 Back
BackWeight Bias - Class 18
Study Guide - Smart Notes

Weight Stigma and Weight Bias in Health Care
Definitions and Core Concepts
Understanding weight stigma and weight bias is essential for promoting equitable and effective health care. These concepts influence patient experiences, health outcomes, and the overall approach to health promotion.
Weight Bias: Negative attitudes, beliefs, or stereotypes about individuals based on their weight, often resulting in unfair treatment or discrimination. (Puhl & Heuer, 2009)
Weight Stigma: The social devaluation of individuals with higher body weight, leading to exclusion, shame, and reduced opportunities. (Puhl & Brownell, 2006)
Obesity Discourses: Societal narratives that focus on weight over health, conflate thinness with health, and reinforce negative stereotypes about larger bodies.
Example: Media portrayals and health campaigns often depict obesity as a personal failing, reinforcing stigma and bias.

Obesity: Epidemiology, Risk, and Public Discourse
Trends and Public Health Framing
Obesity rates have increased dramatically over the past 25 years, leading to widespread public health concern and debate. However, the framing of obesity as an individual problem often oversimplifies complex causes and consequences.
Obesity as a Public Health Issue: Frequently described as a 'global threat' and 'ticking time bomb,' especially in relation to childhood obesity.
Science and Public Debate: Media and policy discussions often intertwine, shaping public perceptions and responses.

Mortality Risk and the Obesity Paradox
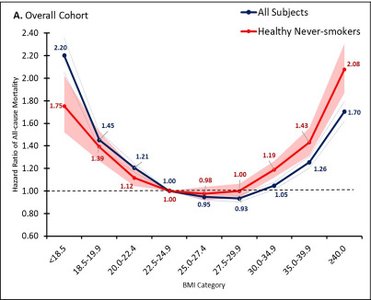
Recent research challenges the assumption that higher BMI always correlates with increased mortality risk. The relationship between BMI and health outcomes is complex and influenced by factors such as age, ethnicity, and fitness.
Relative Risk (RR) of Mortality: Underweight (BMI <18.5) and obesity class II+ (BMI >35) are associated with increased mortality risk, while overweight (BMI 25–30) is associated with decreased risk.
Obesity Paradox: In some populations, especially older adults, higher BMI may be associated with lower mortality risk.
Fitness vs. Fatness: Physical fitness may be a stronger predictor of health outcomes than BMI alone.
Example: Individuals with 'metabolically healthy obesity' may not have increased mortality risk compared to those with lower BMI.
Implications of Weight Bias in Health Care
Impact on Patients and Health Outcomes
Weight bias in health care settings can have significant negative consequences for patients, including avoidance of care, distrust of health professionals, and adoption of unhealthy behaviors.
Avoidance of Care: Patients may delay or avoid seeking medical attention due to fear of judgment or mistreatment.
Mental Health Effects: Experiences of stigma can reinforce feelings of shame, inadequacy, and low self-esteem.
Unhealthy Behaviors: Weight bias may lead to disordered eating, restrictive dieting, or other harmful practices.
Example: Case studies illustrate how weight bias can manifest in clinical interactions, affecting both physical and psychological well-being.
Dominant Myths and Societal Beliefs about Obesity
Common Misconceptions
Several pervasive myths about obesity contribute to stigma and ineffective health interventions.
Obesity is solely caused by lack of physical activity or unhealthy eating.
Obese individuals are less active and lack willpower.
Diets are effective long-term solutions.
Stigma and shame will motivate weight loss.
Weight loss is the primary measure of health improvement.
Additional info: These beliefs are not supported by evidence and can perpetuate harm.
Shifting from Weight to Wellbeing: The Body Inclusive Approach
Principles and Benefits
The Body Inclusive Approach emphasizes health and wellbeing over weight loss, recognizing the influence of social determinants of health and the importance of supportive environments.
Focus on Health Behaviors: Encourages physical activity, balanced nutrition, and mental health rather than weight as the primary outcome.
Supportive Health Promotion: Creates safe spaces and positive messaging for all body types.
Addressing Weight Bias: Involves education and training for health professionals to reduce stigma and improve patient care.
Example: Local initiatives and toolkits support health professionals in adopting a body inclusive approach.
The REFLECT Tool for Patient-Centered Care
Strategies for Reducing Weight Bias
The REFLECT tool provides practical strategies for health professionals to engage respectfully and effectively with patients of all body sizes.
R: Respectful conversations about weight
E: Emphasize health-promoting behaviors
F: Food as more than fuel
L: Listen to patient context
E: Exercise as more than calorie burning
C: Collaborate with families and communities
T: Thoughts, beliefs, and experiences matter
Additional info: This approach aligns with patient-centered care and supports holistic health outcomes.
Case Studies: Recognizing and Addressing Weight Bias
Clinical Scenarios and Analysis
Case studies highlight real-world examples of weight bias in health care and offer opportunities to reflect on alternative, supportive strategies.
Case 1 (Casey): A child experiences embarrassment and stigma during a routine medical visit, with health professionals focusing on weight rather than the presenting health concern.
Case 2 (Maria): An adult woman with a history of eating disorder faces judgment and denial of reproductive care based solely on her weight, despite a history of recovery and healthy behaviors.
Supportive Actions: Respectful communication, focus on health behaviors, and consideration of patient history and context.
Implications: Weight bias can lead to emotional distress, avoidance of care, and worsened health outcomes.
Addressing Bias: Health professionals should use the REFLECT tool, prioritize patient dignity, and adopt a body inclusive approach.
Summary Table: Weight Bias vs. Body Inclusive Approach
Aspect | Weight Bias Approach | Body Inclusive Approach |
|---|---|---|
Focus | Weight loss, BMI | Health behaviors, wellbeing |
Patient Experience | Stigma, shame, avoidance | Respect, support, engagement |
Health Outcomes | Potential harm, disordered eating | Improved mental and physical health |
Professional Role | Judgment, prescriptive | Collaborative, patient-centered |
Key Takeaways
Weight stigma and bias are pervasive in health care and society, with significant negative consequences for individuals and public health.
Shifting from a weight-focused to a wellbeing-focused approach improves patient outcomes and supports holistic health.
The REFLECT tool and body inclusive practices are essential for reducing bias and promoting equitable care.
