 Back
BackDigestive System: Structure, Function, and Regulation
Study Guide - Smart Notes

Digestive System Overview
Major Functions and Organization
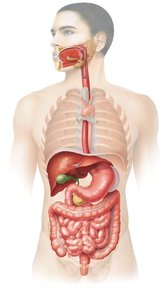
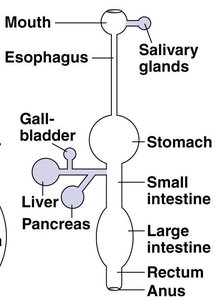
The digestive system is responsible for the breakdown of food, absorption of nutrients, and elimination of waste. It consists of the gastrointestinal (GI) tract—a continuous tube with two openings—and accessory organs that aid in digestion.
GI Tract: Includes the mouth, esophagus, stomach, small intestine, and large intestine.
Accessory Structures: Salivary glands, tongue, teeth, gall bladder, liver, and pancreas.
Key Processes: Ingestion, secretion, propulsion (e.g., peristalsis), digestion (mechanical and chemical), absorption, and elimination (defecation).
Histological Layers of the GI Tract
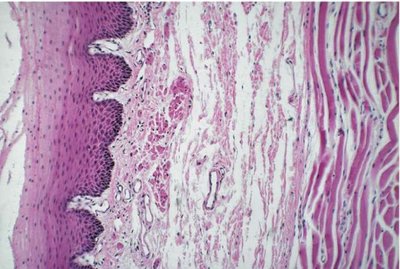
The wall of the alimentary canal is composed of four main layers, each with distinct structures and functions:
Mucosa: Epithelial lining, lamina propria, and muscularis mucosa; involved in secretion and absorption.
Submucosa: Connective tissue containing blood vessels, nerves, and glands.
Muscularis: Two to three layers of smooth muscle responsible for peristalsis and segmentation.
Serosa/Adventitia: Outermost layer; serosa if within the peritoneal cavity, adventitia if outside.
The Peritoneum and Its Folds
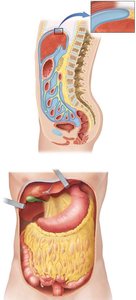
The peritoneum is a serous membrane lining the abdominopelvic cavity, providing protection, suspension, and a route for blood and nerve supply to the organs. It has two layers:
Parietal Peritoneum: Lines the inner wall of the cavity.
Visceral Peritoneum: Covers the organs and is continuous with the serosa.
Major Folds: Mesenteries, greater omentum, and lesser omentum support and stabilize the organs.
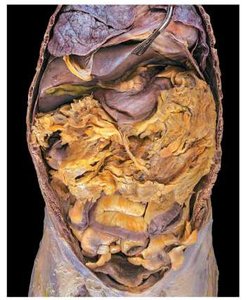
Oral Cavity, Teeth, and Salivary Glands
Structure and Function of the Oral Cavity
The oral cavity (mouth) is formed by the cheeks, lips, tongue, and palate. It contains the teeth and salivary glands and is the entry point for food, initiating ingestion, secretion, mixing, and chemical digestion.
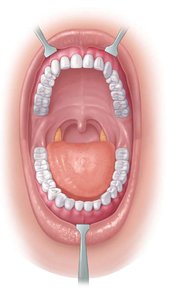
Teeth: Types and Functions
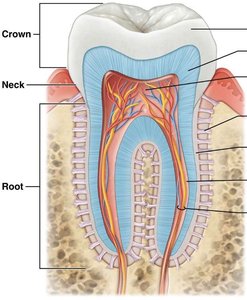
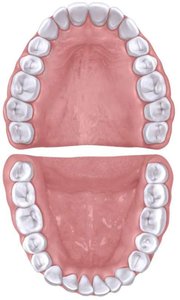
Teeth are specialized for mechanical digestion (mastication), increasing the surface area of food for enzymatic action. Each tooth has three regions: crown, neck, and root. Humans have two sets of teeth (primary and secondary) and four types:
Incisors: Cutting food
Canines: Shearing food
Premolars and Molars: Crushing and grinding food
Salivary Glands
There are three paired salivary glands: parotid, submandibular, and sublingual. Saliva is 99.5% water and 0.5% solutes (enzymes, salts, organics, gases). It lubricates food and begins chemical digestion.
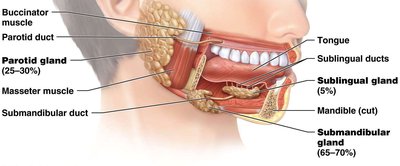
Pharynx and Esophagus
Structure and Function
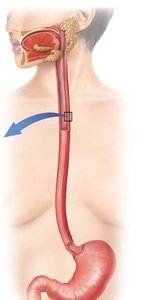
The pharynx connects the oral cavity to the esophagus and is involved in propulsion only. The esophagus is a muscular tube with upper and lower sphincters, transitioning from skeletal to smooth muscle along its length.
