 Back
BackPsychological Disorders: History, Diagnosis, and the Justice System
Study Guide - Smart Notes

Psychological Disorders
Introduction to Psychological Disorders
Psychological disorders, also known as mental disorders, are patterns of behavior or experience that cause distress, impair day-to-day functioning, or increase the risk of harm. The understanding and treatment of mental illness have evolved significantly over time, influenced by cultural, social, and scientific developments.
Historical Conceptions of Mental Illness
Demonic Model and Superstition
During the Middle Ages, mental illnesses were often attributed to supernatural causes, such as demonic possession. Treatments included exorcisms and witch hunts, reflecting a lack of scientific understanding.

The Medical Model and Asylums
With the Renaissance, the medical model emerged, viewing mental illness as a physical disorder requiring treatment. People were housed in asylums, which were often overcrowded and understaffed. Common treatments included bloodletting and the use of 'snake pits.'

Moral Treatment Reform
Reformers like Phillippe Pinel and Dorothea Dix advocated for moral treatment in the 18th and 19th centuries, emphasizing dignity, kindness, and respect for patients. Although this improved conditions, effective treatments were still lacking.

The Modern Era and Deinstitutionalization
The development of antipsychotic medications such as chlorpromazine (Thorazine) in the 1950s led to the deinstitutionalization movement in the 1960s and 70s. Many patients were released from hospitals, but community support systems were often inadequate.

Defining and Diagnosing Mental Illness
Criteria for Mental Disorders
The DSM-5 defines mental disorders as patterns of behavior or experience that cause distress, impair functioning, or increase risk of harm. However, not all maladaptive behaviors are mental illnesses, and some individuals may not meet all criteria but still experience significant distress.
Biopsychosocial Model
The biopsychosocial model considers biological, psychological, and social factors in the development and maintenance of mental disorders:
Biological factors: Brain chemistry, genetics, neurodevelopment, physical health
Psychological factors: Cognitive patterns, emotional regulation, personality, coping skills
Social factors: Environment, culture, family dynamics, socioeconomic status
DSM and Classification
The DSM (Diagnostic and Statistical Manual of Mental Disorders) provides standardized criteria for diagnosing mental disorders. The number of recognized disorders has increased over time, reflecting advances in research and changes in societal attitudes.
Culture and Mental Disorders
Culture-Bound Syndromes
Certain mental disorders are specific to particular cultures, while others (e.g., schizophrenia, alcoholism) are universal. Culture influences how symptoms are expressed and understood.
Malocchio (Italy): Headaches, fatigue, and anxiety attributed to envy or the 'evil eye.'
Calor do corpo/nervos (Portugal/Brazil): Fatigue and anxiety explained by bodily imbalance or 'nerves.'
Taijin Kyofusho (Japan): Social anxiety focused on the fear of offending others, reflecting collectivist values.


Major Categories of Psychological Disorders
Anxiety Disorders
Anxiety disorders are characterized by excessive and persistent anxiety or maladaptive behaviors that reduce anxiety. Common types include:
Generalized Anxiety Disorder (GAD): Chronic worry, tension, and irritability about various topics.
Panic Disorder: Recurrent, unexpected panic attacks and fear of future attacks.
Phobias: Unrealistic fear of specific situations or objects (e.g., agoraphobia).
Obsessive-Compulsive Disorder (OCD): Intrusive thoughts (obsessions) and ritualistic behaviors (compulsions).
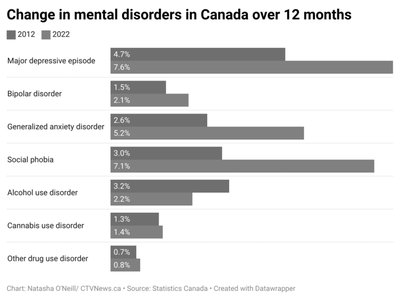
Mood Disorders
Mood disorders include major depression and bipolar disorder, both of which significantly affect emotional state and functioning.
Major Depression: Persistent sadness, hopelessness, social withdrawal, and physical symptoms such as sleep and appetite changes.
Bipolar Disorder: Alternating periods of depression and mania (elevated mood, energy, impulsivity).

