 Back
BackChapter 26: The Urinary System – Structure, Function, and Physiology
Study Guide - Smart Notes

Chapter 26: The Urinary System
Introduction to the Urinary System
The urinary system is essential for maintaining the optimal functioning of body fluids, particularly blood volume and composition. It prevents dehydration, removes metabolic waste, and regulates several physiological parameters to ensure homeostasis.
Main organs: 2 kidneys, 2 ureters, 1 bladder, 1 urethra
Major functions:
Regulation of blood ionic composition (Na+, K+, Cl–)
Regulation of blood pH (H+, HCO3–)
Regulation of blood volume and pressure
Maintenance of blood osmolarity
Production of hormones (Calcitriol and Erythropoietin)
Excretion of metabolic wastes and foreign substances
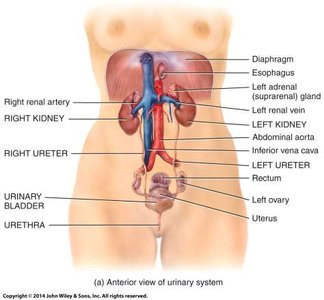
Kidney Anatomy
Location and External Structure
The kidneys are retroperitoneal organs, located inferior to the adrenal glands and partly protected by ribs 11 and 12. They are positioned on either side of the vertebral column.
Renal hilum: The entry and exit site for the renal artery, vein, ureter, nerves, and lymphatics.
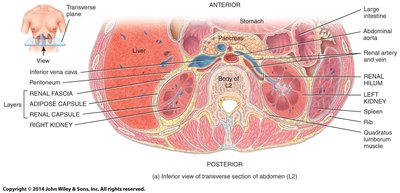
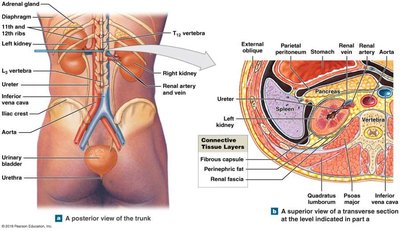
Cross-Sectional Anatomy
The kidney is surrounded by several layers for protection and support, including the renal fascia, adipose capsule, and renal capsule. The renal cortex (outer layer) and renal medulla (inner region) are responsible for urine production, filtration, and reabsorption.
Renal pyramids: Cone-shaped structures in the medulla.
Renal columns: Extensions of cortex anchoring the cortex.
Papillary ducts: Empty urine into calyces, which pass urine to the ureter.
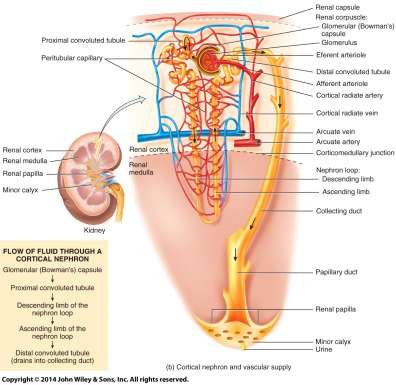
Nephron: The Functional Unit of the Kidney
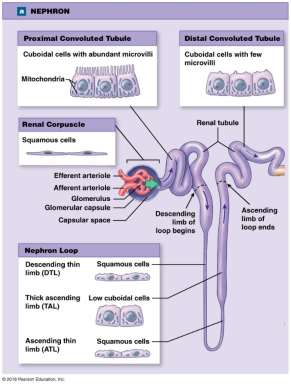
Nephron Structure
Each kidney contains about one million nephrons, which are the functional units responsible for filtering blood and forming urine. Each nephron consists of a renal corpuscle and a renal tubule.
Renal corpuscle: Filters blood plasma (includes the glomerulus and Bowman’s capsule).
Renal tubule: Modifies the filtrate through reabsorption and secretion (includes the proximal convoluted tubule, nephron loop, and distal convoluted tubule).
Nephron Functions
Glomerular filtration: Movement of fluid and solutes from blood into the nephron.
Tubular reabsorption: Return of useful substances from filtrate to blood.
Tubular secretion: Addition of waste products from blood into the filtrate.
