 Back
BackTherapies in Psychology: Historical and Modern Approaches
Study Guide - Smart Notes

Therapies in Psychology
Historical Approaches to Mental Health Treatment
The treatment of mental illness has evolved significantly over the centuries, reflecting changes in societal attitudes, scientific understanding, and available resources.
1400s: The first institutions for the mentally ill were established, often characterized by harsh and inhumane conditions.
Late 1800s: Overcrowded asylums became common, with ineffective and sometimes harmful treatments such as cold water submersion and early forms of electroshock therapy.
1960s: The discovery of antipsychotic medications led to deinstitutionalization, shifting care from asylums to community-based settings and residential treatment centers.


Example: Deinstitutionalization resulted in many individuals with mental illness living in the community, but also contributed to increased rates of homelessness and justice involvement among this population.
Mental Health and Homelessness
Mental health challenges are prevalent among homeless populations, with youth and Indigenous individuals experiencing particularly high rates of mental health and substance use issues.
85% of homeless individuals report at least one health challenge.
Youth (ages 13-24) have the highest prevalence of mental health issues (67%).
Indigenous respondents report higher rates of substance use compared to non-Indigenous peers.
Former youth in care are at increased risk for mental health and substance use problems.
The Courts and Mental Health
The legal system sometimes intersects with mental health care, particularly for individuals whose behavior is highly erratic or disturbing.
Community Treatment Orders: Individuals may be required to live in the community under legally mandated treatment conditions (e.g., medication adherence, psychiatric appointments).
Controversy: Such measures raise ethical questions about individual rights versus public safety and resource allocation.

Modern Mental Health Treatment Settings
Today, mental health care is provided in a variety of settings, with an emphasis on short-term hospitalization and community-based care.
Psychiatric Hospitals: Focus on acute, short-term care for individuals who are an imminent threat to themselves or others.
Involuntary Admission: May occur if there is a risk of serious harm or inability to care for oneself; legal rights and review processes are in place.
Community Services: Include crisis support, therapy, and case management, often provided by organizations such as CMHA and CAMH.

Types of Mental Health Professionals
There are several types of professionals who provide psychological treatment, each with distinct qualifications and roles:
Clinical Psychologists: Hold a PhD or PsyD and specialize in assessment and treatment of psychological disorders.
Counseling Psychologists: Typically address day-to-day adjustment problems.
Psychiatrists: Medical doctors who can prescribe medication and treat severe disorders.
Psychoanalysts: Specialize in psychoanalysis, following Freudian techniques.
Registered Psychotherapists: Provide therapy for a range of issues, with varying educational backgrounds.
Social Workers and Counselors: Offer therapy and support, often for common family and personal problems.
Barriers to Psychological Treatment
Many factors can prevent individuals from seeking or receiving effective mental health care:
Ambiguity of disorders
Stigma and cultural attitudes
Gender roles and expectations
Geographical and financial barriers
Cultural and Gender Barriers
Cultural background and gender norms significantly influence attitudes toward mental health treatment.
Asian Canadians and Indigenous people are less likely to seek therapy compared to Canadians of European descent.
Therapy is more accepted in individualistic cultures than in collectivist ones.
Masculinity norms, symptom recognition, attitudinal barriers, stigma, and service fit all contribute to lower rates of help-seeking among men.




Major Types of Psychological Therapies
Insight Therapies
Insight therapies involve dialogue between client and therapist to increase awareness and understanding of psychological problems and conflicts.
Psychodynamic Therapies: Focus on uncovering unconscious conflicts, often rooted in childhood experiences.
Psychoanalysis: Developed by Freud, uses techniques such as free association and dream analysis to access unconscious material.
Resistance: Client's reluctance to discuss certain topics, which the therapist interprets.
Transference: Client projects feelings about important figures onto the therapist.


Person-Centered Therapy
This humanistic approach, developed by Carl Rogers, emphasizes the importance of the therapeutic relationship, empathy, and unconditional positive regard.
Non-directive, focusing on the client's self-actualization and subjective experience.
Therapeutic alliance is a strong predictor of successful outcomes.

Behavioral Approaches
Behavioral therapies apply principles of learning to modify undesirable behaviors.
Classical Conditioning Techniques: Include aversive conditioning, systematic desensitization, and flooding.
Operant Conditioning Techniques: Use reinforcement and punishment to shape behavior (e.g., token economies, contingency contracts).
Observational Learning: Modeling appropriate behaviors to teach new skills.