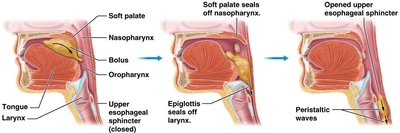
Deglutition (Swallowing)
Swallowing moves the bolus from the mouth to the stomach in three stages:
Voluntary: Tongue pushes food to oropharynx.
Pharyngeal: Epiglottis closes off the airway; food moves to esophagus.
Esophageal: Peristalsis moves food through the esophagus.
Stomach
Gross Anatomy and Regions
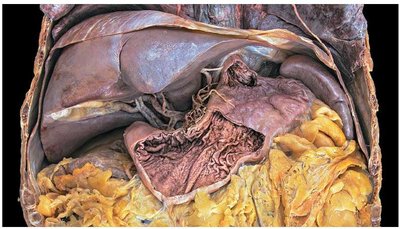
The stomach is a J-shaped organ bounded by the esophageal and pyloric sphincters. It serves as a mixing and holding area for food and has four regions: cardia, fundus, body, and pylorus. The mucosa forms rugae when empty.
Histology of the Stomach
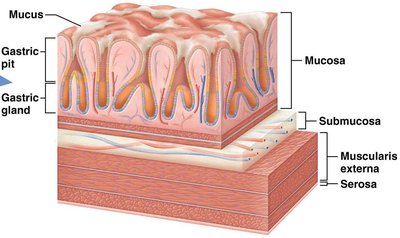
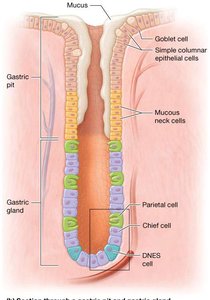
The stomach wall contains simple columnar epithelium, with mucosal folds forming gastric pits and glands. The glands contain several cell types:
Mucous Cells: Secrete mucus
Mucous Neck Cells: Secrete acidic mucus
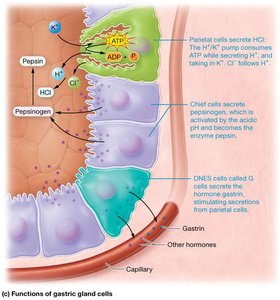
Parietal Cells: Secrete H+, Cl-, and intrinsic factor (for B12 absorption)
Chief Cells: Secrete pepsinogen and gastric lipase
Enteroendocrine Cells (G cells): Secrete gastrin
Mechanical and Chemical Digestion in the Stomach
Mechanical digestion involves peristaltic contractions that mix food. Chemical digestion is primarily by pepsin (protein digestion in the presence of HCl) and gastric lipase (lipid digestion). Minimal absorption occurs in the stomach (e.g., alcohol, aspirin).
Phases of Gastric Secretion and Motility
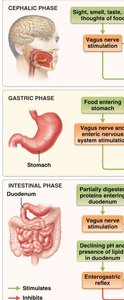
There are three overlapping phases of gastric activity:
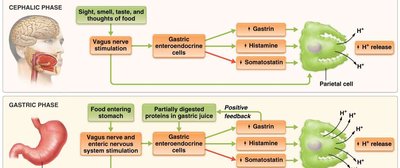
Cephalic Phase: Initiated by sensory input; stimulates gastric secretion and motility.
Gastric Phase: Triggered by food in the stomach; enhances secretion and motility.
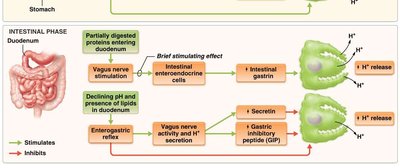
Intestinal Phase: Begins as chyme enters the small intestine; regulates further gastric activity.
Small Intestine
Structure and Regions
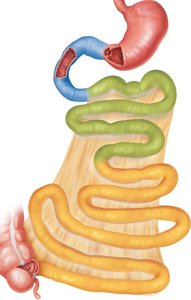
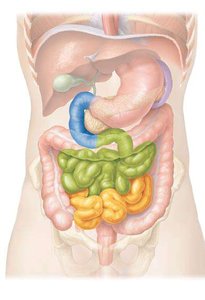
The small intestine is the primary site for chemical digestion and nutrient absorption. It extends from the pyloric sphincter to the ileocecal sphincter and is divided into three regions: duodenum, jejunum, and ileum. Circular folds increase surface area for absorption.
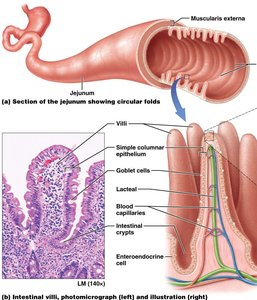
Histology and Absorptive Structures
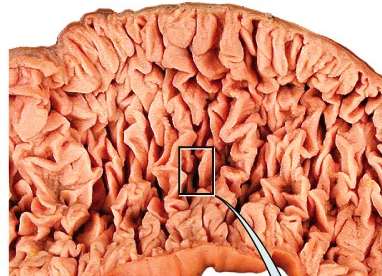
The mucosa of the small intestine is folded into villi, each containing a lacteal and blood supply. Microvilli on enterocytes form the brush border, increasing surface area and containing enzymes for final digestion. Goblet cells secrete mucus, and enteroendocrine cells release hormones (secretin, CCK, GIP).
