 Back
BackSocial Determinants of Health: Concepts, Frameworks, and Policy Implications
Study Guide - Smart Notes

Introduction to Social Determinants of Health
Overview
The social determinants of health (SDH) are the social, economic, and political factors that influence the health of individuals and populations. Understanding SDH is essential for addressing health disparities and promoting health equity within societies. This topic is foundational in sociology, public health, and health policy studies.
Definition: Social determinants of health are the economic and social conditions that shape the health of individuals, communities, and jurisdictions as a whole.
Importance: SDH explain why health outcomes vary across different groups and regions, often reflecting broader patterns of social advantage and disadvantage.
Key Focus: The quantity and quality of resources society makes available to its members (Raphael, 2025).
Concepts of Health
Four Broad Approaches to Health
The concept of health adopted by a society or agency shapes health policy, interventions, and the allocation of resources. There are four main approaches:
Medical (Traditional/Biomedical): Health is the absence of disease or disability. Focuses on physiological risk factors and disease categories.
Behavioural (Lifestyle): Health is seen as a result of individual choices and behaviors, such as diet, exercise, and substance use.
Socio-Environmental (Societal): Health is a positive state supported by social connections, community, and societal structures. Emphasizes psychosocial and environmental risk factors.
Political Economy (Structural-Critical): Health is linked to the equitable distribution of resources and power within society. Focuses on structural determinants and the influence of institutions and class.
Comparison of Health Approaches
Approach | Definition of Health | Main Strategies | Target | Actors |
|---|---|---|---|---|
Medical | Absence of disease/disability | Treatment, screening, medical care | High-risk individuals | Physicians, nurses, allied health |
Behavioural | Healthy behaviors, functional ability | Health education, social marketing | High-risk groups, youth | Public health workers, advocacy groups |
Socio-Environmental | Connectedness, control, meaningful life | Community development, advocacy | High-risk societal conditions | Citizens, welfare organizations |
Political Economy | Equitable resource distribution | Political action, policy change | Influence of wealthy/powerful | Political movements, parties |
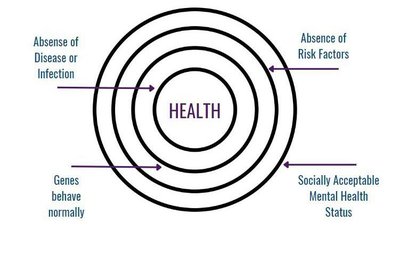
Medical (Traditional/Biomedical) Approach
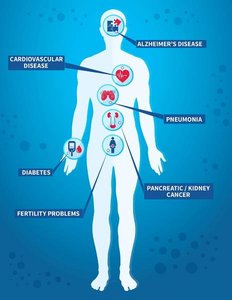
This approach defines health as the absence of disease or disability and focuses on physiological risk factors. Strategies include medical interventions, screening, and individualized care.
Examples of health problems: Cardiovascular disease, diabetes, AIDS, obesity, mental illness.
Principal strategies: Surgery, medication, patient education, screening for risk factors.

Behavioural (Lifestyle) Approach
This approach emphasizes individual responsibility for health through lifestyle choices. Health is seen as energy, functional ability, and disease prevention through behaviors.
Examples of risk factors: Smoking, poor diet, lack of exercise, substance abuse, poor stress management.
Principal strategies: Health education, social marketing, advocacy for supportive policies.



