 Back
BackSocial Determinants of Health: Structured Study Notes for Personal Health Students
Study Guide - Smart Notes

Introduction to Social Determinants of Health (SDOH)
Overview of Determinants of Health
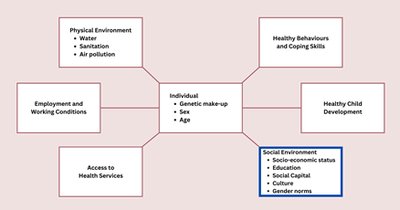
The determinants of health are a broad set of factors that influence individual and population health outcomes. These include genetic, environmental, social, and behavioral factors, which interact to shape health status.
Individual Factors: Genetic make-up, sex, age
Physical Environment: Water, sanitation, air pollution
Employment and Working Conditions: Job security, workplace safety
Access to Health Services: Availability and quality of healthcare
Healthy Behaviours and Coping Skills: Lifestyle choices, stress management
Healthy Child Development: Early life experiences
Social Environment: Socio-economic status, education, social capital, culture, gender norms
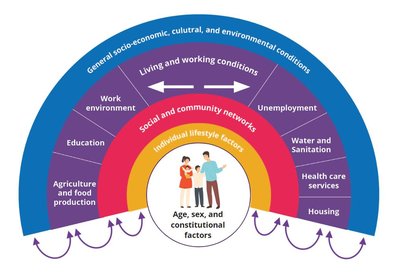
Dahlgren and Whitehead Model
This model illustrates the layers of influence on health, from individual factors to broader societal conditions. It emphasizes the interconnectedness of social, economic, and environmental determinants.
Individual lifestyle factors are surrounded by social and community networks.
Living and working conditions include work environment, education, housing, and healthcare services.
General socio-economic, cultural, and environmental conditions form the outermost layer.
Social Determinants of Health (SDOH)
Definition and Examples
SDOH are the conditions in which people are born, grow, work, live, and age, shaped by the distribution of money, power, and resources. They are critical in determining health outcomes and health inequities.
Social relationships and supports
Social norms and policies
Societal features
Political and economic systems
Lifestyle Factors vs. SDOH
Lifestyle factors are individual behaviors and choices, such as diet, physical activity, and smoking. SDOH influence these choices by shaping the environment and opportunities available to individuals.
Example: A culture where smoking is common may increase the likelihood of individuals adopting this behavior.
SDOH impact: Access to healthy food, safe environments, and education can facilitate or hinder healthy lifestyle choices.
Cultural Influences on Health
What is Culture?
Culture is a shared set of beliefs, values, and behaviors that form the identity of a group. It is transmitted across generations and influences health behaviors and perceptions.
Ethnicity: Related to culture but not identical; different ethnic groups may have distinct cultures.
Active Cognition: Cultural practices may influence individuals unconsciously.
Health Behaviours and Culture
Cultural practices affect health through nutrition, gender roles, tobacco and alcohol use, hygiene, marriage, and funeral rites.
Negative impacts: Unhealthy food preferences, settlement patterns increasing disease risk, structural violence
Positive impacts: Adaptive practices like Sardinian cattle grazing and Vietnamese stilt houses
Social Connectedness and Socioeconomic Status (SES)
Social Connectedness
Social connectedness refers to feelings of inclusion and support within relationships and communities. Strong social connections are associated with better physical and mental health outcomes.
Individuals with strong community belonging are more likely to report excellent health.
Social connectedness promotes healthier behaviors and reduces health declines.
Socioeconomic Status (SES)
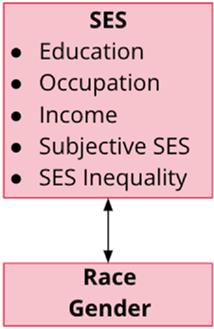
SES is an individual's or group's position within a social hierarchy, determined by education, occupation, income, and subjective perceptions. It is a major determinant of health.
Individual indicators: Education, income, occupation
Area-level indicators: Community education levels, average income
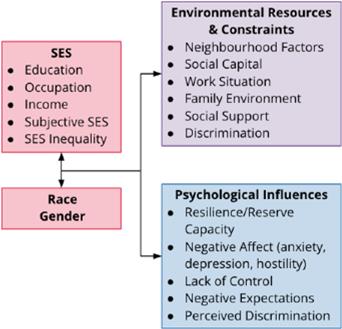
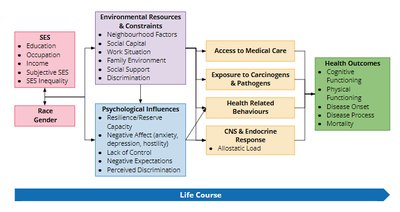
Pathways Linking SES to Health
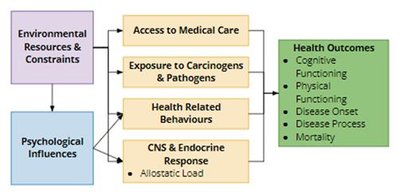
SES affects health through environmental resources and psychological influences. These pathways impact access to care, exposure to hazards, health behaviors, and stress responses.
