 Back
BackThe Male Reproductive System: Structure, Function, and Spermatogenesis
Study Guide - Smart Notes

The Male Reproductive System
Overview
The male reproductive system is responsible for the production, maturation, nourishment, and transport of male gametes (sperm), as well as the secretion of male sex hormones (androgens). It consists of the testes, duct system, accessory glands, and external genitalia.
Structures of the Male Reproductive System
Testes (Male Gonads)
Function: Produce sperm and secrete androgens (mainly testosterone).
Location: Housed in the scrotum, outside the body cavity to maintain a temperature lower than core body temperature, which is essential for normal spermatogenesis.
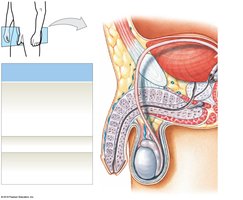
Scrotum and Temperature Regulation
Dartos Muscle: Smooth muscle in the scrotal dermis; causes wrinkling of the scrotal surface.
Cremaster Muscle: Skeletal muscle deep to the dermis; tenses the scrotum and pulls the testes closer to the body in response to cold or arousal.
Temperature Regulation: Sperm development requires temperatures about 1.1ºC lower than body temperature. The muscles contract or relax to move the testes closer or further from the body to maintain optimal temperature.
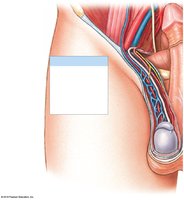
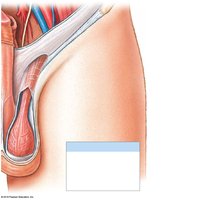
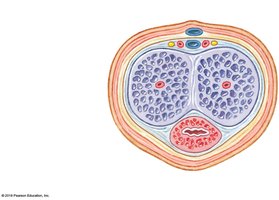
Anatomy of the Testes
Tunica Vaginalis: Serous membrane covering the testes.
Tunica Albuginea: Dense connective tissue capsule surrounding the testes.
Seminiferous Tubules: Site of sperm production; highly coiled tubes within each testicular lobule.
Rete Testis: Network of tubules that collect sperm from seminiferous tubules.
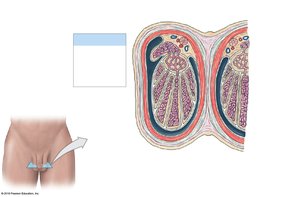
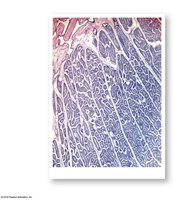
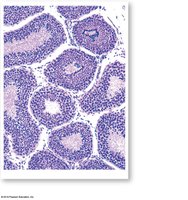
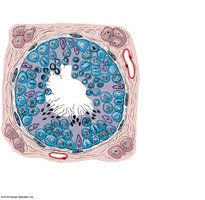
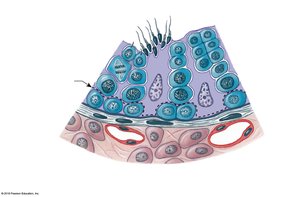
Seminiferous Tubules
Structure: Lined with spermatogenic cells at various stages of development and nurse (Sertoli) cells.
Function: Site of spermatogenesis (sperm production).
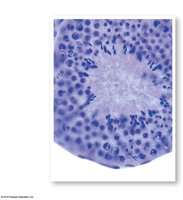
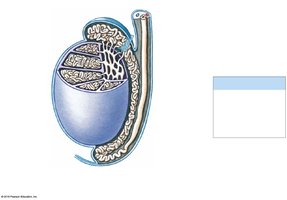
Epididymis
Structure: Coiled tube (~7 m long) attached to the posterior border of each testis; divided into head, body, and tail.
Function: Monitors and adjusts fluid from seminiferous tubules, recycles damaged sperm, stores and protects sperm, and facilitates their functional maturation.
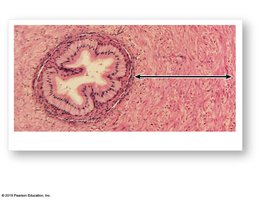
Ductus Deferens (Vas Deferens)
Structure: Muscular tube (40–45 cm) that transports sperm from the epididymis to the ejaculatory duct.
Function: Stores and transports sperm during ejaculation; wall contains thick smooth muscle for peristalsis.
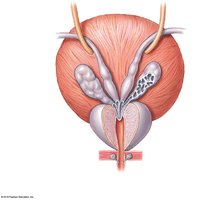
Male Urethra
Function: Shared by urinary and reproductive systems; conducts urine and semen to the exterior.
Regions: Prostatic, membranous, and spongy urethra.
Accessory Glands
Seminal Glands (Vesicles): Produce majority of semen volume; secrete alkaline fluid with fructose, prostaglandins, and fibrinogen.
Prostate: Encircles proximal urethra; secretes slightly acidic fluid (25% of semen volume) containing enzymes and seminalplasmin.
Bulbo-Urethral (Cowper’s) Glands: Secrete thick, alkaline mucus to neutralize urinary acids and lubricate the tip of the penis.
Semen and Seminal Fluid
Semen: Contains sperm, seminal fluid, and enzymes.
