 Back
BackSocial Determinants of Health: Mechanisms, Pathways, and Inequalities
Study Guide - Smart Notes

Social Determinants of Health
Defining Social Determinants of Health
The social determinants of health (SDOH) are the conditions in which people are born, grow, live, work, and age. These determinants are shaped by the distribution of money, power, and resources at global, national, and local levels. SDOH are primary predictors of health outcomes, often exerting stronger effects than individual behaviors such as smoking, diet, or exercise.
Key determinants: early life, education, employment and working conditions, food security, geography, health care services, housing, income and its distribution, social exclusion, social safety net, unemployment and employment security.
Social locations: disability, gender, immigrant status, Indigenous ancestry, race.

Upstream vs Downstream Interventions
Addressing health requires moving beyond treating symptoms to tackling root causes. Upstream interventions focus on changing social and structural factors that lead to poor health, while downstream interventions address immediate health needs.
Upstream: Policy, education, social supports.
Downstream: Therapy, medical treatment.

Equality, Equity, and Reality in Health
Conceptualizing Fairness
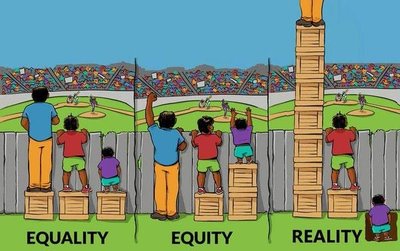
Health outcomes are influenced by how resources and opportunities are distributed. Equality means everyone gets the same resources, equity means resources are distributed based on need, and reality reflects actual disparities.
Equality: Uniform distribution, may not address needs.
Equity: Adjusted distribution, aims to level the playing field.
Reality: Shows persistent gaps and structural barriers.
Health Gradients and Social Factors
The Health Gradient
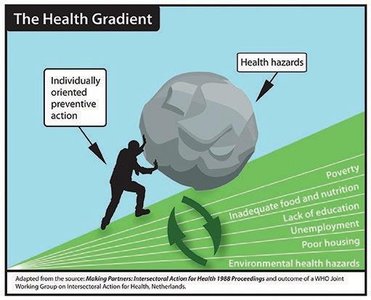
The health gradient describes stepwise differences in health outcomes across socioeconomic groups. Individuals face increasing health hazards as they move down the gradient, with poverty, poor housing, and environmental risks compounding disadvantage.
Health hazards: Poverty, inadequate food/nutrition, lack of education, unemployment, poor housing, environmental health hazards.
Preventive action: Often limited by structural barriers.
Premature Years of Life Lost and Income-Related Causes
Premature Mortality in Canada
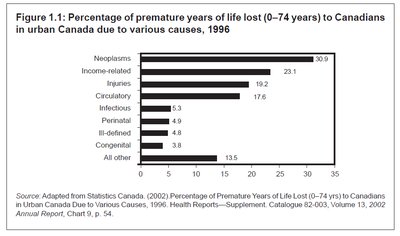
Premature years of life lost (YLL) are disproportionately caused by income-related factors. Data from urban Canada (1996) show neoplasms, income-related causes, and circulatory diseases as leading contributors.
Neoplasms: 30.9%
Income-related: 23.1%
Circulatory: 17.6%
Income-Related Disease Burden
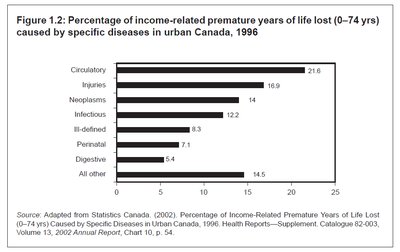
Specific diseases contribute to income-related premature YLL, with circulatory diseases and injuries being most prominent.
Circulatory: 21.8%
Injuries: 16.9%
Neoplasms: 14%
Income Inequality and Excess Deaths
Risk Ratios and Excess Deaths
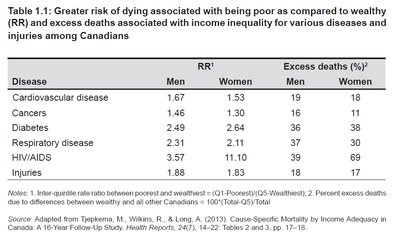
Being poor is associated with a greater risk of dying from various diseases and injuries. The table below shows relative risk (RR) and excess deaths for men and women in Canada.
Disease | RR (Men) | RR (Women) | Excess Deaths (%) Men | Excess Deaths (%) Women |
|---|---|---|---|---|
Cardiovascular disease | 1.67 | 1.53 | 19 | 18 |
Cancers | 1.46 | 1.30 | 16 | 11 |
Diabetes | 2.49 | 2.64 | 21 | 26 |
Respiratory disease | 2.31 | 2.11 | 37 | 39 |
HIV/AIDS | 3.14 | 3.11 | 18 | 30 |
Injuries | 1.88 | 1.83 | 17 | 17 |
International Comparisons: Social Determinants and Health Outcomes
Finland, Canada, and US Rankings
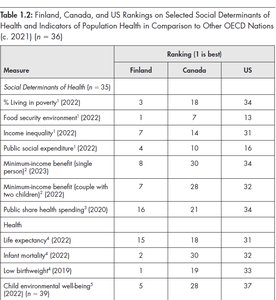
Countries differ in their social determinants and health outcomes. Finland consistently ranks higher than Canada and the US in measures such as poverty, food security, income inequality, public expenditure, and child well-being.
Measure | Finland | Canada | US |
|---|---|---|---|
% Living in poverty (2022) | 3 | 18 | 34 |
Food security environment (2022) | 1 | 7 | 34 |
Income inequality (2022) | 7 | 14 | 36 |
Public expenditure (2022) | 8 | 30 | 34 |
Life expectancy (2022) | 15 | 18 | 31 |
Child well-being (2022) | 5 | 19 | 37 |
Frameworks for Understanding Health Inequalities
Materialist Framework
The materialist framework emphasizes objective living conditions and socioeconomic position as predictors of health. Health gradients reflect stepwise differences, not just a rich-poor divide. Early life experiences, education, and employment shape future health and income potential.
Psychobiological Stress Response
Chronic stress leads to allostatic load, the cumulative wear and tear on the body. Dysfunctional stress responses can cause cardiovascular and immune system damage, accelerate aging, and increase risks for diabetes, heart disease, and premature death.
Lifecourse Perspective
Health outcomes are shaped across the life course by early exposures and accumulated conditions. Latent, pathway, and cumulative effects explain how disadvantage compounds over time.
Neo-Materialist Perspective
Health inequalities are shaped by how societies allocate resources. Universal health care, quality education, and strong public investment lead to better living conditions and fairer, healthier societies.
Social Comparison Perspective
Health inequalities arise not only from material deprivation but also from perceived social position. Feelings of shame, worthlessness, and envy activate stress pathways, leading to poorer physical and mental health.
Structural Inequities and Health
Gender, Race, Disability, and Immigration
Structural inequities concentrate disadvantage among certain groups. Women, racialized groups, immigrants, and people with disabilities face higher poverty, unemployment, and barriers to access, resulting in poorer health outcomes.
Best Practices for Scholarly Research
Effective Article Searching
Use Google Scholar with university access for peer-reviewed sources.
Filter results by year, relevance, and publication type.
Prefer sources with stable identifiers (DOI), credible authors, and recent publication dates.
Avoid non-academic sources such as blogs, social media, and opinion pieces.
Summary
Social determinants of health are central to understanding health inequalities. Material conditions, stress pathways, social comparisons, and structural inequities all contribute to health outcomes. International comparisons highlight the importance of policy and resource allocation in shaping population health.
