 Back
BackThe Immune System: Innate and Adaptive Defenses
Study Guide - Smart Notes

The Immune System: Innate and Adaptive Defenses
Introduction to the Immune System
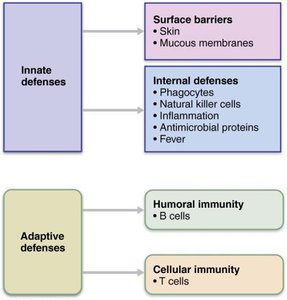
The immune system is a functional system that provides resistance to disease by recognizing and eliminating pathogens and abnormal cells. It consists of two main branches: innate (nonspecific) defenses and adaptive (specific) defenses. These systems work together to protect the body from infection and disease.
Innate (Nonspecific) Defenses
Overview of Innate Defenses
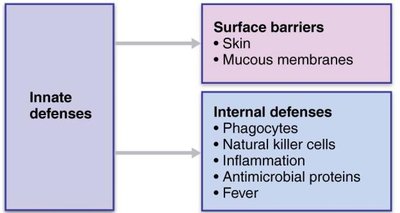
Innate defenses are present at birth and provide the first and second lines of defense against pathogens. They respond quickly and non-specifically to a wide range of invaders.
First line of defense: Surface barriers such as skin and mucous membranes.
Second line of defense: Internal defenses including phagocytes, natural killer cells, inflammation, antimicrobial proteins, and fever.
First Line of Defense: Surface Barriers
The skin and mucous membranes, along with their secretions, form physical and chemical barriers to most microorganisms. These barriers are essential in preventing pathogen entry.
Keratin: Provides resistance against acids, alkalis, and bacterial enzymes.
Mucosae: Line body cavities open to the exterior and trap microorganisms.
CATEGORY/ASSOCIATED ELEMENTS | PROTECTIVE MECHANISM |
|---|---|
Intact skin epidermis | Forms mechanical barrier that prevents entry of pathogens and other harmful substances into body |
Acid mantle of skin | Skin secretions make epidermal surface acidic, which inhibits bacterial growth; also contain various bactericidal chemicals |
Keratin | Provides resistance against acids, alkalis, and bacterial enzymes |
Intact mucous membranes | Mechanical barrier that prevents entry of pathogens |
Mucus | Traps microorganisms in respiratory and digestive tracts |
Nasal hairs | Filter and trap microorganisms in nasal passages |
Cilia | Propel debris-laden mucus away from nasal cavity and lower respiratory passages |
Gastric juice | Contains concentrated hydrochloric acid and protein-digesting enzymes that destroy pathogens in stomach |
Acid mantle of vagina | Inhibits growth of bacteria and fungi in female reproductive tract |
Lacrimal secretion, saliva | Continuously lubricate and cleanse eyes (tears) and oral cavity (saliva); contain lysozyme, an enzyme that destroys microorganisms |
Urine | Normally acid pH inhibits bacterial growth; cleanses the lower urinary tract as it flushes from the body |

Second Line of Defense: Internal Defenses
If pathogens breach surface barriers, the second line of defense is activated. This includes various cells and chemicals that inhibit the spread of invaders and initiate inflammation.
Phagocytes: White blood cells that ingest and digest pathogens. Main types include neutrophils and macrophages.
Natural Killer (NK) Cells: Nonphagocytic lymphocytes that kill virus-infected and cancer cells by inducing apoptosis.
Inflammation: Local tissue response to injury or infection, characterized by redness, heat, swelling, pain, and loss of function.
Antimicrobial Proteins: Interferons and complement proteins that attack microorganisms or hinder their reproduction.
Fever: Systemic response that increases body temperature to inhibit pathogen growth and speed up tissue repair.