Sperm Count: Normal range is 20–100 million sperm/mL; typical ejaculation releases 2–5 mL.
Seminal Fluid: Contains nutrients (fructose), prostaglandins, fibrinogen, and buffers to neutralize acidity.
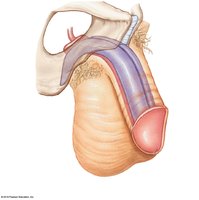
Penis and Erectile Tissue
Penis: Tubular organ that conducts urine and introduces semen into the female reproductive tract.
Erectile Tissue: Network of vascular channels surrounded by elastic and smooth muscle fibers; fills with blood during erection.
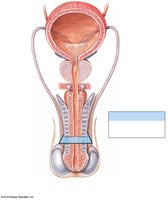
Mitosis, Meiosis, and Spermatogenesis
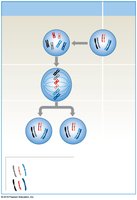
Mitosis
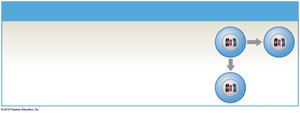
Mitosis is a type of cell division that produces two genetically identical diploid (2n) daughter cells. It is essential for growth and tissue repair in somatic cells.
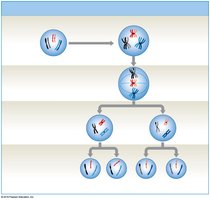
Meiosis
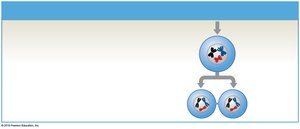
Meiosis is a specialized form of cell division that produces four haploid (n) gametes, each with 23 chromosomes. It involves two successive divisions (meiosis I and II) and introduces genetic variation through crossing over and independent assortment.
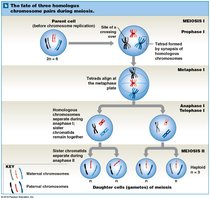
Spermatogenesis
Spermatogenesis is the process of sperm production, beginning at puberty and continuing throughout life. It occurs in the seminiferous tubules and involves three main phases: mitosis, meiosis, and spermiogenesis.
Mitosis: Spermatogonia (stem cells) divide to produce more spermatogonia and primary spermatocytes.
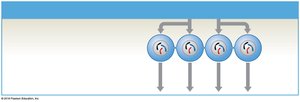
Meiosis: Primary spermatocytes undergo meiosis I to form secondary spermatocytes, which then undergo meiosis II to produce spermatids.
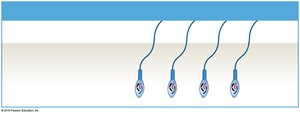
Spermiogenesis: Spermatids mature into spermatozoa (sperm).
Seminiferous Tubule Contents
Spermatogonia
Spermatocytes (various stages)
Spermatids
Spermatozoa
Nurse (Sertoli) cells
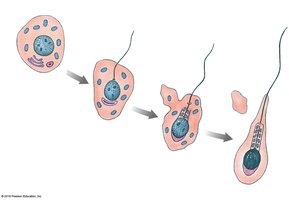
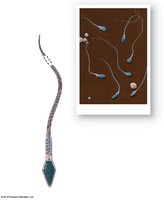
Spermiogenesis
Final maturation phase where spermatids transform into spermatozoa.
Involves condensation of the nucleus, formation of the acrosome, development of the flagellum, and shedding of excess cytoplasm.
Nurse Cells (Sertoli Cells)
Maintain the blood-testis barrier, support mitosis and meiosis, support spermiogenesis, secrete inhibin and androgen-binding protein (ABP).
Blood-testis barrier isolates developing sperm from the immune system.
Secrete inhibin to regulate FSH and GnRH via negative feedback.
Secrete ABP to concentrate testosterone in the seminiferous tubules, promoting spermatogenesis.
Hormonal Regulation of Male Reproductive Function
GnRH (Gonadotropin-Releasing Hormone): Produced by the hypothalamus; stimulates the anterior pituitary to release FSH and LH.
FSH (Follicle-Stimulating Hormone): Stimulates nurse cells to promote spermatogenesis and secrete ABP and inhibin.
LH (Luteinizing Hormone): Stimulates interstitial endocrine cells to secrete testosterone.
Testosterone: Maintains male sexual function, stimulates spermatogenesis, maintains libido, and develops secondary sex characteristics.
Estradiol: Small amounts produced from testosterone by aromatase; increases with age.
Summary Table: Key Structures and Functions of the Male Reproductive System
Structure | Main Function(s) |
|---|---|
Testes | Produce sperm and androgens |
Epididymis | Store, mature, and recycle sperm |
Ductus Deferens | Transport sperm during ejaculation |
Seminal Glands | Produce majority of seminal fluid |
Prostate | Secrete enzymes and seminalplasmin |
Bulbo-Urethral Glands | Secrete alkaline mucus for lubrication |
Penis | Delivers semen to female tract |
Additional info: This guide covers the male reproductive system as outlined in Module 17: Reproductive System, including structure, function, spermatogenesis, and hormonal regulation. For a comprehensive understanding, students should also review the female reproductive system and human development in subsequent modules.
