 Back
BackBlood Vessels: Structure, Function, and Hemodynamics
Study Guide - Smart Notes

Blood Vessels: Overview and Functional Organization
The Circulatory Pathways
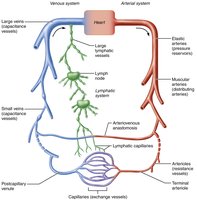
The blood vessels form a closed delivery system that begins and ends at the heart, ensuring efficient transport of blood throughout the body. The main types of vessels are arteries, arterioles, capillaries, venules, and veins. Arteries carry oxygen-rich blood away from the heart, while veins return oxygen-poor blood toward the heart. The pulmonary circuit is an exception, with pulmonary arteries carrying oxygen-poor blood to the lungs and pulmonary veins returning oxygen-rich blood to the heart. Only capillaries directly serve cells by facilitating exchange with tissues.
Structure of Blood Vessel Walls
General Vessel Wall Architecture
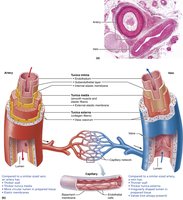
Blood vessel walls (except for capillaries) are composed of three layers (tunics):
Tunica Intima: Innermost layer; consists of endothelium (simple squamous epithelium) and a subendothelial connective tissue layer.
Tunica Media: Middle layer; primarily smooth muscle and sheets of elastin. Responsible for vasoconstriction and vasodilation, regulated by sympathetic nerve fibers.
Tunica Adventitia (Externa): Outermost layer; composed mainly of loose collagen fibers, nerves, and lymphatic vessels. Anchors the vessel to surrounding structures.
Capillaries: Consist only of endothelium and a sparse basal lamina, allowing for efficient exchange.
Vasa Vasorum: Small vessels that supply blood to the walls of larger vessels.
Types of Blood Vessels
Arterial Vessels
Elastic (Conducting) Arteries: Large, thick-walled arteries near the heart (e.g., aorta). Abundant elastic fibers allow them to expand and recoil, maintaining blood pressure and flow. Inactive in vasoconstriction.
Muscular (Distributing) Arteries: Deliver blood to organs. More smooth muscle than elastic tissue; active in vasoconstriction.
Arterioles (Resistance Vessels): Smallest arteries; control blood flow into capillaries via vasodilation and vasoconstriction. Major determinants of peripheral resistance.
Vessel Type | Diameter (D) | Wall Thickness (T) | Relative Tissue Makeup |
|---|---|---|---|
Elastic artery | 1.5 cm | 1.0 mm | High elastic tissue, moderate smooth muscle, moderate fibrous tissue |
Muscular artery | 6.0 mm | 1.0 mm | Moderate elastic tissue, high smooth muscle, moderate fibrous tissue |
Arteriole | 37.0 μm | 6.0 μm | Low elastic tissue, moderate smooth muscle, low fibrous tissue |