Phagocytes
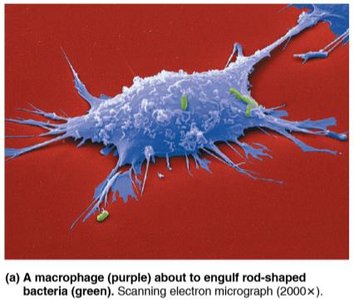
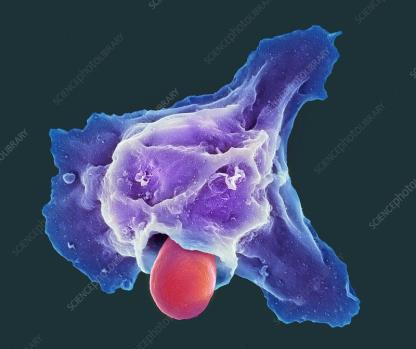
Phagocytes are essential for engulfing and destroying pathogens. Neutrophils are the most abundant but short-lived, while macrophages are the main phagocytic cells and can be free or fixed in tissues.
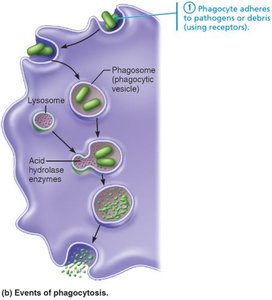
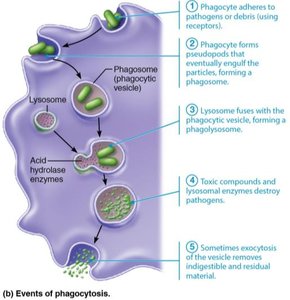
Phagocytosis Process
Phagocyte recognizes and adheres to pathogen (often enhanced by opsonization).
Cytoplasmic extensions (pseudopods) engulf the particle, forming a phagosome.
Phagosome fuses with a lysosome, forming a phagolysosome.
Lysosomal enzymes digest the pathogen.
Indigestible material is expelled by exocytosis.
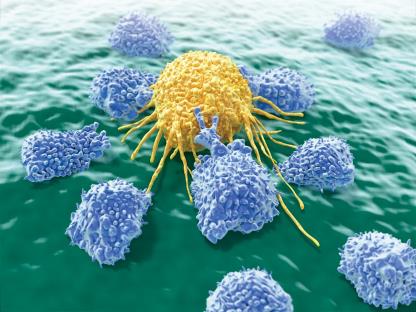
Natural Killer (NK) Cells
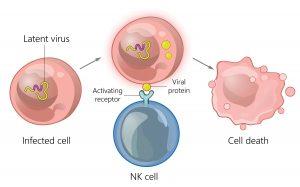
NK cells patrol the body, targeting cells that lack "self" markers, such as virus-infected or cancerous cells. They induce apoptosis and secrete chemicals that enhance inflammation.
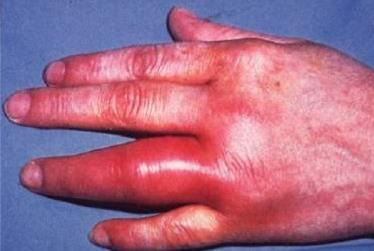
Inflammation
Inflammation is triggered by tissue injury and serves to prevent the spread of damaging agents, dispose of debris, alert the adaptive immune system, and set the stage for repair. The five cardinal signs are redness, heat, swelling, pain, and loss of function.
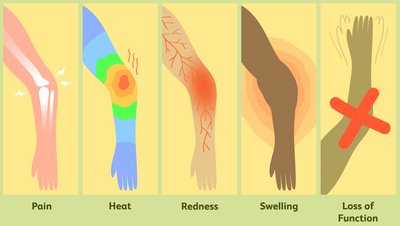
Inflammatory Chemicals
Chemical | Source | Physiological Effects |
|---|---|---|
Histamine | Mast cells and basophils | Vasodilation, increased permeability, chemotaxis |
Kinins | Plasma protein, kininogen | Similar to histamine, induces pain |
Prostaglandins | Fatty acid molecules | Similar to histamine, induces pain |
Complement | Plasma proteins | Enhances inflammation, promotes phagocytosis |
Cytokines | Various cells | Mediate inflammation and immune responses |

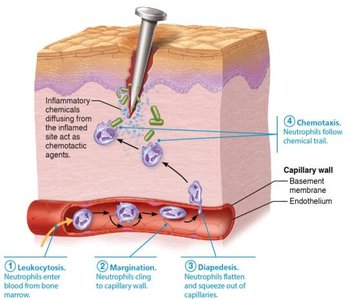
Phagocyte Mobilization
Leukocytosis: Neutrophils enter blood from bone marrow.