Socio-Environmental (Societal) Approach
This approach defines health as a positive state supported by social connections and community structures. It focuses on psychosocial and environmental risk factors such as poverty, social isolation, and hazardous environments.
Principal strategies: Community development, coalition building, political advocacy, societal change.
Target: High-risk societal conditions.
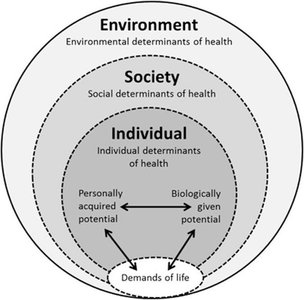
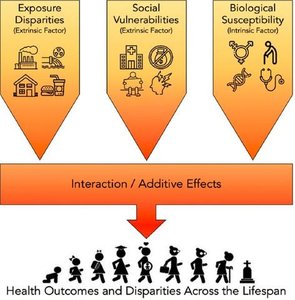
Political Economy (Structural-Critical) Approach
This approach links health to the distribution of resources and power in society. It emphasizes the role of institutions, class, and political structures in shaping health outcomes.
Principal strategies: Political action, regulation of business, public policy reform, strengthening the welfare state.
Target: Structural inequalities and the influence of the wealthy and powerful.
Social Determinants of Health (SDH)
Definition and Frameworks
SDH are the interrelated social, political, and economic factors that create the conditions in which people live, learn, work, and play. They are concerned with the resources available to individuals and communities, and how these shape health outcomes.
Key SDH in Canada: Indigenous ancestry, disability status, early life, education, employment, food security, health services, gender, housing, income, racism, social exclusion, social safety net, unemployment.
Geographical Patterns of Health Inequities
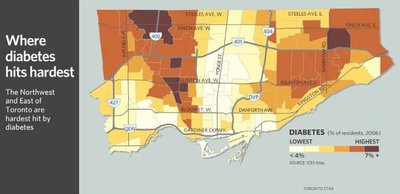
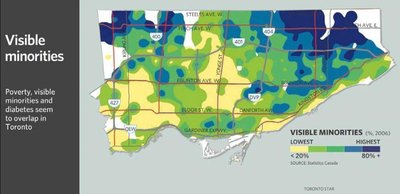
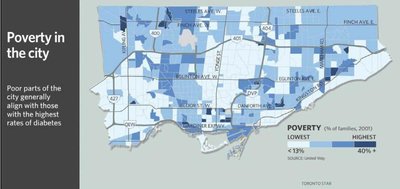
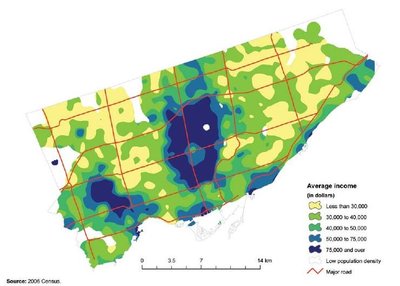
Health outcomes such as diabetes, poverty, and crime often show clear geographical patterns, reflecting underlying social determinants. For example, certain neighborhoods in Toronto experience higher rates of diabetes, poverty, and crime, which often overlap with areas of higher visible minority populations and lower average incomes.
Health Equity and Inequity
Definitions
Health Equity: The absence of unfair, avoidable, or remediable differences among groups of people, whether defined socially, economically, demographically, or geographically (WHO, 2010).
Health Inequity: Differences in health associated with social disadvantages that are modifiable and considered unfair. These are systematic, avoidable, and relate to differences in opportunity (e.g., access to healthcare, education, or healthy living conditions).
Health Inequality: Measurable differences in health between individuals, groups, or communities, which may be natural or unavoidable (e.g., genetics, age).
Public Policy and Health Promotion
Shifting the Focus from Health Care to Health Promotion
Health care spending alone cannot reduce health disparities. Addressing the root causes of poor health—such as poverty, housing, and education—requires a broader focus on health promotion and prevention. Governments must expand their efforts to include social supports and policies that address these determinants.
Key strategies: Expanding public policy to address root causes, promoting healthy environments, and supporting social equity.

Ten Tips for Better Health: Traditional vs. Social Determinants Perspective
Traditional Tips
Don’t smoke. If you can, stop. If you can’t, cut down.
Follow a balanced diet with plenty of fruit and vegetables.
Keep physically active.
Manage stress by talking things through and making time to relax.
If you drink alcohol, do so in moderation.
Cover up in the sun, and protect children from sunburn.
Practice safer sex.
Take up cancer screening opportunities.
Be safe on the roads: follow the Highway Code.
Learn the First Aid ABCs: airways, breathing, circulation.
Social Determinants Tips
Don’t be poor. If you can, stop. If you can’t, try not to be poor for long.
Don’t have poor parents.
Own a car.
Don’t work in a stressful, low paid manual job.
Don’t live in damp, low quality housing.
Be able to afford to go on a foreign holiday and sunbathe.
Practice not losing your job and don’t become unemployed.
Take up all benefits you are entitled to, if you are unemployed, retired or sick or disabled.
Don’t live next to a busy major road or near a polluting factory.
Learn how to fill in complex housing benefit/asylum application forms before you become homeless and destitute.
APA 7th Edition: Best Practices for Students
Academic Integrity and Citation
Use in-text citations whenever you use someone else’s ideas, data, or words. Format: (Author, Year).
Paraphrase instead of quoting; always put ideas in your own words and cite the source.
Include a reference list at the end of your paper, with all sources cited in text.
Follow formatting rules: 12 pt. Times New Roman (or Calibri/Arial), double-spaced, 1-inch margins, page numbers, and a title page.
Avoid plagiarism by crediting all ideas, even if paraphrased.
Summary Table: Key Social Determinants of Health in Canada
Determinant | Description |
|---|---|
Income and Income Distribution | Access to resources, ability to afford healthy living conditions |
Education | Opportunities for employment, health literacy, social mobility |
Employment and Working Conditions | Job security, workplace safety, stress levels |
Housing | Quality, affordability, and stability of living environment |
Food Security | Reliable access to sufficient, safe, and nutritious food |
Social Exclusion | Marginalization based on race, gender, disability, etc. |
Health Services | Availability and accessibility of medical care |
Additional info: The course also covers academic honesty, the use of AI in academic work, and best practices for assignments and exams, emphasizing critical thinking and independent scholarship.