Capillaries
Capillaries are the smallest blood vessels and serve as the primary site for exchange of gases, nutrients, and wastes between blood and tissues. Their thin walls consist of only the tunica intima, allowing for efficient diffusion. Pericytes help stabilize capillary walls and regulate permeability. Capillaries are absent in cartilage, epithelia, cornea, and lens of the eye.
Types of Capillaries
Continuous Capillaries: Uninterrupted lining; abundant in skin, muscle, lungs, and CNS.
Fenestrated Capillaries: Endothelial cells with pores; found in kidneys and intestines for active filtration and absorption.
Sinusoidal Capillaries: Large, leaky capillaries with fewer tight junctions; found in liver, bone marrow, spleen, and endocrine organs.
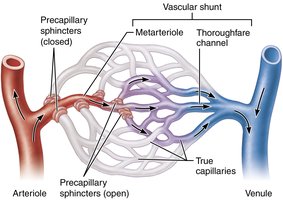
Capillary Beds and Microcirculation
Capillary beds are networks of capillaries between arterioles and venules. Blood flow through these beds is regulated by the diameter of terminal arterioles and precapillary sphincters, which act as valves to control entry into true capillaries. Vascular shunts (metarteriole and thoroughfare channel) allow blood to bypass true capillaries when necessary.
Venules and Veins
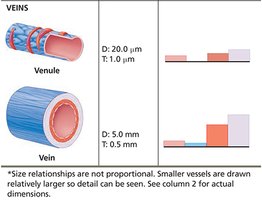
Venules: Formed when capillaries merge; postcapillary venules consist mainly of endothelium and a few fibroblasts. Larger venules have sparse tunica media and thin tunica externa.
Veins: Formed when venules converge; have thinner walls and larger lumens than arteries. Key adaptations include one-way valves (prevent backflow), large lumens, and thin, flexible walls. Veins act as blood reservoirs, containing 60-65% of blood volume at rest.
Hemodynamics: Blood Flow, Pressure, and Resistance
Blood Flow
Blood flow is the volume of blood moving through a vessel, organ, or the entire circulation per unit time (ml/min). It is equivalent to cardiac output for the entire vascular system and can be regulated independently for different organs.
Blood Pressure
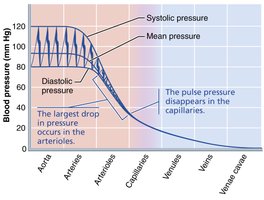
Blood pressure is the force per unit area exerted on a vessel wall by the blood, measured in mmHg. Systemic arterial blood pressure is highest in the aorta and declines throughout the vascular pathway, with the steepest drop in arterioles due to high resistance.
Peripheral Resistance
Resistance is the opposition to blood flow due to friction between blood and vessel walls. It is influenced by:
Blood Viscosity: Increased viscosity increases resistance.
Total Blood Vessel Length: Longer vessels increase resistance.
Blood Vessel Diameter: The most significant factor; resistance varies inversely with the fourth power of the radius (). Small changes in diameter cause large changes in resistance.
Relationship Between Flow, Pressure, and Resistance
Blood flow () is directly proportional to the pressure gradient () and inversely proportional to total peripheral resistance ():
Thus, increasing resistance decreases flow, and increasing pressure increases flow.
Arterial Blood Pressure: Systolic, Diastolic, and Mean Arterial Pressure (MAP)
Systolic Pressure: Pressure during ventricular contraction.
Diastolic Pressure: Lowest pressure during ventricular relaxation.
Pulse Pressure (PP): Difference between systolic and diastolic pressure ().
Mean Arterial Pressure (MAP): Average pressure propelling blood to tissues during the cardiac cycle:
For a BP of 120/80 mmHg: mmHg.
Venous Return and Blood Pressure Regulation
Factors Aiding Venous Return
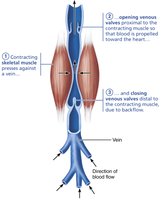
Muscular Pump: Skeletal muscle contractions "milk" blood toward the heart; valves prevent backflow.
Respiratory Pump: Pressure changes during breathing move blood toward the heart.
Venoconstriction: Sympathetic stimulation reduces vein diameter, pushing blood toward the heart.
Regulation of Blood Pressure
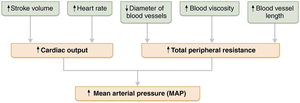
Blood pressure is regulated by cardiac output (CO), total peripheral resistance (TPR), and blood volume. The main equation is:
Where (heart rate × stroke volume).
Neural and Hormonal Controls
Neural: Baroreceptors (pressure sensors), chemoreceptors (detect CO2, O2, pH), and higher brain centers (hypothalamus, cortex) regulate vessel diameter and heart rate via the cardiovascular center in the medulla.
Hormonal: Hormones such as epinephrine, norepinephrine, angiotensin II, ADH, and atrial natriuretic peptide (ANP) influence blood pressure by altering vessel diameter or blood volume.
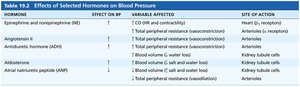
Renal Regulation
The kidneys regulate blood pressure long-term by adjusting blood volume. Increased blood volume leads to increased urine output, lowering blood pressure. The renin-angiotensin system increases blood pressure by promoting vasoconstriction and increasing blood volume via aldosterone and ADH.
Blood Flow Control and Tissue Perfusion
Intrinsic vs. Extrinsic Controls
Intrinsic (Autoregulation): Local control within tissues; includes metabolic and myogenic mechanisms.
Extrinsic: Systemic control via nerves or hormones; redistributes blood flow during exercise or stress.

Blood Flow in Special Areas
Skeletal Muscle: Blood flow increases with activity (active hyperemia).
Brain: Maintains constant flow; sensitive to CO2 and pH changes.
Heart: Coronary circulation is greatest during diastole.
Skin: Regulates temperature and acts as a blood reservoir.
Lungs: Low O2 causes vasoconstriction; high O2 causes vasodilation (opposite of systemic circulation).
Capillary Exchange and Bulk Flow
Mechanisms of Capillary Exchange
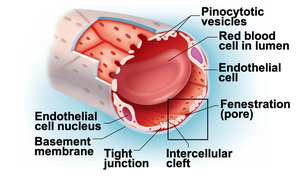
Capillary exchange occurs via diffusion, intercellular clefts, fenestrations, and active transport (pinocytosis). The four main routes are:
Direct diffusion through endothelial membranes (lipid-soluble substances)
Passage through intercellular clefts (water-soluble substances)
Passage through fenestrations (water-soluble substances)
Active transport via pinocytotic vesicles (large molecules)
Bulk Flow and Fluid Movements
Bulk flow is the movement of fluid across capillary walls, driven by hydrostatic and osmotic pressures. Most fluid leaves at the arterial end and returns at the venous end, maintaining interstitial fluid balance. Excess fluid is returned to the blood by the lymphatic system.
Hydrostatic Pressure (HP): Force exerted by fluid against the capillary wall.
Colloid Osmotic Pressure (OP): Pressure exerted by plasma proteins drawing water into the capillary.
Edema results from an imbalance in these pressures or impaired lymphatic drainage.
Clinical Correlations and Homeostatic Imbalances
Hypertension: Sustained high blood pressure (≥130/80 mmHg); primary (no identifiable cause) or secondary (due to another disorder).
Hypotension: Low blood pressure (<90/60 mmHg).
Circulatory Shock: Inadequate blood flow to tissues; types include hypovolemic, vascular, and cardiogenic shock.
Edema: Excess interstitial fluid due to increased capillary hydrostatic pressure, decreased capillary osmotic pressure, or lymphatic obstruction.
