 Back
BackPsychological Disorders: History, Diagnosis, and the Justice System
Study Guide - Smart Notes

Topic 13: Psychological Disorders
Introduction to Psychological Disorders
Psychological disorders are patterns of behavior or experience that cause distress, impair day-to-day functioning, or increase the risk of harm. The definition and understanding of mental illness have evolved significantly over time, influenced by cultural, social, and scientific developments.
Historical Conceptions of Mental Illness
Demonic Model (Middle Ages): Mental illnesses were often attributed to evil spirits or demonic possession. Treatments included exorcisms and witch hunts.
Medical Model (Renaissance): Emergence of the view that mental illness is a physical disorder requiring treatment. Patients were housed in asylums, but these were often overcrowded and used ineffective treatments such as bloodletting and "snake pits."
Moral Treatment (1700s-1800s): Reformers like Phillippe Pinel and Dorothea Dix advocated for treating patients with dignity and kindness, allowing them more freedom and interaction, though effective treatments were still lacking.



The Modern Era of Mental Health Care
Pharmacological Advances: The development of chlorpromazine (Thorazine) in the 1950s marked the beginning of effective antipsychotic treatment, reducing symptoms of schizophrenia and related disorders.
Deinstitutionalization: In the 1960s and 70s, many psychiatric hospitals were closed, and patients were released into the community. This shift had mixed results due to insufficient community support and services.

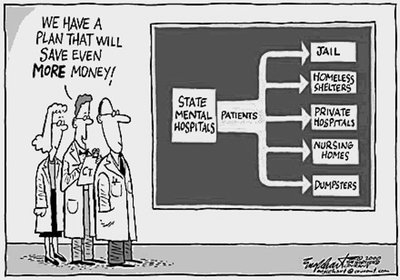
Defining Mental Illness
The DSM-5 (Diagnostic and Statistical Manual of Mental Disorders) provides official diagnostic criteria and decision rules for mental disorders. It uses a biopsychosocial approach, considering biological, psychological, and social factors, as well as prevalence and functioning.
Maladaptive Behavior: Not all maladaptive behaviors are mental illnesses, and not all mental illnesses fit neatly into the criteria of distress or impairment.
Explosion of Diagnoses: The number of recognized mental disorders has increased dramatically with each DSM revision, raising debates about over-diagnosis and the influence of insurance requirements.
Diagnosis Across Cultures
Cultural context shapes the expression and recognition of mental disorders. Some conditions are culture-bound, while others (e.g., schizophrenia, alcoholism) are universal. Examples include:
Malocchio (Italy): Headaches, fatigue, and anxiety attributed to the "evil eye."
Calor do corpo/nervos (Portugal/Brazil): Psychological distress expressed as physical symptoms due to bodily imbalance or "nerves."
Taijin Kyofusho (Japan): A form of social anxiety focused on the fear of offending or embarrassing others, reflecting collectivist cultural values.


Major Categories of Psychological Disorders
Anxiety-Related Disorders
Anxiety disorders are characterized by excessive, persistent anxiety and maladaptive behaviors aimed at reducing anxiety. While some anxiety is adaptive, it can become pathological when disproportionate or chronic.
Generalized Anxiety Disorder (GAD): Chronic worry, tension, and irritability about various aspects of life. More common in females and Caucasians.
Panic Disorder: Recurrent, unexpected panic attacks and persistent concern about future attacks.
Phobias: Unrealistic fear of specific situations, activities, or objects. Agoraphobia is the fear of being away from a safe place or person.
Obsessive-Compulsive Disorder (OCD): Intrusive, unwanted thoughts (obsessions) and repetitive behaviors (compulsions) performed to reduce distress.
OCD-Related Disorders: Hoarding disorder, excoriation disorder (skin picking), trichotillomania (hair pulling), and body dysmorphic disorder.
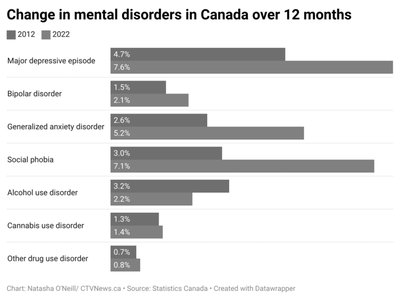
Mood Disorders
Mood disorders involve disturbances in emotional state, including depression and bipolar disorder. These conditions are common and have significant genetic, psychological, and sociocultural risk factors.
Major Depression: Persistent sadness, hopelessness, social withdrawal, cognitive and physical sluggishness, and changes in sleep and appetite.
Bipolar Disorder: Alternating periods of depression and mania (elevated mood, energy, impulsivity). Difficult to treat and associated with high suicide risk.

