 Back
BackTherapies in Psychology: Historical and Modern Approaches
Study Guide - Smart Notes

Therapies in Psychology
Historical Approaches to Mental Health Treatment
The treatment of mental illness has evolved significantly over the centuries, moving from inhumane institutionalization to more effective and ethical interventions.
1400s: The first institutions for the mentally ill were established, often with brutal conditions.
Late 1800s: Overcrowded asylums and ineffective treatments such as cold water submersion and early forms of electroshock therapy were common.
1960s: The discovery of antipsychotic medication led to deinstitutionalization and the rise of residential treatment centers.


Example: Deinstitutionalization resulted in many mentally ill individuals becoming homeless or involved with the justice system.
Mental Health and Homelessness in Canada
Mental health challenges are prevalent among homeless populations, with youth and Indigenous individuals being particularly affected.
85% of homeless individuals report at least one health challenge.
Youth (13-24) have the highest prevalence of mental health issues (67%).
Indigenous respondents have higher rates of substance use (69%) compared to non-Indigenous (57%).
Former youth in care have significantly higher rates of mental health and substance use issues (59% vs. 41%).
Additional info: Deinstitutionalization has contributed to the intersection of mental health issues with homelessness and the criminal justice system.
The Courts and Mental Health
The legal system sometimes mandates mental health treatment for individuals whose behavior is highly erratic or disturbing.
Community Treatment Orders: Individuals may be required to live in the community under legally mandated treatment conditions (e.g., medication, psychiatric appointments).
This is a controversial issue, balancing public safety and individual rights.

Modern Mental Health Treatment Settings
Today, mental health treatment is provided in a variety of settings, with a focus on short-term care and community integration.
Psychiatric hospitals and local community hospitals focus on short-term care, usually for individuals who are an imminent threat to themselves or others.
Involuntary admission (Form 1) is used when there is a risk of serious harm or inability to care for oneself. Legal rights include access to representation and review boards.

Sources of Psychological Treatment
Mental health care can be accessed through various professionals and organizations:
Family doctors & primary care clinics: Initial assessments, medication, referrals.
Psychiatrists: Medical doctors who can prescribe medication (covered by public health insurance).
Private psychologists & therapists: Provide therapy and assessments but cannot prescribe medication.
Community mental health services: Offer low-cost support, therapy, crisis intervention, and case management.
Crisis & emergency services: Immediate support for acute mental health crises.
Types of Therapists
Different mental health professionals have varying qualifications and roles:
Clinical Psychologists: PhD or PsyD, specialize in assessment and treatment of psychological difficulties.
Counselling Psychologists: PhD, EdD, or master's degree, focus on day-to-day adjustment problems.
Psychiatrists: MDs with postgraduate training, can prescribe medication.
Psychoanalysts: Specialize in psychoanalysis, often with medical or psychology backgrounds.
Registered Psychotherapists: Varying educational backgrounds, provide talk therapy.
Licensed Professional Counsellors/Clinical Mental Health Counsellors: Master's degree, certified to provide therapy.
Clinical or Psychiatric Social Workers: Master's degree, provide therapy for family and personal problems.
Barriers to Psychological Treatment
Several factors can prevent individuals from seeking or receiving effective mental health care:
Ambiguity of disorders
Stigma about mental illness
Attitudes toward treatment
Gender roles and cultural expectations
Geographical and financial barriers
Cultural Barriers to Therapy
Cultural background influences attitudes toward mental health treatment.
Asian Canadians and Indigenous people are less likely to seek treatment than Canadians of European background.
Therapy is more accepted in individualistic cultures (e.g., Canada, USA) than in collectivist cultures.
Men and Mental Health
Men face unique barriers to seeking mental health treatment, including masculinity norms, symptom recognition, attitudinal barriers, stigma, and service fit.
Masculinity Norms: Emotional disclosure seen as weakness.
Symptom Recognition: Depression may manifest as anger or substance use.
Attitudinal Barriers: Preference for self-reliance, discomfort with vulnerability.
Stigma: Fear of judgment from peers and family.
Service Fit: Services may not be tailored to men's communication styles.
Insight Therapies
Insight therapies involve dialogue between client and therapist to gain awareness and understanding of psychological problems and conflicts.
Psychodynamic Therapies: Emphasize discovering and resolving unconscious conflict.
Psychoanalysis
Developed by Freud, psychoanalysis aims to release unconscious thoughts and feelings to reduce their influence on behavior.
Techniques: Free association, dream analysis.
Resistance: Inability or unwillingness to discuss certain topics.
Transference: Transferring feelings onto the therapist.