Urine formation equation:
Renal Physiology
Glomerular Filtration
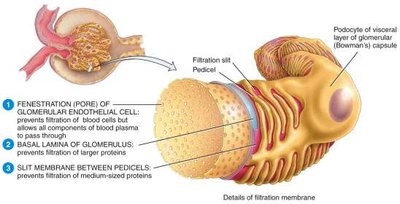
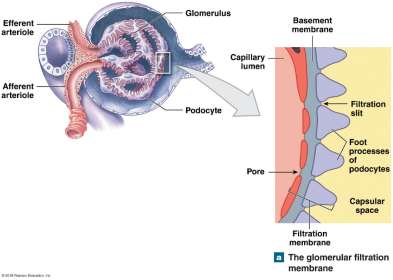
Filtration occurs in the renal corpuscle, where blood pressure forces water and solutes through a filtration membrane. The membrane consists of three layers:
Fenestrated endothelium: Prevents passage of large particles.
Basement membrane: Blocks medium-sized proteins.
Filtration slits (podocytes): Restrict small proteins and macromolecules.
Filtration Pressures
Three main pressures determine the net filtration pressure (NFP):
Glomerular hydrostatic pressure (GHP): Blood pressure in glomerular capillaries (favors filtration).
Capsular hydrostatic pressure (CHP): Pressure of filtrate in the capsule (opposes filtration).
Blood colloid osmotic pressure (BCOP): Osmotic pull of proteins in blood (opposes filtration).
Net Filtration Pressure (NFP) equation:
Example calculation:
Glomerular Filtration Rate (GFR)
The GFR is the amount of filtrate formed by both kidneys each minute. Homeostasis requires a relatively constant GFR:
Too high: Needed substances pass too quickly and are not reabsorbed.
Too low: Nearly all filtrate is reabsorbed, including wastes.
GFR is regulated by:
Renal autoregulation: Adjusts afferent arteriole diameter to maintain steady GFR.
Neural regulation: Sympathetic nervous system constricts afferent arterioles.
Hormonal regulation: Angiotensin II increases GFR when blood volume or pressure drops.
Production of Dilute and Concentrated Urine
Osmolarity Regulation
The kidneys regulate the osmolarity of body fluids by adjusting water and solute reabsorption. This is achieved through the medullary osmotic gradient and the action of antidiuretic hormone (ADH).
High osmolarity: More solutes, less water.
Low osmolarity: Less solutes, more water.
ADH: Increases water reabsorption by inserting aquaporins in the distal convoluted tubule and collecting duct.
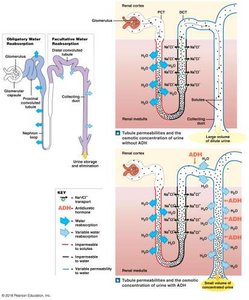
Countercurrent Mechanisms
Countercurrent multiplication: Establishes the osmotic gradient in the renal medulla.
Countercurrent exchange: Maintains the gradient via the vasa recta.
Evaluation of Kidney Function
Urinalysis and Plasma Creatinine
Urinalysis evaluates the physical, chemical, and microscopic properties of urine, including the presence of albumin, glucose, red blood cells, ketone bodies, and microbes. Plasma creatinine is used to assess kidney function.
Urine Transportation and Storage
Urinary Tract Anatomy
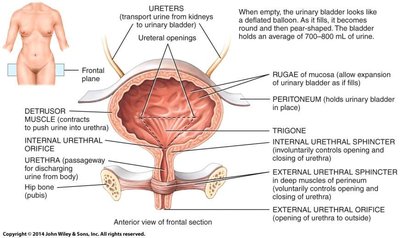
Urine formed in the kidneys is transported via the ureters to the urinary bladder, where it is stored until excretion through the urethra. The bladder's structure allows for expansion and controlled release of urine.
Summary Table: Main Functions of the Urinary System
Function | Description |
|---|---|
Regulation of blood ions | Controls Na+, K+, Cl– levels |
Regulation of pH | Balances H+ and HCO3– |
Regulation of volume & pressure | Adjusts water excretion and hormone release |
Osmolarity maintenance | Regulates solute and water balance |
Hormone production | Calcitriol (vitamin D), erythropoietin (RBC production) |
Excretion | Removes metabolic wastes and toxins |