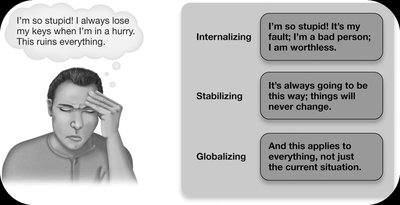
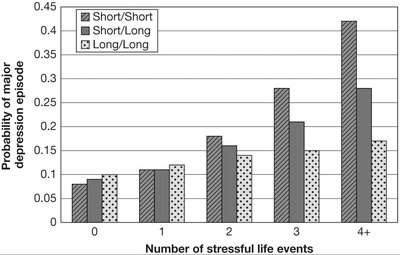
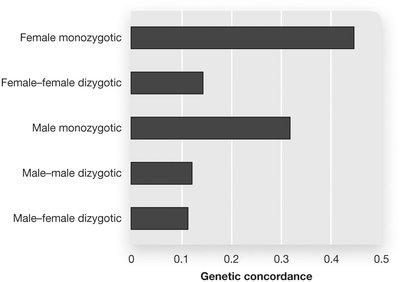
Schizophrenia
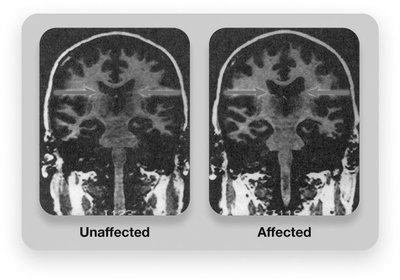
Schizophrenia is a severe disorder involving breaks from reality, disorganized thinking, and emotional disturbances. Symptoms are classified as positive (hallucinations, delusions), negative (social withdrawal, lack of emotion), and cognitive (disorganized thinking).
Brain Structure: Larger ventricles, loss of brain tissue, and differences in the hippocampus and amygdala.
Brain Activity: Reduced activity in the frontal lobes and emotion/memory regions.
Neurotransmitters: Dopamine overactivity (positive symptoms), glutamate underactivity.
Environmental Factors: Extreme stress, low socioeconomic status, minority status, prenatal environment, and cannabis use.

Personality Disorders
Personality disorders are enduring patterns of behavior that are maladaptive, distressing, and resistant to change. They are grouped into three clusters:
Cluster A: Odd or eccentric behavior (e.g., paranoid, schizoid).
Cluster B: Dramatic, emotional, or erratic behavior (e.g., antisocial, borderline, narcissistic).
Cluster C: Anxious, fearful, or inhibited behavior (e.g., avoidant).
Borderline Personality Disorder: Marked by intense emotional swings, unstable relationships, impulsivity, and maladaptive coping strategies, often rooted in early trauma.
Antisocial Personality Disorder (APD): Characterized by lack of empathy, disregard for others' rights, and impulsive or violent behavior. Linked to frontal lobe dysfunction and early conduct disorder.
Psychopathy: Extreme form of APD with interpersonal/emotional deficits (e.g., lack of remorse) and social deviance (e.g., impulsivity). Associated with amygdala and frontal lobe abnormalities.
Uncommon Psychiatric Syndromes
Capgras’s Syndrome: Belief that a loved one has been replaced by an impostor.
Ekbom’s Syndrome: Delusions of infestation.
Munchausen Syndrome: Fabrication of medical symptoms for attention or care.
Mental Illness and the Justice System
Intersection of Mental Health and Law
Mental illness can influence legal outcomes, particularly regarding criminal responsibility. The insanity defense (NCRMD: Not Criminally Responsible by Reason of Mental Disorder) is a legal, not psychological, concept. It requires that the individual was incapable of appreciating the nature or wrongfulness of their actions due to mental disorder at the time of the offense.
Actus Reus: The guilty action.
Mens Rea: The guilty mind (intent).
Possible outcomes after an NCRMD finding include absolute discharge, conditional discharge, or detention in a hospital, depending on risk to public safety and treatment needs. Myths about NCRMD include its frequency, effectiveness as a loophole, and the danger posed by mentally ill individuals.

Mental Health in the Correctional System
High prevalence of mental illness among incarcerated individuals (up to 70% in federal prisons).
Prisons are often ill-equipped to provide adequate mental health care.
Segregation and solitary confinement are common, with profound psychological and neurological effects, including hallucinations, cognitive disabilities, and increased suicide risk.
Disproportionate impact on marginalized groups, including Black and Indigenous populations.
Advocacy and Support
Organizations such as the John Howard Society, Fred Victor, Elizabeth Fry Society, Addictions and Mental Health Ontario (AMHO), CMHA, and CAMH work to support individuals with mental illness and advocate for systemic change.