Cognitive-Behavioral Therapies (CBT)
CBT combines cognitive and behavioral techniques to address faulty thinking patterns and maladaptive behaviors.
Cognitive Restructuring: Identifying and challenging negative beliefs.
Exposure: Gradual confrontation of feared situations.
Relaxation Training: Techniques to manage emotional responses.
Homework and Practice: Clients actively work on skills outside of sessions.


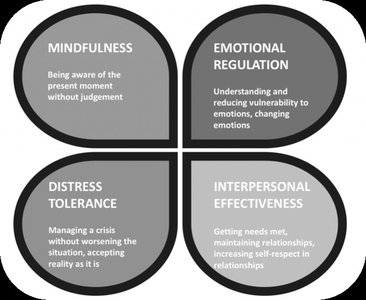
Dialectical Behavioral Therapy (DBT)
DBT is a form of CBT that emphasizes acceptance and change, teaching skills in distress tolerance, mindfulness, emotional regulation, and interpersonal effectiveness. It is especially effective for some personality disorders.
Interoceptive Exposure Therapy
This therapy is used for panic disorder, helping clients become accustomed to physical sensations associated with panic attacks, reducing their fear response.

Mindfulness-Based Cognitive Therapy (MBCT)
MBCT integrates mindfulness meditation with cognitive-behavioral strategies, helping clients "decenter" from their thoughts and observe them more objectively.
Group and Family Therapies
Group therapy provides support and advice among peers, while family therapy aims to improve family dynamics and communication. Self-help groups like Alcoholics Anonymous are also common.


Effectiveness of Therapy
Research shows that psychotherapy is effective for most people, though not universally so. Different therapies are suited to different problems, and therapists often use an eclectic approach.
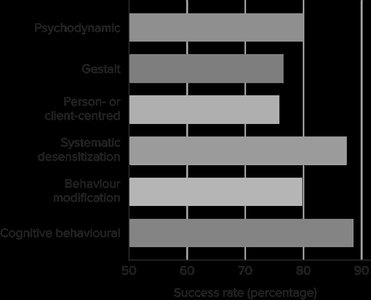
Therapy Type | Success Rate (%) |
|---|---|
Psychodynamic | ~75 |
Gestalt | ~70 |
Person- or client-centred | ~75 |
Systematic desensitization | ~85 |
Behaviour modification | ~80 |
Cognitive behavioural | ~85 |
Biomedical Therapies
Pharmacological Treatments
Medications are commonly used to manage symptoms of mental disorders, though they are not always curative and may have side effects.
Antipsychotic Drugs: Block dopamine receptors to reduce psychotic symptoms; newer drugs may increase dopamine in specific brain regions.
Antianxiety Drugs: Benzodiazepines (e.g., Xanax, Valium, Ativan) enhance GABA activity but carry risks of dependence and interaction with alcohol.
Antidepressants: Include tricyclics, MAO inhibitors, and SSRIs (e.g., Prozac, Zoloft), which affect neurotransmitter levels to improve mood.
Herbal Remedies: St. John’s Wort may reduce depression but lacks standardization and can interact with other medications.
New Directions in Psychopharmacology
Ketamine Therapy: Blocks NMDA receptors, affecting glutamate; promising for treatment-resistant depression but with potential side effects and addiction risk.
Brain Stimulation and Psychosurgery
Transcranial Magnetic Stimulation (TMS): Uses magnetic pulses to stimulate brain regions, effective for depression but may cause seizures.
Electroconvulsive Therapy (ECT): Involves brief electrical stimulation under sedation, used for severe depression; controversial due to side effects like memory loss.
Psychosurgery: Rarely used today, but historically included lobotomies and lesions; now a last resort for severe, treatment-resistant cases.
Other Therapies
Eye Movement Desensitization and Reprocessing (EMDR): Involves recalling traumatic events while performing guided eye movements; controversial due to limited evidence.
Critical Perspectives
While biomedical therapies have revolutionized mental health care, they are not a cure-all and may only provide temporary symptom relief. Addressing underlying psychological and social factors remains essential.
Case Study: On Being Sane in Insane Places (Rosenhan, 1970s)
This classic study highlighted the challenges of psychiatric diagnosis and the depersonalization experienced by patients in mental hospitals. Eight "sane" individuals were admitted to hospitals after feigning auditory hallucinations and were subsequently diagnosed with schizophrenia, receiving little meaningful interaction or treatment.