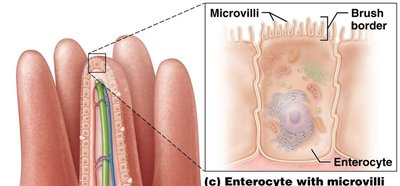
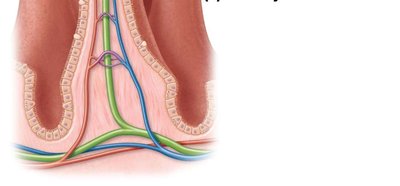
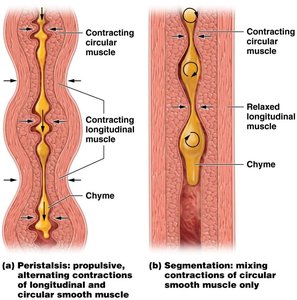
Motility in the Small Intestine
Motility includes segmentation (mixing by circular muscle contractions) and peristalsis (propulsive, alternating contractions of longitudinal and circular muscle). These processes mix and propel contents through the intestine.
Large Intestine
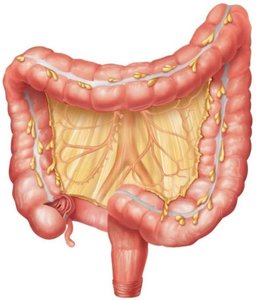
Structure and Function
The large intestine completes water absorption, produces certain vitamins, and forms and expels feces. It extends from the ileocecal sphincter to the anus and is divided into the cecum, colon (ascending, transverse, descending, sigmoid), rectum, and anal canal. The appendix is attached to the cecum.
Histology of the Large Intestine
The mucosa contains many goblet cells but lacks villi and circular folds. The muscularis layer has longitudinal muscle modified into taeniae coli, which contract to form pouches called haustra.
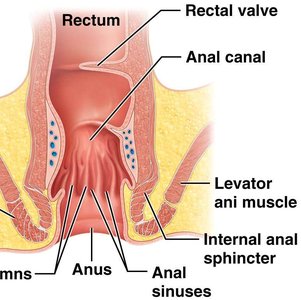
Defecation Reflex
The defecation reflex is triggered by stretch receptors in the sigmoid colon. Voluntary contraction of the diaphragm and abdominal muscles, along with relaxation of the external anal sphincter, allows elimination of feces.
Accessory Organs: Pancreas, Liver, and Gallbladder
Pancreas
The pancreas is located posterior to the stomach and has both endocrine (1%) and exocrine (99%) functions. Its exocrine acini secrete digestive enzymes:
Pancreatic Amylase: Digests starch
Trypsin, Chymotrypsin, Carboxypeptidase: Digest proteins
Pancreatic Lipase: Digests fats
Ribonuclease, Deoxyribonuclease: Digest nucleic acids
Liver and Gallbladder
The liver is the largest internal organ and produces bile, which emulsifies fats and aids in waste excretion. It also processes nutrients and detoxifies substances. The gallbladder stores and releases bile into the duodenum as needed.
Liver Lobules: Functional units containing hepatocytes arranged around a central vein. Blood flows through sinusoids, and bile is collected in canaliculi.
Portal Triads: Consist of a bile duct, hepatic arteriole (O2-rich blood), and hepatic portal venule (nutrient-rich, O2-poor blood).
Nutrient Digestion and Absorption
Enzymatic Hydrolysis and Chemical Digestion
Enzymatic hydrolysis breaks down macromolecules into absorbable units:
Carbohydrates: Digested into monosaccharides (e.g., glucose, galactose)
Proteins: Digested into amino acids
Lipids: Digested into fatty acids and monoglycerides
Absorption Mechanisms
Absorption occurs primarily in the small intestine:
Monosaccharides, amino acids, short-chain fatty acids, nucleic acids, water, electrolytes, and vitamins are absorbed into blood capillaries.
Lipids are emulsified by bile salts, digested by pancreatic lipase, and absorbed as micelles. They are reassembled into chylomicrons and absorbed into lacteals (lymphatic vessels), bypassing the liver initially.
Water-soluble vitamins (B, C) are absorbed in the small intestine; fat-soluble vitamins (A, D, E, K) are absorbed with micelles. Vitamin B12 requires intrinsic factor for absorption in the ileum.
More than 9 liters of water enter the small intestine daily, with most absorbed in the small intestine and the remainder in the large intestine. Only about 0.1 L is excreted in feces.
Additional info: The notes above integrate and expand upon the provided lecture slides, adding definitions, examples, and academic context for clarity and completeness.