Margination: Neutrophils cling to capillary walls.
Diapedesis: Neutrophils squeeze out of capillaries into tissues.
Chemotaxis: Neutrophils follow chemical signals to the injury site.
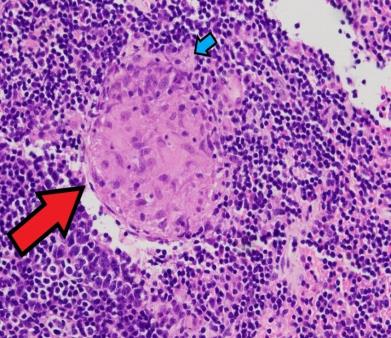
Pus and Granulomas
Pus is a mixture of dead neutrophils, tissue cells, and pathogens. Some bacteria resist digestion and can form granulomas—tumor-like masses of infected macrophages surrounded by other immune cells.
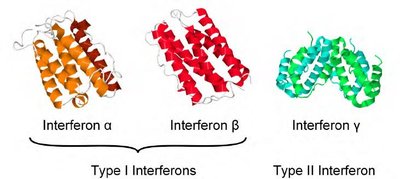
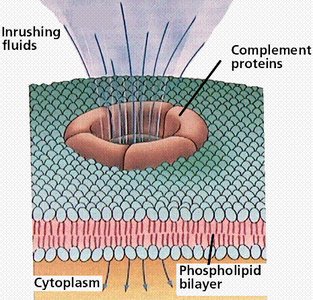
Antimicrobial Proteins
Antimicrobial proteins such as interferons and complement proteins enhance innate defenses by attacking microorganisms or hindering their ability to reproduce.
Fever
Fever is a systemic response to infection, mediated by pyrogens that reset the hypothalamic thermostat. Moderate fever helps by sequestering iron and zinc and increasing metabolic rate for repair.
Adaptive (Specific) Defenses
Overview of Adaptive Defenses
The adaptive immune system is specific, systemic, and has memory. It eliminates almost any pathogen or abnormal cell and amplifies the inflammatory response. It is divided into two main branches: humoral (antibody-mediated) and cellular (cell-mediated) immunity.
Humoral immunity: Mediated by B cells and antibodies; targets extracellular pathogens.
Cellular immunity: Mediated by T cells; targets intracellular pathogens and abnormal cells.
Antigens
Antigens are substances that provoke an immune response. They are usually large, complex molecules not normally found in the body. Antigens can be complete (immunogenic and reactive) or haptens (incomplete, only immunogenic when attached to body proteins).
Antigenic determinants: Specific sites on antigens where antibodies or lymphocyte receptors bind.
Self-antigens (MHC proteins): Unique to each individual; present self or foreign antigens to T cells.
Lymphocytes and Antigen-Presenting Cells (APCs)
Adaptive immunity involves three major cell types:
B lymphocytes (B cells): Responsible for humoral immunity.
T lymphocytes (T cells): Responsible for cellular immunity.
Antigen-presenting cells (APCs): Engulf antigens and present fragments to T cells (e.g., dendritic cells, macrophages, B cells).
Lymphocyte Development, Maturation, and Activation
Origin: Both B and T cells originate in red bone marrow.
Maturation: B cells mature in bone marrow; T cells mature in thymus. They develop immunocompetence and self-tolerance.
Seeding secondary lymphoid organs: Immunocompetent but naïve lymphocytes circulate and colonize secondary lymphoid organs.
Antigen encounter and activation: Lymphocytes encounter antigens and become activated.
Proliferation and differentiation: Activated lymphocytes proliferate and differentiate into effector and memory cells.
Summary Table: Innate vs. Adaptive Defenses
Innate Defenses | Adaptive Defenses |
|---|---|
Surface barriers (skin, mucous membranes) | Humoral immunity (B cells, antibodies) |
Internal defenses (phagocytes, NK cells, inflammation, antimicrobial proteins, fever) | Cellular immunity (T cells) |
