability
Indigenous ancestry
Gender
Immigration
Race
Globalization

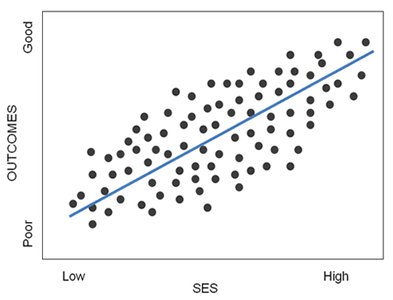
The Social Gradient in Health
The social gradient describes how health outcomes improve with higher socioeconomic status (SES). Even within wealthy nations, those with lower SES experience poorer health outcomes, highlighting the importance of addressing income inequality and social factors.
Wilkinson Hypothesis: Inequality, rather than absolute wealth, is a key determinant of health.
Health Gradient: Higher income levels are associated with better health outcomes.
Population Health in Practice: Jason's Story
A Causal Chain Example
Jason's story illustrates how social determinants impact individual health outcomes. A series of interconnected factors—such as unsafe environments, parental unemployment, and lack of education—can lead to poor health.
Environmental hazards (e.g., playing in a junkyard) can lead to injury and infection.
Underlying social issues (e.g., poverty, unemployment, lack of education) contribute to health risks.


Nursing Roles in Health Promotion
Key Roles of Nurses
Nurses play a central role in health promotion and population health by acting as advocates, care managers, consultants, direct caregivers, educators, and researchers.
Advocate: Helps clients access resources and ensures the health system meets their needs, promoting social justice.
Care Manager: Coordinates services to ensure appropriate and efficient care.
Consultant: Provides expertise in health, illness, and community dynamics.
Direct Caregiver: Delivers care in various settings, often collaborating with other professionals.
Educator: Facilitates health education and supports healthy changes in populations.
Researcher: Engages in research to advance health promotion practices.

Critiques and Future Directions
Critique of the Population Health Approach
While the population health approach is rooted in epidemiology and scientific analysis, it has been critiqued for lacking a values base, ignoring social justice, and not addressing political influences. It is often seen as a model for research rather than direct change, and may employ a top-down approach.
The "social gradient" highlights persistent inequities based on income and social status.
Calls for expanding the determinants of health to better reflect lived experiences and social realities.
Future Directions
Recent developments emphasize a whole-government approach, intersectoral collaboration, and expanding the list of determinants to address emerging social factors. Ongoing research and policy development aim to further reduce health inequities and improve population health outcomes.