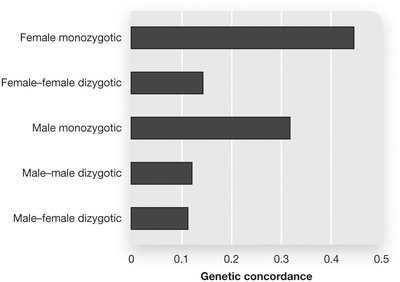
Genetic and Environmental Factors in Depression
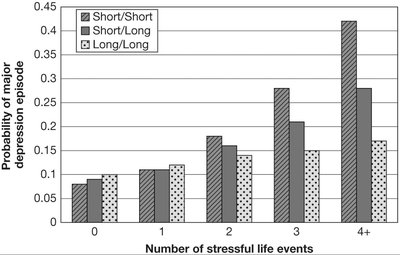
Depression risk is influenced by genetic predisposition, stressful life events, and sociocultural factors such as poverty and social support.
Diathesis-Stress Model: Interaction between genetic vulnerability and environmental stressors.
Explanatory Style: Tendency to attribute negative events to internal, stable, and global causes increases depression risk.
Schizophrenia
Schizophrenia is a severe disorder involving breaks from reality, disorganized thinking, and emotional disturbances. Symptoms are classified as:
Positive symptoms: Hallucinations, delusions, disorganized thought and movement
Negative symptoms: Social withdrawal, lack of emotional expression
Biological factors include brain structure abnormalities (e.g., enlarged ventricles), neurotransmitter imbalances (dopamine, glutamate), and reduced frontal lobe activity. Environmental factors such as stress, low socioeconomic status, and cannabis use also contribute.

Personality Disorders
Personality disorders are enduring patterns of behavior that are maladaptive and resistant to change. They are grouped into three clusters:
Cluster A: Odd or eccentric (e.g., paranoid, schizoid)
Cluster B: Dramatic, emotional, or erratic (e.g., borderline, antisocial, narcissistic)
Cluster C: Anxious or fearful (e.g., avoidant)
Borderline Personality Disorder is marked by emotional instability, impulsivity, and unstable relationships. Antisocial Personality Disorder involves a lack of empathy, disregard for others' rights, and often criminal behavior. Psychopathy is a severe form of antisocial personality with additional traits such as superficial charm and lack of remorse.
Mental Illness and the Justice System
Intersection of Mental Health and Law
Mental illness can affect legal responsibility and outcomes in the justice system. The insanity defense (NCRMD: Not Criminally Responsible by Reason of Mental Disorder) is a legal, not psychological, concept. It requires that the individual was unable to appreciate the nature or wrongfulness of their actions due to mental disorder at the time of the offense.

Outcomes of NCRMD
Possible outcomes after an NCRMD finding include absolute discharge, conditional discharge, or detention in a psychiatric hospital. Decisions are based on risk to public safety and treatment needs, not criminal guilt.
Myths and Realities of NCRMD
Myth: NCRMD is frequently used and successful.
Reality: Used in only 1% of felony cases and rarely successful.
Myth: NCRMD allows dangerous individuals to go free.
Reality: Most are detained longer than if found guilty.
Mental Illness in Correctional Settings
Mental illness is highly prevalent in correctional facilities, with rates much higher than in the general population. Prisons often lack adequate mental health services, and harsh conditions such as solitary confinement can worsen symptoms and lead to severe psychological harm.
Conclusion
The understanding and treatment of psychological disorders have evolved from superstition and confinement to scientific diagnosis and biopsychosocial approaches. However, challenges remain, especially at the intersection of mental health and the justice system, where stigma, inadequate resources, and legal complexities persist.