Environmental resources: Neighborhood, social capital, work situation, family environment, social support, discrimination
Psychological influences: Resilience, negative affect, lack of control, negative expectations, perceived discrimination
Health Outcomes
Intermediate variables such as access to medical care, exposure to carcinogens, health behaviors, and stress responses (allostatic load) ultimately affect cognitive and physical functioning, disease onset, and mortality.
Allostatic load: The cumulative wear and tear on the body from chronic stress.
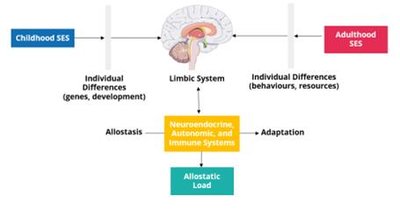
Neurobiological Pathways
Childhood and adulthood SES influence the limbic system, which regulates stress responses. Chronic exposure to low SES increases allostatic load, impairing neuroendocrine, autonomic, and immune systems.
Allostasis: Adaptation to stress
Allostatic load: Accumulated physiological burden from chronic stress
Income, Education, and Employment
Income as a Key SDOH
Income is a critical determinant of health, affecting access to resources, education, housing, and healthcare. Higher income is associated with better health outcomes and longer life expectancy.
Material deprivation indices measure hardship and resource availability.
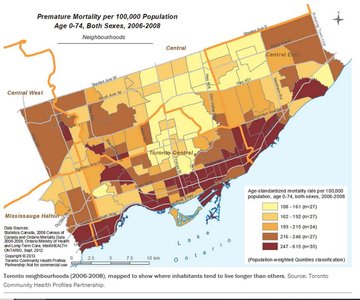
Premature Mortality by Neighbourhood
Location impacts longevity due to differences in resources, opportunities, and environmental conditions. In Toronto, premature mortality rates vary significantly by neighbourhood.
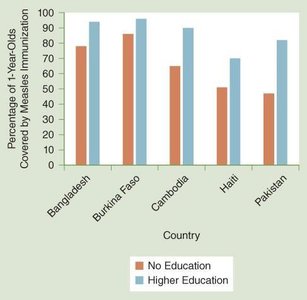
Education as a Key SDOH
Education improves health outcomes by increasing health literacy, enabling informed health decisions, and promoting healthy behaviors. Higher educational attainment is linked to better health across generations.
Health literacy is the ability to find, understand, and use health information.
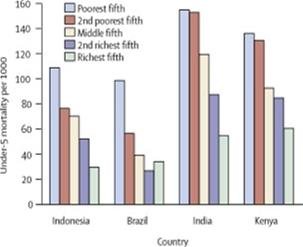
Socioeconomic Gradient in Health
Health outcomes follow a socioeconomic gradient, with poorer populations experiencing higher rates of negative health outcomes. This relationship is consistent across countries and health indicators.
Under-5 mortality rates are higher in lower income quintiles.
Health Inequities and Addressing SDOH
Language Used for Populations Facing Inequities
Populations facing health inequities are described using various terms, each with pros and cons. Language can influence perceptions and policy approaches.
Priority, marginalized, vulnerable, hard/difficult to reach, targeted, disadvantaged, under-served, disenfranchised, disempowered, underprivileged, at-risk, high-risk, equity seeking/equity deserving

Addressing SDOH
Critical actions to address SDOH include improving daily living conditions, tackling inequitable distribution of power and resources, and expanding knowledge and awareness. Policy interventions and community engagement are essential for reducing health disparities.
Living conditions: Improve circumstances in which people are born, grow, live, work, and age
Policy and resources: Address inequitable distribution through economic policies and governance
Problem solving: Expand knowledge, train workforce, raise public awareness
Summary
The social determinants of health are foundational to understanding health outcomes and disparities. By examining factors such as culture, social connectedness, SES, income, education, and employment, students can appreciate the multidimensional nature of health and the importance of addressing SDOH in personal and public health contexts.