Psychodynamic Therapy Today
Modern psychodynamic therapy is shorter in duration and may focus on early childhood experiences and emotional attachments (object relations therapy). Evidence is mixed regarding its effectiveness.
Person-Centered Therapy
This humanistic approach emphasizes the importance of the therapeutic relationship, self-actualization, and empathy.
Core Conditions: Congruence, unconditional positive regard, empathy.

Behavioral Approaches
Behavioral therapies apply principles of learning to change undesirable behaviors.
Aversive Conditioning: Pairing an unpleasant stimulus with an unwanted behavior.
Systematic Desensitization: Gradual exposure to anxiety-provoking stimuli paired with relaxation techniques.
Flooding: Rapid and intense exposure to the feared stimulus.
Operant Conditioning Techniques: Rewarding desirable behaviors, using token systems, contingency contracting, and observational learning.




Cognitive-Behavioral Therapies (CBT)
CBT, developed by Aaron Beck, assumes that negative emotions stem from faulty thinking. It helps clients find more logical, positive ways to interpret situations.
Cognitive Restructuring: Rethinking negative beliefs.
Exposure: Facing avoided situations.
Relaxation: Regaining emotional control.

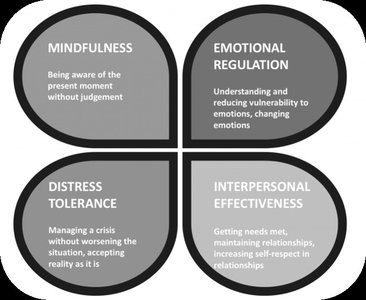
Dialectical Behavioral Therapy (DBT)
DBT focuses on acceptance and change, teaching behavioral skills for emotional regulation, distress tolerance, mindfulness, and interpersonal effectiveness. It is especially effective for some personality disorders.

Interoceptive Exposure Therapy
Used for panic disorder, this therapy involves purposefully arousing physical sensations associated with panic attacks to help clients perceive them as harmless.
Mindfulness-Based Cognitive Therapy (MBCT)
MBCT combines mindfulness meditation with CBT tools, encouraging clients to "decenter" and observe their thoughts and feelings objectively.
Group and Family Therapies
Group therapy provides support and advice among members, while family therapy aims to improve family dynamics and roles. Self-help groups like Alcoholics Anonymous are also common.

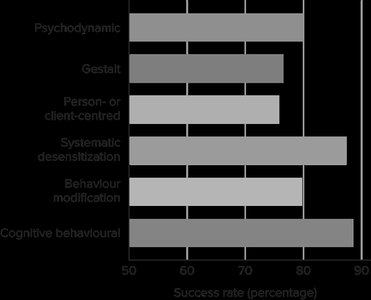
Evaluating Therapy Effectiveness
Psychotherapy is generally effective for most people, though not universally. Different treatments are suited to different problems, and therapists often use an eclectic approach.
Biomedical Therapies
Biomedical therapies involve altering brain chemistry or function to alleviate symptoms of mental disorders.
Antipsychotic Drugs: Block dopamine receptors to reduce psychotic symptoms.
Antianxiety Drugs: Benzodiazepines (e.g., Ativan) increase GABA activity but carry risks of dependence.
Antidepressant Drugs: Tricyclics, MAO inhibitors, and SSRIs (e.g., Prozac) target neurotransmitters like serotonin and norepinephrine.
Herbal Remedies: St. John’s Wort may reduce depression but lacks standardization and can interact with other medications.
New Directions: Ketamine therapy, transcranial magnetic stimulation (TMS), and electroconvulsive therapy (ECT) are used for treatment-resistant cases.
Psychosurgery: Rarely used today, reserved for severe, treatment-resistant cases.
Controversial and Emerging Therapies
Some therapies, such as Eye Movement Desensitization and Reprocessing (EMDR), are controversial due to limited evidence for their effectiveness.
Classic Study: On Being Sane in Insane Places (Rosenhan, 1970s)
Rosenhan's study involved "sane" individuals gaining admission to psychiatric hospitals by feigning auditory hallucinations. The study highlighted issues of misdiagnosis, depersonalization, and the challenges of distinguishing sanity from insanity in institutional settings.
